US Pharm. 2016;41(11):34-37.
ABSTRACT: Bipolar disorder is a chronic illness that causes periodic shifts in mood through episodes of dysthymia, depression, hypomania, and mania. There are two major types of bipolar disorder: bipolar I disorder, which is characterized by the presence of at least one acute manic episode, and bipolar II disorder, which is typified by hypomania and longer depressive episodes and is sometimes misdiagnosed as major depressive disorder. Pharmacotherapeutic options include lithium, anticonvulsants, antipsychotics, and antidepressants. Pharmacists play a role in ensuring proper dosing regimens, checking for drug interactions, and monitoring for potential drug toxicity. When counseling patients, pharmacists should review optimal administration times and potential side effects to make certain that the patient has a comprehensive understanding of how to manage symptoms.
Bipolar disorder is a chronic illness that causes periodic shifts in mood through episodes of dysthymia, depression, hypomania, and mania. There are two major types of bipolar disorder. Bipolar I disorder (BD I) involves the presence of at least one acute manic episode, whereas bipolar II disorder (BD II) is characterized by hypomania and longer depressive episodes. Because it involves longer depressive episodes, BD II is sometimes misdiagnosed as major depressive disorder (MDD). It is estimated that patients with BD I are depressed for a maximum of 3 weeks for every week of hypomania, whereas patients with BD II are depressed for 37 weeks for every week of hypomania.1 Patients who are misdiagnosed with MDD and are accordingly prescribed antidepressants are at heightened risk for a rapid switch to mania.2 Pharmacists can help patients develop a thorough history of their mood episodes so that an accurate diagnosis of the patient’s psychiatric disorder can be made.
EPIDEMIOLOGY
Symptoms of bipolar disorder typically present in early adulthood. Bipolar disorder affects about 2% of the world’s population, with 1% diagnosed as BD I and 1.1% as BD II.1,3 BD I is equally present in men and women, but BD II occurs more frequently in women.4 BD II is slightly more common than BD I, but it is difficult to obtain an accurate percentage of patients because BD II is commonly misdiagnosed as MDD.
ETIOLOGY AND PATHOPHYSIOLOGY
The exact etiology of bipolar disorder is not known, as there are no significant differences in the pathogenesis of bipolar disorder based on race, ethnicity, or gender. There are genetic studies that show an increased frequency of bipolar disorder in individuals who have first-degree relatives with bipolar disorder.3 The leading causes of bipolar disorder include environmental triggers, an imbalance of neurotransmitters and neurohormones, and genetics.3
TREATMENT APPROACH
The optimal treatment approach for bipolar disorder includes a combination of pharmacologic and nonpharmacologic therapies. Targeted psychosocial therapy combined with pharmacologic treatment offers substantial benefit compared with pharmacologic treatment alone. Forms of psychotherapy for bipolar disorder include individual and group psychoeducation, family-focused therapy, and cognitive-behavioral therapy.1
PHARMACOTHERAPY
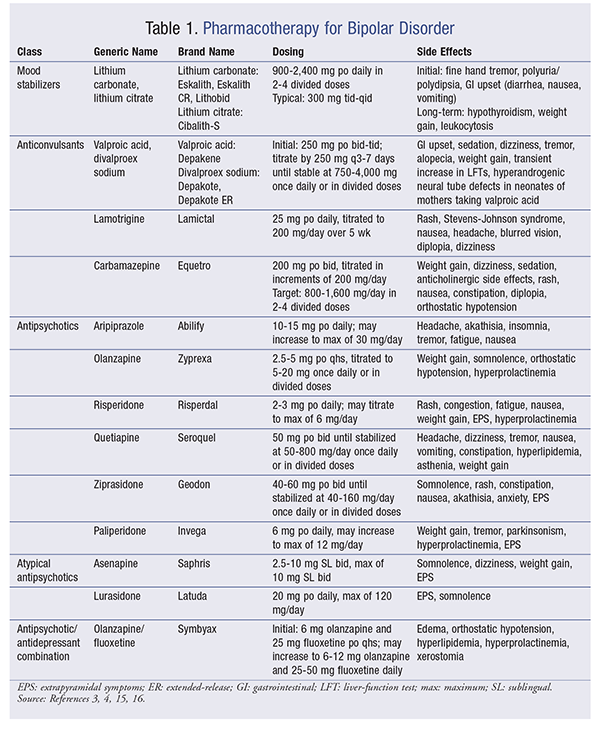
Pharmacotherapeutic agents necessary for the successful management of bipolar disorder include mood stabilizers, atypical antipsychotics, and antidepressants (TABLE 1). Medications approved by the FDA for managing both manic and depressive episodes include lithium salts, anticonvulsants (valproic acid, carbamazepine, and lamotrigine), and atypical antipsychotics (aripiprazole, asenapine, olanzapine, combination olanzapine and fluoxetine, lurasidone, paliperidone, quetiapine, risperidone, and ziprasidone). The goal for managing acute manic phases is symptom reduction, with the long-term objective of full remission.5 In the treatment of depressive episodes, the primary goal comprises the remission of depressive symptoms and the reduction of hypomanic, manic, or mixed manic episodes. Maintenance therapy aims to prevent the development of mood episodes.
Lithium
Lithium is the first-line choice for preventing mood instability and treating mania. This agent is successful in treating aggressive behavior during acute manic episodes, and it is also the most successful long-term treatment for bipolar disorder. Lithium is effective as monotherapy in the depressive phase, with approximately 60% to 80% of patients demonstrating an improvement in symptoms.8 Depressive symptoms may require up to 6 to 8 weeks of continuous treatment for improvement, so if a patient’s depressive symptoms require a short onset of response, lithium should be administered with antidepressants or other mood stabilizers.9 Lithium also has provided the strongest evidence for reducing the risk of suicide in bipolar disorder,5 demonstrating an eight- to 10-fold reduction in suicide rates.10
Dosing of lithium in average-sized healthy adults is initiated at 300 mg two to three times daily, but elderly patients should be started on 150 mg once daily or twice daily.3 The dosage may be increased by 300 to 600 mg every 1 to 5 days, depending on how well the medication is tolerated. The target dosage, which is typically 900 to 2,400 mg per day, may be divided into multiple doses. Patients should be closely monitored when dosage increases are made because lithium has a very narrow therapeutic index (usual therapeutic levels of 0.6-1.2 mEq/L, toxic levels >1.5 mEq/L). Serum lithium levels should be checked approximately 5 days after any dosing adjustment and monitored at least every 6 months in stable patients. Patients who experience frequent mood episodes should be monitored every 1 to 2 months.
The most commonly reported initial side effects associated with lithium include gastrointestinal upset (nausea, vomiting, diarrhea), intention tremor of the hand, polyuria, and polydipsia. Patients taking lithium who show symptoms of confusion, ataxia, or slurred speech may be experiencing lithium toxicity and require medical attention. More severe effects associated with long-term use of lithium include leukocytosis, hypothyroidism, weight gain, acne, nephropathy, and cardiac-rhythm disturbances.
Anticonvulsants
Valproic Acid: This agent is indicated for the treatment of acute manic episodes in either BD I or BD II, but it is mainly used as maintenance monotherapy.3 Compared with lithium, valproic acid has a more rapid onset of action in the treatment of acute mania, and it is the most commonly used mood stabilizer.5 Valproic acid should not be used in pregnant patients because many cases of fetal neural-tube defects have been reported.3 Patients should be started on valproic acid 250 to 500 mg per day, divided into multiple doses, and the dosage should gradually be increased to 750 to 4,000 mg per day to produce therapeutic serum levels of 50 to 125 mcg/mL.9 Serum levels of valproic acid should be checked every 6 to 12 months, and more often if a patient experiences frequent mood episodes. Side effects reported in patients taking valproic acid include gastrointestinal upset (vomiting), sedation, dizziness, tremor, alopecia, weight gain, and transient increases on liver-function tests. If a patient experiences an abnormal level of gastrointestinal discomfort, he or she should be switched from valproic acid to extended-release divalproex. Depakote is enteric-coated, so patients should be counseled on the risk of stomach irritation with concurrent use of antacids.3 If valproic acid is used for long-term treatment, the patient should be closely monitored every 6 to 12 months for signs of hepatic failure, thrombocytopenia, or pancreatitis.
Lamotrigine: Lamotrigine is most effective for treating depressive episodes associated with BD I. It also has been efficacious, in rapid-cycling BD II, as an adjunct medication for preventing the recurrence of depressive episodes.10 Lamotrigine should be started at 25 mg daily for 2 weeks, increased to 50 mg daily for 2 weeks, and then increased by 50 mg weekly until a target dose of 200 mg is achieved. The most commonly reported side effects of lamotrigine include rash, sedation, headache, dizziness, nausea, ataxia, diplopia, and blurred vision.3 In more extreme cases, instances of life-threatening effects, such as the skin disorders Stevens-Johnson syndrome and toxic epidermal necrolysis, have been reported. If a patient experiences rash while taking lamotrigine, these skin disorders should be ruled out by the primary care physician.
Carbamazepine: Carbamazepine is effective for manic and depressive phases of BD I, and it is also a useful alternative for patients with rapid-cycling bipolar disorder who do not respond to lithium. Carbamazepine should be started at 100 to 200 mg once or twice daily and increased by 200 mg every 1 to 4 days until a target dosage of 800 mg to 1,600 mg per day is reached.3 Since carbamazepine will increase its own metabolism and that of other CYP450-metabolized drugs, the patient should be closely monitored when carbamazepine is used with other medications metabolized by CYP450, especially those affected by CYP1A2, CYP2C9, or CYP3A4.3 The most common side effect of carbamazepine is constipation. Patients may also experience sedation, dizziness, nausea, vomiting, dry mouth, blurred vision, rash, weight gain, pruritus, ataxia, or diplopia. Carbamazepine has been associated with increased incidences of Stevens-Johnson syndrome and toxic epidermal necrolysis. Patients of Asian descent are more likely to develop these conditions because they possess the HLA-B*1502 allele, so they should be educated about genomic testing. A patient with signs of developing rash should contact his or her primary care physician to rule out the possibility of these skin disorders.
Antipsychotics
An antipsychotic may be used as monotherapy or as an adjunct to other treatments for bipolar disorder. A mood stabilizer, such as lithium or valproic acid, in combination with an antipsychotic frequently is used for treatment of mania with psychotic features because this combination provides greater efficacy than either agent used alone.3 If a patient experiences a severe depressive episode, either the dosage of the mood stabilizer should be increased or another antipsychotic should be added. Olanzapine is a first-line agent or adjunctive treatment because of its efficacy against acute mania associated with agitation, aggression, or psychosis. Whenever an antipsychotic is used as monotherapy, the dosage should be increased if the patient experiences frequent manic episodes.11
Treatment for acute bipolar depression is more challenging than that for acute mania because of the controversy surrounding the role of antipsychotics. Only quetiapine is FDA-approved as monotherapy for treating bipolar depression.3 Quetiapine has a relatively fast onset of action, which enables the early initiation of treatment in the case of quickly worsening depression.1 Symbyax (olanzapine/fluoxetine) is FDA-approved to treat acute depressive episodes associated with BD I in adults, but its adverse effects of weight gain, risk of diabetes, and hypertriglyceridemia render it more appropriate as a second-line option.12
Second-generation long-acting injectable (LAI) antipsychotics may be effective for reducing relapses of bipolar disorder. Risperidone LAI is indicated as monotherapy or as adjunctive therapy to lithium or valproate for maintenance treatment of BD I. This medication also reduces the rate of relapse and better controls clinical symptoms compared with the oral formulation or placebo injection.13 More studies are needed to determine the usefulness of new LAIs, such as olanzapine pamoate and aripiprazole. The risks versus benefits of long-term treatment with antipsychotics should be periodically evaluated. A major adverse effect of atypical antipsychotics is the development of metabolic syndrome, which may include weight gain, diabetes mellitus, and hyperlipidemia.2 Hyperprolactinemia and extrapyramidal symptoms also may develop. Patients should be regularly monitored for all of these adverse effects.3 Tapering should also be taken into account when the dosage of an antipsychotic is being increased or decreased.
Antidepressants
The utility of antidepressants for bipolar disorder is controversial because there are limited studies supporting its use. Antidepressants are rarely used with mood stabilizers to treat bipolar mania or depression because they can cause mania. The rate of mood switching with use of a selective serotonin reuptake inhibitor is about 3.8%, similar to that for placebo.3 Patients who experience rapid cycling should avoid antidepressants entirely.14 Many clinicians consider antidepressants as third-line treatment for bipolar depression. Generally, an antidepressant is used only adjunctively with a mood stabilizer or an atypical antipsychotic, and the dosage should be tapered after the depressive episode subsides. The antidepressant should be gradually withdrawn 2 to 6 months after remission while the patient is continuing on a mood stabilizer.
ROLE OF THE PHARMACIST
Pharmacists have a role in promoting the importance of medication adherence and educating patients about how to recognize triggers for their mood episodes. Pharmacists can use motivational interviewing techniques to help patients become comfortable with their diagnosis, educate them about the effectiveness and adverse effects of their medications, and encourage them to take responsibility for managing their condition. Reviewing optimal administration times and potential side effects with patients will help pharmacists improve adherence in patients and reduce the number of hospital visits.
REFERENCES
1. Geddes JR, Miklowitz DJ. Treatment of bipolar disorder. Lancet. 2013;381:1672-1682.
2. Manning JS. Tools to improve differential diagnosis of bipolar disorder in primary care. Prim Care Companion J Clin Psychiatry. 2010;12(suppl 1):17-22.
3. Drayton SJ, Pelic CM. Bipolar disorder. In: DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 9th ed. New York, NY: McGraw-Hill Education; 2014:1067-1082.
4. Stovall J. Bipolar disorder in adults: epidemiology and diagnosis. UpToDate. www.uptodate.com/contents/bipolar-disorder-in-adults-epidemiology-and-pathogenesis. Accessed June 26, 2016.
5. McCormick U, Murray B, McNew B. Diagnosis and treatment of patients with bipolar disorder: a review for advanced practice nurses. J Am Assoc Nurse Pract. 2015;27:530-542.
6. Price LH, Heninger GR. Lithium in the treatment of mood disorders. N Engl J Med. 1994;331:591-598.
7. Keck PE, Perlis RH, Otto MW, et al. The Expert Consensus Guideline Series: treatment of bipolar disorder 2004. Postgrad Med Special Report. 2004:1-120.
8. Goodwin FK. Rationale for long-term treatment of bipolar disorder and evidence for long-term lithium treatment. J Clin Psychiatry. 2002;63(suppl 10):5-12.
9. Bowden CL, Brugger AM, Swann AC, et al. Efficacy of divalproex vs lithium and placebo in the treatment of mania. The Depakote Mania Study Group. JAMA. 1994;271:918-924.
10. Vieta E, Valenti M. Pharmacological management of bipolar depression: acute treatment, maintenance, and prophylaxis. CNS Drugs. 2013;27:515-529.
11. Miklowitz DJ, Johnson SL. The psychopathology and treatment of bipolar disorder. Annu Rev Clin Psychol. 2006;2:199-235.
12. Symbyax (olanzapine and fluoxetine) package insert. Indianapolis, IN: Eli Lilly and Co; January 2015.
13. Chou YH, Chu PC, Wu SW, et al. A systemic review and experts’ consensus for long-acting injectable antipsychotics in bipolar disorder. Clin Psychopharmacol Neurosci. 2015;13:121-128.
14. Pacchiarotti I, Bond DJ, Baldessarini RJ, et al. The International Society for Bipolar Disorders (ISBD) task force report on antidepressant use in bipolar disorders. Am J Psychiatry. 2013;170:1249-1262.
15. Saphris (asenapine) package insert. St. Louis, MO: Forest Laboratories, LLC; March 2015.
16. Latuda (lurasidone HCl) package insert. Marlborough, MA: Sunovion Pharmaceuticals Inc; July 2013.
To comment on this article, contact rdavidson@uspharmacist.com.





