US Pharm. 2014; (39):6.
One percent of the population carries methicillin-resistant Staphylococcus aureus (MRSA), one of 18 microbes listed by the CDC as being resistant to numerous antibiotics. Since 2007, the National Center for Health Statistics’ Active Bacterial Core surveillance (ABCs) program has tracked the prevalence of invasive MRSA infections. The prevalence decreased by 12.3%, 19.7%, and 25.92%, respectively, in 2009, 2010, and 2011. Most MRSA infections develop in people in hospitals or other healthcare settings, such as nursing homes and dialysis centers, but they also occur in high-risk persons in the community.
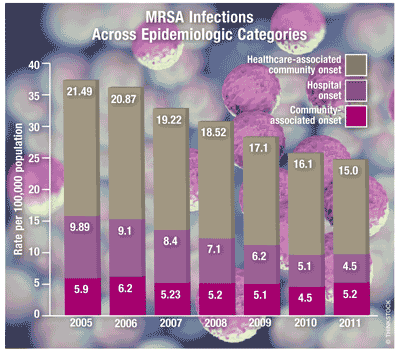
Hospital Onset: Each year, 1.2 million people acquire invasive MRSA infections while inpatients (20% of all hospital infections). At any given time, one in every 20 inpatients has a MRSA infection related to hospital care. Of all invasive MRSA infections, 85% were acquired in the hospital; of these, two-thirds of cases were detected after the hospital stay, and the rest were detected during the stay. MRSA infections have occurred during invasive procedures or through the use of invasive devices. On average, MRSA-infected patients spent an additional 5 days in the hospital. The rate of staph infections fell by nearly 30% in the last decade. Patients who were treated and did well had a high risk of recurrence (20%-40%). Overall, the number of serious MRSA infections diagnosed in hospitalized patients fell by 54% between 2005 and 2011, from 9.7 to 4.5 per 100,000 people. The biggest drop—more than 50%—was in hospital-acquired infections, whereas rates of drug-resistant infections not linked to hospitals or other healthcare settings barely changed.
Healthcare-Associated Community Onset: This type of MRSA infection is acquired by individuals following a hospital stay. The incidence of serious infections diagnosed in individuals who had previously been in a healthcare setting decreased 28% between 2009 and 2011, from 21 to 15 infections per 100,000 population.
Community-Associated Onset: In these cases, MRSA infection is not an outcome of hospitalization, but may include residency at a long-term care facility prior to acquisition of the infection. In the community setting, MRSA infection spreads by skin-to-skin contact, so at-risk populations such as childcare workers and high school wrestlers must pay attention to small red bumps resembling pimples, boils, or spider bites. The CDC reported that, in 2007, 14% of people with MRSA infections contracted the infection outside of a healthcare setting. This number continues to grow.
Dialysis Versus Nondialysis Patients: Invasive MRSA infection is more prevalent in dialysis patients than in the general population. The primary goal of clinicians is to prevent bloodstream infections, particularly among chronic dialysis recipients.
To comment on this article, contact rdavidson@uspharmacist.com.





