U.S. Pharm. 2011;36(1):20-24
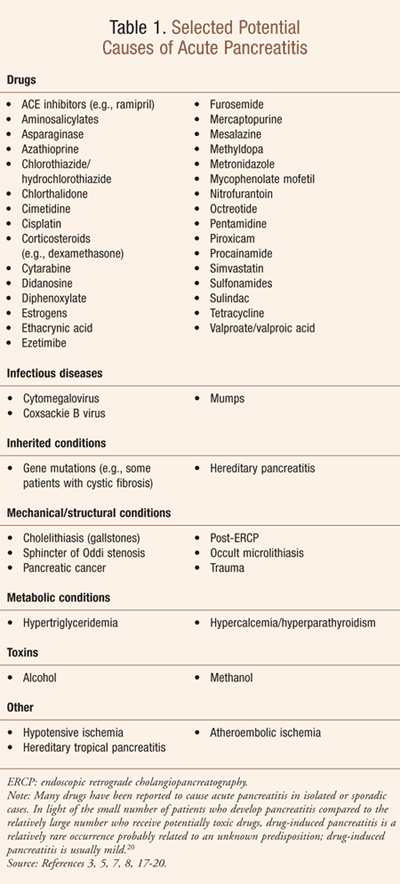
Inflammation of the pancreas, known as pancreatitis, may be acute or chronic. It may pre-sent as a single episode, recurring attacks, or chronic pain.1 While acute pancreatitis (AP) and chronic pancreatitis (CP) can be caused by similar etiologies, they tend to follow distinct courses.2AP is an acute inflammatory process of the pancreas that may involve other regional tissues or remote organs.3,4 The range of disease is from self-limiting to fatal, with an incidence and mortality rate that increases with age.5,6 While there are multiple etiologies for AP (Table 1), approximately 80% of cases manifest secondary to gallstone disease and alcohol abuse.2 Patients with inflammatory bowel disease (IBD) seem to be at increased risk for AP.7 In the elderly, AP is most commonly caused by gallstones and results in a higher incidence of organ failure and death.8 Factors associated with mortality in AP are advanced age, alcohol use, and diabetes, whereas female gender, employment, and co-living were associated with better survival.9 The patient with AP usually seeks urgent medical attention for the sudden onset of severe pain of the upper abdomen that radiates to the back.2 The onset of pain may be related to a recent rich, fatty meal or an alcohol binge.2
When death secondary to AP occurs within the first several days, it is usually attributed to cardiovascular instability or respiratory failure; death after the first week is usually attributed to infection of the pancreas or rupture of a pseudocyst.3 Death secondary to heart failure may occasionally occur.3
AP can progress to CP. Although approximately 80% of CP etiologies are alcohol related, Nøjgaard indicates that AP can progress to CP not only from alcoholic but also from idiopathic AP within a mean interval of 3.5 years.9,10 While both alcohol consumption and smoking are risk factors for transitioning from AP to CP, Nøjgaard et al found smoking to be the strongest risk factor associated with progression.11,12 Patients with CP can experience a flare-up of AP.3 Onset of CP usually occurs in the fourth decade, is more common in men, and is rare in those over the age of 65 years.13 In contrast, most patients with pancreatic cancer (87%) are older than 55 years at diagnosis, with the median age being 72.5 Adenocarcinoma of the pancreas, a malignant tumor with a poor prognosis, accounts for 90% of all tumors of the pancreas.8
Signs and Symptoms of AP
Nausea and vomiting are common in AP. In gallstone pancreatitis, pain develops suddenly; in alcoholic pancreatitis, pain develops over a few days.3 The AP attack causes exquisite abdominal tenderness and boring upper abdominal pain that is steady and typically severe enough to require high dosages of parenteral opioids; tachycardia may also be noted.2,3 If the patient has an elevated temperature and white blood cell count, along with a toxic appearance, it should be suspected that an infection in the pancreas or adjacent fluid collection is present; infection may also be the culprit if deterioration occurs following an initial course of stabilization.3
Of note, a new diagnosis of diabetes mellitus in an elderly individual should alert a clinician to consider the presence of an underlying pancreatic cancer, especially if the patient has other suggestive symptoms.8 The clinical presentation of adenocarcinoma includes epigastric or back pain, anorexia, weight loss, and obstructive jaundice.8
Diagnosis
Whenever severe abdominal pain occurs, particularly in an individual with gallstones or significant alcohol use, pancreatitis is suspected.3 Diagnosis is based on clinical presentation and serum amylase (elevated on day 1 and returning to normal in 3-7 days) and lipase levels (more specific for pancreatitis).3 A spectrum of additional laboratory tests typically includes CBC, glucose, blood urea nitrogen, creatinine, electrolytes, calcium, and magnesium.3 The differential diagnosis includes conditions such as perforated gastric or duodenal ulcer, diverticulitis, appendicitis, intestinal obstruction, dissecting aneurysm, and biliary colic, among others.3
Since the level of serum amylase has been found to have no impact on AP mortality, Nøjgaard recommends that in the future, when diagnosing AP, a focus be placed more on the elimination of differential diagnoses than on the level of serum amylase.9 For further discussion of diagnostic testing for AP and CP, refer to online Reference 3.
Treatment of Acute Pancreatitis
Fluid resuscitation (e.g., 6-8 L/day) is essential in the management of AP; inadequate fluid replacement increases the risk of pancreatic necrosis.3 Until acute inflammation subsides (i.e., resolution of abdominal tenderness and pain, serum amylase within normal limits, return of appetite, overall feeling of well-being), fasting is indicated; in severe cases, total parenteral nutrition may be necessary in the first few days to prevent malnutrition.3 Parenteral opioids are necessary to relieve pain, while antiemetic agents (e.g., prochlorperazine IV) relieve vomiting.3 If vomiting is significant and persistent, a nasogastric tube is required. H2 blockers and proton pump inhibitors are administered parenterally; there is no proven benefit to the administration of drugs (e.g., anticholinergics, glucagon, somatostatin, octreotide) to reduce pancreatic secretions.3
The patient with severe AP should be placed in the ICU. Complications such as hypoxia, heart failure, and prerenal azotemia require specialized treatment. Renal failure may require dialysis, usually peritoneal dialysis.3 While infected pancreatic necrosis requires sectional surgical debridement, prevention of infection of sterile pancreatic necrosis requires antibiotic prophylaxis.3 Percutaneous drainage is used to remove infected fluid that collects outside the pancreas; however, there is no proven benefit to peritoneal lavage.3 In cases of uncontrolled biliary sepsis or certain severe types of trauma, surgery early in the course is justified.3
Most patients with gallstone pancreatitis (>80%) pass the stone spontaneously; for those in whom improvement is not seen subsequent to 24 hours of treatment, surgical stone removal is indicated.3 Elective cholecystectomy, performed laparoscopically, usually follows in patients who have spontaneously improved.3
Nøjgaard indicates that since AP and CP are multifaceted and there is high mortality in progressive AP, patients with risk factors for CP should be followed up, and treatment for smoking dependency and alcohol dependency, together with social and nutritional support, is encouraged.9
Drug-Induced Pancreatitis
Drug-induced AP is considered to be a rare diagnosis, as it is often a challenge to establish the diagnosis accurately.7,14 There are no unique clinical characteristics to distinguish drugs from other causes of pancreatitis.15 Although many drugs (Table 1) have been implicated in the etiology of acute pancreatitis, literature is sparse and limited to case reports with regard to the various features of drug-induced pancreatitis, such as patterns of presentation, including the time from initiation to the development of disease (latency).14,16 Few data exist regarding the mechanisms of drug-induced pancreatitis.15
Some medications have been documented to cause acute pancreatitis, backed by a substantial body of evidence (including rechallenge), while others have been noted as a cause merely by a single published case report in which no other cause was found.14 The prevalence of drug-induced acute pancreatitis is unclear and the incidence is, therefore, usually estimated from case reports.7 The overall incidence range is most probably 0.1% to 2% of pancreatitis cases.17According to data from case-control studies, it is suggested that even drugs with concrete evidence for an association with pancreatitis only rarely cause the condition.17 Certain special populations may be at higher risk for drug-induced acute pancreatitis, such as children, women, the elderly, and patients with advanced HIV infection or IBD.15 Although the majority of cases are mild, severe and sometimes fatal cases may occur; therefore, identification of the offending agent is critical.15
While 525 different drugs can induce acute pancreatitis as an adverse reaction, according to a World Health Organization (WHO) database, only 31 drugs have been associated with an established definite causality.17 According to Nitsche et al, epidemiologic data suggest that the risk of pancreatitis is highest for mesalazine, azathioprine, and simvastatin; the authors further note that even when a definite association has been demonstrated, it is often impossible to determine whether the drug or the underlying condition for which the drug was taken has conferred the risk of pancreatitis (e.g., azathioprine for Crohn’s disease or pentamidine for HIV).17 Generally, it is accepted that a cause-and-effect relationship exists when a rechallenge provokes symptoms to recur. According to Nitsche et al, the disease course of drug-induced pancreatitis is usually mild or even subclinical.17
In another recent study, Vinklerová et al found azathioprine to be the most frequent causative factor (three cases in two patients) with all other causative drugs documented only in single cases: mesalazine, dexamethasone, ramipril, mycophenolate mofetil, cytarabine, and valproate.7 The researchers found the diagnosis of drug-induced acute pancreatitis to be underestimated due to difficulties in determining the causative agent; they also noted the need for a retrospective re-evaluation of the suspected causative factors.7 Further, they found the disease to be more probable in younger persons, women, and patients with Crohn’s disease.7
Bermejo et al retrospectively extracted information from the clinical records of patients with IBD. Based on the study, the researchers concluded that not only was the incidence of acute pancreatitis in the IBD patients (1.6%) similar to that previously described, but that drugs, chiefly azathioprine/mercaptopurine (AZA/MP), were the leading cause.18 Bermejo et al also concluded that AZA-induced acute pancreatitis is always mild, and patients with Crohn’s disease are at a higher risk for AZA/MP–associated acute pancreatitis.18 Since they found the frequency of idiopathic acute pancreatitis to be higher than expected, they suggested that a portion of the cases could be extraintestinal manifestations of IBD.18
Management of drug-induced acute pancreatitis involves withdrawal of the offending agent and supportive care; prevention requires a current knowledge of drugs associated with the strongest evidence linking their use to the development of pancreatitis (including proposed mechanisms through which the reaction may be caused).15
Conclusion
Acute pancreatitis is a potentially severe condition that has multiple etiologies. While drug-induced AP is considered to be a rare diagnosis due to challenges in establishing an accurate diagnosis, it should not be overlooked. Since AP results in a higher incidence of organ failure and death in the elderly, understanding the risks, factors associated with mortality, and recommended treatment interventions as they relate to seniors is essential for the delivery of quality care and for better survival.
REFERENCES
1. Kinney TP, Freeman ML. Approach to acute, recurrent, and chronic pancreatitis. Minn Med.
2. Skipworth JR, Shankar A, Pereira SP. Managing acute and chronic pancreatitis. Practitioner. 2010;254(1733):23-27, 2.
3. Acute pancreatitis. Gastrointestinal disorders.Merckmanuals.com. Revised August 2007. www.merckmanuals.com/ 2008;91(6):29-33.
acute_pancreatitis.html. Accessed November 28, 2011.
4. Bradley EL III. A clinically based classification system for acute pancreatitis. Summary of the International Symposium on Acute Pancreatitis, Atlanta, GA, September 11 through 13, 1992. Arch Surg.
5. Rice JC, Barancin C, Benson M, et al. Hepatic, biliary and pancreatic diseases. In: Halter JB, Ouslander JG, Tinetti ME, et al, eds. Hazzard’s Geriatric Medicine and Gerontology. 6th ed. New York, NY: McGraw-Hill; 2009:1063-1073.
6. Yadav D, Lowenfels AB. Trends in the epidemiology of the first attack of acute pancreatitis: a systemic review. Pancreas. 2006;33(4):323-330.
7. Vinklerová I, Procházka M, Procházka V, et al. Incidence, severity, and etiology of drug-induced acute pancreatitis. Dig Dis Sci. 2010;55(10):2977-2981.
8. Beaton C, Puntis MC. The pancreas. In: Fillit HM, Rockwood K, Woodhouse K, eds. Brocklehurst’s Textbook of Geriatric Medicine and Gerontology. 7th ed. Philadelphia, PA: Saunders Elsevier; 2010:626-634.
9. Nøjgaard C. Prognosis of acute and chronic pancreatitis—a 30-year follow-up of a Danish cohort. Dan Med Bull. 2010;57(12):B4228.
10. Ammann RW, Muellhaupt B, Meyenberger C, et al. Alcoholic nonprogressive chronic pancreatitis: prospective long-term study of a large cohort with alcoholic acute pancreatitis.
1993;128(5):586-590.
Pancreas. 1994;9:365-373.
11. Lankisch PG, Breuer N, Bruns A, et al. Natural history of acute pancreatitis: a long-term population-based study. Am J Gastroenterol. 2009;104(11):2797-2805.
12. Nøjgaard C, Becker U, Matzen P, et al. Progression from acute to chronic pancreatitis: prognostic factors, mortality, and natural course. Pancreas. 2011;40(8):1195-1200.
13. Strate T, Yekebas E, Knoefel WT, et al. Pathogenesis and the natural course of chronic pancreatitis. Eur J Gastroenterol Hepatol. 2002;14(9):929-934.
14. Badalov N, Baradarian R, Iswara K, et al. Drug-induced acute pancreatitis: an evidence-based review. Clin Gastroenterol Hepatol. 2007;5(6):648-61; quiz 644.
15. Balani AR, Grendell JH. Drug-induced pancreatitis: incidence, management and prevention. Drug Saf. 2008;31(10):823-837.
16. Dhir R, Brown DK, Olden KW. Drug-induced pancreatitis: a practical review. Drugs Today (Barc). 2007;43(7):499-507.
17. Nitsche CJ, Jamieson N, Lerch MM, et al. Drug induced pancreatitis. Best Pract Res Clin Gastroenterol. 2010;24(2):143-155.
18. Bermejo F, Lopez-Sanroman A, Taxonera C, et al. Acute pancreatitis in inflammatory bowel disease, with special reference to azathioprine-induced pancreatitis. Aliment Pharmacol Ther. 2008;28(5):623-628.
19. Johnson JL, Loomis IB. A case of simva-statin-associated pancreatitis and review of statin-associated pancreatitis. Pharmacotherapy. 2006;26(3):414-422.
20. Khoury G, Deeba S, Talavera F, et al. Emergent management of pancreatitis. Medscape.com. Updated June 9, 2011. http://emedicine.medscape.com/
To comment on this article, contact rdavidson@uspharmacist.com.





