US Pharm. 2019:44(12):HS-2-HS-9.
Abstract: Acute appendicitis is the most common abdominal emergency, with a lifetime risk of 7% to 8%. Clinical features vary but typically include right lower-quadrant abdominal pain, anorexia, nausea, and vomiting. Although there are many theorized etiologies, appendicitis is thought to occur primarily as a result of luminal obstruction that has progressed to inflammation, ischemia, and possibly perforation. Treatment is usually by appendectomy after appropriate fluid resuscitation, analgesia, and antibiotics. Emerging evidence suggests an antibiotic-treatment approach may be an alternative to surgery.
Acute appendicitis is one of the most common causes of acute abdominal pain requiring emergent surgery. The overall estimated lifetime risk is 7% to 8% with a slight predominance in Caucasian males.1,2 While no age is exempt, acute appendicitis commonly affects those aged 10 to 20 years.3 It is characterized by a wide range of symptoms that overlap with other gastroenterological, gynecologic, or urologic conditions, such as peptic ulcer disease, Meckel’s diverticulum, Crohn’s disease, gastroenteritis, irritable bowel disease, ectopic pregnancy, endometriosis, testicular or ovarian torsion, pelvic inflammatory disease, urinary tract infection, and renal stones.3
Most patients suffering from acute appendicitis will experience a typical migratory periumbilical pain, which intensifies in the first 24 hours. This eventually localizes to right lower quadrant abdominal pain, anorexia, nausea, and vomiting.2,4 Other nonspecific symptoms include general malaise, indigestion, diarrhea, and flatulence. A mild leukocytosis (white blood cell count >10,000 cells/microL), a slight hyperbilirubinemia (total bilirubin >1.0 mg/dL), and a low-grade fever (101.0°F) are additional findings that may be observed during acute appendicitis.5 Signs and symptoms usually correlate with the timing of disease onset (TABLE 1). Since symptoms may vary, imaging studies with CT (preferred), US, and MRI may be performed to increase the specificity of the diagnosis and help rule out perforation.
Despite being so common, the exact etiology of appendicitis is unknown.2 There are several proposed etiologies, yet they are all poorly understood.6 Most evidence suggests that the primary etiology is likely due to an obstruction of the appendiceal lumen secondary to a fecalith, calculi, hypertrophied lymphatic tissue, an infectious process, or a neoplasm.2,7 When obstruction occurs, gut bacteria will build up in the appendix causing acute inflammation, thrombosis, and localized ischemia. If significant enough, the appendix may rupture, leading then to localized abscess formation and generalized peritonitis.8 While timing of perforation varies, one study reported 65% of patients who had a perforated appendix had symptoms for longer than 48 hours.9 There is a possible genetic link supported by evidence to suggest that patients with a positive family history experience appendicitis at a three-times higher rate.10 Lastly, environmental factors have also been established in the development of appendicitis, with a largely seasonal presentation during the summer months.11
Because of the variability in the clinical presentation, making a diagnosis and selecting a management approach for a patient with acute appendicitis can be challenging. A variety of validated scoring tools have been developed that incorporate findings from the patient’s presentation and laboratory markers.12-15 Although the Alvarado Score System is the most common and widely applied diagnostic validating system, the Appendicitis Inflammatory Response (AIR) score is a newer, more commonly used tool (TABLE 2). These aids stratify patients as low, moderate, or high risk, assisting clinicians in making a decision on appropriate management.
Surgical removal of the appendix, via open laparotomy or laparoscopy, is the standard of therapy for acute appendicitis.16 Initial antibiotic therapy may precede surgery for some. More recent evidence suggests antibiotics may be used as the sole therapy in those with uncomplicated appendicitis, thus avoiding surgery. Additionally, pain control is an important part of care in patients with acute appendicitis. This article briefly reviews the current evidence-based therapeutic management of acute appendicitis in the adult population.
THERAPEUTIC APPROACHES
Surgery
Traditionally, the gold-standard curative therapeutic approach for acute appendicitis is IV cystalloid fluids along with source control via an appendectomy, using either an open laparotomy or laparoscopy.16 A recent meta-analysis consisting of 33 studies and over 3,600 patients compared both surgical techniques.17 Those who underwent a laparoscopic appendectomy had a longer operation time but experienced a lower incidence of wound infection, fewer postoperative complications, shorter length of stay, and a faster return to activity.17 Thus, the laparoscopic surgical approach is recommended. For those who develop an appendiceal abscess, percutaneous drainage may be required.18
Antibiotics
The obstructed appendix leads to bacterial overgrowth. Aerobic organisms predominate in early appendicitis, and mixed aerobes and anaerobes are seen later in the course. Anaerobic organisms that may be found include Bacteroides fragilis, Clostridium species (spp), and Prevotella spp, while aerobic, gram-negative bacilli found may include Escherichia coli, Klebsiella spp, and Proteus mirabilis.8,19 Pseudomonas aeruginosa, streptococci, enterococci, and mixtures of aerobes and anaerobes should also be considered when empirically selecting an antimicrobial regimen.8,19 Several treatment guidelines exist that offer therapeutic recommendations. The most recent guidelines by the Surgical Infection Society and Infectious Diseases Society of America were published in 2010.19 Due to emerging evidence, a revised guideline on the management of intra-abdominal infections was published in 2017 by the Surgical Infection Society.20 Updated guidelines are expected to be published in the fall of 2020.
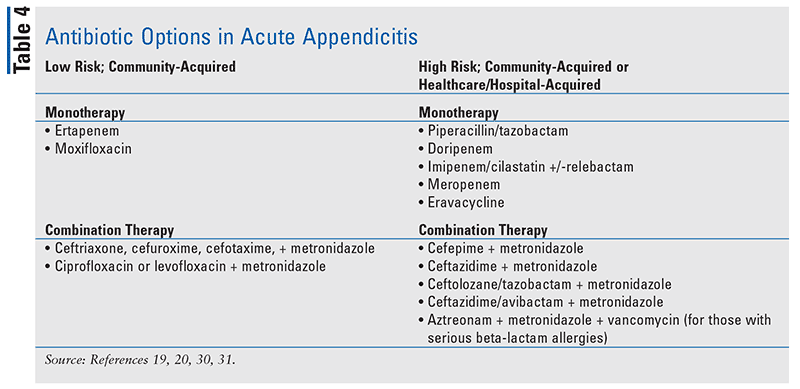
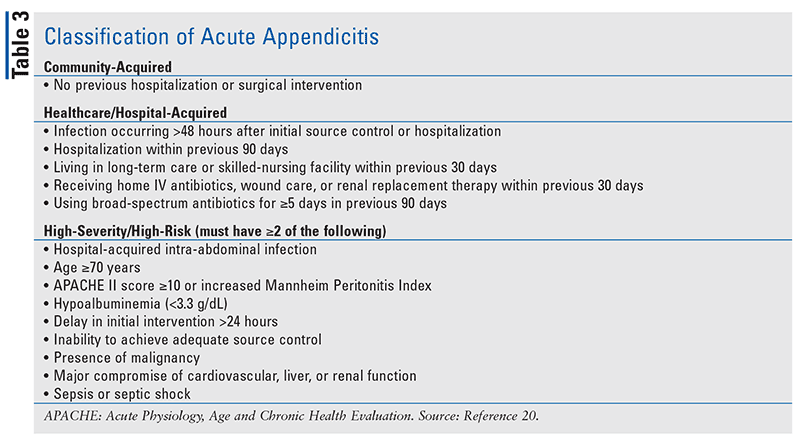
Patients may be classified as having uncomplicated or complicated appendicitis. Uncomplicated appendicitis is defined as an infection confined within the visceral organ. However, if the infection proceeds beyond the organ (e.g., ruptures), it is considered to be complicated appendicitis. Furthermore, patients may be categorized as having community-acquired or healthcare/hospital-associated infection as well as being at low or high risk for treatment failure or death (TABLE 3). Guidelines recommend that empiric antimicrobial selection and dosing be based upon the classification, the patient’s comorbidities, physiologic conditions, and the risk of adverse outcomes (TABLE 4).20 Standard antibiotic dosing should be used in lower-risk patients who are not obese and have normal renal or hepatic function, while higher doses of antimicrobials should be used in higher-risk patients.20 For patients needing antifungal therapy, fluconazole is recommended for susceptible strains of Candida albicans while voriconazole should be considered for nonsusceptible strains of Candida.20 In severely ill patients, an echinocandin should be used.20
For some with uncomplicated appendicitis, evidence suggests antibiotic therapy alone may be sufficient instead of proceeding to surgery.21-23 The single-cohort, prospective, observational NOTA Study (Non Operative Treatment for Acute Appendicitis) evaluated the outcomes of patients (n = 159) with suspected appendicitis (mean AIR score 4.9) treated nonoperatively with a 7-day course of amoxicillin/clavulanic acid.22 The follow-up period was 2 years. Results showed that for patients who successfully completed antibiotic therapy, the 2-year efficacy was 83% (118 patients recurrence-free and 14 patients with recurrence nonoperatively managed), and the recurrence rate was 13.8%.22
Most recently, the Appendicitis Acuta (APPAC) trial (Antibiotic Therapy vs Appendectomy for Treatment of Uncomplicated Acute Appendicitis) randomized more than 500 patients with uncomplicated appendicitis to early appendectomy or antibiotic treatment alone.23 Patients in the antibiotic arm of the study received IV ertapenem (1 g daily) for 3 days followed by 7 days of oral levofloxacin (500 mg, once daily) and metronidazole (500 mg, 3 times daily).23 The primary outcome was resolution of appendicitis without the need for surgical intervention and no recurrence for one year. At study end, 99.6% of those in the appendectomy group had a successful appendectomy with an overall complication rate of 20.5%; 27.3% of those in the antibiotic group needed an appendectomy, with an overall complication rate of 7%.23 Thus, the study did not meet noninferiority criteria when compared with appendectomy. Limitations acknowledged by the authors included small sample size, thereby underpowering the study, and a short follow-up period. The investigators also completed a 5-year follow-up of patients included in the APPAC trial.24 At the 5-year mark, late recurrent appendicitis and complication rates were assessed. Appendicitis had recurred in 39% of patients in the antibiotic group, and the overall complication rate was 24% in the appendectomy group compared with 7% for those randomized to antibiotics.24 The authors concluded that for some a nonoperative treatment approach might be reasonable.24
The appropriate duration of antibiotic therapy has been debated, and it is dependent on the clinical scenerio. Results from the Study to Optimize Peritoneal Infection Therapy (STOP-IT) trial determined there was no difference between 3 to 5 days of antibiotic therapy compared with 5 to 10 days.25 Current guidelines suggest postoperative antibiotic therapy continue for 24 to 72 hours.20 In patients who do not undergo source control, 5 to 7 days of therapy are recommended.20 If the patient has no response after 5 to 7 days, the patient should be reassessed for another source-control procedure.20 For patients who have bacteremia, antibiotics may be stopped after 7 days if there is adequate source control and the bacteremia has resolved.20
Analgesics
Given the degree of pain most will experience with acute appendicitis, analgesic therapy should be included in the treatment plan. Historically, administration of analgesics had been discouraged because of concerns that the therapeutic effects might mask appendicitis symptoms. However, data do not support this claim. Several randomized, controlled studies have demonstrated that administering opioid analgesia is safe and does not lead to a diagnostic error.26-28 In those unable to receive opioids, acetaminophen and nonsteroidal anti-inflammatories should be considered for pain management in patients with suspected acute appendicitis.26-28
COMPLICATIONS
While appendicitis therapy is straightforward, complications may still arise. The most concerning complication is perforation of the appendix. This may occur if therapy is delayed. Perforations may lead to peritonitis, which increases morbidity and mortality. A study of more than 4,000 patients revealed that perforation increases postsurgical morbidity from 16.3% to 24.9% and mortality from 1.8% to 4.0%.29 Prompt treatment of appendicitis, whether operative or nonoperative, is crucial in reducing further complications.
CONCLUSION
Acute appendicitis is a common abdominal emergency requiring immediate attention. Pharmacists are in a position to quickly identify and refer patients who may be affected with this condition. Furthermore, pharmacists have the opportunity to be an integral part of the healthcare team and can assist in appropriate selection and dosing of antibiotic and analgesic regimens for these patients. While a laparoscopic appendectomy is considered the standard of treatment for appendicitis, emerging evidence suggests antibiotic regimens alone may also be effective.
REFERENCES
1. Stewart B, Khanduri P, McCord C, et al. Global disease burden of conditions requiring emergency surgery. Br J Surg. 2014;101(1):e9-e22.
2. Humes DJ, Simpson J. Acute appendicitis. BMJ. 2006;333(7567):530-534.
3. Jacobs DO. Acute appendicitis and peritonitis. In: Jameson J, Fauci AS, Kasper DL, et al, eds. Harrison’s Principles of Internal Medicine, 20th ed. New York, NY: McGraw-Hill; 2018:2298-2302.
4. Laurell H, Hansson LE, Gunnarsson U. Manifestations of acute appendicitis: a prospective study on acute abdominal pain. Dig Surg. 2013;30:198-206.
5. Tehrani HY, Petros JG, Kumar RR, Chu Q. Markers of severe appendicitis. Am Surg. 1999;65:453-455.
6. Carr NJ. The pathology of acute appendicitis. Ann Diagn Pathol. 2000;4:46-58.
7. Bhangu A, Soreide K, Di Saverio S, et al. Acute appendicitis: modern understanding of pathogenesis, diagnosis, and management. Lancet. 2015;386:1278-1287.
8. Hamilton AL, Kamm MA, Ng SC, Morrison M. Proteus spp. as putative gastrointestinal pathogens. Clin Microbiol Rev. 2018;31(3):e00085-17.
9. Temple CL, Huchcroft SA, Temple WJ. The natural history of appendicitis in adults: a prospective study. Ann Surg. 1995;221(3):278-281.
10. Ergul E. Heredity and familial tendency of acute appendicitis. Scand J Surg. 2007;96:290-292.
11. Wei PL, Chen CS, Keller JJ, Lin HC. Monthly variation in acute appendicitis incidence: a 10-year nationwide population-based study. J Surg Res. 2012;178:670-676.
12. Ebell MH, Shinholser J. What are the most clinically useful cutoffs for the Alvarado and Pediatric Appendicitis scores? A systematic review. Ann Emerg Med. 2014;64(4):365-372.e2.
13. Kollár D, McCartan DP, Bourke M, et al. Predicting acute appendicitis? A comparison of the Alvarado score, the Appendicitis Inflammatory Response score and clinical assessment [published correction appears in World J Surg. 2015;39(1):112]. World J Surg. 2015;39(1):104-109.
14. Pogorelic Z, Rak S, Mrklic I, Juric I. Prospective validation of Alvarado score and Pediatric Appendicitis Score for the diagnosis of acute appendicitis in children. Pediatr Emerg Care. 2015;31(3):164-168.
15. Scott AJ, Mason SE, Arunakirinathan M, et al. Risk stratification by the Appendicitis Inflammatory Response score to guide decision-making in patients with suspected appendicitis. Br J Surg. 2015;102(5):563-572.
16. Jaschinski T, Mosch C, Eikermann M, et al. Laparoscopic versus open appendectomy in patients with suspected appendicitis: a systematic review of meta-analyses of randomised controlled trials. BMC Gastroenterol. 2015;15:48.
17. Dai L, Shuai J. Laparoscopic versus open appendectomy in adults and children: a meta-analysis of randomized controlled trials. United European Gastroenterol J. 2017;5(4):542-553.
18. Marin D, Ho LM, Barnhart H, et al. Percutaneous abscess drainage in patients with perforated acute appendicitis: effectiveness, safety, and prediction of outcome. AJR Am J Roentgenol. 2010;194:422-429.
19. Solomkin JS, Mazuski JE, Bradley JS, et al. Diagnosis and management of complicated intra-abdominal infection in adults and children: guidelines by the Surgical Infection Society and the Infectious Diseases Society of America. Clin Infect Dis. 2010;50:133-164.
20. Mazuski JE, Tessier JM, May AK, et al. The Surgical Infection Society Revised Guidelines on the Management of Intra-Abdominal Infection. Surg Infect (Larchmt). 2017;18(1):1-76.
21. Mason RJ, Moazzez A, Sohn H, Katkhouda N. Meta-analysis of randomized trials comparing antibiotic therapy with appendectomy for acute uncomplicated (no abscess or phlegmon) appendicitis. Surg Infect (Larchmt). 2012;13(2):74-84.
22. Di Saverio S, Sibilio A, Giorgini E, et al. The NOTA Study (Non Operative Treatment for Acute Appendicitis): prospective study on the efficacy and safety of antibiotics (amoxicillin and clavulanic acid) for treating patients with right lower quadrant abdominal pain and long-term follow-up of conservatively treated suspected appendicitis. Ann Surg. 2014;260(1):109-117.
23. Salminen P, Paajanen H, Rautio T, et al. Antibiotic therapy vs appendectomy for treatment of uncomplicated acute appendicitis: the APPAC randomized clinical trial. JAMA. 2015;313(23):2340-2348.
24. Salminen P, Tuominen R, Paajanen H, et al. Five-year follow-up of antibiotic therapy for uncomplicated acute appendicitis in the APPAC randomized clinical trial. JAMA. 2018;320(12):1259-1265.
25. Sawyer RG, Claridge JA, Nathens AB, et al. Trial of short-course antimicrobial therapy for intraabdominal infection. N Engl J Med. 2015;372:1996-2005.
26. Ranji SR, Goldman LE, Simel DL, Shojania KG. Do opiates affect the clinical evaluation of patients with acute abdominal pain? JAMA. 2006;296(14):1764-1774.
27. Mousavi SM, Paydar S, Tahmasebi S, Ghahramani L. The effects of intravenous acetaminophen on pain and clinical findings of patients with acute appendicitis; a randomized clinical trial. Bull Emerg Trauma. 2014;2(1):22-26.
28. Manterola C, Vial M, Moraga J, Astudillo P. Analgesia in patients with acute abdominal pain. Cochrane Database Syst Rev. 2011;(1):CD005660.
29. Margenthaler JA, Longo WE, Virgo KS, et al. Risk factors for adverse outcomes after the surgical treatment of appendicitis in adults. Ann Surg. 2003;238(1):59-66.
30. Solomkin J, Evans D, Slepavicius A, et al. Assessing the efficacy and safety of eravacycline vs ertapenem in complicated intra-abdominal infections in the Investigating Gram-Negative Infections Treated with Eravacycline (IGNITE 1) trial: a randomized clinical trial. JAMA Surg. 2017;152(3):224-232.
31. FDA. FDA approves new treatment for complicated urinary tract and complicated intra-abdominal infections [news release]. July 17, 2019. www.fda.gov/news-events/press-announcements/fda-approves- new-treatment-complicated-urinary-tract-and-complicated intra-abdominal infections. Accessed August 31, 2019.
To comment on this article, contact rdavidson@uspharmacist.com.