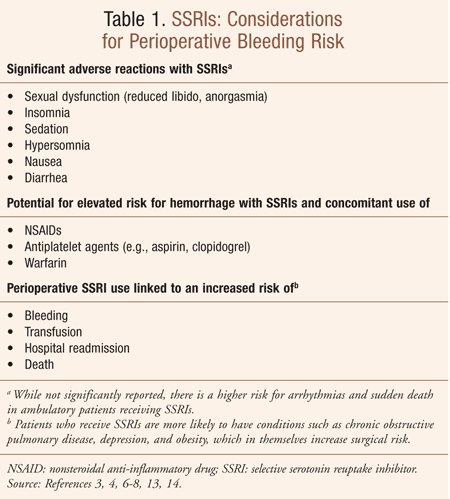
Selective serotonin reuptake inhibitors (SSRIs) are among the most commonly prescribed medications in the United States. With regard to the treatment of depression in the elderly, these agents are frequently considered the preferred choice over other classes of antidepressants owing to their more favorable safety profile.1,2 While the SSRI-associated elevated risk for hemorrhage has been small, it is particularly attributed to the concomitant use of nonsteroidal anti-inflammatory drugs (NSAIDs) or warfarin.3,4 Recent research has shown that perioperative use of SSRIs has been associated with a higher risk for adverse events and a range of poorer outcomes after surgery (TABLE 1).3,4 This article will focus on the concern of many pharmacists and other healthcare practitioners as to whether or not there is a need to modify SSRI therapy, particularly in the perioperative period, to address these potential adverse events.
Effects of SSRIs on Platelet Function
SSRIs selectively inhibit presynaptic serotonin (5-HT) reuptake.2 Generally, it is supposed that SSRIs increase the risk of abnormal bleeding events by inhibiting the uptake of serotonin into platelets, thus leading to impairment in the platelet hemostatic response.5 At this time, it appears that serotoninergic mechanisms play an important role in hemostasis.1 A prothrombotic state may result from abnormal activation, which may occur in patients with major depressive disorder, whereas patients treated with SSRIs experience down-regulation which may lead to one of the following possible consequences: 1) an increased risk of bleeding or 2) a reduction in thrombotic risk.1 Both of the aforementioned clinical consequences are of particular interest in the elderly population.1 With the use of SSRIs, epidemiologic evidence has provided a variety of results from populations including the elderly, and generally supports a moderately increased risk of bleeding that may be critically dependent on the susceptibility of the patient and the presence of risk factors.1 One epidemiologic study including patients 50 years of age or older who were discharged from the hospital following acute myocardial infarction (MI), showed that patients taking an SSRI together with aspirin or dual antiplatelet therapy (aspirin plus clopidogrel) following acute MI were at increased risk of bleeding.6
Perioperative Use of SSRIs
Results of a recent retrospective study by Auerbach et al showed that compared with non-SSRI users, patients who received SSRIs perioperatively had higher overall mortality and higher odds of bleeding.3,4 Sertraline was the most commonly used SSRI, followed by escitalopram, fluoxetine, paroxetine, citalopram, and fluvoxamine; 13.7% of the patients received an SSRI perioperatively. The researchers report that, based on data from this large multicenter (375 hospitals) study involving more than 500,000 adult patients and a broad range of surgical procedures and surgeons, results suggest that SSRIs are associated with a range of poorer outcomes after major surgery; these agents have been linked to an increased risk of bleeding, transfusion, hospital readmission, and death.3,4 SSRIs have previously been linked to an increased bleeding risk in coronary bypass surgery and orthopedic surgical procedures.3,4 Case studies of hemorrhage have also been reported subsequent to orbital surgery (i.e., hematoma with SSRI use) and oral surgery (i.e., SSRI plus NSAID use).7,8 Of note, patients taking SSRIs are more likely to have conditions such as chronic obstructive pulmonary disease, depression, and obesity, which in themselves increase surgical risk; SSRIs have also been linked to a higher risk for arrhythmias and sudden death in ambulatory patients.3,4 Therefore, while receiving SSRIs in the perioperative period is associated with a higher risk for adverse events, determining whether patient factors or SSRIs themselves are responsible for elevated risks requires well-designed prospective study.
SSRIs and Concomitant Warfarin
Warfarin is frequently used as concomitant therapy with antidepressants; however, researchers conducting a recent study indicated that it has been unclear whether concomitant use increases the risk of bleeding beyond that with warfarin alone.9 Study data indicate that the use of any antidepressant with warfarin was not associated with the incidence of any bleeding or major bleeding during the 6-month period; however, the use of an SSRI with warfarin was associated with an increase in any bleeding event.9 After accounting for other factors associated with bleeding risk, the use of an SSRI remained a significant predictor of bleeding. The conclusions drawn state that it is important to clarify the interaction between warfarin and SSRIs with regard to bleeding risk given the high frequency of their concomitant use.9
Appropriate Course of Action
Should an SSRI Be Held Prior to Surgery? The question of whether or not to hold an SSRI perioperatively has been discussed in the literature with regard to previous data and the recent large retrospective study mentioned above. Auerbach et al note that holding SSRI therapy at the time of surgery may be an appropriately conservative approach.3 However, Mrkobrada and Hackam maintain that owing to the observational nature of the aforementioned study, the recent findings to date do not warrant changes in practice—that risk for the average patient, even if a causal relationship exists, would be very small.4,10 Further, the cessation of an SSRI before surgery may potentially precipitate a discontinuation syndrome, which may exacerbate depression and increase sensitivity to postoperative pain. Rather, Mrkobrada and Hackam4,10 suggest that
• SSRI therapy only be initiated when clinically indicated
• Internists, anesthesiologists, and surgeons should be aware of potential perioperative SSRI-associated bleeding risks
• To date, the evidence base has not evolved sufficiently to confirm routine tapering or discontinuation of SSRI therapy before surgery.
While there is at present no uniform recommendation for which patients should stop taking an SSRI prior to surgery and which should not, suggested variables to consider include the type of surgical procedure (e.g., associated with a large amount of blood loss), the type of SSRI (as determined by half-life), and the severity of the patient’s condition, such as depression or anxiety, for which the SSRI is prescribed.11 It is suggested that, in some cases, tailoring the adjustment of the SSRI to the individual may be achieved by holding the SSRI for one week prior to the surgical procedure; or, that the dose may be lowered if the surgery is associated with a substantial amount of blood loss.11 Furthermore, it is suggested that a discussion regarding the potential for adverse bleeding events take place between prescriber and patient and possibly even between prescriber and surgeon if deemed necessary.11
Acid Suppression: To date, study data have provided tips to guide clinicians in taking the most appropriate course of action.1 Considering age-associated increased risk of gastrointestinal (GI) bleeding, it would be prudent to suggest the addition of an acid-suppressing agent, such as a proton pump inhibitor, to the medication regimen of seniors in whom SSRIs are indicated.1 Epidemiologic evidence indicates that the risk of SSRI-associated GI bleeding is increased with the concurrent use of NSAIDs, anticoagulants, and antiplatelet agents and is decreased by concurrent proton pump inhibitors.5 Of note, the risk of bleeding has also been shown to be increased in patients with cirrhosis of the liver or liver failure.5 Acid-suppression consideration would be appropriate for high-risk patients such as those with a prior history of upper-GI bleeding or peptic ulcer, and in individuals who take corticosteroids, oral anticoagulants, antiplatelet drugs, or NSAIDs; the elderly are a high-risk population for adverse effects from NSAIDs, with up to 60% developing peptic ulceration and/or hemorrhage asymptomatically.1,2 Consideration of individual patient factors and the medications that may potentiate risk is required to tailor perioperative pharmaceutical care for the individual patient.12
Conclusion
While a large national retrospective study has shown that SSRIs are associated with bleeding risk and increased risk for adverse effects perioperatively, prospective study is required to ultimately determine whether specific patient factors or the SSRIs are responsible for the elevated risks. While there is no consensus thus far as to whether routine holding of an SSRI is warranted perioperatively, an increased awareness of the issue by pharmacists, surgeons, and other healthcare practitioners is warranted. At this time, it is worthwhile for pharmacists in all practice settings who care for an individual taking an SSRI to tailor pharmaceutical care services, with special consideration given to patient factors, risk factors, and the particular SSRI.
REFERENCES
1. de Abajo FJ. Effects of selective
serotonin reuptake inhibitors on platelet function: mechanisms, clinical
outcomes and implications for use in elderly patients. Drugs Aging. 2011;28(5):345-367.
2. Semla TP, Beizer JL, Higbee MD. Geriatric Dosage Handbook. 18th ed. Hudson, OH: Lexi-Comp, Inc; 2013.
3. Auerbach AD, Vittinghoff E, Maselli J, et al.
Perioperative use of selective serotonin reuptake inhibitors and risks
for adverse outcomes of surgery. JAMA Intern Med. 2013;173(12):1075-1081.
4. SSRIs linked to bleeding risk, death in surgical patients. Medscape. Apr 30, 2013. www.medscape.com/viewarticle/803334. Accessed October 4, 2013.
5. Andrade C, Sandarsh S, Chethan KB, et
al. Serotonin reuptake inhibitor antidepressants and abnormal bleeding: a
review for clinicians and a reconsideration of mechanisms. J Clin Psychiatry. 2010;71(12):1565-1575.
6. Labos C, Dasgupta K, Nedjar H, et al.
Risk of bleeding associated with combined use of selective serotonin
reuptake inhibitors and antiplatelet therapy following acute myocardial
infarction. CMAJ. 2011;183(16):1835-1843.
7. Van Cann EM, Koole R. Retrobulbar hematoma associated with selective serotonin reuptake inhibitor: a case report. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009;108(4):e1-e2.
8. Van Cann EM, Koole R. Abnormal
bleeding after an oral surgical procedure leading to airway compromise
in a patient taking a selective serotonin reuptake inhibitor and a
nonsteroidal antiinflammatory drug. Anesthesiology. 2008;109(3):568-569.
9. Cochran KA, Cavallari LH, Shapiro NL, et al. Bleeding incidence with concomitant use of antidepressants and warfarin. Ther Drug Monit. 2011;33(4):433-438.
10. Mrkobrada M, Hackam DG. Abstract, Commentary. JAMA Intern Med. 2013;173(12):1082-1083.
11. Some antidepressants linked to
surgical risks. Depression Health Center. WebMD.com. April 29, 2013.
www.webmd.com/depression/news/20130429/some-antidepressants-linked-to-bleeding-risk-with-surgery.
Accessed October 10, 2013.
12. American Society of Health-System
Pharmacists. Best Practices for Hospital & Health-System Pharmacy.
2011-2012 ed. Bethesda, MD: American Society of Health-System
Pharmacists; 2012:327-334.
13. Umland EM, Weinstein LC, Buchanan EM. Menstrual-related disorders. In: DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 8th ed. New York, NY: McGraw-Hill Inc; 2011:1393-1407.
14. Tata LJ, Fortun PJ, Hubbard RB, et
al. Does concurrent prescription of selective serotonin reuptake
inhibitors and non-steroidal anti-inflammatory drugs substantially
increase the risk of upper gastrointestinal bleeding? Aliment Pharmacol Ther. 2005;22(3):175-181.
To comment on this article, contact rdavidson@uspharmacist.com.





