Breast cancer is the most common type of cancer diagnosed in women in the United States (excluding cancers of the skin), affecting more than 2.5 million women. In most cases, individuals between the ages of 75 and 79 years account for the highest incidence (i.e., 441.9/100,000). Caucasian women have a higher incidence of breast cancer beginning at the age of 45 years, while African American women have a higher incidence before age 45 years. Caucasian women experience a lower death rate than do their African American counterparts at any age.1 In 2010, the American Cancer Society projects, 207,090 new cases of invasive breast cancer and 54,010 cases of noninvasive breast cancer in situ will be diagnosed among women; an estimated 39,840 women will die of breast cancer.2
Risk Factors
Though the etiology of breast cancer remains unknown, several factors have been associated with its incidence: menarche before the age of 12 years, menopause after 55 years of age, the number of times a woman has given birth, use of birth control, and removal of the ovaries before the age of 35 years.3,4 Not all risk factors are hormonally related, as gene abnormalities have also been associated with risk. For example, mutations to the HER2 gene have been identified as a potential cause of cancer; overexpression of the gene appears to assist in cancerous cell growth.3 In addition, it has been postulated that the alterations in the expression of the TOP2A gene may determine prognosis and response to therapy.5-7
Signs and Symptoms
In most cases, breast cancer in its early stages is asymptomatic. As the cancer evolves, a woman may feel a hard, painless lump characterized by irregular edges in her breast or armpit. Changes in the breast or nipple (i.e., size, shape, etc.) and the secretion of blood or pus may be noted. Further, in the late stage, as the cancer metastasizes to other areas of the body, symptoms may worsen and the patient may present with breast discomfort, bone pain, skin ulceration, difficulty breathing, changes in mental status, loss of weight, jaundice, or swelling of the arm closest to the affected breast.3,4
Methods of Detection
The National Cancer Institute recommends that women should be screened using mammography by the age of 40 years and every 1 to 2 years thereafter. A mammogram, the most common screening tool, examines the soft tissue of the breasts, affording visualization and evaluation of changes in breast tissue. Other diagnostic tools include ultrasound and computer aided detection. MRI, positron emission tomography (PET scanning), and ductal lavage are currently under investigation as methods of breast cancer detection.8
Determining Prognosis
Once breast cancer is detected, clinicians must determine prognosis. A new tool, the TOP2A FISH pharmDx Kit, is available for use in assessing the clinical course of the disease and response to therapy in certain patients with breast cancer. It was approved by the FDA in 2008.
Designed by Dako, the TOP2A FISH pharmDx Kit (FIGURE 1) is a medical device that utilizes fluorescent DNA probes to measure the number of copies of the TOP2A gene located on chromosome 17 in breast cancer cells. Changes in the expression of the TOP2A gene may determine long-term survival rates and the risk of recurrence.5-7

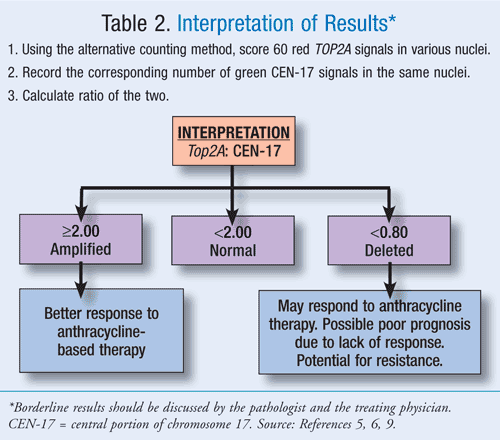
The kit includes a pretreatment solution, pepsin, probe mix, stringent wash buffer, wash buffer, visualization system, and a mounting medium. When using the kit, reagents must be diluted prior to staining, and all procedures must be performed in very specific temperatures. Directions for use, including the required temperatures and interpretation of results, are summarized in TABLE 1 and TABLE 2, respectively.9

Efficacy
The efficacy and accuracy of this product has been tested in several studies. In a study of 126 specimens, 124 specimens were hybridized using the TOP2A FISH pharmDx Kit. When evaluating sensitivity, five nonamplified tissue samples were scored by three different technicians. Samples were confirmed as non-amplified with a mean ratio of approximately 1.0. In a specificity analysis, hybridization was found to be specific for chromosome 17. Repeatability was investigated using consecutive sections of one normal sample and one cancerous sample; a total of 10 cancerous sections were tested. Low variation was found upon interpretation of results ranging from 1.02 to 1.10 with a mean coefficient variation of 3%.9
Conclusion
Though effective, TOP2A testing should not be used alone as a prognostic tool. Nonetheless, the ability to detect the TOP2A gene may influence how we approach the treatment of breast cancer, as preliminary studies appear promising. For more information regarding this product, contact Dako North America, Inc., at 805-566-6655.
REFERENCES
1. American Cancer Society. Breast Cancer Facts & Figures 2009-2010. Atlanta, GA; 2009.
2. American Cancer Society. Cancer Facts & Figures 2010. Atlanta, GA; 2010.
3. MedlinePlus. Breast cancer. www.nlm.nih.gov/medlineplus/ ency/article/000913.htm. Accessed August 10, 2010.
4. Chisholm-Burns M, Wells B, Schwinghammer T, et al, eds. Pharmacotherapy Principles & Practice. New York, NY: McGraw-Hill; 2008.
5. Coon J, Marcus E, Gupta-Burt S, et al. Amplification and overexpression of topoisomerase IIalpha predict response to anthracycline-based therapy in locally advanced breast cancer. Clin Cancer Res. 2002; 8:1061-1067.
6. Nielsen KV, Ejlertsen B, Moller S, et al. The value of TOP2A gene copy number variation as a biomarker in breast cancer: Update of DBCG trial 89D. Acta Oncol. 2008;47:725-734.
7. Sparano J, Goldstein L, Barrett C, et al. Relationship between topoisomerase 2A RNA expression and recurrence after adjuvant chemotherapy for breast cancer. Clin Cancer Res. 2009;15:7693-7700.
8. National Cancer Institute. Mammograms. www.cancer.gov/cancertopics/factsheet/Detection/mammograms. Accessed on August 10, 2010.
9. TOP2A FISH pharmDx™ Kit package insert. Carpinteria, CA: Dako; 2008.
To comment on this article, contact rdavidson@uspharmacist.com





