US Pharm. 2016;41(3):20.
According to the National Health Interview Survey (NHIS), disabling chronic pain affects 10% of the population. Undiagnosed and untreated chronic pain can result in complications such as depression, anger, reduced self-esteem, and impaired ability to function in day-to-day activities.
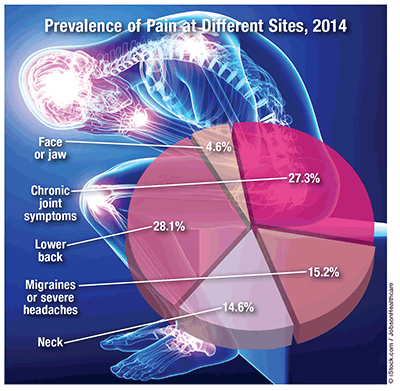
Prevalence: The NHIS notes that 126 million adults (55.7%) experienced some type of pain in 2014. Of these, 20.1% (25.3 million) had pain daily (i.e., chronic pain); additionally, 31.8% (40 million) experienced severe levels of pain, 23.4 million (10.3%) reported a lot of pain, 25.4 million had category 3 pain, and 14.4 million had the highest level of pain (category 4). Based on the persistence and bothersomeness of the pain, adults with category 3 or 4 pain were likely to have worse health status, use more healthcare services, and have more disability than those with less severe pain. Even though chronic ankle or foot pain was the least prevalent type (17%), it had the greatest negative impact on activities (42%), occurred most frequently (61%), and topped the list with respect to duration >3 months (80%).
Women Versus Men: Women were more likely than men (20.7% vs. 16.9%) to have pain across all age groups, except those aged >75 years. Among men and women, those aged 18 to 44 years were less likely to have pain than those in older age groups. Women, older adults, and non-Hispanic patients were more likely to report any pain, whereas Asian patients were less likely. Women were more likely than men to have experienced migraines or severe headaches (21.8% vs. 10%), neck pain (17.5% vs. 12.6%), lower back pain (30.2% vs. 26%), and facial or jaw pain (6.6% vs. 3.3%). In both sexes, lower back pain was most common, and facial or jaw pain was least common. One-year prevalence of migraines peaked around age 40 years for both men and women (8% vs. 25%).
Economic Consequences: Pain is the most prevalent workforce health condition. The total annual economic cost of chronic pain, including treatment and lost productivity, is $635 billion. Adults who used complementary therapies for pain relief spent $14.9 billion out of pocket, and the four most common pain conditions (i.e., back pain, neck pain, joint pain, and arthritis) cost $13.7 billion. For back pain, the highest out-of-pocket expense ($8.7 billion) was for complementary treatments, which constituted 28.5% of all healthcare expenses for back pain ($30.5 billion). Most spending on complementary therapies for back pain ($4.7 billion) was for practitioner visits, not dietary supplements. People with chronic headaches spent a minimum of $568 annually to treat symptoms.
To comment on this article, contact rdavidson@uspharmacist.com.





