US Pharm. 2008;33(2):HS-30-HS-33.
Patients
who suffer from certain types of heart conditions are at risk for developing
infective endocarditis (IE) after undergoing invasive dental procedures,
according to the American Heart Association (AHA) and the American Dental
Association (ADA).1 This infection of the myocardium is caused by
the colonization of bacteria in the heart that reach transient high levels in
the bloodstream after soft-tissue manipulation during dental procedures. This
rare condition, previously termed subacute bacterial endocarditis, is
associated with high morbidity and mortality.1 The AHA recommends
that patients with certain types of heart conditions be treated
prophylactically with antibiotics prior to the dental procedure to prevent IE.
1 Recently, the AHA appointed a task force to review and amend the
existing guidelines because of a lack of evidence regarding patients who
acquire IE after dental treatment. As a result, new guidelines for
prophylactic antibiotic treatment of cardiac patients undergoing dental
procedures were issued by the AHA in March 2007.1
The purpose of this article is
twofold: to educate pharmacists about the revised recommendations for
antibiotic prophylaxis for dental patients and to provide a summary of the
AHA's newly updated guidelines.

History
The first AHA
recommendation for the antibiotic prophylaxis of dental patients was made in
1955, when the emergence of IE after a dental procedure was first noted.1
After several revisions were made based on ongoing evaluation of patient
risk, the ADA endorsed the recommendations in 1972, placing heavy
emphasis on the importance of excellent home care and oral hygiene.2
Until the 2007 revisions were made, the most recent version of the guidelines
dated from 1997 and was based on information that was taken from animal
studies and extrapolated to humans.3 The ration!=ale for revising
the 1997 guidelines comes from the theory that IE is more likely to result
from frequent random exposure to oral microbes during daily activities such as
eating, brushing the teeth, and flos!=sing than from exposure occurring during
dental procedures.1
It also is believed that the
risk of adverse effects from antibiotic treatment outweighs the benefit of the
treatment. The ADA further advises that maintenance of good oral health and
daily practice of oral hygiene may decrease the patient's risk of bacteremia.
This may be more important than the antibiotic regimen for preventing IE.
4
Pathogenesis
The pathogenesis of
IE is complex. IE occurs when nonbacterial thrombotic endocarditis (NBTE) is
pres!=ent at a site of endothelial damage or on the surface of one of the
cardiac valves. During certain dental procedures, manipulation of and trauma
to the oral mucosa, soft tissue, or teeth lead to a transient bacteremia. The
most common microbes released into the bloodstream are Streptococcus
viridans species, which are considered normal oral flora. The bacteremia
may be more severe if inflammation of the soft tissues is present; this is
often the case in patients with poor oral health and periodontal problems. The
bacteria adhere to the NBTE and proceed to proliferate within the vegetation,
resulting in clinical IE. Patients experiencing IE present with variable signs
and symptoms; diagnosis of IE is based on the presence of bacteremia, evidence
of active valvu!=litis, the presence of peripheral emboli, and
immunologic vascular phenomena.5
Patients at Risk
Upon reviewing the
existing body of literature and evidence supporting IE acquired following
dental treatment, the AHA Science Advisory and Coordinating Committee removed
from the list many heart conditions previously thought to put patients at high
risk for IE. The heart conditions currently associated with high risk of IE
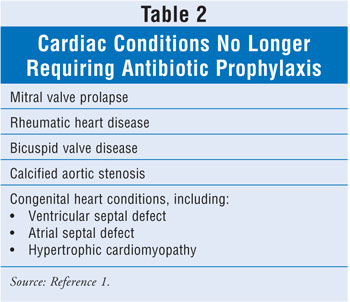
are listed in TABLE 1. The cardiac conditions for which antibiotic
prophylaxis is no longer indicated are specified in TABLE 2.1
It is the hope of the committee that if fewer patients are receiving
prophylaxis, there will be a decrease in adverse outcomes and in the drug
resistance caused by antibiotic therapy.1
Dental Procedures
Studies have shown that 50% of
community-acquired IE cases (not associated with IV drug use) are caused by
viridans group streptococci.6 S viridans is released into
the bloodstream as a result of the manipulation of soft tissues and teeth
during dental procedures and from routine daily brushing and flossing at home.
For healthy patients, this transient bacteremia poses no health threat. Those
patients with the cardiac conditions listed in TABLE 1, however, will
require anti!=biotic treatment prior to specific dental procedures (TABLE 3
); dental extractions and dental prophylaxis were the procedures found to be
most highly associated with bacteremia.7-9
The lack of prospective,
randomized, placebo-controlled studies to determine precisely which dental
procedures cause bacteremia and IE has led to a focus on maintenance of good
oral health as a measure for IE prevention. The ADA currently emphasizes good
oral hygiene and the prevention and treatment of active disease in cardiac
patients to lower their risk of developing IE from bacteremia caused by daily
brushing, flos!=sing, chewing food, and using toothpicks and irrigation
devices.4

Antibiotic Regimen
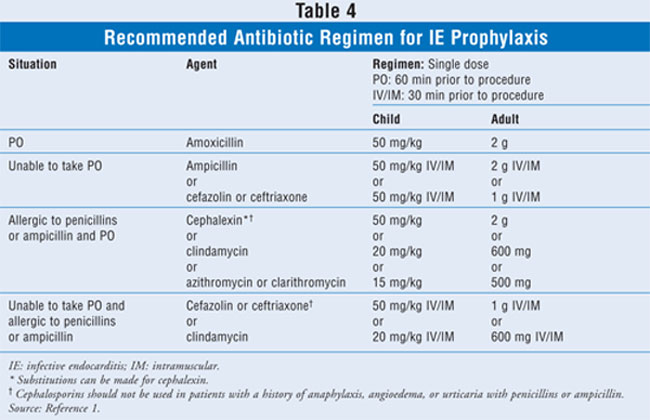
The antibiotic
regimen recommended for IE prophylaxis consists of a single dose 60 minutes
prior to the dental procedure for oral medication, or 30 minutes prior to the
dental procedure for IV or intramuscular medication. If the dose is not given
in this manner, the antibiotic may be administered effectively for up to two
hours after the dental treatment has been rendered. The antibiotics of choice
are targeted to eradicate viridans group streptococci. The antibiotic regimens
recommended for IE prophylaxis are outlined in TABLE 4.
Special Considerations
Several factors
should be taken into consideration when antibiotic prophylaxis is prescribed
for cardiac patients undergoing dental procedures. Cephalosporins should not
be used in patients with a history of anaphylaxis, angioedema, or urticaria
after the use of penicillins or ampicillin. Patients already taking an
antibiotic for another illness should be prescribed a different antibiotic for
dental prophylaxis (e.g., a child who is currently taking amoxicillin for an
ear infection should be prescribed a second agent for dental prophylaxis).
Intramuscular injections should be avoided in patients who are receiving
anticoagulant therapy. Patients who will be undergoing cardiac surgery should
have a preoperative dental evaluation, and all dental treatment should be
completed before the surgery.
Conclusion
Pharmacists play a
crucial role in patient education due to their accessibility and the more
frequent contact they have with patients in the community. They should be
cognizant of the current dental-prophylaxis guidelines and should inform
patients who may have had antibiotics in the past that they no longer require
them prior to dental treatment. Pharmacists also can educate physicians and
dentists who may be unaware of the new guidelines regarding which patients
require IE prophylaxis. Increased awareness of the current recommendations for
prophylaxis may curtail the unnecessary prescribing of antibiotics and lead to
decreased adverse events and antibiotic resistance as physicians and dentists
manage their patients appropriately.
REFERENCES
1. Wilson W, Taubert KA, Gewitz M, et al. Prevention of infective carditis. Guidelines from the American Heart Association. A guideline from the American Heart Association Rheumatic Fever, Endocarditis, and Kawasaki Disease Committee, Council on Cardiovascular Disease in the Young, and the Council on Clinical Cardiology, Council on Cardiovascular Surgery and Anesthesia, and the Quality of Care and Outcomes Research Interdisciplinary Working Group.
Circulation. 2007;116:1736-1754.
2. Rheumatic Fever Committee and the Committee on Congenital Cardiac Defects, American Heart Association. Prevention of bacterial endocarditis.
Circulation. 1972;46:S3-S6.
3. Dajani AS, Taubert KA, Wilson W, et al. Prevention of bacterial endocarditis: recommendations by the American Heart Association. JAMA. 1997;277:1794-1801.
4. American Dental Association. Antibiotics and your heart. Available at: www.ada.org/public/topics/antibiotics/asp. Accessed October 5, 2007.
5. Baddour LM, Wilson WR, Bayer AS, et al. Infective endocarditis: diagnosis, antimicrobial therapy, and management of complications: a statement for healthcare professionals from the Committee on Rheumatic Fever, Endocarditis, and Kawasaki Disease, Council on Cardiovascular Disease in the Young, and the Councils on Clinical Cardiology, Stroke, Cardiovascular Surgery and Anesthesia. Circulation. 2005;111:e394-e434.
6. Fowler VG, Scheld WM, Bayer AS. Endocarditis and intravascular infections. In: Mandell GL, Bennett JE, Dolin R, eds. Principles and Practices of Infectious Diseases. Philadelphia, PA: Elsevier Churchill Livingstone; 2005:975-1021.
7. Lockhart PB. The risk of endocarditis in dental practice. Periodontology 2000. 2000;23:127-35.
8. Conner HD, Haberman S, Collings CK, Winford TE. Bacteremia following periodontal scaling in patients with healthy appearing gingiva. J Periodontol. 1967;38:466-472.
9. Lockhart PB, Brennan MT, Fox PC,
et al. Decision-making on the use of antimicrobial prophylaxis for dental
procedures: a survey of infectious disease consultants and review. Clin
Infect Dis. 2002;34:1621-1626.
To comment on this article, contact
editor@uspharmacist.com.





