US Pharm. 2012;37(6)(Generic Drug Review suppl):40-45.
One of the most confusing markets for consumers is located at the pharmacy counter. The rise of health care costs has lawmakers and employers scrambling to find ways to provide access to care without going bankrupt. Numerous policies at different levels of government and in the private sector have further complicated this market, creating a system nearly impossible for the average person to navigate.
“Market-ish”
Basic microeconomics explains the relationship of supply and demand with the pricing of goods and services. Changes in supply and demand influence market price, and then a price change influences consumer decisions to purchase. In the case of drug pricing, there are several factors that have complicated this particular market.
Expert Influence and Inelasticity of Demand
A major factor in the drug pricing market revolves around the influence physicians and other prescribers have on demand. The process starts when patients visit their physician and receive a prescription for a medication. The prescriber decides on appropriate therapy pursuant to the diagnosis and provides a request for a pharmacist to dispense the medication. While prescribers consider cost important in decision making for their patients, they are often inconsistent or hesitant in applying that awareness in practice.1 When patients are sick, they are likely to heed the expert opinion of the physician, making the price elasticity of demand lower. In other words, price changes will have little effect on the purchasing decision of a sick patient.2 One interesting thing about the demand for health care is that when the patient is not sick the demand for “preventive care” and “prescription medications” is actually more elastic than health care in general.2 So when the price patients have to pay for their medication or other preventive measures goes up, the demand goes down much faster. The cost of doing nothing is hard to define and may not be realized for years, so even small copayment amounts on preventive treatment may be enough to deter a patient from purchasing.
Influence of Supply and Supply Chain Markup
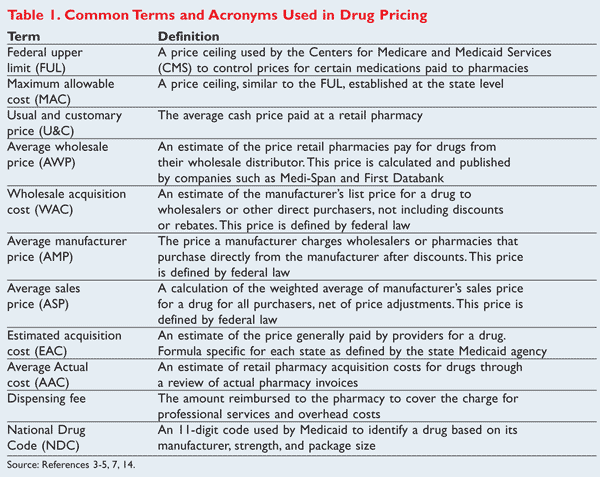
The abundance of pharmaceutical manufacturers makes it difficult for pharmacies to purchase drug products directly from the factory where the drug is produced. The supply of pharmaceuticals involves a chain of wholesalers that help distribute drugs to pharmacies before they reach the patient. The business model for wholesalers relies on the ability to purchase large orders of drug products from manufacturers and sell them to pharmacies at a higher price. The pharmacies benefit from not having to coordinate with all of the manufacturers, and they enjoy reduced inventory carrying costs. This supply chain dynamic has created three transaction areas of particular interest: from manufacturer to wholesaler, from wholesaler to pharmacy, and from pharmacy to patient. Each transaction within the chain allows for measurement of drug pricing, as displayed by the acronyms in TABLE 1 . Using data collected through legally required reporting, voluntary price submissions, or other calculations allows payers to estimate the cost of drugs.
The first transaction in the supply chain between the manufacturer and wholesaler or pharmacy as a direct purchaser produces several different measurements for drug costs. The average manufacturer price (AMP) is a measurement of the price wholesalers pay to purchase drug products from the pharmaceutical manufacturer. The AMP was originally mandated as a part of the Omnibus Budget Reconciliation Act of 1990 (OBRA ’90), and the actual definition continues to evolve.3 AMP is meant to calculate the cost of a drug directly from a manufacturer after any rebate or discount is included. The wholesale acquisition cost (WAC) is an estimate of the manufacturer’s list price for a drug to wholesalers or direct purchasers, but does not include discounts or rebates.3 Without including rebates and other incentives provided by manufacturers, it is hard to estimate the actual cost of the drug. The average sales price (ASP) is derived from the sales from manufacturers to all purchasers and includes practically all discounts, but is limited in that it is only available for Medicare Part B covered drugs.3
The next transaction, between the wholesaler and the pharmacy, is another area of interest for drug cost calculation. The average wholesale price (AWP) is a measurement of the price paid by pharmacies to purchase drug products from wholesalers in the supply chain.4 The most common source for AWP data for drug pricing comes from the compendia produced by Medi-Span and First DataBank.3 The estimated acquisition cost (EAC) is an estimated price that state Medicaid programs use to reimburse pharmacies for the cost of the drug plus a “reasonable” dispensing fee. The EAC is meant to reflect the cost of the drug to the provider from the wholesaler, but is not a published figure. The average actual cost (AAC) is considered the final cost paid by pharmacies to their wholesalers after all discounts have been deducted and is derived from actual audits of pharmacy invoices. Currently, two states are using the AAC for pharmacy reimbursement.3
The final step of the supply chain is at the retail level of distribution where the patient is the end consumer. Usual and customary (U&C) prices reflect the costs of the drugs to the consumer at the retail level without the use of insurance.5 The U&C rate is often referred to as the “cash price” for patients. FIGURE 1 shows a basic supply chain example from manufacturer to consumer along with some of the pricing acronyms and their relation to the supply chain.
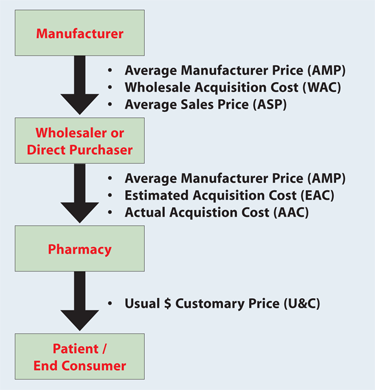
Third-Party System
In most markets, consumers see a price for a good or service and make a decision to purchase if the benefit of the good or service outweighs the cost. In the prescription-drug market, most patients are enrolled with a third-party plan (government and/or insurance company) that utilizes a pharmacy benefits manager (PBM) to help manage this process. The patient pays the third party in the form of premiums along with a contribution from the government or the patient’s employer as a part of the total work compensation to the PBM. At the point of sale when patients pick up their prescription from the pharmacy, they usually pay a smaller portion of the transaction and the PBM reimburses the pharmacy for the balance. Low copays disguise the actual cost of medications, increasing patients’ demand for prescriptions. For example, a patient may be prescribed a medication with a U&C price of $100 for a month’s supply, but with a contracted third-party plan the patient may only be responsible for a $20 copayment to the pharmacy. This reduction in price helps drive consumer demand for this prescription medication. When patients are responsible for a larger proportion of the cost, they are less likely to utilize the health care service.6
Reimbursement Formulation and Contract Pricing
Business owners set prices for the goods and services they provide based on a variety of factors. For a business to be profitable, revenue from the pricing of all goods and services should be greater than the sum of all costs of the business. In the case of pharmacies, pricing of medications for insured patients is determined by contracts with each PBM and the government. In an effort to control spending on prescription drugs in the Medicaid system, the federal government sets a price ceiling for certain drugs called the federal upper limit (FUL).3,7 Individual states and PBMs then take this cost containment a step further by establishing a maximum allowable cost (MAC) for drug products.4 If costs for a pharmacy to dispense a medication are higher than the contracted price agreements, the pharmacy will operate at a loss in order to service the patient, or the pharmacy may withdraw from participation in the network. To offset losses on some drug products in third-party contracts, some pharmacies may increase their U&C prices for noninsured patients or attempt to offer other services or nonprescription products to capture revenue.
Pharmacy revenue may also be derived from a dispensing fee added to the drug price. Some third-party contracts include a dispensing fee to help cover the pharmacy’s professional and operational expenses. Operating expenses are different for every pharmacy. These expenses may include wages, advertising, utilities, administration, and supplies. According to the National Association of Chain Drug Stores (NACDS) 2011-2012 Chain Pharmacy Industry Profile, the average cost for retail pharmacy operations is $11.34 for each prescription.8 This means that in order for a pharmacy to earn income beyond the cost of doing business, it must have an average reimbursement that is greater than the cost of the drug plus $11.34. Dispensing fees paid to pharmacies vary. For example, state Medicaid dispensing fees paid to pharmacies in 2010 were anywhere from $1 to $14.01 per prescription.9,10 In reimbursement models with low dispensing fees, pharmacies are dependent on the margin they can make from the cost of the drug to the final sale to the patient.
Gaining From Pharmacy Loss
The competition in the retail market has become fierce, and leverage from PBMs has made it more difficult for pharmacies to profit solely from medication dispensing. Some community pharmacies utilize the prescription dispensing service as a way to draw in customers and so generate revenue from other sources.11 Pharmacies offer a wide variety of nonprescription products and general retail merchandise. As revenue from prescription dispensing decreases, pharmacies rely more on this portion of the business.
Other Profit Incentives
The simple transaction of a pharmacy dispensing a drug to a patient pursuant to a prescription has provided multiple opportunities for companies to profit. In the case of the PBM, two additional revenue generators have emerged: spread pricing and manufacturer rebates.12
Spread pricing refers to the difference between what the PBM charges a patient or patient’s health insurance and what the PBM pays the pharmacy for dispensing the medication. When the patient receives an explanation of benefits (EOB) from the insurance company, the apparent total cost of the medication may be higher than what the pharmacy is actually paid due to the markup by the PBM within the spread. This value may vary depending on the drug product. This type of markup is much more complicated than a simple flat fee per claim submitted to the PBM. For example, a PBM may contract to bill an employer using the AWP estimation for drug costs. If the PBM then contracts with a pharmacy to reimburse the pharmacy for drug costs using MAC pricing, the PBM would then profit from the difference of this calculation. In this oversimplified example, in cases where the AWP and MAC are similar, the profit margin or “spread” may be quite small, but in some cases the AWP may be much greater than the MAC, allowing for a very profitable spread.12
Manufacturer rebates are direct payments from pharmaceutical companies to PBMs in order to have their drug in an advantageous position on a formulary. In therapeutic classes where multiple brand-name medications are available as acceptable treatment, PBMs are able to negotiate with pharmaceutical manufacturers to make a particular drug preferred to patients under the prescription drug plan.12 This example was illustrated in 2011 following the release of atorvastatin (generic for the Pfizer blockbuster drug Lipitor) into the prescription market. One of the largest PBMs negotiated with Pfizer to make brand Lipitor preferred over the newly released generic version for a specified period of time.13
Percentages Do Not Equal Dollars
The complexity of the prescription-drug market makes it very difficult for the general public to understand and for policy makers to develop a fair way to reimburse pharmacies for dispensing a drug. For example, on paper a 175% markup on a drug may seem like a great deal for a pharmacy. When you apply this example to a generic medication that may cost a pharmacy only $1 for 30 tablets, the margin for the pharmacy is only 75 cents. This gross profit amount is not enough to cover the cost of the vial, label, lid, prescription bag, or of overhead to keep the electricity on in the pharmacy and pay wages to employees. If you apply that same formula of a 175% markup on a more expensive therapy that costs the pharmacy $100 for 30 tablets, the margin for the pharmacy is now $75. Laws with good intentions often have unintended consequences. In this simple theoretical case, the incentive at the pharmacy level is much greater to dispense a more expensive therapy.
Conclusion
Drug pricing is influenced by a variety of factors, and the complexity can be overwhelming for health care professionals as well as the public. It is important that we continue to discuss current and proposed models for drug pricing, pharmacy reimbursement, and the final cost to the patient. While being an expert on pricing acronyms and federal statutes does not help pharmacists provide care to patients, understanding the basic language used in drug pricing is an essential skill for anyone involved in the prescription-drug market.
REFERENCES
1. Ginsburg M, Kravitz RL, Sandberg WA.
A survey of physician attitudes and practices concerning
cost-effectiveness in patient care. West J Med. 2000;173:390-394.
2. Ringel JS, Hosek SD, Vollaard BA,
Mahnovski S. The elasticity of demand for health care: a review of the
literature and its application to the military health system. Santa
Monica, CA: RAND Corporation; 2002.
www.rand.org/pubs/monograph_reports/MR1355.
3. Curtiss F, Lettrich P, Fairman K. What is the price benchmark to replace average wholesale price (AWP)? J Manag Care Pharm. 2010;16(7):492-501.
4. Gencarelli DM. One pill, many
prices: variation in prescription drug prices in selected government
programs. NHPF issue brief / National Health Policy Forum, George
Washington University. 2005(807):1-20.
5. Prescription drugs: Trends in usual and customary prices for commonly used Drugs. GAO Reports. March 14, 2011:1-26.
6. Wong MD, Andersen R, Sherbourne CD,
et al. Effects of cost sharing on care seeking and health status:
results from the Medical Outcomes Study. Am J Public Health. 2001;91:1889-1894.
7. Office of the Inspector General
(OIG). A Comparison of Medicaid Federal Upper Limit Amounts to
Acquisition Costs, Medicare Payment Amounts, and Retail Prices.
Washington, DC: US Department of Health and Human Services; August
2009:OEI-03-08-00490.
8. NACDS 2011-2012 Chain Pharmacy Industry Profile. Alexandria, VA. National Association of Chain Drug Stores; 2011.
9. Office of the Inspector General
(OIG). Replacing Average Wholesale Price: Medicaid Drug Payment Policy.
Washington, DC: US Department of Health and Human Services; July
2011:OEI-03-11-00060.
10. CMS. Medicaid Prescription
Reimbursement Information by State – Quarter Ending December 2010.
www.cms.gov/Reimbursement/Downloads/1Q2011ReimbursementChart.pdf.
Accessed March 18, 2012.
11. Meszaros L. Pharmacy of tomorrow: the future will embrace pharmacists’ unique clinical capabilities. Drug Topics.
August 10, 2009.
http://drugtopics.modernmedicine.com/drugtopics/Modern+Medicine+Now/Pharmacy-of-tomorrow/ArticleStandard/Article/detail/617024.
Accessed March 18, 2012.
12. Rentmeester CA, Garis RI. Rebates and spreads: pharmacy benefit management practices and corporate citizenship. J Health Polit, Policy Law. October 2008;33(5):943-963.
13. Peterson M. Medco won’t cover generic Lipitor for Coventry Health Members. Bloomberg Businessweek.
November 22, 2011.
www.businessweek.com/news/2011-11-22/medco-won-t-cover-generic-lipitor-for-coventry-health-members.html.
Accessed March 18, 2012.
14. Office of the Inspector General
(OIG). Medicaid Drug Price Comparisons: Average Manufacturer Price to
Published Prices. Washington, DC: US Department of Health and Human
Services; June 2005:OEI-05-05-00240.
To comment on this article, contact rdavidson@uspharmacist.com.






