US Pharm. 2016;41(7):30-34.
ABSTRACT: Seasonal allergic rhinitis is an inflammatory response to seasonal allergens in the nasal mucosa that produces symptoms of rhinorrhea, sneezing, and nasal itching and/or congestion. The treatment of seasonal allergic rhinitis consists of a variety of options, including nonpharmacologic therapies, oral antihistamines, intranasal antihistamines, intranasal corticosteroids, oral leukotriene receptor antagonists, and mast cell stabilizers. At this time, intranasal corticosteroids and oral antihistamines remain the mainstay of treatment for seasonal allergic rhinitis. Evidence of the efficacy of the combination of intranasal corticosteroids and oral antihistamines is lacking; therefore, the simultaneous use of these agents is not recommended.
In the United States, it is estimated that 15% to 30% of people have allergic rhinitis.1 Approximately 19 million U.S. adults were diagnosed with allergic rhinitis in 2014, representing about 8% of the population.2 Allergies are the sixth leading cause of chronic illness in the U.S.3 In one study, allergic rhinitis was the most causative chronic condition associated with productivity loss, at an estimated cost of $593 per employee per year.4 The healthcare cost of allergic rhinitis, when combined with allergic conjunctivitis, is estimated to exceed $6 million annually.5
Allergic rhinitis, often called hay fever, is an inflammatory response to an allergen that is mediated by immunoglobulin E.6 The inflammatory response occurs in the nasal mucosa and produces symptoms of anterior or posterior rhinorrhea, nasal congestion and/or itching, and sneezing. Diagnosis of allergic rhinitis is not typically made until around age 3 or 4 years owing to the multitude of viral respiratory infections that occur in young children. During the first year of life, infants begin to become sensitized to inhaled allergens, starting with indoor allergens, then outdoor.7
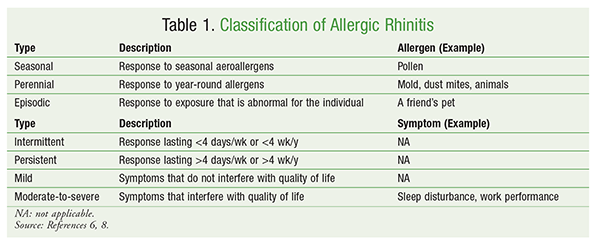
Allergic rhinitis is classified according to pattern of exposure, frequency of symptoms, and severity of symptoms. The pattern of exposure can be categorized as seasonal, perennial, or episodic; the frequency of symptoms can be classified as intermittent or persistent, and the symptom severity can be mild or moderate-to-severe.6,8 Treatment of allergic rhinitis depends on the classification. TABLE 1 summarizes the classification criteria for allergic rhinitis.
SEASONAL ALLERGIC RHINITIS
In seasonal allergic rhinitis, the triggering allergens do not occur year-round; rather, they are present for a specific time period.8 Depending on the allergens and the location, the length of exposure is variable. It can sometimes be difficult to differentiate between seasonal and perennial allergic rhinitis, since a patient with multiple seasonal triggering allergens may exhibit symptoms year-round. Accordingly, seasonal allergic rhinitis may present with intermittent or persistent symptoms. Some allergens, such as mold, may be considered either seasonal or perennial. Perennial allergic rhinitis may be compounded by additional seasonal allergens. Therefore, knowledge of the symptom severity and frequency is of paramount importance in determining the most appropriate treatment.8
MANAGEMENT OF SEASONAL ALLERGIC RHINITIS
Commonly referenced guidelines include the 2010 update to Allergic Rhinitis and Its Impact on Asthma (ARIA) and the American Academy of Otolaryngology–Head and Neck Surgery Foundation’s (AAO-HNSF’s) 2015 clinical practice guideline for allergic rhinitis.6,8,9
Nonpharmacologic Measures
Allergen avoidance is a nonpharmacologic strategy often recommended to patients with allergic rhinitis. Interestingly, the majority of measures used to reduce indoor allergens do not have a clinically significant impact on allergic rhinitis when they are practiced individually. It is still recommended that patients with animal allergies avoid the specific animals they react to.6 It is possible that a multicomponent approach to allergen avoidance would be more effective for allergen-exposure reduction; however, evidence supporting this theory is not available. In patients who are sensitized to occupational allergens, avoidance is recommended; in cases where this is not possible, exposure to the occupational allergen should be controlled.6
Nasal saline has long been touted as a nonpharmacologic measure for allergic rhinitis. A 2015 Cochrane review on the use of nasal saline for acute upper respiratory infections, including the common cold and rhinosinusitis, found a minimally significant reduction of nasal discharge and obstruction.10 Another nonpharmacologic treatment for allergic rhinitis is acupuncture, which in randomized, controlled trials has shown promise in providing some symptom control with minimal risk of harm to the patient.8
Pharmacologic Measures
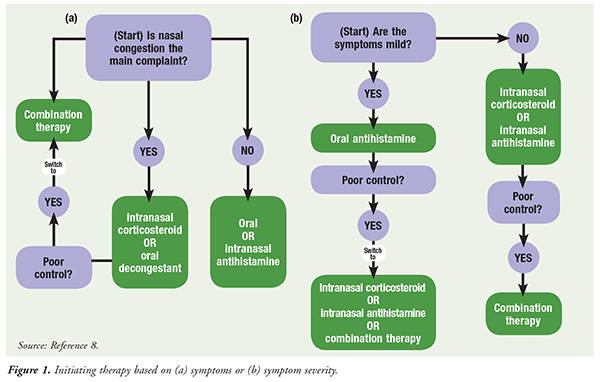
FIGURE 1 summarizes the treatment-initiation recommendations for seasonal allergic rhinitis from the AAO-HNSF’s 2015 clinical practice guideline for allergic rhinitis.8
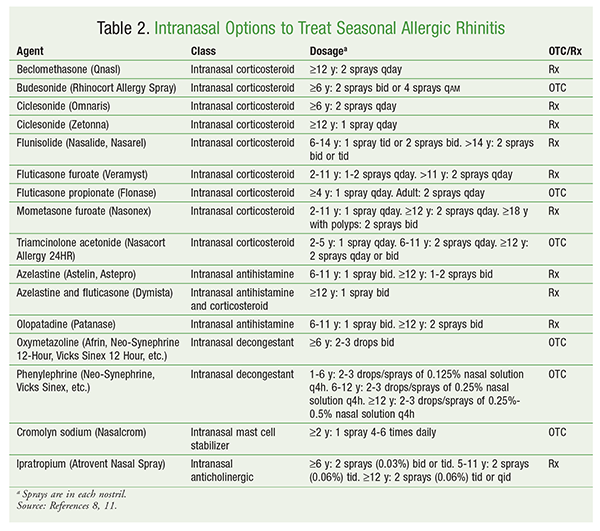
Intranasal Corticosteroids: Intranasal corticosteroids, recognized as the most effective agent for symptom control in allergic rhinitis, are currently recommended as first-line therapy for patients with moderate-to-severe symptoms or those with nasal congestion as the dominant complaint.8 The onset of action ranges from 3 to 36 hours after the first dose, and continuous use is more effective than intermittent use. If efficacy is not established within 1 week, treatment is considered ineffective. No single product is recommended over another, as studies have shown comparable efficacy among products. In the control of nasal symptoms, intranasal corticosteroids have shown superior efficacy compared with oral antihistamines; however, intranasal antihistamines have a faster onset of action, which may be beneficial. Local stinging and burning, dryness, and nosebleeds are common adverse effects (AEs) of intranasal corticosteroids. Concerns over stunted growth in children precipitated several clinical trials; reduced growth was seen with budesonide and beclomethasone, but not with fluticasone furoate, triamcinolone acetonide, mometasone furoate, or fluticasone propionate. Accordingly, for pediatric patients, guidelines recommend using those agents not shown to reduce growth.8 The use of nasal saline 5 minutes after taking intranasal corticosteroids may reduce the incidence or severity of side effects. TABLE 2 summarizes the available intranasal products for seasonal allergic rhinitis.
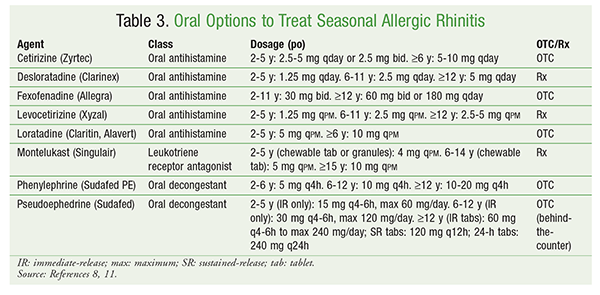
Oral Antihistamines: Oral antihistamines are recommended as first-line agents in patients with mild symptoms of allergic rhinitis or those with sneezing and itching as the primary complaint.8 Second-generation antihistamines are used to manage allergic rhinitis because they do not penetrate the central nervous system to the extent that first-generation antihistamines do, and therefore have milder sedative properties. These agents, although less effective than intranasal corticosteroids, are recommended because they are readily available OTC, cost less, have a fast onset of action (average of 150 minutes), and are dosed once daily. Patients who fail treatment with one agent in this class may exhibit a response to an alternative agent. Higher efficacy is demonstrated with regular use than with intermittent use. Common AEs include dryness of the mucous membranes, urinary retention, and occasional sedation.8 These agents may be dosed at night if a patient experiences sedation. TABLE 3 summarizes the oral products used to treat seasonal allergic rhinitis.
Intranasal Antihistamines: These agents are the second most effective treatment for seasonal allergic rhinitis and are recommended as second-line therapy for patients with intermittent nasal symptoms in whom congestion is not dominant.8 They are also next in line after oral antihistamines for patients with mild allergic rhinitis symptoms and may be used in patients with moderate-to-severe symptoms of allergic rhinitis. In clinical trials, intranasal antihistamines have been shown to be equal or superior to oral antihistamines for symptom control. Compared with oral antihistamines, they are superior for reducing intranasal congestion and systemic effects. The available preparations are of equal efficacy. These agents have been shown to be beneficial in patients who fail to respond to oral antihistamines. Some trials found that intranasal antihistamines were equal in efficacy to intranasal corticosteroids, and certain antihistamines were superior. Intranasal antihistamines have an onset of action of 15 to 30 minutes and are approved for use in children aged ≥6 years.8 See TABLE 2 for a summary of products used to treat seasonal allergic rhinitis.
Oral Decongestants: These agents are recommended in patients with allergic rhinitis whose primary complaint is nasal congestion.8 There are currently two available products: pseudoephedrine and phenylephrine. Pseudoephedrine is widely recognized as the more effective of the two agents. These agents are contraindicated in patients with severe coronary artery disease and uncontrolled hypertension (HTN). Caution should be used when recommending these agents to patients with a history of HTN (controlled or uncontrolled), arrhythmias, glaucoma, hyperthyroidism, benign prostatic hyperplasia, ischemic heart disease, and renal failure. Common AEs include HTN, tachyarrhythmia, anxiety, insomnia, and restlessness. Serious AEs include atrial fibrillation and myocardial infarction.11 See TABLE 3 for a summary of products used to treat seasonal allergic rhinitis.
Intranasal Decongestants: Because of the possibility of rhinitis medicamentosa (rebound congestion), these agents should be used only as adjuvant therapy for 3 to 5 days.8 Intranasal decongestants are contraindicated in patients with uncontrolled HTN, narrow-angle glaucoma, and ventricular tachyarrhythmia. Common AEs include burning and stinging in the eye.11 See TABLE 2 for a summary of products used to treat seasonal allergic rhinitis.
Leukotriene Receptor Antagonists: No longer recommended as primary therapy in allergic rhinitis, leukotriene receptor antagonists are reserved for combination therapy.8 This recommendation is based on several factors, including the higher cost, lower efficacy, and more prominent AEs associated with these agents. Postmarketing data have demonstrated drug-induced aggression, depression, suicidal thinking, and behavioral issues. The leukotriene receptor antagonist montelukast was found to be either equally effective or less effective than oral antihistamines, and it was less efficacious than intranasal corticosteroids. Because this agent treats both allergic rhinitis and asthma, a patient with both conditions is the best candidate.8 See TABLE 3 for more information on montelukast.
Intranasal Mast Cell Stabilizers: Also called cromones, these products have long been available OTC for the treatment of allergic rhinitis. The intranasal agent cromolyn sodium (e.g., Nasalcrom) is not mentioned in the AAO-HNSF’s 2015 guideline, but the ARIA guidelines recommend its use when other, more effective agents are not available. Intranasal antihistamines are preferred over cromolyn sodium, based on efficacy results.6,8,9 Intranasal cromolyn must be dosed four times daily and titrated up to six times daily if needed, making adherence more difficult compared with other therapies. For seasonal allergic rhinitis, it is recommended to start using intranasal cromolyn sodium 1 to 2 weeks prior to the allergy season. These agents have a long history of safe use, making them a good option for pregnant patients (Category B). The most commonly reported AEs include bad taste in the mouth, cough, and throat irritation.11 See TABLE 2 for more information on cromolyn sodium.
Intranasal Anticholinergics: Intranasal anticholinergics are available by prescription only. Currently, only one product is on the market. This agent, ipratropium, exclusively targets rhinorrhea. Although it is discussed in the ARIA guidelines, it is not mentioned in the AAO-HNSF’s guideline.6,8 See TABLE 2 for more information on ipratropium.
Combination Therapy: In patients with inadequate symptom control on intranasal corticosteroid monotherapy, an intranasal antihistamine or a 3-day regimen of oxymetazoline may be added.8 In the event of inadequate symptom control with intranasal antihistamine monotherapy, intranasal corticosteroids may be added. Additionally, patients who experience inadequate symptom control on oral antihistamine monotherapy may be switched to intranasal corticosteroids or intranasal antihistamine. If adjunct therapy to an oral antihistamine is preferred, oral decongestants and leukotriene receptor antagonists are options.8
The combination of intranasal corticosteroids and oral antihistamine is not recommended owing to the lack of benefit of this combination. The combination of intranasal corticosteroids and leukotriene receptor antagonists also lacks sufficient evidence of benefit to be recommended for use.8
CONCLUSION
Given the recent updates to guidelines and the availability of OTC medications in most of the pharmaceutical classes, pharmacists are uniquely positioned to positively impact the management of seasonal allergic rhinitis. The two main classes to recommend are intranasal corticosteroids and oral antihistamines, followed by intranasal antihistamines. Proper classification of allergic rhinitis is important in determining the most appropriate choice of medication. Patients with moderate-to-severe seasonal allergic rhinitis and those with congestion as the predominant symptom will obtain the most benefit from intranasal corticosteroids. Patients with mild seasonal allergic rhinitis and those with itching and sneezing as predominant symptoms should use oral antihistamines. Combination therapy for poorly controlled seasonal allergic rhinitis can be complicated, but proper guidance by a pharmacist can help relieve the discomfort caused by this condition.
REFERENCES
1. Salo PM, Calatroni A, Gergen PJ, et al. Allergy-related outcomes in relation to serum IgE: results from the National Health and Nutrition Examination Survey 2005-2006. J Allergy Clin Immunol. 2011;127:1226-1235.e7.
2. CDC. Allergies and hay fever. www.cdc.gov/nchs/fastats/allergies.htm. Accessed March 31, 2016.
3. CDC. Allergies. www.cdc.gov/healthcommunication/ToolsTemplates/EntertainmentEd/Tips/Allergies.html. Accessed March 31, 2016.
4. Lamb CE, Ratner PH, Johnson CE, et al. Economic impact of workplace productivity losses due to allergic rhinitis compared with select medical conditions in the United States from an employer perspective. Curr Med Res Opin. 2006;22:1203-1210.
5. Bernstein DI, Schwartz G, Bernstein JA. Allergic rhinitis. Immunol Allergy Clin North Am. 2016;36:261-278.
6. Bousquet J, Khaltaev N, Cruz AA, et al. Allergic Rhinitis and its Impact on Asthma (ARIA) 2008 update (in collaboration with the World Health Organization, GA(2)LEN and AllerGen). Allergy. 2008;63(suppl 86):8-160.
7. Wheatley LM, Togias A. Allergic rhinitis. N Engl J Med. 2015;372:456-463.
8. Seidman MD, Gurgel RK, Lin SY, et al. Clinical practice guideline: allergic rhinitis. Otolaryngol Head Neck Surg. 2015;152(suppl 1):S1-S43.
9. Brozek JL, Bousquet J, Baena-Cagnani CE, et al. Allergic Rhinitis and its Impact on Asthma (ARIA) guidelines: 2010 revision. J Allergy Clin Immunol. 2010;126:466-476.
10. King D, Mitchell B, Williams CP, Spurling GK. Saline nasal irrigation for acute upper respiratory tract infections. Cochrane Database Syst Rev. 2015;(4):CD006821.pub3.
11. Micromedex (electronic version). Greenwood Village, CO: Truven Health Analytics; 2016. www.micromedexsolutions.com/micromedex2/librarian. Accessed April 11, 2016.
To comment on this article, contact rdavidson@uspharmacist.com.






