US Pharm. 2013;38(9):36-39.
ABSTRACT: Depression, like many other psychiatric illnesses, may present differently in women versus men. These disparities go beyond the depressive syndromes unique to women—namely, postpartum and menopausal depression—and often manifest in women with major depressive disorder. The STAR*D study found that women may be more prone to atypical symptoms of depression. Also, some data indicate that women may respond more robustly to selective serotonin reuptake inhibitors, whereas men may favor tricyclic antidepressants. Additional treatment considerations include variability in pharmacokinetics, effects on bone density, and key drug interactions more likely in women. An understanding of the etiology, presentation, and specific treatment of depression in women will lead to a more successful outcome.
Cardiovascular disease, osteoporosis, autoimmune disease—these are just a few of the conditions in which clinicians consider gender when making a diagnosis or selecting therapy. So why isn’t gender necessarily considered in the identification and treatment of psychiatric disorders, which also can vary greatly between the sexes? One of the most common examples of gender variation in psychiatric disorders is major depressive disorder (MDD). MDD and similar depressive disorders do not necessarily manifest identically in men and women. Prevalence, comorbid disorders, and optimal therapy may differ between men and women. Certainly, depressive symptoms occurring during the perinatal and postmenopausal periods or as part of premenstrual dysphoric disorder are recognized to be unique to women, but clinicians should be aware of disparities seen outside of these specific conditions. For these reasons, it is crucial for the clinician to anticipate and recognize gender distinctions when evaluating female patients at risk for, or diagnosed with, depression.
PREVALENCE
As much as 10% to 20% of the population will be diagnosed with depression.1 When the female population is specifically considered, this already substantial percentage grows even larger. While rates of depression are similar between the sexes during childhood and adolescence, women are twice as likely as men to be diagnosed with depression.2 The 12-month prevalence rate for MDD in nonpregnant women aged 18 to 50 years is between 8% and 16%—roughly double the rate observed in men.3 Of even greater concern is that more than half of women who meet criteria for MDD are not properly diagnosed. One explanation may be that women and men present differently and nonpsychiatric clinicians have difficulty recognizing depression in women.4
ETIOLOGY
Various causes of—and factors contributing to—the higher rate of depression in women have been considered. Hormonal fluctuations and their role in depression are a natural starting point for elucidating gender differences in this mood disorder. Indeed, estrogen may play some role in differentiating depression in women. This hormone may initially seem to be an outlier in the neurotransmitter model of MDD, but its involvement becomes more evident upon closer examination.5 Estrogen is involved in modulating neurotransmitter turnover and regulating receptor number and function. This affects serotonin and possibly norepinephrine, two of the three most commonly targeted neurotransmitters in the treatment of depression. Alterations in estrogenic activity in women may lead to disruptions in these systems, which may partially explain the increased rate of depression.5 Additionally, some studies suggest that certain estrogen receptor (ER) polymorphisms may increase the risk of depression—particularly severe depression—in women.6 Another link between estrogen and depression involves possible activity between estrogens and monoamine oxidase (MAO), the same enzyme on which the oldest class of antidepressants exerts its effects.7
To date, however, there is no clear understanding of what causes disparities in depression between genders. Most likely, it is a combination of many factors: the hormonal and neurobiological variables already discussed, as well as social and behavioral factors (e.g., burdens associated with caregiving or traumatic events and stressors more likely encountered by women).8
PRESENTATION
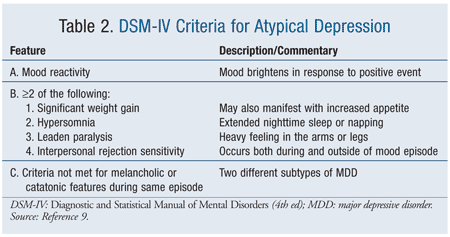
Depressive disorders are identified primarily through subjective patient symptoms. To fulfill a diagnosis, a depressed mood or lack of interest in pleasurable activities for 2 weeks plus an additional five or more symptoms must be present.9 These symptoms include, but are not limited to, feelings of guilt and changes in weight, sleep, energy, or concentration. On the surface, men and women may seem to meet these criteria similarly. However, an examination of how these symptoms present reveals marked differences between genders (TABLE 1).

STAR*D (Sequenced Treatment Alternatives to Relieve Depression), a large, pragmatic study that evaluated multiple therapies for depression, found that, compared with men, women typically had an earlier onset of first major depressive episode, made an increased number of suicide attempts, and reported symptoms correlating to a more severe depressive episode. Women also were more likely to report increased appetite and weight, reduced energy, and greater interpersonal sensitivity.10 These complaints are components of atypical depression (TABLE 2), a depressive subtype that occurs more often in women than in men.11 An awareness of the STAR*D findings will assist clinicians treating female patients with depression who report a depressed mood or decreased pleasure, but do not report (or are vague about) other common symptoms of depression. Considering that all antidepressants have a similar efficacy profile, these complaints are useful in driving therapy to target specific symptoms.
TREATMENT
Pharmacologic Therapy
Because the etiology of depression in women may sometimes be distinct and women may present differently from men, it has been proposed that effective treatments, particularly pharmacologic ones, may differ by gender. However, supporting data are limited and sometimes conflicting. Additionally, no major treatment guideline currently steers therapy according to gender.4 Regardless, it is prudent to examine how pharmacotherapeutic efficacy may differ between men and women.
One of the better-studied gender-specific treatment comparisons for depressed patients is selective serotonin reuptake inhibitors (SSRIs) versus tricyclic antidepressants (TCAs). Multiple studies, such as one by Baca and colleagues, have demonstrated that women may respond better to SSRIs than to TCAs.12 In this study, women with nonmelancholic depressive disorders who received sertraline had significantly larger reductions on the Hamilton Rating Scale for Depression (HAM-D) versus those receiving imipramine. Sertraline also was better tolerated than imipramine, with imipramine being discontinued more than three times as often as sertraline. Similarly, in an analysis of STAR*D data, Trivedi and colleagues found that, compared with men, women taking citalopram were more likely to show remission on the HAM-D, a goal of therapy that is ideal but sometimes difficult to achieve.13 It is unclear why women may have a better response to SSRI therapy, but one theory is the interaction between estrogen and serotonin activity, which may cause women to respond better to medications that act solely on the serotonergic system.2
Limited data indicate that women may have an inherent slight preference for SSRIs over serotonin-norepinephrine reuptake inhibitors (SNRIs). Keers and Atchison suggest this in an analysis of a review by Khan and colleagues of 15 trials and six different antidepressants.2,14 Compared with men, women taking SSRIs were more likely to complete therapy and responded better on the HAM-D scale; in subjects treated with SNRIs, however, there was little difference between genders. The clinical significance is questionable, but the finding is noteworthy nonetheless, since both of these drug classes are considered first-line, and occasionally one class is not more appropriate than the other for initial treatment of depression.
If no single first-line agent is more suitable than another for a female patient, it may be reasonable to select an SSRI, since women taking SSRIs may be more likely to complete therapy. However, this has not been fully determined, since evidence concerning preferential pharmacotherapy by gender is conflicting. Studies such as that by Thiels and colleagues failed to duplicate results favoring SSRIs in women.15 Furthermore, Yang and colleagues found that, regardless of type, women responded better to antidepressants than men did.16 Therefore, the extent to which gender should guide the choice between SSRIs and SNRIs is unknown, and more traditional and better-studied factors for determining appropriate therapy should be considered first.
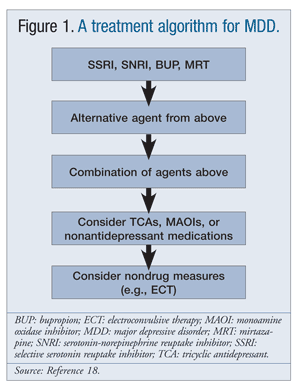
As previously discussed, women are more likely to present with symptoms congruent with atypical depression. This is a key consideration, since this form of depression may respond more robustly to SSRIs and MAO inhibitors (MAOIs) than to TCAs.2,17 SSRIs are usually among the first agents chosen for depression because of their favorable adverse-effect (AE) profile; MAOIs, however, are not (FIGURE 1). MAOIs are most often reserved for depression that is unresponsive to multiple other drug therapies.18 In treating depression in women with a confirmed atypical subtype, it may be appropriate to consider MAOIs somewhat earlier in patients who have failed other agents. In some studies, women responded better to MAOIs than to TCAs, a class that is usually chosen before MAOIs in depressed patients.7 Additionally, women with depression and coinciding panic attacks responded more favorably to MAOIs than to TCAs.7
Nonpharmacologic Therapy
Nonpharmacologic methods for treating depression, such as exercise and psychotherapy, are key components of a treatment plan for patients with depression. With these methods, there does not seem to be a difference in response rate between genders.4 Therefore, these treatment modalities should not be guided based on gender, whereas pharmacotherapy may be somewhat influenced by gender.
PHARMACOKINETIC CONSIDERATIONS
Pharmacokinetic disparities may influence a patient’s response to antidepressant treatment. The absorption and volume of distribution (VD) of many drugs vary between the sexes because women have a higher percentage of adipose tissue than men, resulting in increased VD of lipophilic drugs, a property held by many antidepressants. Both trazodone and bupropion have demonstrated a greater VD in women.7,19 Furthermore, clearance of antidepressants may be reduced in women, since they secrete less gastric acid and exhibit decreased gastric motility and emptying times.5
Differences in enzymatic activity may exist as well, since women are known to have a smaller concentration of P-glycoprotein (Pgp) than men.7 This enzyme plays a crucial role in determining drug concentrations in the gut and the central nervous system (CNS), largely by functioning as an efflux transporter. In women, antidepressants—which are transported by Pgp out of the CNS and into the circulation or out of the circulation and into the gut—may be more highly concentrated in CNS tissue and plasma because of an attenuated efflux. This could result in a greater response or an increase in AEs.
The CYP450 system is not lacking in gender variances, either. Drugs metabolized by CYP3A4 may clear faster in women, whereas substrates of CYP2D6 may clear faster in men.5,19 Citalopram concentrations are higher in women than in men, possibly owing to these factors or to differences in hepatic blood flow. There also may be disparities in enzymatic activity in glucuronidation and other pathways.7 The clinical significance of these parameters is undetermined.
OTHER CONSIDERATIONS
Also to be considered in the appropriate treatment of depression in women are the risk of osteoporosis with antidepressant use and possible interactions with tamoxifen. SSRIs have been linked to decreased bone mineral density (BMD), although the magnitude and clinical significance remain unclear. One cohort study followed nearly 3,000 women for 5 years to assess whether certain antidepressants reduced BMD. Subjects were categorized as those taking TCAs, those taking SSRIs, and nonusers of these classes. Subjects taking SSRIs, but not those taking TCAs, had a significant reduction in hip BMD compared with nonusers.20 This is of particular concern given that antidepressant use may predispose patients, particularly elderly ones, to falls and subsequent fractures.21,22
Tamoxifen, a selective ER modulator, is a neoplastic agent often used to treat ER-positive breast cancer. This agent is considered a prodrug; the metabolites produced from various enzymes, including CYP2D6, have much higher activity at ERs than the parent compound does. Accordingly, patients with decreased CYP2D6 activity induced by genetic variability or concurrent drug therapy may be at risk for reduced tamoxifen effectiveness.23 Some antidepressants, including paroxetine, fluoxetine, and duloxetine, are known to inhibit CYP2D6. Whether these interactions produce significantly worse outcomes is unknown, since studies have been inconsistent. If it is desirable to avoid this interaction, an antidepressant with little CYP2D6 inhibition (e.g., venlafaxine, desvenlafaxine, mirtazapine) should be used.23
CONCLUSION
Women are disproportionately affected by depression. They are more likely than men to be diagnosed, and depression in women may manifest with earlier, more severe episodes that may involve a greater incidence of suicidality. Although the reasons for this are unclear, it is evident that women may present differently and may perhaps respond uniquely to certain classes of drugs versus others. More information is necessary before gender can play a large role in guiding pharmacotherapy for depression; however, clinicians must always consider gender along with many other individual factors when determining the most appropriate medication regimen.
REFERENCES
1. Patten SB. Accumulation of major depressive episodes over time in a
prospective study indicates that retrospectively assessed lifetime
prevalence estimates are too low. BMC Psychiatry. 2009;9:19.
2. Keers R, Atchison KJ. Gender differences in antidepressant drug response. Int Rev Psychiatry. 2010;22:488-500.
3. Morbidity and Mortality Weekly Report (MMWR). QuickStats:
prevalence of current depression among persons aged ≥12 years, by age
group and sex—United States, National Health and Nutrition Examination
Survey, 2007-2010. 2012;60:1747.
www.cdc.gov/mmwr/preview/mmwrhtml/mm6051a7.htm. Accessed July 30, 2013.
4. Farr SL, Dietz PM, Williams JR, et al. Depression screening and
treatment among nonpregnant women of reproductive age in the United
States, 1990-2010. Prev Chronic Dis. 2011;8:A122.
5. Sramek JJ, Cutler NR. The impact of gender on antidepressants. Curr Top Behav Neurosci. 2011;8:231-249.
6. Ryan J, Ancelin ML. Polymorphisms of estrogen receptors and risk of depression: therapeutic implications. Drugs. 2012;72:1725-1738.
7. Bigos KL, Pollock BG, Stankevich BA, Bies RR. Sex differences in
the pharmacokinetics and pharmacodynamics of antidepressants: an updated
review. Gend Med. 2009;6:522-543.
8. Dalla C, Pitychoutis PM, Kokras N, Papadopoulou-Daifoti Z. Sex
differences in animal models of depression and antidepressant response. Basic Clin Pharmacol Toxicol. 2010;106:226-233.
9. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders (4th ed, text rev). Washington, DC: American Psychiatric Association; 2000.
10. Marcus SM, Young EA, Kerber KB, et al. Gender differences in depression: findings from the STAR*D study. J Affect Disord. 2005;87:141-150.
11. Posternak MA, Zimmerman M. Symptoms of atypical depression. Psychiatry Res. 2001;104:175-181.
12. Baca E, Garcia-Garcia M, Porras-Chavarino A. Gender differences
in treatment response to sertraline versus imipramine in patients with
nonmelancholic depressive disorders. Prog Neuropsychopharmacol Biol Psychiatry. 2004;28:57-65.
13. Trivedi MH, Rush AJ, Wisniewski SR, et al. Evaluation of outcomes
with citalopram for depression using measurement-based care in STAR*D:
implications for clinical practice. Am J Psychiatry. 2006;163:28-40.
14. Khan A, Brodhead AE, Schwartz KA, et al. Sex differences in
antidepressant response in recent antidepressant clinical trials. J Clin Psychopharmacol. 2005;25:318-324.
15. Thiels C, Linden M, Grieger F, Leonard J. Gender differences in
routine treatment of depressed outpatients with the selective serotonin
reuptake inhibitor sertraline. Int Clin Psychopharmacol. 2005;20:1-7.
16. Yang SJ, Kim SY, Stewart R, et al. Gender differences in 12-week
antidepressant treatment outcomes for a naturalistic secondary care
cohort: the CRESCEND study. Psychiatry Res. 2011;189:82-90.
17. Quitkin FM, Stewart JW, McGrath PJ, et al. Columbia atypical
depression. A subgroup of depressives with better response to MAOI than
to tricyclic antidepressants or placebo. Br J Psychiatry Suppl. 1993;21:30-34.
18. Crismon ML, Trivedi M, Pigott TA, et al. The Texas Medication
Algorithm Project: report of the Texas Consensus Conference Panel on
Medication Treatment of Major Depressive Disorder. J Clin Psychiatry. 1999;60:142-156.
19. Meibohm B, Beierle I, Derendorf H. How important are gender differences in pharmacokinetics? Clin Pharmacokinet. 2002;41:329-342.
20. Diem SJ, Blackwell TL, Stone KL, et al. Use of antidepressants
and rates of hip bone loss in older women: the study of osteoporotic
fractures. Arch Intern Med. 2007;167:1240-1245.
21. Richards JB, Papaioannou A, Adachi JD, et al. Effect of selective serotonin reuptake inhibitors on the risk of fracture. Arch Intern Med. 2007;167:188-194.
22. Hegeman J, van den Bemt B, Weerdesteyn V, et al. Unraveling the
association between SSRI use and falls: an experimental study of risk
factors for accidental falls in long term paroxetine users. Clin Neuropharmacol. 2011;34:210-215.
23. Breitbart W. Do antidepressants reduce the effectiveness of tamoxifen? Psychooncology. 2011;20:1-4.
To comment on this article, contact rdavidson@uspharmacist.com.





