Millions of Americans travel abroad each
year, with many individuals spending time in rural areas or developing
countries--locations where the risks of contracting an illness are great.
Over the past 25 years, Americans have received a steady stream of news on
emerging infectious diseases such as Lyme disease, Hantavirus, West Nile
virus, and most recently, mumps (sidebar). Due to an increased awareness of
communicable infectious diseases and other illnesses associated with travel,
pharmacists are often asked for advice regarding disease prevention. The
following safety precautions can be used to help counsel individuals on
avoiding travel-related illnesses.

General Travel Health Advice
Health problems associated with
travel can result from such factors as exposure to infectious agents; use of
certain types of transportation, such as cruise ships and airplanes; and
participation in certain activities, such as kayaking and camping. However,
most travel-related illnesses can be prevented with the use of pretravel
planning, immunizations, and safety precautions during travel.1
Pharmacists can be very helpful with this pretravel review, especially if they
are certified to administer vaccines.1
Pretravel planning should involve a visit to
a physician at least one month before a trip to allow time for any recommended
immunizations or other special preparations. Travelers should be advised to
consult their health care provider regarding the length of their trip, season
of travel, areas that will be visited, planned activities, and lodging
arrangements. Current medical status, current medications, conditions or
treatments that may weaken the immune system, and special conditions such as
pregnancy should also be considered.1 Travelers who take medication
regularly should pack an adequate supply to last the duration of the trip.
Travelers should carry their medications with them, rather than pack them in
luggage, to avoid losing their medications.1
Food and Water Safety
Individuals traveling to areas
with poor sanitation should be advised to take food and water precautions.
Contaminated food and water are common causes of infectious traveler's
diarrhea and hepatitis A. Tap water can carry infectious organisms and should
be boiled before use for drinking, brushing teeth, or washing food. Since some
sources of bottled water may be contaminated, it is safer to drink beverages
made from boiled water or to consume carbonated beverages, beer, or wine. Food
precautions include peeling fruits and vegetables before consumption and
avoiding raw vegetables, unpasteurized dairy products, and undercooked or raw
fish or shellfish.1
Traveler's diarrhea is the most common
travel-related disease, affecting 20% to 50% of international travelers--about
10 million people annually.2 About 80% of cases are caused by
bacterial enteropathogens, with enterotoxigenic Escherichia coli (ETEC)
being the most common.2 The primary symptom of ETEC-associated
diarrhea is sudden onset, with four to five watery stools daily. Other
symptoms include nausea, abdominal cramping, vomiting, fever, urgency, and
malaise. Most cases resolve in one to two days, even without treatment, and
are rarely life-threatening. Without treatment, 90% of cases resolve within a
week, and 98% of cases resolve within a month.2
Bismuth subsalicylate taken as two tablets
four times daily or as 2 fluid ounces four times daily has shown to be an
effective preventive measure.2 Clear liquids for rehydration or to
prevent dehydration are also important. If antibiotics are required,
fluoroquinolones are the drugs of choice. Antibiotics are usually given to
patients who experience three or more loose stools in an eight-hour period,
especially if accompanied by nausea, vomiting, abdominal cramps, fever, or
blood in the stool. People with fever or bloody stools should not use
antimotility medications (e.g., loperamide, diphenoxylate), as they can
increase the severity of the disease by reducing clearance of the causative
organisms from the gut.2
Travelers should be advised to avoid
infection-causing organisms in the open water, soil, and sand. It is important
to avoid contact with water infected with schistosoma, a parasite, since even
brief exposure can result in infection. Travelers should also avoid walking in
sand or soil that might be contaminated by human or dog feces, to avoid worm
infections such as hookworm.1
Insect-Borne Diseases
Diseases transmitted by
mosquitoes and arthropods include the domestic arboviral encephalitis, Lyme
disease, tularemia, and plague. Common arboviral (arthropod-borne viruses)
encephalitides in the United States include eastern equine encephalitis,
western equine encephalitis, St. Louis encephalitis, La Crosse encephalitis,
and West Nile encephalitis (table 1). Viruses causing encephalitis are all
transmitted by mosquitoes. Lyme disease is caused by bacteria transmitted by
ticks; plague is caused by bacteria transmitted by rodent fleas; and tularemia
is caused by a bacterium that can be transmitted by ticks, deerflies, and
other insects, as well as by handling infected animal tissue or contaminated
food or water and by inhalation of the bacteria.3
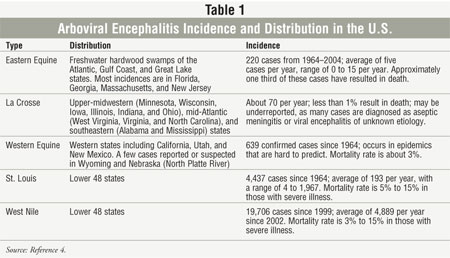
Arboviral encephalitis:
Arboviruses that cause encephalitis are maintained in complex life cycles
that involve nonhuman vertebrate primary hosts (e.g., horses, birds) and
primary arthropod vectors. Most human infections are asymptomatic or involve
nonspecific flu-like symptoms, such as headache, fever, myalgia, and malaise.
Only a small percentage progress to frank encephalitis. Since there are no
effective medications to treat the viral infection and no vaccines for these
diseases, treatment is supportive and is aimed at controlling inflammation of
brain tissues and maintaining breathing. Treatment of secondary bacterial
infections, such as pneumonia, may also be included.
Preventing mosquito bites and using insect
repellents are the most effective ways of preventing the disease. Mosquito
control measures include removing sources of standing water near the home,
such as pet dishes and old tires, and the safe removal of dead animals. Most
states ask that people report dead birds to the department of health, as this
can indicate the presence of viruses, especially West Nile virus.4
Lyme disease:
Lyme disease is the most common vector-borne disease in the U.S., with 74,795
cases reported between 1999 and 2002. The disease, most common in the
northeastern and upper midwestern states of the U.S., is caused by the
bacterium Borrelia burgdorferi, transmitted to humans by infected
black-legged ticks. The bacterium normally lives in squirrels, mice, and other
small rodents. Lyme disease is characterized by arthritis, encephalopathy, and
neuropathy.5 Most cases can be cured with antibiotics, especially
if treatment is started early. However, a small percentage of patients can
suffer muscle and joint pain, cognitive defects, and fatigue, even after
antibiotic treatment. The first sign of infection is usually a circular rash,
seen in about 70% to 80% of cases, which appears three to 30 days after a tick
bite. Patients also may experience fatigue, chills, fever, headache, muscle
and joint aches, and swollen lymph nodes. If left untreated, the infection may
produce a number of symptoms, including loss of muscle tone on one or both
sides of the face (known as facial palsy or Bell's palsy),
severe headaches, neck stiffness due to meningitis, shooting pains that may
interfere with sleep, heart palpitations and dizziness due to changes in
heartbeat, and pain that moves from joint to joint. Many of these symptoms
resolve without treatment.6 Lyme disease rarely results in death,
but even treated cases can result in late Lyme disease characterized by
arthritis, encephalopathy, and neuropathy.7
Tularemia:
Tularemia, also known as rabbit fever, is caused by the bacterium
Francisella tularensis. People usually become infected through the bite of
infected insects, such as ticks and deerflies, by handling sick or dead
infected animals, by eating or drinking contaminated food or water, or by
inhaling airborne bacteria. F. tularensis can stay alive for weeks in
water and soil. About 200 human cases of tularemia are reported each year in
the U.S., with most occurring in the south-central and western states.
Symptoms include skin ulcers, swollen and painful lymph glands, inflamed eyes,
sore throat, mouth sores, diarrhea, and pneumonia. If left un treated,
tularemia can be fatal. The incubation period for the disease is three to five
days, with a range of one to 14 days. Several antibiotics, such as
tetracyclines, fluoroquinolones, streptomycin, and gentamicin, are effective
in treating tularemia infections. The appropriate antibiotic is determined by
lab tests.8
Bubonic plague:
Plague is caused by the Yersinia pestis bacterium, transmitted to
humans through rodent flea bites. About 10 to 15 cases are reported each year
in the U.S., mostly in rural areas of northern New Mexico, northern Arizona,
southern Colorado, California, southern Oregon, or far-western Nevada. Onset
of plague usually occurs two to six days after a person is exposed. Initial
symptoms include fever, headache, and general illness, followed by the
development of painful, swollen regional lymph nodes.
The distinguishing sign of plague is a very
painful and swollen lymph node, called a bubo. Without treatment, a
progressive and potentially fatal illness generally results. Progression leads
to blood infection and, finally, to lung infection, termed plague pneumoni
a, which can be transmitted to others through the expulsion of infective
respiratory droplets by coughing. The death rate for plague pneumonia patients
is over 50%. Streptomycin or gentamicin are the antibiotics of choice, but
other antibiotics, such as tetracyclines and chloramphenicol, are also
effective. Drug therapy should begin as soon as possible after laboratory
specimens are taken. As soon as a diagnosis of suspected plague
is made,
the patient should be isolated, and local and state health departments should
be notified.9
Malaria:
Forty-one percent of the world's population live in areas where malaria is
considered endemic.10 There were 1,337 cases of malaria reported in
the U.S. in 2002; all but five were acquired in malaria-endemic countries and
imported to the U.S.10 The World Health Organization estimates that
300 million to 500 million cases occur worldwide, resulting in more than one
million deaths annually.
Malaria is caused by four kinds of parasites--
Plasmodium falciparum, Plasmodium vivax, Plasmodium ovale,
and Plasmodium malariae. Large areas of Central and South America,
Hispaniola, Africa, the Indian subcontinent, Southeast Asia, the Middle East,
and Oceania are considered malaria-risk areas. The disease, transmitted by an
infected female Anopheles mosquito, can be prevented by avoiding
mosquito bites, taking antimalarial drugs, eliminating mosquito-breeding
places, spraying insecticides on walls, sleeping under bed nets (especially
effective if they are treated with insecticide), and wearing insect repellent
and long-sleeved clothing when outdoors. Appropriate antimalarial medication
is determined by the parasite involved and its resistance to the drug therapy.
Travelers leaving the U.S. should visit their health care provider four to six
weeks before travel to obtain any necessary vaccinations (there are no
vaccines against malaria) and a prescription for an antimalarial drug, if
needed. Antimalarial medication should be taken exactly on schedule, without
missing doses.10
Insect Protection
Precautions should be taken to
avoid insect and arthropod bites, since mosquitoes, flies, fleas, and lice,
ticks, and mites can transmit serious infectious diseases, including malaria,
West Nile virus, plague, Rocky Mountain spotted fever, tularemia, and
arthropod-borne encephalitis.11 The U.S. Environmental Protection
Agency has approved insect repellents containing permethrin, such as
Permanone, for use on clothing, shoes, bed nets, and camping gear. Insect
repellents are covered in detail on page 70.
Transportation Issues
Air travel can involve exposure
to a low-oxygen environment, which can exacerbate chronic obstructive
pulmonary disease and heart conditions. Changes in air pressure can also cause
ear and sinus problems; travelers with these problems may want to use
decongestants prior to flying to avoid discomfort. Sitting still during long
flights can be dangerous for people with clotting or circulatory disorders;
these individuals should discuss the use of medications or compression
stockings with their physicians. Adequate hydration, frequent stretching,
changing positions every one or two hours during a flight, and avoiding
constrictive clothing can help prevent circulatory problems.1
There have been occasional reports of
outbreaks of disease on cruise ships, including infectious gastroenteritis,
measles, rubella, varicella, meningococcal meningitis, hepatitis A, and
legionnaires' disease.12 The CDC established the Vessel
Sanitation Program and has enforced strict sanitation guidelines for all
cruise ships that dock in American ports. Information about health records for
cruise ships can be obtained from travel agents, state health departments, and
the CDC.1
Travel Within the U.S.
Individuals traveling within the
U.S. should be advised to take certain precautions. Plague, Rocky Mountain
spotted fever, tularemia, and arthropod-borne encephalitis occur occasionally
in North America, along with seasonal outbreaks of influenza.13
Coccidioidomycosis is considered endemic in the southwestern U.S., and
histoplasmosis is highly endemic in the Mississippi, Ohio, and St. Lawrence
river valleys. Lyme disease is endemic in the northeastern, mid-Atlantic, and
upper-midwestern U.S. and the southwestern provinces of Canada, while
rodent-borne Hantavirus has been identified in the western states. In
addition, food-borne diseases, such as E. coli and salmonellosis, have
increased in some areas, and outbreaks of hepatitis A have occur red in the
U.S. and Canada.13
Pharmacist's Role
The pharmacist is often asked for
advice prior to travel and should stay current with infectious disease
outbreak information and their common means of transmission, preventive
measures, and signs and symptoms. In most cases, early diagnosis and treatment
can significantly reduce severity of illness, risk of long-term sequelae, and
death. Pharmacists can help identify possible infections in individuals who
present with symptoms and have recently returned from travel. Pharmacists are
well-positioned to provide useful advice, products, and services that can make
travel safer for their patients.
REFERENCES
1. UpToDate Patient Information.
Patient information: General travel advice. Available at:
www.patients.uptodate.com/topic.asp?file=inf_immu/5620&title=Travel+advice,
Accessed May 12, 2006.
2. Centers for Disease Control and
Prevention. Traveler's Diarrhea. Available at:
www.cdc.gov/ncidod/dbmd/diseaseinfo/travelersdiarrhea_g.htm#causes. Accessed
May 18, 2006.
3. Centers for Disease Control and
Prevention. National Center for Infectious Diseases. Division of Vector-Borne
Infectious Diseases. Available at: www.cdc.gov/ncidod/dvbid/index.htm.
Accessed May 13, 2006.
4. Centers for Disease Control and
Prevention. National Center for Infectious Diseases. Information on Arboviral
Encephalitides. Available at: www.cdc.gov/ncidod/dvbid/arbor/arbdet.htm.
Accessed May 2006.
5. Wormser GP, Nadelman RB, Dattwyler
RJ, et al. Practice guidelines for the treatment of Lyme disease. The
Infectious Diseases Society of America. Clin Infect Dis. 2000;31(Suppl
1):S1–S14.
6. Centers for Disease Control and
Prevention. National Center for Infectious Diseases. Lyme Disease. Available
at www.cdc.gov/ncidod/dvbid/lyme/index.htm. Accessed May 14, 2006.
7. Centers for Disease Control and
Prevention. Morbidity and Mortality Weekly Report. Exposure to Mumps During
Air Travel–United States, April, 2006. Available at:
www.cdc.gov/mmwr/preview/mmwrhtml/mm5514a6.htm. Accessed May 11, 2006.
8. Centers for Disease Control and
Prevention. National Center for Infectious Diseases. Tularemia. Available at:
www.cdc.gov/ncidod/dvbid/tularemia.htm. Accessed May 15, 2006.
9. Centers for Disease Control and
Prevention. National Center for Infectious Diseases. Plague. Available at:
www.cdc.gov/ncidod/dvbid/plague/index.htm. Accessed May 15, 2006.
10. Centers for Disease Control and
Prevention. Frequently Asked Questions About Malaria. Available at:
www.cdc.gov/malaria/faq.htm. Accessed May 19, 2006.
11. Centers for Disease Control and
Prevention. Protection Against Mosquitoes and Other Arthropods. Available at:
www2.ncid.cdc.gov/travel/yb/
utils/ybGet.asp?section=recs&obj=bugs.htm&cssNav=browseoyb. Accessed May 12,
2006.
12. Centers for Disease Control and
Prevention. Cruise Ship Travel. Available at: www2.ncid.cdc
.gov/travel/yb/utils/ybGet.asp?section=transportation&obj=cruise.htm&cssNav=browsecyb.
Accessed May 22, 2006.
13. Centers for Disease Control and
Prevention. Health Information for Travelers to North America, including
Canada, St. Pierre and Miquelon [France], United States [including Hawaii].
Available at: www.cdc.gov/travel/namerica.htm. Accessed May 12, 2006.
To comment on this article,
contact
editor@uspharmacist.com.






