US Pharm. 2023;48(1):17-28.
ABSTRACT: Epilepsy continues to be one of the most common neurologic disorders in the United States. This complex disorder affecting the central nervous system is characterized by recurrent seizures that are unprovoked by an acute neurologic or systemic insult. In epilepsy, several different types of seizures can occur, with tonic-clonic seizures being the most commonly recognized because of the characteristic signs of jerking and shaking. Epilepsy often requires treatment with antiepileptic drugs, but the use of these medications is not without risks. Because of their high accessibility, community pharmacists can initiate discussions with patients with epilepsy and their family members regarding drug interactions, adverse events, medication adherence, and potential optimization of antiepileptic treatment.
Epilepsy continues to be one of the most common neurologic disorders in the United States.1 Approximately 3.4 million Americans had an active diagnosis of epilepsy in 2015.2 This complex disorder affecting the central nervous system is characterized by recurrent seizures that are unprovoked by an acute neurologic or systemic insult.3 A seizure is “the clinical manifestation of an abnormal, excessive, hypersynchronous discharge of a population of cortical neurons.”3 Epilepsy has a bimodal distribution, meaning that there is a peak in newborns and young children and a second peak occurring in adults aged 65 years and older.4
In epilepsy, several different types of seizures can occur. Partial seizures (i.e., focal seizures) typically start in one part of the brain but can become generalized and spread to other areas. Generalized seizures, which affect both sides of the brain, can be further divided into several categories: tonic-clonic, absence, myoclonic, and atonic. Tonic-clonic seizures (also known as grand mal seizures) are the most commonly recognized type because of the characteristic signs of jerking and shaking. Absence seizures involve rapid blinking or staring off into space. Myoclonic seizures are characterized by short jerking motions in different parts of the body, commonly the extremities. Atonic seizures cause the muscles of the body to relax.5
An analysis of data from the 2013 and 2015 CDC National Health Interview Surveys revealed that 90% of U.S. adults who reported having active epilepsy were taking antiepileptic medications.6 Just 44% of those patients taking antiepileptic drugs (AEDs) reported that their seizures were currently controlled. Patients who had an annual follow-up with a specialist were found to have a higher rate of AED use.6 A CDC report from 2010 determined that epilepsy accounted for $15.5 billion in direct and indirect costs each year.6
Community Pharmacists’ Knowledge About Epilepsy Treatment
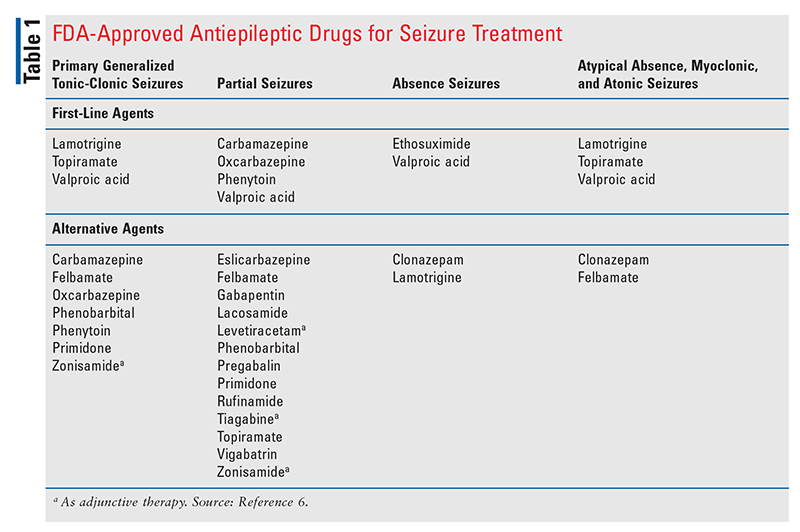
Epilepsy often requires treatment, which may include AEDs, surgery, and nonpharmacologic procedures such as vagus nerve stimulation. AEDs have become the mainstay of epilepsy treatment for most patients. All AEDs have the following three goals: 1) eliminate seizures or reduce seizure frequency; 2) avoid adverse effects associated with long-term AED therapy; and 3) normalize the patient’s lifestyle. It is important to be aware that the use of AEDs is not without risks. The current FDA-approved AEDs not only may fail to control seizure activity in certain patients but also can lead to serious adverse events, including death from aplastic anemia or hepatic failure. See TABLE 1 for a listing of FDA-approved AEDs available for seizure treatment.6
The community pharmacist is generally the last healthcare professional a patient sees before taking a medication.7 Particularly for higher-risk medications, community pharmacists should make sure to perform a thorough review of the epileptic patient’s medication profile, including drug interactions, potential barriers to care, and antiepileptic regimen. A study by Roth and colleagues used a written questionnaire to evaluate pharmacists’ knowledge of the different pharmacologic options for epilepsy treatment and their recommendations for a number of hypothetical situations. The researchers determined that the participating pharmacists were knowledgeable in only some scenarios involving appropriate care of patients with epilepsy. Several knowledge gaps were identified, including urgent situations in which the patient’s clinician should be contacted immediately.8
There are several areas in which community pharmacists can make a major impact on the care of patients receiving AEDs, including but not limited to drug interactions, the importance of medication adherence, thorough education on epilepsy, adverse reactions, the effect of diabetes on epilepsy, and evaluation of the AED’s appropriateness.9-19
Drug-Drug Interactions
Several AEDs are known to induce or autoinduce the metabolism of other drugs, and some AEDs inhibit the metabolism of other drugs.9 Drugs that may induce the metabolism of other drugs include carbamazepine, phenytoin, phenobarbital, and primidone. Drugs that inhibit the metabolism of other drugs include felbamate and valproate.9
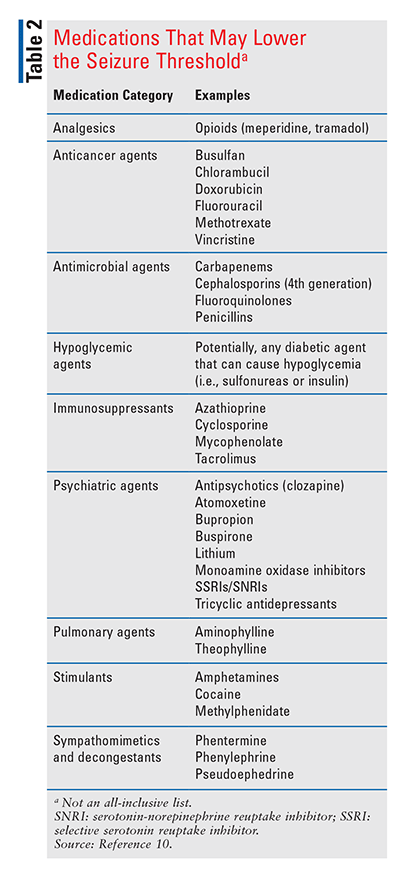
The identification of medications associated with lowering the seizure threshold is an area in which community pharmacists can have a major impact. Once the pharmacist identifies which agents are a concern, one possible intervention is to contact the prescriber to determine whether the patient can be transitioned to a different medication. For example, a patient taking tramadol for chronic pain could potentially be switched to another opioid that does not lower the seizure threshold. TABLE 2 lists some of the most common medications associated with lowering of the seizure threshold.10
Medication Adherence
Because of their accessibility, community pharmacists have a prime opportunity to educate patients on the importance of medication adherence. Adherence to AEDs is crucial for preventing or minimizing seizures. Nonadherence can result in breakthrough seizures, which can have a serious impact on a patient’s quality of life.11 The rationale behind a patient’s nonadherence to medications is often multifaceted. Reasons for nonadherence include forgetfulness, misunderstanding the clinician’s recommendations, or even intentionality based on lifestyle choice or expectations regarding treatment or adverse effects.11 In a study conducted by Cramer and colleagues, 45% of the study population reported having a seizure after missing a dose of the AED regimen.12 If a community pharmacist were to intervene and provide information about the importance of adhering to treatment with seizure medications, it is highly likely that the seizure incidence would decline. It is estimated that about 70% of epileptic patients who are treated with AEDs could be seizure free with adherence to their most effective regimen.11
Patients’ and Family Members’ Lack of Knowledge
Educating patients and their family members about what to do during status epilepticus (an acute, prolonged epileptic crisis) is just as important as providing information about medication adherence. Only one-fourth of participants in a survey by Kobau and Price that examined a representative U.S. sample thought that they were knowledgeable about epilepsy, and only one-third knew what to do in the event of a seizure.13 A literature review by Couldridge and colleagues determined that epileptic patients and their families needed specific information about epilepsy diagnosis; seizures, including how to control them; treatment options; drugs, including their adverse effects; safety and prevention of injury; and common psychological and social problems.14
Adverse Effects of AEDs
Community pharmacists can counsel patients on possible adverse effects of AEDs. The following key points address the most common adverse effects of several FDA-approved AEDs15,16:
• AEDs associated with neurotoxicity (sedation, ataxia, confusion, dizziness, blurred vision) include carbamazepine, phenobarbital, phenytoin, topiramate, and valproic acid.
• Gabapentin, levetiracetam, oxcarbazepine, and valproic acid are associated with weight gain.
• Carbamazepine, eslicarbazepine, oxcarbazepine, phenobarbital, and phenytoin are associated with thyroid abnormalities.
• AEDs associated with rash/hypersensitivity reactions include carbamazepine, lamotrigine, phenobarbital, and phenytoin. (Note: For carbamazepine and phenytoin, screen for HLA-B*1502 allele in patients of Asian descent because of the increased risk of dangerous and possibly fatal skin reactions, including Stevens-Johnson syndrome and toxic epidermal necrolysis.)
Epilepsy and Diabetes
An area in which community pharmacists can make a difference is the care of epileptic patients with diabetes. The relationship between glucose levels and seizure provocation has been studied for many years but is not completely understood. In one trial, Kinnear and colleagues determined that higher glucose concentrations corresponded to left temporal seizures, with lower glucose concentrations corresponding to right temporal seizures.17 It is known that maintaining glucose concentrations within the appropriate range for epileptic patients could be crucial in seizure prevention. Continuous glucose monitors could potentially play a role in the treatment of epilepsy in diabetic patients. Community pharmacists can identify patients with both disorders, conduct interventions, and provide education regarding what is known about the connection between diabetes and epilepsy.
AED Appropriateness and Seizure Control
Through conversations with the patient or family members, the community pharmacist can evaluate an AED’s appropriateness to ensure that the patient’s seizures are being adequately controlled. One area of discussion for the community pharmacist is to determine whether a patient has been prescribed the appropriate seizure rescue medication. First-line agents for status epilepticus include benzodiazepines such as midazolam, diazepam, and lorazepam.18 It is important to consider the differing pharmacokinetics of these benzodiazepines when determining which agent to use, but the route of administration should also be weighed when choosing the best agent for individual patients. For example, diazepam comes in a rectal formulation that may be preferred for young children or patients in whom the oral route is not an option. Intranasal midazolam may also be considered, as it is suitable for epileptic patients of all ages and has been shown to be efficacious and safe for treatment of acute seizures.19
Community Pharmacists’ Impact on Treatment of Epilepsy
Few studies have been conducted to evaluate the impact that community pharmacists can have on epilepsy treatment in the U.S. However, one cross-sectional study by McAuley and colleagues surveyed a total of 75 patients with epilepsy to determine the role that community pharmacists played—or potentially could play—in their care. The researchers determined that patients most frequently consulted a community pharmacist for information about drug interactions (65%) or adverse effects (56%). Community pharmacists were consulted less often for information about AED adherence, medication profiles, or epilepsy’s impact on their lifestyle. Patients reported that despite having a good relationship with their pharmacist, they had concerns about lack of privacy and did not want to pay for additional services. The feedback from this study could be used to identify potential areas in which pharmacists can play a larger role in epilepsy treatment.20
Conclusion
As one of the most accessible types of healthcare professionals, community pharmacists have the opportunity to provide appropriate care to patients experiencing seizures, perform interventions, and provide education to their patients. By having regular conversations with patients with epilepsy, community pharmacists have the potential to improve patient care and patients’ knowledge about their disease state.
REFERENCES
1. Johns Hopkins Medicine. Epilepsy overview. www.hopkinsmedicine.org/health/conditions-and-diseases/epilepsy. Accessed October 2, 2022.
2. CDC. Epilepsy data and statistics. www.cdc.gov/epilepsy/data/index.html. Accessed October 3, 2022.
3. Basic mechanisms of underlying seizures and epilepsy. In: Bromfield EB, Cavazos JE, Sirven JI, eds. An Introduction to Epilepsy. West Hartford, CT: American Epilepsy Society; 2006:1-26.
4. Thijs RD, Surges R, O’Brien TJ, Sander JW. Epilepsy in adults. Lancet. 2019;393(10172):689-701.
5. CDC. Types of seizures. www.cdc.gov/epilepsy/about/types-of-seizures.htm. Accessed October 25, 2022.
6. Tian N, Boring M, Kobau R, et al. Active epilepsy and seizure control in adults—United States, 2013 and 2015. MMWR Morb Mortal Wkly Rep. 2018;67(15):437-442.
7. Manolakis PG, Skelton JB. Pharmacists’ contributions to primary care in the United States collaborating to address unmet patient care needs: the emerging role for pharmacists to address the shortage of primary care providers. Am J Pharm Educ. 2010;74(10):s7.
8. Roth Y, Neufeld MY, Blatt I, et al. An evaluation of pharmacist knowledge on treatment with antiepileptic drugs. Seizure. 2016;34:60-65.
9. Johannessen SI, Landmark CJ. Antiepileptic drug interactions—principles and clinical implications. Curr Neuropharmacol. 2010;8(3):254-267.
10. UpToDate. Medications associated with seizures. www.uptodate.com/contents/image?imageKey=NEURO%2F106961. Accessed October 2, 2022.
11. Eatock J, Baker GA. Managing patient adherence and quality of life in epilepsy. Neuropsychiatr Dis Treat. 2007;3(1):117-131.
12. Cramer JA, Glassman M, Rienzi V. The relationship between poor medication compliance and seizures. Epilepsy Behav. 2002;3(4):338-342.
13. Kobau R, Price P. Knowledge of epilepsy and familiarity with this disorder in the U.S. population: results from the 2002 HealthStyles Survey. Epilepsia. 2003;44(11):1449-1454.
14. Couldridge L, Kendall S, March A. ‘A systematic overview—a decade of research’. The information and counselling needs of people with epilepsy. Seizure. 2001;10(8):605-614.
15. Elshorbagy HH, Barseem NF, Suliman HA, et al. The impact of antiepileptic drugs on thyroid function in children with epilepsy: new versus old. Iran J Child Neurol. 2020;14(1):31-41.
16. Perucca E, Meador KJ. Adverse effects of antiepileptic drugs. Acta Neurol Scand Suppl. 2005;181:30-35.
17. Kinnear KM, Warner NM, Haltiner AM, Doherty MJ. Continuous monitoring devices and seizure patterns by glucose, time and lateralized seizure onset. Epilepsy Behav Case Rep. 2018;10:65-70.
18. Isojärvi JI, Tokola RA. Benzodiazepines in the treatment of epilepsy in people with intellectual disability. J Intellect Disabil Res. 1998;42(Suppl 1):80-92.
19. Humphries LK, Eiland LS. Treatment of acute seizures: is intranasal midazolam a viable option? J Pediatr Pharmacol Ther. 2013;18(2):79-87.
20. McAuley JW, Miller MA, Klatte E, Shneker BF. Patients with epilepsy’s perception on community pharmacist’s current and potential role in their care. Epilepsy Behav. 2009;14(1):141-145.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.






