US Pharm.
2007;32(3):66-71.
Coronary heart disease is the leading cause
of death in the United States. Each year, approximately 1.2 million Americans
will have a new or recurrent event related to coronary heart disease.1
Furthermore, considering the increasing prevalence of type 2 diabetes in the
U.S., it is important to note that cardiovascular disease is the leading cause
of death among patients with both types of diabetes and accounts for two out
of three diabetes-related deaths.2 Many patients who have diabetes
with dyslipidemia remain poorly controlled despite recommendations for lower
LDL cholesterol levels.3 Large, well-designed, placebo-controlled
studies have shown that lowering LDL cholesterol level reduces coronary heart
disease events. With so many patients in need of lipid-lowering therapy, this
question arises: Are we treating LDL cholesterol levels sufficiently to
achieve the desired goals? This article reviews the LDL cholesterol goals
recommended by recent guidelines and focuses on barriers to achieving these
goals, as well as some ways to overcome them.
Before considering some of the
reasons why patients don't meet their LDL cholesterol goals, it is important
to understand what those goals are and what the criteria for treatment is. In
2004, the National Cholesterol Education Program (NCEP) released a report that
included an assessment of five major clinical trials published since the Adult
Treatment Panel III (ATP III) issued guidelines in 2001. These trials--the
Heart Protection Study (HPS), the Prospective Study of Pravastatin in the
Elderly at Risk (PROSPER) study, the Antihypertensive and Lipid-Lowering
Treatment to Prevent Heart Attack Trial–Lipid-Lowering Trial (ALLHAT-LLT), the
Anglo-Scandinavian Cardiac Outcomes Trial–Lipid-Lowering Arm (ASCOT-LLA), and
the Pravastatin or Atorvastatin Evaluation and Infection-Thrombolysis in
Myocardial Infarction 22 (PROVE IT-TIMI 22) trial--contained information that
had not been fully evaluated in previous studies.4
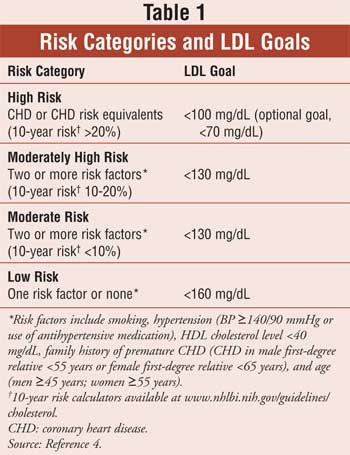
Based on review of these
recent trials, NCEP updated the guidelines. (See Table 1 for risk
levels and corresponding LDL cholesterol goals).4 The new
guidelines include an optional therapeutic LDL cholesterol goal of less than
70 mg/dL for patients in the very high-risk category. Patients considered to
be at very high risk are those with established cardiovascular disease plus
one or more of the following: multiple risk factors (including diabetes),
other severe or poorly-controlled risk factors (e.g., cigarette smoking),
multiple risk factors of the metabolic syndrome (elevated triglyceride level
>200 mg/dL plus non-HDL cholesterol level >130 mg/dL, with low HDL <40 mg/dL),
and acute coronary syndromes. Both HPS and PROVE IT, as well as the recent
Treating to New Targets (TNT) study, suggest that there is additional benefit
by reducing LDL cholesterol levels to below 100 mg/dL.5
Guidelines in Clinical
Practice
A review of the
literature gives some insight into how successfully guidelines are implemented
in clinical practice. The Lipid Treatment Assessment Process (L-TAP), a
multicenter survey evaluating the number of patients on lipid-lowering therapy
who have reached their LDL cholesterol goals, showed that 38% of patients
achieved the targets specified by NCEP for LDL cholesterol, but only 18% of
those with coronary heart disease met their goal.6 Some
explanations for the low percentages include failure to increase
lipid-lowering therapy, failure to use combination therapy, and poor patient
adherence. In a study involving Veterans Affairs patients in Texas, a majority
of patients received therapy for hypertension and dyslipidemia, but less than
50% met the therapeutic goals for each disease state.7 Findings
from a managed care study showed that older individuals, men, and patients
compliant with statin therapy were more likely to meet their LDL cholesterol
goal. On the other hand, women, high-risk younger patients, and patients with
fewer outpatient visits associated with dyslipidemia and cholesterol lab
testing had a much lower level of compliance.8 Additionally, a
retrospective review of 600 patients followed by cardiologists at a heart
clinic revealed that only about 76% of patients achieved the recommended LDL
cholesterol level of less than 100 mg/dL. Of these patients, 81% were on
lipid-lowering therapy, but only 18% were taking the maximal dose, and 6% were
taking combination therapy.9
Clearly, there is still some
room for improvement across the board. Although the efficacy and benefits of
lipid-lowering therapies are well documented, they are irrelevant if the
patient is not compliant. Adherence is a complex topic, because there are
several different aspects to consider that are related to the patient, the
provider, and the medication regimen.10
Patient-Related Barriers
Delaying
Pharmacotherapy:
Therapeutic lifestyle changes, which include diet, physical activity, and
weight loss, remain first-line treatment for dyslipidemia. Therefore, it is
not uncommon for treatment with medication to be delayed while patients first
try diet and lifestyle changes. ATP III reduced the trial of therapeutic
lifestyle changes from six months to 12 weeks and simplified the diet
recommendations from a two-step to a one-step diet recommendation for all
patients.11 Despite the guidelines for a shorter trial of
therapeutic lifestyle changes, patients sometimes extend the trial period in
order to postpone taking medication.
Treatment Adherence:
Patients may not adhere to their prescribed treatment for a variety of
reasons. Once patients are prescribed lipid-lowering agents, they may not
understand the treatment regimen or why the medication(s) have been
prescribed. The prevalence of multiple medications is increasing, since more
than one lipid-lowering agent may be required to reach the newer goals.
Patients may question why they must take many different medicines. Although
dyslipidemia does not typically make patients feel sick, side effects of some
of the medications prescribed may make them feel poorly. In addition, patients
now use the Internet and other forms of media for medical information;
incorrect or misunderstood information can influence a patient's decision to
initiate or discontinue therapy. Without proper education, patients may decide
not to follow prescribed therapy.
Adherence to lipid-lowering
medications increases the success rate for attaining LDL cholesterol goals.
Clinical trials demonstrate statin adherence rates of 80% to 87% over a period
of three to four years.12 A study looking at pharmacy insurance
claims projected an adherence rate of 78.5% in adults prescribed statin
therapy for secondary prevention.13 However, a study of elderly
patients found an adherence rate of 36.1% in patients with coronary artery
disease.14 Therefore, it is important for clinicians to assess
medication adherence before changing therapy when clinical goals are not met.
15
Financial
Considerations: The
patient's ability to afford the medication(s) should be discussed. If cost is
a barrier, providers may need to emphasize diet and non-prescription
alternatives or consider generic formulations. For the patient who has reached
his or her goal on two lipid-lowering products, a combination product may save
money, but health care providers may fail to offer this option because of the
time and/or effort it would take to make the change. A combination product may
not only offer financial savings but also simplify the regimen by decreasing
the number of medications.
Provider-Related Barriers
Poor
Communication: To
prevent patient-related factors from interfering with adherence, there must be
open dialogue between the patient and provider. Providers have a pivotal role
in screening, diagnosing, and treating dyslipidemia but often face
constraints--lack of time to fully explain treatment, lack of reimbursement for
counseling, inadequate counseling skills, and lack of educational support
staff--that may interfere with providing the patient with the education
necessary to maximize adherence. This may result in too many issues being
addressed in one visit. Optimally, patient instructions should be given over
several appointments.10
Regimen-Related Barriers
Number of
Medications: For some
patients, such as those with comorbid conditions, the number of medications
they must take may seem unmanageable. For example, the average patient with
diabetes takes eight medications, and approximately 25% of patients will
require more than two lipid-lowering drugs to reach an LDL cholesterol level
of less than 70 mg/dL.12 Pharmacists have been effective in
reducing the burden for patients who are taking several medicines. For
example, in one study, a pharmacy-care program used custom blister-packed
medications to enhance adherence in elderly patients on complex medication
regimens.16 Other alternatives to custom blister packs include
weekly or monthly medication trays or boxes.
Adequate Dosing:
Despite therapeutic lifestyle changes, many patients will require
lipid-lowering therapy to reach their LDL cholesterol goal. HMG-CoA reductase
inhibitors, or statins, are the most potent agents for lowering LDL
cholesterol. They offer the ability to lower LDL cholesterol by 18% to 55%,
depending on the strength of medication.11 Often, physicians
initiate statin therapy at a low dose and then fail to titrate to the LDL
cholesterol goal. In high-risk or moderately high-risk patients, statin
therapy should be dosed to achieve a 30% to 40% reduction in LDL cholesterol
levels.6 Lipid levels should be re-checked six weeks after
initiation of therapy, and dosage adjustments should be decided at that time.
11
For patients who require
lowering of their LDL cholesterol level by more than 40%, combination therapy
may be considered. Combination therapy offers the advantage of lower doses of
statins, which may minimize side effects, while enhancing LDL-lowering
capabilities.17 For example, in a large community-based trial, the
addition of ezetimibe to statin therapy allowed 71% of patients to reach their
LDL cholesterol goal, compared with 20.6% of patients treated with statin
therapy plus placebo.18 Some disadvantages of combination therapy
include increased medications and cost, unless there is a combination product
available.
Side Effects:
Statins reduce coronary events, coronary heart disease mortality, coronary
procedures, stroke, and total mortality, but as with any other medication,
there are adverse effects to monitor,19 some of which may reduce
compliance with treatment. Common side effects associated with statin therapy
include gastrointestinal symptoms, headache, and rash.20 These side
effects are often mild and transient. Bile acid sequestrants can be difficult
to tolerate due to gastrointestinal side effects. Flushing decreases
compliance with niacin. The FDA acknowledges that the incidence of side
effects in clinical practice may be higher than in clinical trials where the
patients are monitored more closely.
Statins are associated with a
variety of muscle effects ranging from mild pain to rhabdomyolysis. (The
withdrawal of cerivastatin [Baycol] in 2001 due to fatal rhabdomyolysis may
make providers and patients fearful of possible side effects with this class
of drugs.) Drug interactions are a common cause of myopathy in patients taking
statin therapy. Concurrent use of CYP3A4 inhibitors, such as itraconazole,
ketoconazole, erythromycin, clarithromycin, and nefazodone, retroviral drugs
used for HIV, and large amounts of grapefruit juice increase the risk of
interactions. Fluvastatin, pravastatin, and rosuvastatin are not metabolized
by the cytochrome system and are least affected by other drugs. Gemfibrozil
inhibits the metabolism of statins and increases the risk of rhabdomyolysis
when used in combination therapy.21,22
The monitoring of creatine
phosphokinase (CPK) in patients taking statins remains controversial, and
there is no evidence that routine monitoring of CPK reduces the risk of
myopathy.23 However, baseline CPK does allow a comparison with
subsequent levels if a patient develops myalgia.24 CPK levels
should be assessed in patients who develop unexplained muscle pain/discomfort,
generalized weakness, or brown urine.23 Elevations in transaminase
levels typically occur during the first three months of therapy, and though
usually asymptomatic, should be monitored.20,21
Some patients who cannot
tolerate one statin may tolerate another. Because more patients are now
eligible for statin therapy, this increases the risk of drug interactions and
adverse reactions in a population that is on multiple medications.
Support Systems Enhance
Compliance
Support systems are
available to enhance patient adherence to treatment; for example, some
providers have the option to refer for multidisciplinary services like
nutrition or lipid clinics run by pharmacists. Individual pharmacists can also
enhance patient adherence.
Nutritional Education:
There is evidence from dietary studies that supports the reduction of LDL
cholesterol based on therapeutic lifestyle changes. A meta-analysis showed
NCEP's Step I and II diets lower LDL cholesterol by 12% to 16%.12
Factors that increase LDL cholesterol include saturated and trans fatty
acids, overweight, and dietary cholesterol. Nutritional counseling should
focus on the intake of heart-healthy foods and calorie restriction to improve
LDL cholesterol and body weight. In addition to dietary changes, the
beneficial effects of exercise are well documented and should be encouraged in
all patients.11 Lifestyle changes should include smoking cessation,
weight management, aerobic activity (30 minutes daily, most days of the week),
diet, and limiting alcohol consumption. Ongoing nutritional counseling, in
addition to an initial consultation, is key to achieving LDL cholesterol goals.
Lipid Clinics:
There is a documented increase in compliance when patients are followed by
pharmacist-managed clinics. A study at two Veterans Affairs medical centers in
Texas compared a pharmacist-managed dyslipidemia clinic with usual care
provided by other health professionals. The study found that two-thirds of
patients enrolled in the lipid clinics had an LDL cholesterol level at or
below the NCEP target compared to 16% of patients who received usual care.
Interestingly, 94% of patients in the lipid clinic were on lipid-lowering
agents, compared to 24% of patients receiving usual care.25 Other
studies have documented improvement in glycosylated HbA1c, blood pressure, and
LDL cholesterol in patients followed by a pharmacist-run diabetes drug therapy
program.26 The literature and NCEP supports pharmacist management
of lipids to increase compliance and achieve LDL cholesterol goals.27
Other systems that help
pharmacists enhance patients' adherence to treatment allow tracking of refill
history to assess compliance and accessing cholesterol lab values to review
with patients. Other supportive steps pharmacists can take include simplifying
regimens to reduce cost and/or number of medications, issuing refill reminders
to patients by phone or mail, and discussing adherence with patients at every
visit.
Conclusion
The data clearly
show that aggressive treatment is needed to achieve LDL cholesterol goals and,
in turn, reduce coronary heart disease mortality. Pharmacists have a unique
opportunity to enhance cholesterol management by educating patients and
providers about treatment guidelines and medications. A collaborative approach
may help meet the patient's need for more extensive counseling regarding
lifestyle changes and medications. Pharmacists have the skills to recommend
optimal drug therapy and enhance patient compliance.
References
1. American Heart Association. Heart disease and stroke statistics–2007 update. Available at: http://www.americanheart.org/presenter.jhtml?identifier=300090. Accessed December 11, 2006.
2. American Diabetes Association. Diabetes and cardiovascular disease toolkit. Available at http://www.diabetes.org/for-health-professionals-and-scientists/CVD.jsp. Accessed December 11, 2006.
3. Jacobs MJ, Kleisli T, Plo JR, et al. Prevalence and control of dyslipidemia among persons with diabetes in the United States. Diabetes Res & Clin Pract.. 2005;70:263-269.
4. Grundy SM, Cleeman JI, Merz CN, et al. Implications of recent clinical trials for the National Cholesterol Education Program adult treatment panel III guidelines. Circulation. 2004;110:227-239.
5. Shepherd J, Barter P, Carmenza R, et al. Effect of lowering LDL cholesterol substantially below currently recommended levels in patients with coronary heart disease and diabetes: the Treating to New Targets (TNT) study. Diabetes Care. 2006;29:1220-1226.
6. Pearson TA, Laurora I, Chu H, Kafonek S. The Lipid Treatment Assessment Project (L-Tap): a multicenter survey to evaluate the percentages of dsylipidemic patients receiving lipid-lowering therapy and achieving low-density lipoprotein cholesterol goals. Arch Intern Med. 2000;160:459-467.
7. Johnson ML, Pietz K, Battleman DS, Beyth RJ, et al. Therapeutic goal attainment in patients with hypertension and dyslipidemia. Med Care. 2006;44:39-46.
8. Schultz JS, O'Donnell JC, McDonough KL, Meyer J. Determinants of compliance with statin therapy and low-density lipoprotein cholesterol goal attainment in a managed care population. Am J Manag Care 2005;11:306-312.
9. Rondina MT, Zebrack JS. Achieving National Cholesterol Education Program goals in coronary artery disease. Prev Cardio. 2005;8:18-22.
10. Fletcher B, Berra K, Ades P, Braun LT. Managing abnormal blood lipids A collaborative approach Circulation. 2005;112:3184-3209.
11. Executive Summary of the Third Report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III). JAMA. 2001;285:2486-2497.
12. Kennedy AG, Maclean CD, Littenberg B. et al. The challenge of achieving national cholesterol goals in patients with diabetes. Diabetes Care. 2005;28:1029-1034.
13. Ellis JJ, Erickson SR, Stevenson SR et al. Suboptimal statin adherence and discontinuation in primary and secondary prevention populations. J Gen Intern Med. 2004;19:638-645.
14. Jackevicius CA, Mamdani M, Tu JV. Adherence with statin therapy in elderly patients with and without acute coronary syndromes. JAMA. 2002;288:462-467.
15. Parris ES, Lawerence DB, Mohn LA, Long LB. Adherence to statin therapy and LDL cholesterol goal attainment by patients with diabetes and dyslipidemia. Diabetes Care. 2005;28:595-599.
16. Lee JK, Grace KA, Taylor AJ. Effect of a pharmacy care program on medication adherence and persistence, blood pressure and low-density lipoprotein cholesterol. JAMA. 2006;296:2563-2571.
17. Cholesterol rethink for high-risk patients. Medical Lett Drugs Ther. 2004;46:37-39.
18. Pearson TA, Denke MA, McBride PE, et al. A community-based randomized trial of ezetimibe added to statin therapy to attain NCEP ATP III goals for LDL cholesterol in hypercholesterolemic patients: the ezetimibe add-on to statin for effectiveness (EASE) trial. Mayo Clinic Proc. 2005;80:587-595.
19. National Institutes of Health. National Heart, Lung and Blood Institute National Cholesterol Education Program. Third Report of the Expert Panel on Detection, Evaluation and Treatment of High Blood Cholesterol in Adults. Available at: http://www.nhlbi.nih.gov/guidelines/cholesterol. Accessed December 11, 2006.
20. Koda-Kimble MA, Young LY, Kradjan WA, et al. Applied Therapeutics. 8th ed. Baltimore: Lippincott Williams & Wilkins; 2004:13, 28, 29.
21. Drugs for lipids. Treat Guidel Med Lett2005;3:15-22.
22. Bellosta S, Paoletti R, Corsini A. Safety of statins-focus on cinical pharmacokinetics and drug interactions. Circulation.2004;109[suppIII]:III-50-III-57.
23. Pasternak RC, Smith SC, Bairey-Merz CN, et al. ACC/AHA/NHLBI clinical advisory on the use and safety of statins. Circulation. 2002;106:1024-1028.
24. How to monitor for myopathy in patients taking statins. Pharmacist's Letter. 2006;22:220310.
25. Mazzolini TA, Irons BK, Schell EC, Seifert CF. Lipid levels and use of lipid-lowering drugs for patients in pharmacist-managed lipid clinics verus usual care in 2 VA medical centers. J Manag Care Pharm. 2005;11:763-771.
26. McCord AD. Clinical impact of a pharmacist-managed diabetes mellitus drug therapy management service. Pharmacotherapy. 2006;26:248-253.
27. Straka RJ, Taheri R, Cooper,
Smith JC. Achieving cholesterol target in a managed care organization (ACTION)
trial. Pharmacotherapy. 2005;25:360-371.
To comment on this article, contact
editor@uspharmacist.com.





