Over 50 million Americans are affected by chronic pain, and musculoskeletal pain is especially common.1,2 One area frequently associated with chronic pain and stiffness is the neck, due to degenerative changes in the cervical spine that occur with aging. Chronic pain is a leading cause of disability and is associated with an estimated $100 billion dollars a year in health care costs.3,4
Of concern, however, is that despite the numbers affected and the high costs incurred, numerous studies have reported inadequate pain management in a variety of settings.5-8 It appears the best outcomes have been observed in multidisciplinary pain clinics, but services are not yet widely available.1,9 Therefore, as a result, most patients with chronic pain, including musculoskeletal pain associated with the neck, are managed in primary care.1
The Spine: Structural Component Overview
Comprised of a series of interlocking bones, called vertebrae, the spine is supported by muscles and ligaments. The spine is referred to by its sections known as the cervical (neck) spine, thoracic (upper back) spine, and lumbar (lower back) spine; the sacrum—formed by the fusion of the last five vertebrae—and the coccyx, or tailbone, form a portion of the back wall of a group of relatively flat bones called the pelvis.10 Since the thigh bones insert into sockets in the funnel-shaped pelvis, the pelvis joins the legs to the spine.
I n order for the spine to function mechanically, it affects and is affected by skeletal alignment (e.g., of the foot, knee, and leg), flexibility (e.g., of the hip, lumbar curve), and strength (e.g., of legs, buttocks, abdominal wall) of various parts of the body.10 A series of arches in the vertebrae form the spinal canal, through which descends the spinal cord—a bundle of nerves that is, simply stated, an extension of the brain. Nerves branch off the spinal cord, exiting the spinal column by way of a hole between two vertebrae called an intervertebral foramen. The natural curves of the spine are also an important feature, since alterations to them may lead to dysfunction, pain, and disease.10
Cervical Spondylosis: Signs and Symptoms
With age, degenerative changes in the
cervical vertebrae can lead to a loss of intervertebral height with
narrowing of the central canal and intervertebral foramina.11
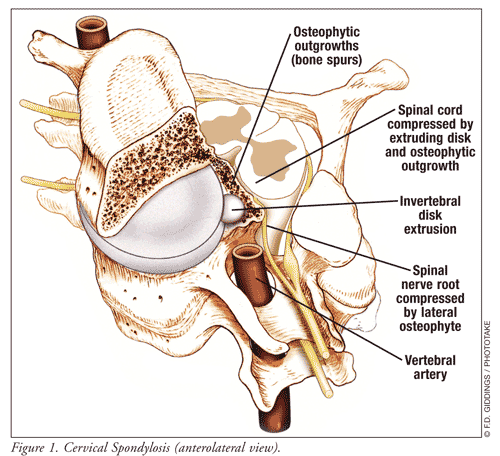
These changes, including dehydrated disks, herniated disks, bone spurs,
and stiff ligaments, are very common, worsen with age, and are referred
to by the general term cervical spondylosis (FIGURE 1).12,13
A neck x-ray will reveal that greater than 90% of senior men and women
aged 65 years and older present with signs of cervical spondylosis and
osteoarthrits.13 If cervical spondylosis causes compression of the spinal cord or nerve roots, permanent nerve damage can ensue.
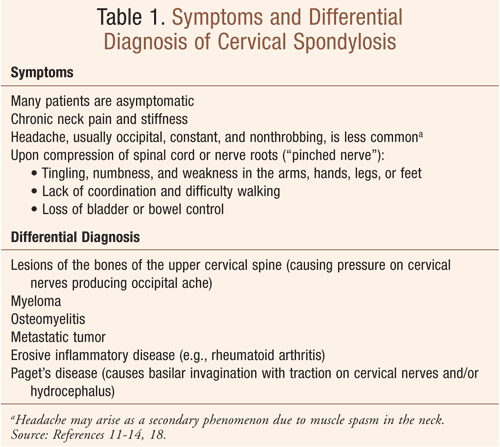
Most patients with cervical spondylosis are asymptomatic.12 Symptoms (TABLE 1) may develop acutely or insidiously and manifest by the fifth or sixth decade of life.12 Upon examination, the patient may have difficulty rotating the head and moving it toward the shoulder.13 Headache, usually occipital, constant, and nonthrobbing, may be less common and arise as a secondary phenomenon due to muscle spasm in the neck.14 Patients should be encouraged to seek medical attention if sudden onset of numbness or weakness occurs, or if there is loss of bladder or bowel control.
Risk Factors
The major risk factor for cervical spondylosis is aging.13,14 The development of this condition is more likely when other factors are present, including obesity and sedentary lifestyle; occupation requiring heavy lifting and frequent bending and twisting; previous neck injury; severe arthritis; osteoporotic fractures; and genetic factors.12,13
Differential Diagnosis and Diagnostic Testing
An x-ray of the skull will usually suffice to rule out other possibilities besides cervical spondylosis (see Differential Diagnosis in TABLE 1) that may cause headache, neck pain and stiffness, and neurologic deficit; if necessary, additional diagnostic testing may include CT scan, MRI, myelograph with contrast, electromyography (EMG), and nerve conduction study.11,12
Treatment
The severity of signs and symptoms
directs the treatment approach for cervical spondylosis with the
following goals: 1) relieve pain; 2) maintain functionality; 3) prevent
permanent nerve damage. Patients with mild cases may respond to
conservative interventions such as regular exercise (see RESOURCES FOR THE PATIENT
),
OTC analgesics (ibuprofen, naproxen, acetaminophen), and heat or ice
for sore muscles; a soft cervical collar may provide rest to the
cervical muscles and should be worn only for short periods so as not to
weaken those muscles.12

When OTC analgesics do not provide adequate pain relief, muscle relaxants (e.g., cyclobenzaprine, methocarbamol), anticonvulsants (e.g., gabapentin, pregabalin), opioids (e.g., hydrocodone, oxycodone), and intra-articular corticosteroid injections (with anesthetic) may be necessary and should be tailored to the individual. Of note, pharmacists are encouraged to review Reference 15, the American Geriatrics Society Updated Beers Criteria for Potentially Inappropriate Medication Use in Older Adults (from the American Geriatrics Society 2012 Beers Criteria Update Expert Panel) when formulating pharmaceutical care plans for geriatric patients.
Stretching and strengthening cervical muscles and the use of traction to relieve cervical nerve compression may be overseen and taught to patients by a physical therapist. Surgery is considered when conservative measures are inadequate or nerve compression produces symptoms (TABLE 1).
Traumatic Injury-Induced Cervical Vertigo
Neck injury, while a known risk factor for cervical spondylosis, may also induce cervical vertigo triggered by neck movements. Diagnosis of cervical vertigo may be confused with migraine-associated, head movement–induced vertigo.16,17 Cervical vertigo is managed with neck movement exercises as permitted by orthopedic considerations.16,17
Conclusion
Pharmacologic agents for pain management, lifestyle modifications, and other interventions used in the treatment of cervical spondylosis are integral in pharmacists’ role as clinician, educator, and patient advocate. Guiding and counseling patients through medication management and referral for medical attention are important to achieve the goals of therapy for cervical spondylosis, including relief of pain, maintenance of functional ability, and prevention of permanent neurologic damage.
REFERENCES
1. Bair MJ, Matthias MS, Nyland KA, et al. Barriers and facilitators to chronic pain self-management: a qualitative study of primary care patients with comorbid musculoskeletal pain and depression. Pain Med. 2009:10:1280-1290.
2. Peter D. Hart Research Associates. America speaks: pain in America survey. 2003.
www.researchamerica.org/uploads/poll2003pain.pdf. Accessed February 19, 2013.
3. Stewart WF, Ricci JA, Chee E, et al. Lost productive time and cost due to common pain conditions in the U.S. workforce. JAMA. 2003;290:2443-2454.
4. Turk DC, Okifuji A, Kalauolalani D. Clinical outcome and economic evaluation of multidisciplinary pain centers. In: Block AR, Kremer EF, Fernandez E, eds. Handbook of Pain Syndromes: Biopsychosocial Perspectives. Mahwah, NJ: Erlbaum; 1999:77-98.
5. Gu X, Belgrade MJ. Pain in hospitalized patients with medical illnesses. J Pain Symptom Manage. 1993;8:17-21.
6. Donovan M, Dillon P, McGuire L. Incidence and characteristics of pain in a sample of medical-surgical inpatients. Pain. 1987;30:69-78.
7. Todd KH, Samaroo N, Hoffman JR. Ethnicity as a risk factor for inadequate emergency department analgesia. JAMA. 1993;269:1537-1539.
8. Cleeland CS, Gonin R, Hatfield AK, et al. Pain and its treatment in outpatients with metastatic cancer. New Engl J Med. 1994;330:592-596.
9. Crook J, Tunks E. Pain clinics. Rheum Dis Clin North Am. 1996;22:599-611.
10. Schatz MP. Back Care Basics: A Doctor's Gentle Yoga Program for Back and Neck Pain Relief. Berkeley, California: Rodmell Press; 1992:9-20.
11. Sandanha GJ. Headache and facial pain. In: Fillit HM, Rockwood K, Woodhouse K, eds. Brocklehurst’s Textbook of Geriatric Medicine and Gerontology. 7th ed. Philadelphia, PA: Saunders Elsevier; 2010:466-477.
12. Cervical spondylosis. Mayoclinic.com. Updated June 12, 2012. www.mayoclinic.com/health/cervical-spondylosis/DS00697. Accessed February 19, 2013.
13. Cervical spondylosis. PubMed Health. U.S. National Library of Medicine, National Institutes of Health. Updated June 4, 2011. www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001472/. Accessed February 19, 2013.
14. Iansek R, Heywood J, Karnaghan J, Balla JI. Cervical spondylosis and headaches. Clin Exp Neurol. 1987;23:175-178.
15. American Geriatrics Society updated Beers Criteria for potentially inappropriate medication use in older adults. American Geriatrics Society 2012 Beers Criteria Update Expert Panel. J Am Geriatr Soc. 2012;60:616-631.
16. Lustig LR, Schindler JS. Ear, nose & throat disorders. In: McPhee SJ, Papadakis MA, Rabow MW, eds. 2011 Current Medical Diagnosis & Treatment. 50th ed. New York, NY: McGraw Hill Medical. 2011:205.
17. Schikora N, Eysel-Gosepath K, Klünter H, et al. Influence of cervical spine stabilization via Stiff Neck on the postural system in healthy patients: compensation or decompensation of the postural system? Eur Arch Otorhinolaryngol. 2010;267:1623-1628.
18. Edmeads J. The cervical spine and headache. Neurology. 1988;38:1874-1878.
To comment on this article, contact rdavidson@uspharmacist.com.





