US Pharm. 2016;41;(7):HS11-HS15.
ABSTRACT: Hospital-acquired pneumonia (HAP) is a commonly encountered infection in the inpatient setting. Challenges to the appropriate management of HAP include delayed diagnosis, inappropriate empiric treatment, presence of multidrug-resistant pathogens, and emergence of antimicrobial resistance. Healthcare professionals play a key role in early identification of HAP and initiation of appropriate antimicrobial therapy in an effort to successfully treat patients, minimize adverse outcomes, and curb the rapid increase of antibiotic resistance. As vital members of interdisciplinary healthcare teams, including antimicrobial stewardship programs, pharmacists can assist with successful management of HAP and improve patient outcomes.
Hospital-acquired pneumonia (HAP) is the leading cause of death among patients with hospital-acquired infections.1-3 Although HAP is not a reportable illness, available data suggest that it occurs at a rate of between 5 and 10 cases per 1,000 hospital admissions, with the incidence increasing by as much as 6-to 20-fold in mechanically ventilated patients.2 Despite advances in prevention and treatment of infections, HAP remains an important problem in hospitalized patients. Although most HAP cases occur outside intensive care units (ICUs), the highest risk is among patients who are mechanically ventilated in the ICU.4
The 2005 American Thoracic Society/Infectious Diseases Society of America (ATS/IDSA) guidelines define pneumonia in hospitalized patients and those with chronic exposures to healthcare systems. HAP is defined as pneumonia that occurs 48 hours or more after hospital admission that was not incubating at the time of admission. Ventilator-associated pneumonia (VAP) refers to pneumonia that develops more than 48 to 72 hours after endotracheal intubation. Healthcare-associated pneumonia (HCAP) includes any patient who was hospitalized in an acute care hospital for 2 or more days within 90 days of the infection, or resided in a nursing home or long-term care facility, received recent IV antibiotic therapy, chemotherapy, or wound care within 30 days of the current infection, or attended a hospital or hemodialysis clinic.1 These categorizations are used for risk stratification, determining the need for hospitalization, and selecting treatment strategies.5 Differences in disease etiology, severity, and demographics make category recognition essential.
One of the challenges clinicians often face in the appropriate management of patients with hospital-acquired infections is the rapid rise in antimicrobial resistance. The World Health Organization has identified antibiotic resistance as one of the three greatest threats to human health.6 The increase in emergence of antimicrobial resistance has rendered some of the most commonly used anti-infective agents ineffective. Healthcare professionals are more than ever required to judiciously select antibiotics when managing patients with infections. Although the development of drug resistance is a natural phenomenon, the inappropriate use of antimicrobial drugs, inadequate sanitary conditions, and poor infection prevention and control practices all contribute to emergence of, and encourage, the further spread of drug-resistant pathogens.7
Almost all infecting organisms are capable of developing multidrug resistance with enhanced morbidity and mortality. Organisms that have in vitro resistance to more than one class of antimicrobial agents are termed multidrug-resistant organisms (MDROs).8 When HAP is suspected, it is crucial to identify risk factors for being infected with MDROs. Certain host and environmental factors make a patient more susceptible to MDROs (Table 1).1 In addition, time of onset of pneumonia is an important epidemiologic variable and risk factor for specific pathogens. Early-onset HAP is defined as pneumonia occurring within the first 4 days of hospitalization and late-onset HAP is defined as pneumonia occurring after 5 or more days of hospitalization. Early-onset HAP usually carries a better prognosis, and is more likely to be caused by antibiotic-sensitive bacteria. Late-onset HAP is more likely to be caused by an MDRO, and is associated with increased patient morbidity and mortality.1

Microbiology
HAP is caused by a wide spectrum of bacterial pathogens. HAP may be polymicrobial and is rarely due to viral or fungal pathogens in immunocompetent hosts. Common pathogens include aerobic gram-negative bacilli, such as Pseudomonas aeruginosa, Escherichia coli, Klebsiella pneumoniae, and Acinetobacter spp.1,9,10 Infections due to gram-positive cocci, such as Staphylococcus aureus, particularly methicillin-resistant S aureus (MRSA), have been rapidly emerging in the United States.1,11 Pneumonia due to S aureus is more common in patients who have diabetes mellitus, head trauma, and who are hospitalized in ICUs.1,9 Infections traceable to fungi or viruses are more commonly seen in immunocompromised patients.9
Risk Factors and Prevention Strategies
Risk factors for the development of HAP can be differentiated into modifiable and non-modifiable conditions and can also be related to patient characteristics (e.g., male sex, older age, preexisting pulmonary disease, or multiple organ-system failure) or to treatment (e.g., intubation or use of acid-suppressive therapies).1 Modifiable risk factors for HAP are targets for improved management and prevention of infection in hospital settings.1 Intubation has been shown to increase the risk of developing pneumonia in hospitalized patients. In those who are mechanically ventilated, it is important to keep the head of the bed elevated 30° to 45°, as a supine position predisposes the patient to aspiration and development of pneumonia.12 Drug therapies that increase gastric pH, such as histamine type 2 (H2) antagonists and proton pump inhibitors, have been identified as independent risk factors for ICU-acquired HAP.13 Therefore, if stress-ulcer prophylaxis in indicated, the risks and benefits of each regimen should be weighed before prescribing acid-suppressive therapies with H2 antagonists and proton pump inhibitors.
Effective prevention strategies include strict infection control with appropriate hand hygiene, use of clearly marked isolation precautions, use of microbial surveillance with timely availability of microbial resistance pattern data, and early removal of invasive devices.1
Antimicrobial Therapy and Special Considerations
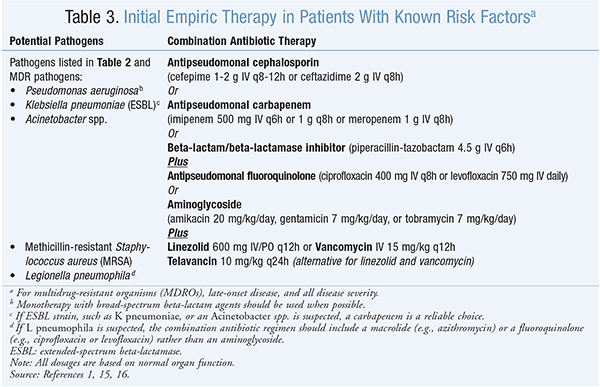
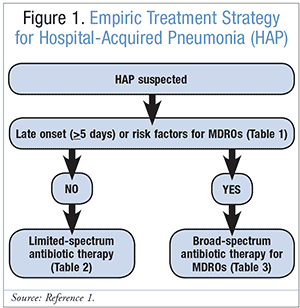
Clinical strategy emphasizes prompt and appropriate empiric antimicrobial therapy for patients with suspected HAP.1 There is consistent evidence that a delay in the initiation of appropriate antibiotic therapy for patients with HAP is associated with increased mortality.1 The selection of initial antibiotic therapy is based on risk factors for specific pathogens, modified by knowledge of local patterns of antibiotic resistance and organism prevalence.1 Therapy is then modified on the basis of clinical response on days 2 and 3 of an empiric antibiotic regimen and the findings of cultures of lower respiratory tract secretions.1 The key decision in initial empiric antimicrobial therapy is whether the patient has risk factors for MDROs and the timing of onset (early vs. late) of HAP (Figure 1).1
The initial empiric antibiotic therapy for patients with early-onset HAP and no known risk factors for MDROs is outlined in Table 2. Additionally, the initial empiric therapy for patients with late-onset HAP or risk factors for MDROs is outlined in Table 3. In patients with risk factors for MDROs, particularly with MRSA, vancomycin or linezolid is an appropriate first choice. Telavancin is an appropriate alternative if vancomycin or linezolid cannot be used due to its activity against gram-positive HAP pathogens (MRSA, vancomycin-intermediate S aureus, and penicillin-resistant Streptococcus pneumoniae).14,15 Telavancin’s once-daily regimen offers an advantage over vancomcycin and linezolid; however, caution should be taken in patients with renal impairment. Other agents such as ceftaroline, daptomycin, quinupristin-dalfopristin, and tigecycline are generally not recommended for management of HAP due to MRSA.

Infections with gram-negative MDROs pose a considerable challenge for the healthcare professional because of the associated poor prognosis and high mortality.16 Combination therapy for suspected gram-negative HAP has been a common practice. In particular, when P aeruginosa is suspected, combination therapy has been utilized as a means to increase the likelihood that the organism will be susceptible to one of the agents in the combination to achieve a synergistic effect and to prevent emergence of resistance during therapy. However, clinical failure and increased risk of nephrotoxicity have been shown to be more common with the use of combination therapy, with no added benefit of preventing antimicrobial resistance. When possible, monotherapy with broad-spectrum beta-lactam agents should be considered and combination therapy should be reserved for patients when benefit outweighs risk. Certain patient populations and circumstances, such as those with severe sepsis and those admitted to the ICU, may benefit from the use of combination empiric therapy.16-18
In patients who receive an initially appropriate antibiotic regimen, efforts should be made to shorten the duration of therapy from the traditional 14 to 21 days to periods as short as 7 to 8 days.19 Longer durations of treatment may be required if MDROs are present.
Vaccination
Two pneumococcal vaccines are approved for use in the U.S.: pneumococcal conjugate vaccine (PCV13 [Prevnar 13]) and 23-valent pneumococcal polysaccharide vaccine (PPSV23 [Pneumovax 23]). The Advisory Committee on Immunization Practices (ACIP) recommends all immunocompetent adults >65 years of age receive a dose of PCV13 followed by a dose of PPSV23 at least 1 year later. Adults 19 years of age or older with immunocompromising conditions (HIV infection, leukemia, lymphoma, Hodgkin’s disease, multiple myeloma, generalized malignancy, chronic renal failure, or nephrotic syndrome), functional or anatomic asplenia (including sickle cell disease), cerebrospinal fluid (CSF) leaks, or cochlear implants should receive a dose of PCV13 followed by a dose of PPSV23 eight weeks later. Adults >19 years of age who have immunocompromising conditions, functional or anatomic asplenia, or who are receiving immunosuppressive chemotherapy that includes a high-dose corticosteroid, or have received an organ or bone marrow transplant, should receive a second PPSV23 dose 5 years after the first dose. PPSV23 only is recommended in individuals 19 to 64 years of age with chronic cardiac or pulmonary diseases, chronic liver disease, alcoholism, or diabetes, or who smoke cigarettes or live in special environments (e.g., nursing homes, long-term care facilities). Individuals who received a dose of PPSV23 before the age of 65 years should receive one final dose at age 65 if at least 5 years have elapsed since the first PPSV23 dose.20,21
Role of Pharmacists
Clinical pharmacists with training in infectious diseases (ID) are considered to have the expertise to identify opportunities for intervention and to judiciously select antimicrobial therapies. Antimicrobial stewardship programs (ASPs) have been promoted to improve appropriate use of antimicrobials, with several governmental and regulatory agencies adopting mandates and recommendations for ASP implementation.22,23 An effective ASP should ideally include an ID physician, a hospital epidemiologist, and a clinical pharmacist with ID training. The responsibilities of an ID pharmacist on an ASP involve identifying patients receiving inappropriate dosing and recognizing patients at high risk for antimicrobial toxicity.22 Pharmacists are uniquely positioned to recommend the appropriate dosing and selection of antibiotics based on pharmacodynamic and pharmacokinetic properties. For example, a pharmacist can optimize the antimicrobial effect of beta-lactam agents by recommending an extended-infusion regimen as a means of curbing the emergence of antibiotic resistance and potentially providing a pharmacoeconomic benefit. Due to beta-lactam agents’ time-dependent activity, prolonged infusion duration increases the time the free drug concentration remains above the minimum inhibitory concentration (MIC) of the organism.24,25
Furthermore, pharmacists are more adept at identifying potential drug-related toxicities as well as implementing appropriate monitoring plans to minimize the risk of adverse events. Fluoroquinolones, for example, have been scrutinized for their potential risk of causing QT prolongation and damage to tendons, muscles, joints, nerves, and the central nervous system. These side effects can be disabling and may become permanent. Therefore, fluoroquinolones should be reserved for patients with no alternative treatment options.26,27
Pharmacists play a major role in designing patient-specific and cost-effective drug regimens. In a study by Gross et al., ASP recommendations given by a clinical pharmacist trained in ID were compared with ASP recommendations given by ID medical fellows. Seventy-six percent of recommendations given by pharmacists were found to be appropriate, whereas only 44% of recommendations given by ID fellows were assessed as appropriate by a physician reviewer; clinical and microbiological cures were achieved in 49% of cases involving a pharmacist recommendation, but in only 35% of those involving an ID fellow recommendation.28 Unfortunately, there are not enough specially trained pharmacists to provide ASP services in all healthcare settings that would benefit from these programs.23 Additionally, proposed standards for pharmacists practicing ID pharmacotherapy may be impractical in resource-limited settings.23 As more pharmacists are considering specialized post-doctoral training in ID, the increasing role of highly trained pharmacists has enabled hospitals to deliver ASP services, provide opportunities to expand this role further, and ensure an increase in positive patient outcomes.
Conclusion
HAP is a serious public health issue that leads to lengthened hospital stays, higher healthcare costs, and increased rates of morbidity and mortality. This is exacerbated by the alarming increase of MDR pathogens. Prompt diagnosis and initiation of appropriate empiric therapy for all patients suspected of having HAP, as well as pharmacotherapeutic modification on the basis of the clinical response on days 2 and 3 and the findings of cultures of lower respiratory tract secretions, are crucial for the successful treatment of HAP. As healthcare providers, pharmacists are uniquely positioned to advocate for the prevention of diseases through promotion and administration of vaccinations. Pharmacists play a vital role in curbing the emergence of antibiotic resistance by appropriately selecting, dosing, and monitoring antibiotic regimens. The increasing role of pharmacists in ASPs enables hospitals to optimize patient care and achieve improved outcomes such as decreases in length of stay, hospital-associated costs, and mortality.
REFERENCES
1. American Thoracic Society, Infectious Diseases Society of America. Guidelines for the management of adults with hospital-acquired, ventilator-associated, and healthcare-associated pneumonia. Am J Respir Crit Care Med. 2005;171(4):388-416.
2. Barbier F, Andremont A, Wolff M, Bouadma L. Hospital-acquired pneumonia and ventilator-associated pneumonia: recent advances in epidemiology and management. Curr Opin Pulm Med. 2013;19(3):216-228.
3. Craven DE, Palladino R, McQuillen DP. Healthcare-associated pneumonia in adults: management principles to improve outcomes. Infect Dis Clin North Am. 2004;18(4):939-962.
4. Melsen WG, Rovers MM, Groenwold RH, et al. Attributable mortality of ventilator-associated pneumonia: a meta-analysis of individual patient data from randomised prevention studies. Lancet Infect Dis. 2013;13(8):665-671.
5. Shorr AF, Owens RC. Quality pneumonia care: distinguishing community-acquired from health care-associated pneumonia. Am J Health-Syst Pharm. 2009;66(12 Suppl 4):S8-S14.
6. The 10 × ‘20 initiative: pursuing a global commitment to develop 10 new antibacterial drugs by 2020. Clin Infect Dis. 2010;50(8):1081-1083.
7. Tanwar J, Das S, Fatima Z, Hameed S. Multidrug resistance: an emerging crisis. Interdiscip Perspect Infect Dis. 2014;(2014):Article ID:541340.
8. Magiorakos AP, Srinivasan A, Carey RB, et al. Multidrug-resistant, extensively drug-resistant and pandrug-resistant bacteria: an international expert proposal for interim standard definitions for acquired resistance. Clin Microbiol Infect. 2012;18(3):268-281.
9. Jones RN. Microbial etiologies of hospital-acquired bacterial pneumonia and ventilator-associated bacterial pneumonia. Clin Infect Dis. 2010;51 Suppl 1:S81-S87.
10. Peahota M, Shah BM, El-Beyrouty C, Schafer JJ. Healthcare-associated pneumonia: Who is truly at risk for multidrug-resistant pathogens? Am J Health-Syst Pharm. 2015;72(21):1897-1904.
11. Rubinstein E, Kollef MH, Nathwani D. Pneumonia caused by methicillin‐resistant Staphylococcus aureus. Clin Infect Dis. 2008;46(S5):S378-S385.
12. Coffin SE, Klompas M, Classen D, et al. Strategies to prevent ventilator-associated pneumonia in acute care hospitals. Infect Control Hosp Epidemiol. 2008;29 Suppl 1:S31-S40.
13. Herzig SJ, Howell MD, Ngo LH, Marcantonio ER. Acid-suppressive medication use and the risk for hospital-acquired pneumonia. JAMA. 2009;301(20):2120-2128.
14. Sandrock CE, Shorr AF. The role of telavancin in hospital-acquired pneumonia and ventilator-associated pneumonia. Clin Infect Dis. 2015;61 Suppl 2:S79-S86.
15. Liu C, Bayer A, Cosgrove SE, et al. Clinical practice guidelines by the infectious diseases society of america for the treatment of methicillin-resistant Staphylococcus aureus infections in adults and children. Clin Infect Dis. 2011;52(3):e18-e55.
16. Tamma PD, Cosgrove SE, Maragakis LL. Combination therapy for treatment of infections with gram-negative bacteria. Clin Microbiol Rev. 2012;25(3):450-470.
17. Johnson SJ, Ernst EJ, Moores KG. Is double coverage of gram-negative organisms necessary? Am J Health Syst Pharm. 2011;68(2):119-124.
18. Boyd N, Nailor MD. Combination antibiotic therapy for empiric and definitive treatment of gram-negative infections: insights from the Society of Infectious Diseases Pharmacists. Pharmacotherapy. 2011;31(11):1073-1084.
19. File, Jr. TM. Recommendations for treatment of hospital‐acquired and ventilator‐associated pneumonia: review of recent international guidelines. Clin Infect Dis. 2010;51(S1):S42-S47.
20. Kobayashi M, Bennett NM, Gierke R, et al. Intervals between PCV13 and PPSV23 vaccines: recommendations of the advisory committee on immunization practices (ACIP). MMWR Morb Mortal Wkly Rep. 2015;64(34):944-947.
21. Kim DK, Bridges CB, Harriman KH. Advisory committee on immunization practices (ACIP), ACIP Adult Immunization Work Group. Advisory committee on immunization practices recommended immunization schedule for adults aged 19 years or older - United States, 2016. Am J Transplant. 2016;16(6):1930-1932.
22. Yu K, Rho J, Morcos M, et al. Evaluation of dedicated infectious diseases pharmacists on antimicrobial stewardship teams. Am J Health Syst Pharm. 2014;71(12):1019-1028.
23. Carreno JJ, Kenney RM, Bloome M, et al. Evaluation of pharmacy generalists performing antimicrobial stewardship services. Am J Health Syst Pharm. 2015;72(15):1298-1303.
24. MacVane SH, Kuti JL, Nicolau DP. Prolonging -lactam infusion: a review of the rationale and evidence, and guidance for implementation. Int J Antimicrob Agents. 2014;43(2):105-113.
25. Roman C, Solh T, Damer KM. Who should receive extended infusion beta-lactam therapy? JAAPA. 2016;29(3):25-26.
26. Bidell MR, Lodise TP. Fluoroquinolone-asssociated tendinopathy: does levofloxacin pose the greatest risk? Pharmacotherapy. May 3, 2016. E-Pub ahead of print.
27. Arabyat RM, Raisch DW, McKoy JM, Bennett CL. Fluoroquinolone-associated tendon-rupture: a summary of reports in the Food and Drug Administration’s adverse event reporting system. Expert Opin Drug Saf. 2015;14(11):1653-1660.
28. Gross R, Morgan AS, Kinky DE, et al. Impact of a hospital-based antimicrobial management program on clinical and economic outcomes. Clin Infect Dis. 2001;33(3):289-295.
29. File TM Jr. Treatment of hospital-acquired, ventilator-associated, and healthcare-associated pneumonia in adults. In: UpToDate, Post TW (Ed). UpToDate, Waltham, MA. Accessed June 8, 2016.
To comment on this article, contact rdavidson@uspharmacist.com.