US Pharm. 2015;40(11):44-47.
ABSTRACT: Borderline personality disorder (BPD) is a condition characterized by impulsiveness, mood instability, negative self-image, and episodes of self-injury and attempted suicide. While the exact underlying causes and pathophysiological processes are yet to be identified, a combination of genetics, environmental factors, and a history of childhood trauma have all been shown to contribute to the development of the disorder. Pharmacists are an important part of the multidisciplinary healthcare team that manages patients with BPD. Psychotherapy should be utilized as the primary treatment for BPD, although pharmacotherapeutic agents are often prescribed for the management of symptoms.
Borderline personality disorder (BPD) is a psychological condition characterized by a pattern of impulsiveness and mood instability. The word personality is a complex term used to describe the way someone thinks, feels, and behaves, underpinning that individual’s sense of self. BPD is associated with an increased risk of suicide together with fears of abandonment.1 Patients with BPD feel empty and have a negative self-image. While BPD and bipolar disorder (types I and II) display over-lapping symptoms, there are certain features that distinguish the two. In particular, the pattern of affective instability, a prominent feature in both disorders, varies. Patients with BPD demonstrate transient mood shifts that occur in response to interpersonal stressors, whereas bipolar disorder is associated with sustained mood changes.2
Recent studies have shown that BPD is present in about 6% of primary care patients in community-based samples and in 15% to 20% of patients in psychiatric hospitals and outpatient clinics.3-5 The majority of these patients tend to be female, with rates as high as 75% in clinical settings.6,7 Most patients with BPD are admitted into a treatment facility following a suicide attempt or an episode of deliberate self-injury.8 The average risk of suicide attempt is 60% to 70%, and about 10% of BPD patients die of suicide (this figure is particularly high for young women).8 On average, patients remain in the hospital for 6.3 days per year and make nearly one emergency room visit every 2 years. These rates are six to 12 times higher than those among patients with a major depressive disorder.9,10 These figures translate to a large economic burden, with the use of expensive healthcare resources, persistent lack of patient productivity, and emotional costs, as well as other costs related to a variety of behaviors such as domestic violence, reckless driving, imprisonment, and pathologic gambling.11-15
Clinical Features
Patients with BPD have characteristically unstable moods and express feeling “up” and “down” without any explanation. Since the person’s thoughts and feelings can be difficult to manage, many patients resort to different ways of self-harm, such as cutting, ligaturing (strangulation), or overdosing on drugs, as a way of managing distress. Those with BPD may experience difficulty maintaining social relationships, and conflicts with other individuals often lead to social isolation and problems at work. Furthermore, they tend to have intense but short-lived relationships due to problematic attachment patterns. Psychotic symptoms may occur, but are usually brief, circumscribed, or accompanied by good reality testing.16 Patients with BPD may manifest over-whelming anger when in a state of crisis. They often display a poor sense of who they are and are frequently dissatisfied with their functioning, feeling empty and negative about themselves.
BPD is often associated with other mental health problems, such as anxiety, depression, eating disorders, posttraumatic stress disorder, and substance abuse, and overlapping symptoms may make it difficult to establish a clear diagnosis. Additionally, the presence of BPD negatively affects the course and treatment of coexisting medical conditions and other psychiatric disorders.17-20
Diagnosis
BPD can be caused by different combinations of symptoms.21 The four main features of BPD include affective instability, identity problems, negative relationships, and self-harm.21 An accurate diagnosis is very important, as it helps such individuals understand their difficulties and seek appropriate help. However, there have been concerns about the validity of the diagnosis, and some consider it stigmatizing. The diagnosis of BPD is made after the age of 18 years using one of two criteria—The Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) or the International Statistical Classification of Disease and Related Health Problems, Tenth Revision (ICD-10). Even though personality disorders are diagnosed only in adults, BPD manifests itself in adolescence in the form of uncontrollable anger, self-mutilations, dissociation, and other such behaviors.22 TABLE 1 lists the DSM-5 diagnostic criteria for BPD.23

Risk Factors
Although the cause of BPD is not fully understood, a combination of genetic and environmental factors, as well as a history of childhood neglect or trauma including emotional, physical, and sexual abuse, has been known to increase an individual’s risk of developing this condition.4,24 Even though specific genes that link the disorder have not yet been identified, BPD is significantly inheritable, with 42% to 68% of the variance being associated with genetic factors.21,25 Furthermore, all the major components of the disorder, including affective instability, identity problems, negative relationships, and self-harm, have been shown to track in families.24 A difficult childhood can impair brain development significantly since neural pathways develop rapidly during this time and children are dependent upon their caregivers for all of their needs.26
Pathophysiology
A number of underlying causes for the development of BPD have been proposed. One proposal suggests that increased cortisol production through stimulation of the hypothalamic-pituitary-adrenal (HPA) axis may occur in cases of chronic stress, such as that associated with childhood adversity.26 The limbic system, which includes the amygdala, the hippocampus, and frontal areas of the brain, have also been linked to BPD. Neuroimaging studies have shown a reduction in the volume of the amygdala in individuals with BPD, possibly as a result of excitotoxicity, a process whereby nerve cells are damaged by excessive stimulation. Yet another study group has proposed that the amygdala actually becomes more sensitive in people with BPD.26-30
Treatment
BPD is a complex and multifaceted condition usually requiring a multidisciplinary treatment approach including drug therapy, occupational therapy, psychological therapy, and housing support. Effective treatment usually leads to a good prognosis, and patients should ideally undergo therapy within the community, as long, unstructured hospital admissions can worsen the condition.31 Healthcare professionals should be aware that patients with BPD may have difficulty establishing relationships and may reject treatments offered or have unrealistic expectations of them due to the nature of the condition.32
Psychological Therapy
Psychotherapy is seen to have a beneficial impact on a variety of factors when used in the treatment of psychiatric disorders such as BPD, bipolar affective disorder, and schizophrenia. It has been noted that psychotherapy reduces inpatient treatment and decreases work impairment.33 As such, psychotherapy should be utilized as the primary treatment for BPD.4,34 Psychotherapy aims to encourage self-reflection, improve interpersonal and emotional understanding, challenge and modify dysfunctional core beliefs, and achieve better environmental adjustment.31 Patients should ideally attend twice weekly psychotherapy sessions, and treatment duration should be a minimum of 3 months.5
Psychotherapy encompasses a number of different techniques including dialectical behavior therapy (DBT), transference-focused psychotherapy, mentalization-based therapy, and general psychiatric management, all of which can be used for the management of BPD. These methods have been shown to reduce the need for other treatments, including emergency room visits and pharmacotherapy, by 80% to 90%, and the occurrence of self-harm and/or suicidal episodes by about 50%. The challenge with psychotherapy is that extensive training is required before it can be delivered, and it is therefore not widely available, even though the clinical and cost benefits are maintained during a period of 2 to 5 years.35,36
DBT is a technique based upon cognitive behavioral therapy that is specifically designed for the management of BPD.37 It was originally developed as an outpatient program, but with time it has been modified for use in hospital settings and among more diverse populations with an aim of increasing the capacity to self-regulate and teaching interpersonal effectiveness, distance tolerance, emotional regulation, and mindfulness.24 DBT is normally delivered as a group skills training session with telephone consultations and individual coaching sessions offered alongside.
Mentalization-based treatment is another method of psychotherapy that was developed specifically for the management of BPD. This therapy is aimed at improving a patient’s ability to understand both his or her own mental state and that of others.38,39 Mentalization-based treatment is much shorter and has fewer requirements than the other forms of psychotherapy, as it is administered as weekly individual therapy sessions as well as group sessions over 18 months.38
Transference-focused psychotherapy is centered on emotions arising in the relationship with the therapist and the use of traditional psychodynamic techniques. Generally, individuals undergo twice-weekly individual therapy sessions for about 1 year.40
Pharmacologic Treatment
While psychotherapy is essential in establishing long-term improvements in the patient’s personality and overall functioning, pharmacotherapeutic agents are often prescribed for the management of symptoms and trait vulnerabilities.41 Pharmacologic therapy might be initiated as an adjunct to psychotherapy in patients with symptoms of impulsivity, affective instability, and/or psychosis.42 No medications have been approved by the FDA specifically for the treatment of BPD. Antipsychotics, mood stabilizers, antidepressants, and dietary supplements have all been used in BPD patients even though there is no conclusive research in this area and the medications are unlicensed for this indication (i.e., used off-label).41
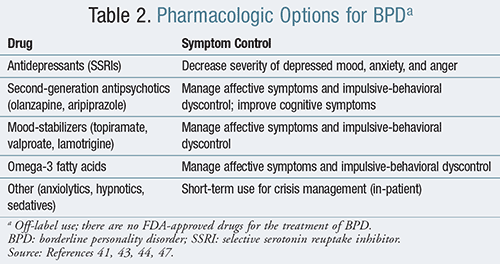
Mood stabilizers (topiramate, valproate, lamotrigine), second-generation antipsychotics (olanzapine, aripiprazole), and omega-3 fatty acids have been shown to be useful in the management of affective symptoms and impulsive-behavioral dyscontrol in BPD patients.41 Antipsychotics have been shown to have an additional role in improving a BPD patient’s cognitive symptoms. They help with impaired cognition and emotional flattening and are therefore useful in patients who experience a high level of emotional distress.43,44 The use of these agents is further limited by common adverse effects including obesity, hypertension, and diabetes with atypical antipsychotic agents, or by sedation and possibly toxic effects to kidneys with mood stabilizers.45,46
Selective serotonin reuptake inhibitors (SSRIs) have been found to be effective in decreasing the severity of depressed mood, anxiety, and anger, mainly in subjects with a concomitant affective disorder. The effects of antidepressants on impulsive behaviors are uncertain. Some randomized trials have concluded that SSRIs and other antidepressants have little benefit, if any, over placebo.47 Since BPD worsens depression outcomes, it is possible that the patients in fact respond poorly to treatment.
Benzodiazepines are contraindicated for use in BPD as they reduce inhibitions and therefore may worsen impulsivity. Furthermore, patients with BPD are at a greater risk of addiction and may become addicted to sedatives.16 Other anxiolytics, hypnotics, and sedatives such as zolpidem may be useful for the treatment of BPD when used for brief periods for crisis management, such as short in-patient hospital admissions. A summary of treatment options is provided in TABLE 2.41,43,44,47
Role of the Pharmacist
Pharmacists are an important part of the multidisciplinary healthcare team that manages patients with BPD. With access to patient medication records, pharmacists can monitor patient compliance as well as ensure that individuals are not overdosing on their prescribed medications. Furthermore, polypharmacy is a common concern in patients with BPD; one study found that 80% of patients with BPD were taking three or more medications.48 Pharmacists are suitably placed to discuss multiple medications with patients and review what drugs they should discontinue, if any.
REFERENCES
1. Grilo CM, Sanislow CA, Skodol AE, et al. Longitudinal diagnostic efficiency of DSM-IV criteria for borderline personality disorder: a 2-year prospective study. Can J Psychiatry. 2007;52:357-362.
2. Paris J, Black DW. Borderline personality disorder and bipolar disorder: what is the difference and why does it matter? J Nerv Ment Dis. 2015;203(1):3-7.
3. Gross R, Olfson M, Gameroff M, et al. Borderline personality disorder in primary care. Arch Intern Med. 2002;162:53-60.
4. Gunderson JG, Links PS. Borderline Personality Disorder: A Clinical Guide. 2nd ed. Washington, DC: American Psychiatric Press, Inc; 2008.
5. National Institute for Health and Care Excellence. Borderline Personality Disorder: Treatment and Management. London, UK: NICE; 2009.
6. Lenzenweger MF, Lane MC, Loranger AW, Kessler RC. DSM-IV personality disorders in the National Comorbidity Survey Replication. Biol Psychiatry. 2007;62:553-564.
7. Grant BF, Chou SP, Goldstein RB, et al. Prevalence, correlates, disability, and comorbidity of DSM-IV borderline personality disorder: results from the Wave 2 National Epidemiologic Survey on alcohol and related conditions. J Clin Psychiatry. 2008;69:533-545.
8. Pascual JC, Córcoles D, Castaño J, et al. Hospitalization and pharmacotherapy for borderline personality disorder in a psychiatric emergency service. Psychiatr Serv. 2007;58:1199-1204.
9. Bender DS, Dolan RT, Skodol AE, et al. Treatment utilization by patients with personality disorders. Am J Psychiatry. 2001;158:295-302.
10. Zanarini MC, Frankenburg FR, Hennen J, Silk KR. Mental health service utilization by borderline personality disorder patients and Axis II comparison subjects followed prospectively for 6 years. J Clin Psychiatry. 2004;65:28-36.
11. Soeteman DI, Hakkaart-van Roijen L, Verheul R, Busschbach JJ. The economic burden of personality disorders in mental health care. J Clin Psychiatry. 2008;69:259-265.
12. Sansone RA, Lam C, Wiederman MW. Road rage: relationships with borderline personality and driving citations. Int J Psychiatry Med. 2010;40:21-29.
13. Tweed RG, Dutton DG. A comparison of impulsive and instrumental subgroups of batterers. Violence Vict. 1998;13:217-230.
14. Trestman RL, Ford J, Zhang W, Wiesbrock V. Current and lifetime psychiatric illness among inmates not identified as acutely mentally ill at intake in Connecticut’s jails. J Am Acad Psychiatry Law. 2007;35:490-500.
15. Fernández Montalvo J, Echeburúa E. Pathological gambling and personality disorders: a pilot study with the MCMI-II [in Spanish]. Psicothema. 2006;18:453-458.
16. Lubit RH. Borderline personality disorder clinical presentation. Medscape. http://emedicine.medscape.com/article/913575-clinical. Accessed July 20, 2015.
17. Rothrock J, Lopez I, Zweilfer R, et al. Borderline personality disorder and migraine. Headache. 2007;47:22-26.
18. Palmer NB, Salcedo J, Miller AL, et al. Psychiatric and social barriers to HIV medication adherence in a triply diagnosed methadone population. AIDS Patient Care STDS. 2003;17:635-644.
19. Massion AO, Dyck IR, Shea MT, et al. Personality disorders and time to remission in generalized anxiety disorder, social phobia, and panic disorder. Arch Gen Psychiatry. 2002;59:434-440.
20. Walter M, Gunderson JG, Zanarini MC, et al. New onsets of substance use disorders in borderline personality disorder over 7 years of follow-ups: findings from the Collaborative Longitudinal Personality Disorder Study. Addiction. 2009;104:97-103.
21. Distel MA, Willemsen G, Ligthart L, et al. Genetic covariance structure of the four main features of borderline personality disorder. J Pers Disord. 2010;24:427-444.
22. Al-Alem L, Omar HA. Borderline personality disorder: an overview of history, diagnosis and treatment in adolescents. Int J Adolesc Med Health. 2008;20(4):395-404.
23. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5). Arlington, VA: American Psychiatric Press; 2013.
24. Linehan MM. Cognitive Behavioural Treatment of Borderline Personality Disorder. London, UK: Guildford Press; 1993.
25. Gunderson JG, Zanarini MC, Choi-Kain LW, et al. Family study of borderline personality disorder and its sectors of psychopathology. Arch Gen Psychiatry. 2011;68(7):753-762.
26. Tyrka A, Burgers D, Philips N, et al. The neurobiological correlates of childhood adversity and implications for treatment. Acta Psychiatrica Scandinavica. 2013;128:434-437.
27. Koenigsberg HW, Siever LJ, Lee H, et al. Neural correlates of emotion processing in borderline personality disorder. Psychiatry Res. 2009;172:192-199.
28. Donegan NH, Sanislow CA, Blumberg HP, et al. Amygdala hyperreactivity in borderline personality disorder: implications for emotional dysregulation. Biol Psychiatry. 2003;54:1284-1293.
29. Silbersweig D, Clarkin JF, Goldstein M, et al. Failure of frontolimbic inhibitory function in the context of negative emotion in borderline personality disorder. Am J Psychiatry. 2007;164:1832-1841.
30. King-Casas B, Sharp C, Lomax-Bream L, et al. The rupture and repair of cooperation in borderline personality disorder. Science. 2008;321:806-810.
31. Bateman AW, Tyrer P. Services for personality disorder: organisation for inclusion. Adv Psychiatric Treat. 2004;10: 425-433.
32. Livesley J. Practical Management of Personality Disorder. London, UK: Guilford Press; 2003.
33. Gabbard GO, Lazar SG, Hornberger J, Spiegel D. The economic impact of psychotherapy: a review. Am J Psychiatry. 1997;154(2):147-155.
34. Oldham JM, Gabbard GO, Goin MK, et al; American Psychiatric Association. Practice guideline for the treatment of patients with borderline personality disorder. Am J Psychiatry. 2001;158(suppl):1-52.
35. Linehan MM, Heard HL. Borderline personality disorder: costs, course and treatment outcomes. In: Miller NE, Magruder KM, eds. The Cost-Effectiveness of Psychotherapy: A Guide for Practitioners, Researchers and Policy Makers. New York, NY: Oxford University Press; 1999:291-305.
36. Bateman A, Fonagy P. Health service utilization costs for borderline personality disorder patients treated with psychoanalytically oriented partial hospitalization versus general psychiatric care. Am J Psychiatry. 2003;160:169-171.
37. Bernhardt K, Friege L, Gerok-Falke K, Aldenhoff JB. In-patient treatment concept for acute crises of borderline patients on the basis of dialectical-behavioral therapy. Psychother Psychosom Med Psychol. 2005;55(9-10):397-404.
38. Bateman A, Fonagy P. Psychotherapy for Borderline Personality Disorder: Mentalization-Based Treatment. Oxford, UK: Oxford University Press; 2004:381.
39. Bateman A, Fonagy P. Randomized controlled trial of outpatient mentalization-based treatment versus structured clinical management for borderline personality disorder. Am J Psychiatry. 2009;166(12):1355-1364.
40. Biskin RS, Paris J. Management of borderline personality disorder. CMAJ. 2012;184(17):1897-1902.
41. Bellino S, Paradiso E, Bogetto F. Efficacy and tolerability of pharmacotherapies for borderline personality disorder. CNS Drugs. 2008;22(8):671-692.
42. Zanarini MC, Frankenburg FR. A preliminary, randomized trial of psychoeducation for women with borderline personality disorder. J Pers Disord. 2008;22: 284-290.
43. Mizrahi R, Bagby RM, Zipursky BB, et al. How antipsychotics work: the patient’s perspective. Prog Neuropsychopharmacol Biol Psych. 2005;29:859-864.
44. Moncrieff J, Cohen D, Mason JP. The subjective experience of taking antipsychotic medication: a content analysis of Internet data. Acta Psychiatr Scand. 2009;120:102-111.
45. Ingenhoven T, Lafay P, Rinne T, et al. Effectiveness of pharmacotherapy for severe personality disorders: meta-analyses of randomized controlled trials. J Clin Psychiatry. 2010;71:14-25.
46. Lieb K, Völlm B, Rücker G, et al. Pharmacotherapy for borderline personality disorder: Cochrane systematic review of randomised trials. Br J Psychiatry. 2010;196:4-12.
47. Gunderson JG, Morey LC, Stout RL, et al. Major depressive disorder and borderline personality disorder revisited: longitudinal interactions. J Clin Psychiatry. 2004;65:1049-1056.
48. Frankenburg FR, Zanarini MC. Obesity and obesity-related illnesses in borderline patients. J Pers Disord. 2006;20:71-80.
To comment on this article, contact rdavidson@uspharmacist.com.





