US Pharm. 2010;35(2):HS8-HS19.
Heart failure (HF) is a common condition affecting approximately 5.7 million people in the United States. It accounts for about 1.1 million hospital admissions annually, and the estimated direct and indirect cost of HF in the U.S. was $37.2 billion in 2009.1 The American College of Cardiology/American Heart Association (ACC/AHA) guidelines define chronic HF as a complex clinical syndrome, resulting from cardiac dysfunction which impairs the ability of the ventricle to fill and eject blood, thereby producing the symptomatic manifestations of HF.2 Acute heart failure (AHF) is defined as a rapid onset of signs and symptoms due to abnormal cardiac function.3 AHF can be caused by a decompensation of chronic HF or can present de novo (i.e., in patients without a history of cardiac dysfunction).3 The management of AHF is complicated by the relative lack of randomized controlled trials and definitive guideline recommendations in comparison to acute myocardial infarction (AMI) and chronic HF.4
Over a three-year period, the Acute Decompensated Heart Failure National Registry (ADHERE) enrolled over 107,000 patients with either a primary or a secondary discharge diagnosis of HF.5 This database demonstrated the mean age of these patients to be 72.4 years (±14); over half were women (52%), and the majority had a comorbid condition of hypertension (73%).5 Three-quarters of the patients had preexisting HF upon admission, thereby classifying them as decompensated HF versus de novo HF. Since this study, the number of patients living with chronic HF has progressively increased.1 Therefore, the issue of acute decompensated HF will continue to be a growing health problem.
This review will discuss the diagnosis and treatment of AHF as directed by the various guidelines that comment on this disease.2,3,6 Additionally, it will define the pharmacist’s role in the management of AHF syndromes, focusing specifically on the impact pharmacists can make in patients hospitalized for AHF.
Recognizing Acute Heart Failure
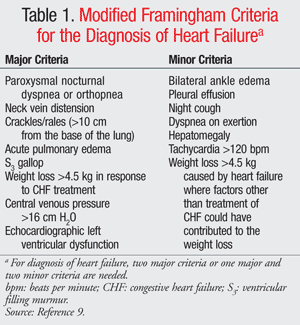
The signs and symptoms of AHF can include dyspnea on exertion (DOE), orthopnea, paroxysmal nocturnal dyspnea (PND), fatigue, edema, weight gain, positive jugular venous distention (JVD), rales, pulmonary edema, tachycardia, ventricular filling murmur (S3), cool extremities, or poor urine output.7,8 The Framingham Heart Failure criteria were developed in the 1970s as a tool to diagnose HF. These criteria can be applied to both acute and chronic HF (TABLE 1).9
Forrester et al developed a classification system for AMI that placed patients into groups based on hemodynamic parameters (cardiac output and pulmonary capillary wedge pressure [PCWP]) and clinical presentation (hypoperfusion or volume overload).10 Later, a comparable classification system was validated in patients with preexisting HF
(Figure 1).11 This classification is used to guide therapy in AHF. Patients classified as “warm and wet” are volume overloaded but perfusing well, and therefore may benefit from diuretic or vasodilator therapy. On the other hand, patients who are “cold and dry” would most likely benefit from volume replacement and/or inotropic therapy.
Other objective measures to assess AHF include B-type natriuretic peptide (BNP) and left ventricular ejection fraction (LVEF). BNP, a cardiac biomarker released from the ventricles in response to wall stretch and volume overload, can be useful in the urgent care setting for those in whom diagnosis of HF is uncertain.2,6 The presence of a BNP level of >100 pg/mL along with clinical judgment has been shown to increase the accuracy of the diagnosis of AHF.12 If the level is <100 pg/mL, other causes of dyspnea should be investigated. Levels are increased in elderly patients, women, and patients with renal dysfunction. Obesity results in lower levels of BNP.12
Patients with HF typically have a depressed (<40%) LVEF. However, since AHF is a clinical diagnosis and may present in patients without a depressed left ventricular function (e.g., in patients with diastolic dysfunction), solely using LVEF can be misleading. Thirty-seven percent of the patients in the ADHERE registry had an LVEF >40% prior to admission.5 Therefore, LVEF of <40% can be used to support the diagnosis of AHF, but an LVEF >40% cannot rule it out.
Treatment of Acute Decompensated Heart Failure
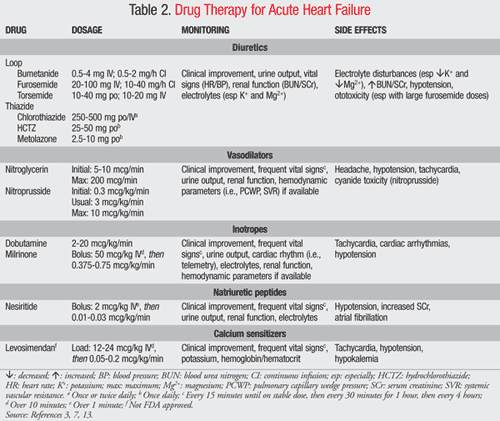
Pharmacologic Therapies: The goals of therapy for AHF are to improve symptoms and stabilize the hemodynamic situation.3,6 Short-term improvements must be balanced against the risk of long-term myocardial damage. Treatment of AHF is based on the presence of pulmonary congestion (volume overload) and the patient’s cardiac output (i.e., “cold and wet” versus “warm and dry”). Treatment choices include diuretic therapy, vasodilators, inotropic medications, natriuretic peptides, and calcium sensitizers (TABLE 2).3,13
Diuretics: IV loop diuretics are the drugs of choice in the management of AHF because of a faster onset of action and a brisk diuretic effect.2,3,6 Diuretics are indicated in patients presenting with signs of fluid overload (i.e., “wet”). Eighty-eight percent of the patients in the ADHERE database were treated with IV diuretics during their admission.14 Randomized controlled trials evaluating clinical outcomes with diuretics in AHF are lacking. Therefore, these medications are primarily prescribed for symptom relief.7
A recent analysis of the ADHERE database suggested negative outcomes in patients treated with IV diuretics; a longer total length of stay and extended stay in the intensive care unit were observed in patients treated with IV diuretics compared with patients who were not.14 Risks of therapy include electrolyte disturbances (hypokalemia, hypomagnesemia), activation of the renin-angiotensin-aldosterone system, and nephrotoxicity.2,3
Diuretic resistance is a phenomenon of diminished diuretic effect prior to achieving the therapeutic goal of edema relief.3 Diuretic resistance can be caused by a number of factors, including drug–drug interactions (e.g., with nonsteroidal anti-inflammatory drugs [NSAIDs]), decreased absorption, neurohormonal activation, increased sodium intake, or sodium reabsorption upregulation (i.e., increased reabsorption in the distal convoluted tubule).3 Patients more likely to have diuretic resistance include patients with chronic severe HF or those receiving long-standing diuretic therapy. Strategies to overcome diuretic resistance are listed in TABLE 3.3

Vasodilators: Vasodilator therapy with either nitroglycerin or nitroprusside should be considered first-line therapy in patients presenting with adequate blood pressure (systolic blood pressure >90 mmHg).2,3,6 Both of these medications cause vasodilation by increasing levels of nitric oxide, a smooth muscle relaxant.15 This results in a reduction in preload (the amount of blood presented to the heart) as well as a small reduction in afterload (systemic blood pressure) and a subsequent improvement in dyspnea. Vasodilators improve hemodynamics but may cause hypotension; therefore, they are most appropriate for patients presenting as “wet and warm” (FIGURE 1).3 Other risks of therapy include headache, tolerance to therapy (with nitroglycerin), and cyanide toxicity (with nitroprusside). Nitroprusside must be used with caution in patients with renal insufficiency.3
Inotropic Medications: Dobutamine and milrinone are the inotropic medications used in the short-term management of AHF to improve hemodynamic symptoms of decreased cardiac output. These medications work by increasing the intracellular level of cyclic adenosine monophosphate (cAMP) and/or calcium, therefore increasing contractility of the heart.16 It is believed that increased contractility comes at the cost of increased oxygen demand and energy consumption resulting in myocardial cell death.16 Recommendations are to use these agents with caution and only in patients with signs of hypoperfusion despite adequate diuretic and vasodilator therapy (i.e., “wet and cold”) (FIGURE 1).2,6,8

The Outcomes of a Prospective Trial of Intravenous Milrinone for Exacerbations of Chronic Heart Failure (OPTIME-CHF) was a large-scale, placebo-controlled study evaluating the use of milrinone.17 This study randomized 951 patients hospitalized with systolic dysfunction and an exacerbation of chronic HF not requiring inotropic support to either 48-hour IV treatment with milrinone or placebo. The milrinone group was associated with a higher incidence of symptomatic hypotension requiring intervention and new atrial arrhythmias. There were no improvements in total days hospitalized, symptomatic relief, or mortality with milrinone compared with placebo.17
Inotropic therapy selection is influenced by patient specific parameters. Dobutamine exerts its inotropic effect by stimulating the beta1-adrenergic receptor. Therefore, a patient maintained on a beta-blocking agent (e.g., bisoprolol, carvedilol, metoprolol) would have less of an effect and would require a higher dose.3 The major risks of therapy with the dobutamine are tachycardia and cardiac arrhythmia.3,18 Milrinone exerts its inotropic effects through inhibition of the phosphodiesterase type III enzyme, increasing the amount of cAMP.18 Milrinone is not dependent on the beta1-adrenergic receptor and is not influenced by the presence of beta-blocking agents. The major risks with this agent are hypotension (more common when a loading dose is used) and cardiac arrhythmia.16,18
Natriuretic Peptides: Nesiritide, the only commercially available natriuretic peptide, is a recombinant form of human BNP.15 Nesiritide causes both vasodilatation and diuresis resulting in increased cardiac output and reduction in dyspnea.2 Nesiritide was compared with IV nitroglycerin in 489 patients with decompensated HF and dyspnea at rest.19 This trial compared IV nesiritide, IV nitroglycerin, or placebo in addition to standard therapy for 24 hours. Nesiritide showed a significant reduction in PCWP at 3 hours versus both placebo and nitroglycerin. However, there was no difference in dyspnea scores between nesiritide and nitroglycerin at 3 hours or 24 hours.19 Concerns over increases in short-term (30-day) and long-term (180-day) mortality as well as renal function decreases in patients treated with nesiritide have limited this medication’s use in the treatment of AHF.20 The most significant side effect with this medication is hypotension, even at recommended doses.15
Calcium Sensitizers: Levosimendan is a novel agent for the treatment of AHF currently commercially available in Europe but investigational in the U.S. It has a dual mechanism of action: 1) increasing calcium activity inside the cardiac cell, therefore increasing contractility; and 2) acting as a smooth muscle relaxant causing vasodilation.21 The mechanism of action does not increase myocardial oxygen demand and therefore, in theory, does not carry the risk of increased cell death. In the Levosimendan Infusion Versus Dobutamine (LIDO) trial, 203 patients with HF with low output were randomized to IV dobutamine or levosimendan.22 Treatment with levosimendan improved the primary end point of hemodynamic performance more effectively than dobutamine. The levosimendan group also had significantly lower 6-month mortality than the dobutamine group.22 However, the survival benefit was not confirmed in a larger trial by Mebazaa et al.23 The SURVIVE trial was designed to assess a mortality difference following 24-hour infusions of levosimendan or dobutamine.23 All-cause mortality was similar at 180 days in both groups (levosimendan 26% and dobutamine 28%; P = .40). Side effects with this medication appear minor and related to vasodilation (hypotension and headache).24
Pharmacist’s Role
There are numerous ways pharmacists can impact the care of patients admitted with AHF. Pharmacists can assist in the evidence-based selection of drug therapy. It is crucial that every therapeutic decision be made with diligence since therapeutic agents that are used only for hours can have an impact on long-term morbidity and mortality.16 AHF requires the use of medications that have weight-based dosing and necessitate dosage adjustments based on renal function. Pharmacists should actively screen patients’ medications for correct dosing. AHF patients carry a high risk of deep venous thrombosis (DVT) and pulmonary embolism.25 Pharmacists need to be diligent to assure that patients receive adequate DVT prophylaxis as indicated by the CHEST guidelines for medical patients (i.e., enoxaparin 40 mg subcutaneously daily).26
Common reasons for admission with HF exacerbation are medication related; noncompliance or addition of a medication that can worsen HF (e.g., an NSAID or negative inotropic drug such as diltiazem).2 Pharmacists play a vital role in identifying these drug-related problems through a detailed medication reconciliation upon admission. The ACC/AHA guidelines recommend that medications be reconciled for every patient admitted with HF at admission.2
Lastly, the care of every patient admitted with HF should be consistent with the core measures of the Joint Commission on Accreditation of Healthcare Organization (JCAHO). The measures for HF include detailed discharge instructions for the patient; an assessment of the left ventricular (LV) function; an angiotensin-converting enzyme inhibitor (ACEI) or angiotensin receptor blocker (ARB) for patients with a decreased LVEF (<40%); and smoking cessation counseling.27 Pharmacists have been shown to be effective providers of smoking cessation interventions, but there is also an opportunity for pharmacists to impact the utilization of ACEIs or ARBs in patients with LV dysfunction.28 Compliance rates with this are approaching 90%; however, pharmacists should always screen patients admitted with HF to determine if an ACEI or ARB is appropriate.1
On the contrary, the measure of discharge counseling is not met consistently. Data from the ADHERE database indicate that this measure is met in only 32.3% of patients admitted with AHF.5 One of its components is education on discharge medications. Pharmacists play a crucial role in educating patients regarding their discharge medications and the importance of compliance and follow-up.2
Summary
Acute decompensated heart failure is a complicated life-threatening disease. Initial management is directed at hemodynamic improvement and reducing congestion. However, some of these therapies carry the risk of worsening myocardial ischemia and renal function, leading to long-term negative outcomes. Pharmacists play a vital role in helping to select the appropriate therapy and monitoring for side effects in patients with AHF. Pharmacists can also impact the long-term outcomes by helping to ensure that patients are being treated to comply with the JCAHO’s core measures.
REFERENCES
1. Lloyd-Jones D, Adams R, Carnethon M, et al. Heart disease and stroke statistics–2009 update: a report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation. 2009;119:e21-e181.
2. Hunt SA, Abraham WT, Chin MH, et al. 2009 focused update incorporated into the ACC/AHA 2005 Guidelines for the Diagnosis and Management of Heart Failure in Adults: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines: developed in collaboration with the International Society for Heart and Lung Transplantation. Circulation. 2009;119:e391-e479.
3. Nieminen MS, Bohm M, Cowie MR, et al. Executive summary of the guidelines on the diagnosis and treatment of acute heart failure. The Task Force on Acute Heart Failure of the European Society of Cardiology. Eur Heart J. 2005;26:384-416.
4. Felker GM, Adams KF Jr, Konstam MA, et al. The problem of decompensated heart failure: nomenclature, classification, and risk stratification. Am Heart J. 2003;145(suppl 2):S18-S25.
5. Adams KF Jr, Fonarow GC, Emerman CL, et al. Characteristics and outcomes of patients hospitalized for heart failure in the United States: rationale, design, and preliminary observations from the first 100,000 cases in the Acute Decompensated Heart Failure National Registry (ADHERE). Am Heart J. 2005;149:209-216.
6. Heart Failure Society of America. Executive summary: HFSA 2006 Comprehensive Heart Failure Practice Guideline. J Card Fail. 2006;12:10-38.
7. DiDomenico RJ, Park HY, Southworth MR, et al. Guidelines for acute decompensated heart failure treatment. Ann Pharmacother. 2004;38:649-660.
8. Allen LA, O’Connor CM. Management of acute decompensated heart failure. CMAJ. 2007;176:797-805.
9. McKee PA, Castelli WP, McNamara PM, Kannel WB. The natural history of congestive heart failure: the Framingham study. N Engl J Med. 1971;285:1441-1446.
10. Forrester JS, Diamond GA, Swan H. Correlative classification of clinical and hemodynamic function after acute myocardial infarction. Am J Cardiol. 1977;39:137-145.
11. Nohria A, Tsang SW, Fang JC, et al. Clinical assessment identifies hemodynamic profiles that predict outcomes in patients admitted with heart failure. J Am Coll Cardiol. 2003;41:1797-1804.
12. Felker GM, Petersen JW, Mark DB. Natriuretic peptides in the diagnosis and management of heart failure. CMAJ. 2006;175:611-617.
13. Physicians’ Desk Reference. 63rd ed. Montvale, NJ: Thomson PDR; 2009.
14. Gheorghiade M, Filippatos G. Reassessing treatment of acute heart failure syndromes: the ADHERE registry. Eur Heart J Suppl. 2005;7:B13-B19.
15. Stough WG, O’Connor CM, Gheorghiade M. Overview of current noninodilator therapies for acute heart failure syndromes. Am J Cardiol. 2005;96:41G-46G.
16. Bayram M, De Luca L, Massie MB, Gheorghiade M. Reassessment of dobutamine, dopamine, and milrinone in the management of acute heart failure syndromes. Am J Cardiol. 2005;96:47G-58G.
17. Cuffe MS, Califf RM, Adams KF Jr, et al. Short-term intravenous milrinone for acute exacerbation of chronic heart failure: a randomized controlled trial. JAMA. 2002;287:1541-1547.
18. Overgaard CB, Dzavik V. Inotropes and vasopressors: review of physiology and clinical use in cardiovascular disease. Circulation. 2008;118:1047-1056.
19. Publication Committee for the VMAC Investigators (Vasodilatation in the Management of Acute CHF). Intravenous nesiritide vs nitroglycerin for treatment of decompensated congestive heart failure: a randomized controlled trial. JAMA. 2002;287:1531-1540.
20. Dontas ID, Xanthos T, Dontas I, et al. Impact of nesiritide on renal function and mortality in patients suffering from heart failure. Cardiovasc Drugs Ther. 2009;23:221-233.
21. Gheorghiade M, Teerlink JR, Mebazaa A. Pharmacology of new agents for acute heart failure syndromes. Am J Cardiol. 2005;96:68G-73G.
22. Follath F, Cleland JG, Just H, et al. Efficacy and safety of intravenous levosimendan compared with dobutamine in severe low-output heart failure (the LIDO study): a randomised double-blind trial. Lancet. 2002;360:196-202.
23. Mebazaa A, Nieminen MS, Packer M, et al. Levosimendan vs dobutamine for patients with acute decompensated heart failure: the SURVIVE Randomized Trial. JAMA. 2007;297:1883-1891.
24. Follath F, Franco F, Cardoso JS. European experience on the practical use of levosimendan in patients with acute heart failure syndromes. Am J Cardiol. 2005;96:80G-85G.
25. Beemath A, Stein PD, Skaf E, et al. Risk of venous thromboembolism in patients hospitalized with heart failure. Am J Cardiol. 2006;98:793-795.
26. Geerts WH, Bergqvist D, Pineo GF, et al. Prevention of venous thromboembolism: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th Edition). Chest. 2008;133(suppl 6):381S-453S.
27. Specifications Manual for National Hospital Inpatient Quality Measures. The Joint Commission. www.jointcommission.org/PerformanceMeasurement/PerformanceMeasurement/Current+NHQM+Manual.htm. Accessed November 5, 2009.
28. Dent LA, Harris KJ, Noonan CW. Randomized trial assessing the effectiveness of a pharmacist-delivered program for smoking cessation. Ann Pharmacother. 2009;43:194-201.
To comment on this article, contact rdavidson@uspharmacist.com.





