US Pharm.
2008;33(4):22-30.
Approximately 25 percent of
Americans are affected by chronic venous insufficiency.1 Deep vein
thrombosis (DVT) is the second most common vascular problem in the United
States and affects as many as 600,000 people every year.2 Graduated
compression stockings are routinely prescribed for DVT prophylaxis by health
care providers in both hospital and community settings.3
Additionally, published clinical-practice guides consider compression
bandaging to be the standard of care for treating venous leg ulcers.4
Compression, whether from hosiery or from bandages, reduces venous
hypertension by increasing pressure on both superficial veins and deep veins.
Some patients refuse to wear compression hosiery or bandages because of
limited mobility or dexterity, so that lack of compliance becomes a barrier to
prevention. Clinically based evidence lacks uniformity regarding patient
compliance with compression therapy and which device should be used to improve
adherence. Given the large number of citations offering a broad range of
clinical opinions, confusion exists regarding the gold standard for
compression therapy. As such, there is wide variation in the prescribing of
compression hosiery for venous ulceration, prevention of varicose veins, and
DVT prevention. Due to the lack of clear evidence-based guidelines,
pharmacists may find themselves at a disadvantage when asked to assist a
patient or health care provider in choosing a suitable compression stocking.
The foremost object of this
review is to empower the pharmacist with relative knowledge about the purpose
of compression hosiery and its function as a preventative tool and treatment
modality. To achieve this end, the pharmacist must first understand the
anatomy and pathophysiology that can lead to DVT and the development of venous
leg ulceration. In addition, the pharmacist must recognize and appreciate the
different classes of compression hosiery available for treating venous leg
ulcers. Finally, in order to counsel patients about proper use of their
compression hosiery, thereby rendering them more likely to comply, the
pharmacist must learn the rules of measurement for these durable goods, as
well as their utility and how to care for them.
Anatomy and Physiology
Both the anatomy
and normal physiology of the venous circulatory system must be understood by
the pharmacist so that the purpose and function of compression hosiery can be
appreciated. The pressure of the blood entering normally functioning veins is
quite low, and the blood has insufficient energy to return to the heart.
Therefore, all veins in the lower extremities contain valves that ensure
upward flow to the heart (FIGURE 1). Blood is returned to the
heart by intrathoracic pressure caused by active respiration that creates a
suction effect within the veins. Pressure exerted by a series of pumps found
in the foot, calf, and thigh also assist with blood return to the right atrium
of the heart.5-7
Adequate venous return from
the lower extremity requires an intricate network of superficial veins, deep
veins, bicuspid valves, and calf muscles all working together, as illustrated
in FIGURE 1.5-7 Deep leg veins have a larger
diameter, creating greater pressure, and are connected by perforator veins to
the smaller-diameter superficial veins that are under less pressure. These
superficial veins are found immediately beneath the skin in subcutaneous fat,
whereas deep veins lie beneath the deep fascia of the leg and usually are
covered by the muscles of the lower limb. The deep veins that carry blood up
the leg consist of the posterior tibial vein, the anterior tibial vein, and
the peroneal veins that unite to form the popliteal vein, which ultimately
feeds into the femoral vein.5-7 Superficial veins comprise the long
saphenous vein, the short saphenous vein, and a number of superficial
collateral and confluents of the saphenous veins.5-7
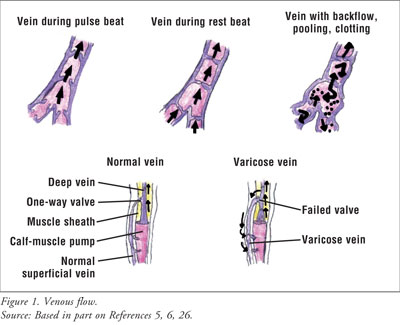
Blood is driven up the lower
extremity by the contracting and relaxing of the calf muscles while in
movement.5 The upward flow of blood to the heart depends on the
integrity of the bicuspid valves.6 When the leg muscles contract,
compression of the deep veins occurs in the calf, thus raising intravenous
pressure and closing the distal valve in the deep vein and the perforating
vein valves, and the blood is propelled up to the heart.5-8 The
cycle of venous blood return continues through relaxation of the calf muscles
that allows the empty deep-vein segments to refill with blood supplied by the
superficial veins.5-7
DVT Pathogenesis and Venous
Leg Ulcers
Deep vein
thrombosis is a condition in which a blood clot, or thrombus, forms in a vein
deep within the body. DVT usually involves the formation of a large thrombus
in the deep veins of the lower legs and thighs. In rare instances, DVT can
occur in the axillary area, collar bone, upper arm, abdomen, or pelvic region.
It is a dangerous condition because the thrombus may become dislodged from the
vein and travel through the vein to the lung, where it may get trapped and
block a vessel in the pulmonary vasculature.
Virchow's triad, described in
1856 by Dr. Rudolf Virchow, comprises three conditions that may arise
simultaneously to create an environment in which a patient is at risk for
hypercoagulability and thrombus formation.9,10 The first condition
is venous stasis, defined as reduced or stagnant blood flow in deep veins that
occurs after long periods of standing or prolonged compression of the back of
the leg while sitting.7,9,10 The second condition is blood
vesselñwall injury resulting in nonfunctioning valves within superficial veins.
7,9,10 Factors that may cause valvular dysfunction include previous
episodes of DVT, increased age, and occupations that require long periods of
standing.7,9,10 The third condition is viscous blood or
hypercoagulability, defined as an increase in the activity of substances in
the blood that are part of the normal clotting mechanism.7,9,10
Scenarios that may facilitate Virchow's triad include immobilization (such as
lying in bed following surgery), surgical procedure, major trauma, increased
age, malignancy, heart failure, diabetes, smoking, obesity, pregnancy, and the
use of oral contraceptives.10
Venous leg ulcers often begin
with an episode of thrombosis in the leg. Wounds caused by venous
insufficiency heal slowly and often recur. Venous leg ulcers are the result of
abnormal mechanisms within the venous system of the leg and most commonly
present between the foot and the upper calf. Valvular incompetence of the
one-way valves in the perforator veins between the superficial and the deep
veins creates venous hypertension that cannot be overcome by the calf-muscle
pump. A rise in venous pressures and subsequent venous stasis lead to more
permeability of capillaries, which allows proteins to leak out of the vascular
bed into the surrounding tissues. Subsequently fibrinogen is activated,
coating the capillaries with fibrin and interfering with the exchange of
oxygen and nutrients. Tissue breakdown is almost inevitable, and
venous ulceration occurs.11-20
In an article published in
1917, Dr. John Homans introduced the term postphlebitic syndrome and
offered insight into the mechanism of venous ulceration.19,20
Homans stated that overstretching of venous walls and destruction of the
valves upon which the mechanism principally depends brought about a degree of
surface stasis that obviously interfered with the nutrition of the skin and
subcutaneous tissue.19,20 Unfortunately, the etiology of venous leg
ulcers is rather more complex than this theory of stagnation and
hypo-oxygenation.15
There are several theories
describing the pathophysiology and mechanisms by which venous hypertension
leads to dermal disruption and ulceration.11-18 The three theories
described in the medical literature are† the fibrin cuff theory, the white
cellñtrapping theory, and the trap hypothesis.11-18 Fibrin
cuffs, which are deposited around the capillaries in lipodermatosclerotic
limbs, may serve as barriers to the diffusion of oxygen, leading to local
ischemia and epidermal necrosis.11,15 The fibrin cuff theory
suggests that sustained venous hypertension causes distention of capillary
beds, allowing fibrin to escape through the capillary wall and leading to a
pericapillary fibrin cuff.11,13,15 This cuff prevents oxygen and
nutrients from reaching the tissue and metabolic wastes from being carried
away. Another study identified the fibrin around the capillaries but suggested
that this does not interfere with healing.11,13,15 According to the
white cellñtrapping theory, neutrophils aggregate in the capillaries, causing
lipodermatosclerosis.12,14,15 Trapped leukocytes in the
microcirculation alter capillary permeability by releasing various
inflammatory mediators that hasten the flow of fibrinogen across the capillary
membrane and promote the formation of fibrin cuffs.15 This theory
suggests that reduced capillary flow rate stimulates leukocyte adherence,
which releases by-products of the white-cell and endothelial-cell interaction:
proteolytic enzymes, oxygen free radicals, and lipids.15,16 The
white cells damage the cell wall, increasing its permeability, and large
molecules are released from the capillaries.14-16 The trap
hypothesis proposes that macromolecules such as fibrin leak out and trap
substances that are needed for normal tissue function and healing.14
When venous insufficiency goes untreated, whether in the deep or the
superficial venous system, it can lead to leg pain, swelling, characteristic
skin changes, and the eventual formation of ulcers.14
Compression Hosiery
Compared with
intermittent-compression devices, compression hosiery is less expensive and
simpler to use and thus remains the most popular method of DVT prophylaxis in
the community setting. The successful application of compression therapy to
manage leg ulceration has been documented since Hippocrates' day.21
Compression therapy is essential to venous ulcer healing and prevention of
recurrence.
Compression therapy consists
of the application of sustained external pressure to the affected lower
extremity, reducing edema and improving venous blood return to the heart.
Graduated, or gradient, compression socks or stockings deliver pressure at the
ankle that gradually decreases as it extends up the leg. Application of a
graduated compression garment reduces blood pooling in the legs and helps
prevent DVT. The physiological effects of graduated compression include
increased blood-flow velocity in deep veins, increases in prostacyclin
production and local capillary clearance, increased transcutaneous oxygen
pressure, and increased release of plasminogen activator.5 Other
physiological effects include decreased edema, decreases in venous capacity
and pressure, and decreases in ambulatory venous pressure.5
The level of compression
required depends on the severity of the chronic venous insufficiency. Two main
groups of patients needful of compression hosiery can be identified: those who
need hosiery for preventive reasons and those who need it for treatment.
3,22 Compression stockings are designed to give graduated compression,
with 18 mmHg at the ankle and 8 mmHg at the knee. This amount of graduated
pressure has been shown to produce the maximum increase in velocity of venous
flow to prevent venous stasis in individuals who are not ambulatory.23
Compression stockings are
available with different grades of pressure. The choice of garment and level
of compression are patient-specific. The essential point to consider when
advising about the type of hosiery needed is the amount of compression
required to reverse or control the pathology.3 The worse the venous
condition, the greater-pressure stocking needed, except in the presence of
ischemia, which is a contraindication.3 Necrotic damage caused by
compression hosiery may result from poorly fitted hose. Direct pressure on the
heel because of insensibility, neuropathy, or failure to change position often
enough to minimize local ischemia are examples of local lower-extremity
ischemic trauma in the presence of mixed vascular pathology or diabetic
microangiopathy.3 Selection criteria include the patient's arterial
status and ability to tolerate as well as don the stocking.17
Compression hosiery may still be advisable even in the presence of mixed
vascular pathology or diabetic microangiopathy. The risk of causing tissue
damage must be weighed against the potential benefit of wearing the hosiery.
3
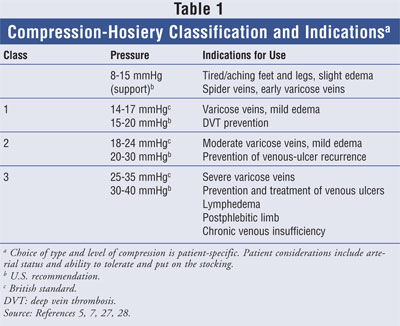
Hosiery options are
categorized based on amount of pressure (in mmHg) and the indication for use (
TABLE 1). There are several types of compression hosiery a physician can
prescribe, including circular knit stockings, flat-bed knit stockings, net
stockings, and one-way stretch stockings.5 Circular knit stockings,
available in nylon and cotton, lack stretch, which makes them difficult to put
on.5 Flat-bed knit hosiery is available in cotton, nylon, and
nylon-plated varieties; they are more flexible than circular knit stockings,
lending to their ease of donning and removal.5 Cotton flat-bed
stockings are the most comfortable, nylon stockings have the least ankle
pressure, and nylon-plated stockings are the most durable.5 Both
net stockings and one-way stretch stockings must be custom-made to a patient's
measurements.5 Compression hosiery comes in thigh-length and
below-the-knee styles; it comes in a choice of colors, and the foot may be
open- toe or closed-toe. For venous insufficiency, there appears to be no
difference between below-the knee and above-the-knee styles.
Pharmacist Interventions for
Compression Hosiery
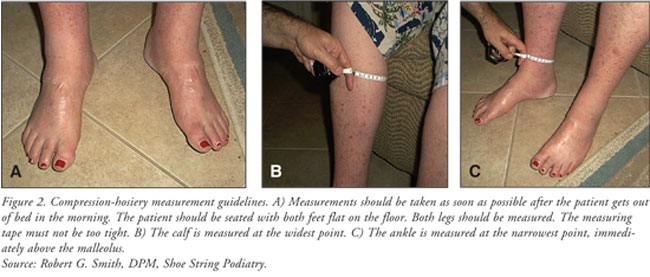
Accurate
measurement of the limb is vital and should be performed by an experienced
professional (podiatrist or other physician, orthotist, or nurse).7
The rules of measurement are provided in FIGURE 2 as a handy
reference. The optimum time for measuring a patient for compression hosiery is
first thing in the morning.7 Incorrect measurements could result in
trauma, discomfort, and possible ulceration.5,24 Ill-fitting
thigh-length stockings may encourage pooling lower in distal portion of the
leg.25 Poorly fitted stockings also can cause pressure necrosis.
7 Too long a stocking can cause the hosiery to roll down, creating a
tourniquet effect.7
Many reasons exist for why
some patients may find it difficult to wear their compression hosiery. These
include age-related issues, like restrictions at the hip, knee, and ankle;
lack of hand strength and dexterity; sensitivity to latex; skin fragility; and
incorrect strength or type of hosiery.3 The pharmacist can be a
valuable resource for teaching patients to apply their own compression
hosiery, thus fostering their independence and enriching their quality of
life. The pharmacist can counsel and instruct patients about the correct
methods of applying and caring for their hosiery. The application technique
and aids for donning compression stockings are presented in TABLE 2.
Suggestions the pharmacist can give to patients to make it easier to don their
stockings include using plastic gloves, moisturizing their legs before
application, or using powder or cornstarch on the leg and regularly trimming
their toenails. The pharmacist should inform patients not to fold their
stockings and to remove all wrinkles. Patients should be advised to remove
their compression stockings at night and to put them on first thing in the
morning.
To extend their life span, the
stockings should be regularly hand-washed at 40C and dried away from direct
heat.5 Finally, the pharmacist should keep in mind that a patient
should be seen a week after the stockings are dispensed to make sure there are
no problems and that the fit is correct. Patients should be seen at
three-month intervals to have their peripheral and arterial blood supply
reassessed and their limbs remeasured. Patients should replace their stockings
every six months.
Conclusion
Some patients
refuse to wear compression hosiery because of a limited degree of mobility or
dexterity or for other reasons, resulting in noncompliance with this mode of
therapy. The information presented in this article should give pharmacists a
solid understanding of the function of compression hosiery so that they can
assist patients achieve greater compliance and have a better quality of life.
Once the pharmacist fully comprehends the benefits of compression hosiery in
the treatment of venous leg ulcers and the prevention of DVT, he or she can
play a vital role in supporting the patient who has been prescribed
compression hosiery.
REFERENCES
1. Beylin M.
Treating venous stasis ulcers in the lower extremity. Podiatry Today.
2004;17:68-74.
2. Tapson VF, Humbert
M. Incidence and prevalence of chronic thromboembolic pulmonary hypertension:
from acute to chronic pulmonary embolism. Proc Am Thorac Soc.
2006;3:564-567.
3. Maylor ME. Accurate
selection of compression and antiembolic hosiery. Br J Nurs.
2001;10:1172-1184.
4. Ennis WJ, Meneses P.
Standard, appropriate, and advance care and medical-legal considerations: part
two--venous ulcerations. Wounds. 2003;15:107-122.
5. Johnson S.
Compression hosiery in the prevention and treatment of venous leg ulcers. J
Tissue Viability. 2002;12:67,70,72-74.
6. Pah-Lavan Z, Hampton
S. JOBST opaque compression hosiery in the management of venous disease. Br
J Nurs. 2004;13:1050-1054.
7. Hampton S. The
purpose and function of compression hosiery. Nurs Residential Care.
2002;4:318-323.
8. Sigel B, Edelstein
AL, Felix WR, Memhardt CR. Compression of the deep venous system of the lower
leg during inactive recumbency. Arch Surg. 1973;106:38-43.
9. Erdman SM, Chuck SK,
Rodvold KA. Thromboembolic disorders. In: DiPiro JT, Talbert RL, Yee GC, et
al, eds. Pharmacotherapy: A Pathophysiological Approach. 4th ed.
Stamford, CT: Appleton & Lange; 1999:295.
10. Smith RG.
Low-molecular-weight heparins: an overview for the podiatric physician. J
Am Podiatr Med Assoc. 2005;95:383-389.
11. Burnand KG,
Whimster I, Naidoo A, Browse NL. Pericapillary fibrin in the ulcer-bearing
skin of the leg: the cause of lipodermatosclerosis and venous ulceration.
Br Med J (Clin Res Ed). 1982:285:1071-1072.
12. Coleridge Smith PD,
Thomas P, Scurr JH, Dormandy JA. Causes of venous ulceration: a new
hypothesis. Br Med J (Clin Res Ed). 1988;296:1726-1727.
13. Falanga V, Kirsner
R, Katz MH, et al. Pericapillary fibrin cuffs in venous ulceration.
Persistence with treatment and during ulcer healing. J Dermatol Surg Oncol
. 1992;18:409-414.
14. Falanga V,
Eaglstein WH. The "trap" hypothesis of venous ulceration. Lancet
. 1993;341:1006-1008.
15. Gourdin FW, Smith
JG. Etiology of venous ulceration. South Med J. 1993;86:1142-1146.
16. S·ndor T.
Pathomechanism of chronic venous insufficiency and leg ulcer. Act Physiol
Hung. 2004;91:131-145.
17. Mulder G. Venous
ulcers: clinical considerations for treatment. Podiatr Manage.
2004;23:129-140.
18. Clarke-Moloney M,
Lyons GM, Burke PE, et al. A review of technological approaches to venous
ulceration. Crit Rev Biomed Eng. 2005;33:511-556.
19. Homans J. The
etiology and treatment of varicose ulcer of the leg. Surg Gynecol Obstet
. 1917;24:300-311.
20. Pappas PJ, Duran
WN, Hobson RW II. Pathophysiology of chronic venous insufficiency. In:
Hobson RW II, Wilson SE, Veith FJ, eds. Vascular Surgery: Principles and
Practice. 3rd ed. New York, NY: Marcel Dekker, Inc; 2004:973.
21. Negus D. Leg
Ulcers: A Practical Approach to Management. Oxford, England: Butterworth
Heinemann Ltd; 1991:3-10.
22. Stemmer R,
Marescaux J, Furderer C. Compression treatment of the lower extremities
particularly with compression stockings. Dermatologist.
1980;31:355-365.
23. Sigel B, Edelstein
AL, Savitch L, et al. Type of compression for reducing venous stasis. A study
of lower extremities during inactive recumbency. Arch Surg.
1975;110:171-175.
24. Edwards L, Moffatt
C. Tissue viability. The use of compression hosiery in the care of leg ulcers.
Nurs Stand. 1996;10:53-56.
25. Sparrow RA, Hardy
JG, Fentem PH. Effect of ëantiembolism' compression hosiery on leg blood
volume. Br J Surg. 1995;82:53-59.
26. Ames Walker.
Economy-Class Syndrome. How your veins function.
www.economyclasssyndrome.net/howveinswork.html. Accessed March 24, 2008.
27. Jobst. Facts about
Jobst gradient compression hosiery.
www.economyclasssyndrome.com/resources/productfactsheet.pdf. Accessed August
12, 2007.
28. Ames Walker.
Economy-Class Syndrome. Graduated compression hosieryñtypical use.
www.economyclasssyndrome.net/typicalgchcharts.html. Accessed August 15, 2007.
To comment on this article, contact
rdavidson@jobson.com.





