US Pharm. 2011;36(12):12-15.
Hemorrhoids are swollen veins in the anal canal that cause a variety of symptoms.1-3 Anorectal problems such as hemorrhoids cause untold misery for many people at one time or another.1,4,5 Some persons may put off a pharmacist or physician consultation until the symptoms become unbearable. Unfortunately, many patients who initially seek relief through the use of a nonprescription product will require referral to a physician.
Prevalence
The number of people with hemorrhoids is impossible to determine, as many who experience the symptoms consider them too embarrassing to share with a physician or pharmacist. However, at least 50% of people will have experienced hemorrhoidal symptoms by the time they reach the age of 50 years.2
The Anatomy of Hemorrhoids
The anal opening is also referred to as the anal verge. Approximately 2 to 3 cm above this is an anatomical landmark known as the dentate or pectinate line, which is distinguished by a circular row of glands that secrete mucus that acts to lubricate the anal canal. Groups of normal submucosal vascular beds composed of supportive connective tissue, smooth muscle, and blood vessels surround the anal canal. When these beds enlarge, the result is hemorrhoids.2 The exact cause of the enlargement is open to further dispute, although the “straining” theory asserts that straining interrupts the tissues that support the vascular bundles, displacing them and leading to their congestion.4
Classifications
Hemorrhoids are divided into three broad categories, depending on the point of origin.4 If the hemorrhoidal tissue originates above the dentate line, it is classified as an internal hemorrhoid, even if some of the tissue extends below.2,6 External hemorrhoids originate below the dentate line. Mixed hemorrhoids have features of both.2
Manifestations
The degree of discomfort experienced by the patient is dependent on the type of hemorrhoids and the extent of their severity. Internal hemorrhoids lack nerves and are painless. When they cause bleeding, it is usually bright red and seen on the outer part of stools after defecation.6 The patient does not usually bleed at other times. The internal tissues may enlarge and push below the dentate line to protrude from the anal opening, especially after defecation.2 The patient may describe this to the pharmacist as a soft bit of tissue that shrinks back to normal shortly after defecation or requires the patient to manually push the tissue back into its normal position above the dentate line after each bowel movement (in more severe cases).
Eventually, the patient with long-standing prolapse may discover that the tissue can no longer be replaced, a condition known as permanent prolapse. This tissue interferes with proper closure of the anal sphincter, and the patient may notice fecal staining of underwear. The irritant effect of the fecal material may in turn cause perianal dermatitis, in the same way that exposure to fecal material in infants causes diaper dermatitis. The patient with prolapse or bleeding is well advised to seek a physician’s care.2 Rectal bleeding must always be considered possible colorectal carcinoma until proven otherwise, and nonprescription products cannot reverse prolapse.7
External hemorrhoids are fully innervated. Patients asking the pharmacist for assistance may be experiencing any degree of discomfort from minor itching or burning to severe pain.6 When they first occur, external hemorrhoids are often no more than small skin tags hardly noticed by the patient. However, they usually enlarge until the patient begins to notice perianal irritation, persistent moisture in the area, and increasing difficulty/pain in cleansing after defecation.2 If a vessel thromboses, the resultant perianal hematoma can cause severe and acute pain. It usually subsides slowly over several weeks, but the patient experiences extreme pain in the interim.6 Thrombosis may be induced by diarrhea, constipation, or physical activity such as riding a bicycle with a seat that places undue pressure on the anal area.2,4
Nonprescription Treatments
For most minor hemorrhoids, conservative therapy may be all that is needed (e.g., adding fiber to the diet, drinking more water, using stool softeners).2,4,8 Pharmacists can advise patients to wash well with soap and water following each bowel movement, blotting the area rather than rubbing to minimize irritation. Patients should also take sitz baths, sitting in warm water 2 to 3 times daily for 15 to 30 minutes.1,6
If these simple methods do not provide relief, the pharmacist may suggest nonprescription products unless their use is contraindicated. Contraindications include prolapse (especially prolapse that must be manually replaced or cannot be reduced), any rectal bleeding, use in patients less than 12 years old, or a problem that has persisted for more than 7 days.1,2,7 Due to the chronic nature of hemorrhoids, the 7-day rule regarding self-therapy means that many patients with hemorrhoidal symptoms will require physician referral when they initially speak to the pharmacist. These products should be recommended cautiously for the pregnant patient. Products that are placed above the dentate line (e.g., suppositories, ointments with a long applicator tube) could be absorbed, and could be toxic to the fetus. Thus, they are contraindicated in pregnancy. Products that are applied externally do not require the warning.
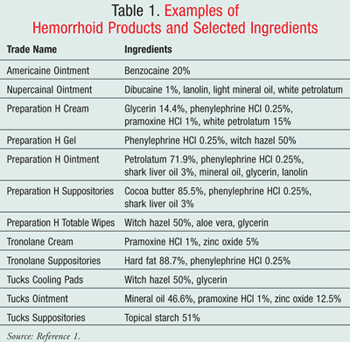
If there are no contraindications, several ingredients and products may provide relief. Some anorectal product ingredients are safe enough to be used internally or externally, and can be found in ointments, suppositories, and wipes. Other ingredients are not suitable for internal use, and they are limited to external products (e.g., ointments and wipes). TABLE 1 presents examples of selected hemorrhoidal products.1
Protectants: Protectants are useful ingredients due to their ability to form a protective coating over the skin that prevents tissues from drying out; protect irritated areas; relieve burning and skin irritation; protect inflamed, irritated anorectal areas from abrasion and pain during bowel movements; and protect inflamed perianal skin.1,2 Cocoa butter, hard fat, lanolin, mineral oil, petrolatum, and topical starch may be used internally or externally. Glycerin may only be applied externally. Some protectants are internal or external but are only to be used in combination products. These include calamine, cod liver oil, shark liver oil, and zinc oxide. Protectants are applied after each bowel movement or as needed, up to 6 times daily; however, petrolatum may be applied liberally whenever needed.
Local Anesthetics: Local anesthetics are not appropriate for internal use, as the mucosal lining of the rectum does not contain sensory nerve fibers.1 Thus, anesthetics are not included in suppositories or ointments meant for internal use, but they are included in external creams, gels, ointments, and wipes. They relieve pain, itching, soreness, burning, irritation, and discomfort.1,6 Benzocaine, benzyl alcohol, dyclonine, lidocaine, and tetracaine may be applied up to 6 times daily; pramoxine up to 5 times daily; and dibucaine 3 to 4 times daily. Patients may develop contact dermatitis to local anesthetics, leading to the following required warning: “Certain persons can develop allergic reactions to ingredients in this product. If the symptom being treated does not subside, or redness, irritation, swelling, pain or other symptoms develop or increase, discontinue use and consult a physician.”1
Astringents: These ingredients exert a local and limited protein coagulant effect, temporarily protecting irritated anorectal areas and relieving irritation and burning. Calamine and zinc oxide have astringent activity (in addition to being protectants) and may be applied internally or externally. Witch hazel is applied only externally.6 Astringents may be used after each bowel movement or as needed, up to 6 times daily.
Vasoconstrictors: These products constrict the blood vessels underlying tissues where they are applied, temporarily reducing the swelling associated with irritated hemorrhoidal tissues.1 Phenylephrine is the only vasoconstrictor in widespread use, and it is appropriate for internal or external use, applied up to 4 times daily. Products containing phenylephrine should not be recommended for patients with heart disease, hypertension, thyroid disease, diabetes, or difficulty in urination caused by an enlarged prostate. These products should also be avoided in patients taking prescription medications for hypertension or depression.
Hydrocortisone: Hydrocortisone relieves anal itching.1,6 It is found in Preparation H Hydrocortisone 1% Cream and Tucks Hydrocortisone Ointment.
Internal Analgesics: OTC internal analgesics may also help. Acetaminophen reduces minor pain, and ibuprofen and naproxen can help with pain and inflammation.1,2 They may be used concomitantly with the topical products in TABLE 1 (e.g., creams or ointments).
Physician Treatments
Physician treatment of internal hemorrhoids depends on the degree of severity.5,8 If they have not yet prolapsed, or if they have prolapsed but spontaneously reduce, some medical experts suggest hydrocortisone, bulk laxatives, and institution of a high-fiber diet with increased liquid intake to keep stools soft.1,6 Should symptoms persist or worsen (e.g., prolapse requiring manual replacement or irreducible prolapse), the physician may choose from several procedures, such as sclerotherapy (injection of a sclerosing agent such as sodium morrhuate into the tissues); rubber band ligation (placement of a tiny rubber band at the base of each internal hemorrhoid); photocoagulation using infrared light; electrocoagulation; laser coagulation; or cryotherapy (using a liquid nitrogen probe inserted via an anoscope).1,2 Each treatment modality has it relative advantages and disadvantages (e.g., offensive discharge with cryotherapy) when compared to the other options. In light of the wide variety of office procedures available, surgical hemorrhoidectomy is usually reserved for only the most severe cases.2
If the patient complains of intense pain, the pharmacist should consider the presence of a thrombosed external hemorrhoid.8 These hemorrhoids usually resolve in 7 to 10 days, but if they persist beyond this period, office excision and the application of a pressure dressing may be the treatment of choice.

Causes of Hemorrhoids
The main cause of hemorrhoids is straining to pass a bowel movement. Since constipation is a major factor in causing people to strain to pass feces, it is a major factor in developing hemorrhoids. Similarly, bouts of diarrhea cause straining and can also lead to hemorrhoids. Sitting for long periods of time also leads to hemorrhoids, as do certain anal infections and some medical conditions, such as cirrhosis of the liver.
Who Is More Prone to Hemorrhoids?
Hemorrhoids are especially common in pregnancy and the postpartum period. This is partly due to the changes that occur during pregnancy. It is also caused by the strain of pushing during labor, which can cause new hemorrhoids and also worsen existing ones. Overweight individuals and those with a family history of hemorrhoids are more likely to develop them. The risk increases with aging, with at least half of people who are 50 years or older seeking some form of care for them.
Symptoms of Hemorrhoids
The classic symptoms of hemorrhoids are anal itching, aching or pain (especially when sitting), bright red blood on the rectal tissues or in the stool, painful bowel movements, protruding tissues, and one or more hard lumps in the anal area.
When to See a Physician
If you experience anorectal discomfort of some type (such as burning, itching, or pain), the first thing to consider is that it may be a more serious condition, such as a fissure, abscess, or fistula, or simple anal irritation caused by allergies or incomplete cleansing following a bowel movement. For this reason, it is wise to follow directions on the product labels that advise use for no more than 7 days. If the problem persists for longer than 1 week from the time it began, see a physician to ensure that you do not have a more serious condition.
It is also important to note that rectal bleeding requires an immediate physician appointment. Never assume that rectal bleeding is a minor problem that will disappear on its own. Rather, view it as a cause for alarm that requires an immediate physician appointment to screen you for such problems as colorectal cancer.
Hemorrhoids occur with greater frequency as a person ages. Thus, hemorrhoid products should never be used on anyone under the age of 12 years. If you experience protrusion (your rectal tissues protrude from the anal opening after a bowel movement), you should also see a physician. These are prolapsed internal hemorrhoids that should be checked to see if they require surgical correction.
Nonprescription Products
If none of the above situations apply, you may be able to safely use nonprescription products such as ointments, creams, gels, wipes, and suppositories (e.g., Preparation H, Tronolane, Tucks). Consult Your Pharmacist for assistance in choosing an appropriate OTC product to treat your hemorrhoids.
REFERENCES
1. Pray WS. Nonprescription Product Therapeutics. 2nd ed. Baltimore, MD: Lippincott Williams & Wilkins; 2006.
2. Hemorrhoids. WebMD. www.webmd.com/a-to-z-guides/
3. Avsar AF, Keskin HL. Haemorrhoids during pregnancy. J Obstet Gynaecol. 2010;30:231-237.
4. Hemorrhoids. Definition. Mayo Clinic. www.mayoclinic.com/health/
5. Chen JS, You JF. Current status of surgical treatments for hemorrhoids—systematic review and meta-analysis. Chang Gung Med J. 2010;33:488-500.
6. Hemorrhoids. PubMed Health. www.ncbi.nlm.nih.gov/
7. Khan R, Hyman D. Hematochezia in the young patient: a review of health-seeking behavior, physician attitudes, and controversies in management. Dig Dis Sci. 2010;55:233-239.
8. Arezzo A, Podzemny V, Pescatori M. Surgical management of hemorrhoids. State of the art. Ann Ital Chir. 2011;82:163-172.
To comment on this article, contact rdavidson@uspharmacist.com.






