US Pharm.
2008;33(4):20-26.
A
mong all adverse reactions to medications, 6% to 10% are allergic in nature.
1 Of the wide variety of allergic drug reactions, the most frequently
recognized and reported manifest dermatologically.1,2 Cutaneous
adverse reactions have been reported in 2.7% of hospitalized patients.1,3
And while serious dermatologic drugñinduced reactions are estimated to occur
in only 1.9 cases per million people per year, they can be associated with a
mortality rate as high as 40%.1,4,5 Most dermatologic reactions are
generally mild and will resolve quickly after the discontinuation of the
offending drug. Others, however, can progress into serious or life-threatening
conditions.1 The drug-induced reactions considered most dangerous
because of their association with significant morbidity and mortality include
erythema multiforme major (Stevens-Johnson syndrome [SJS]), toxic epidermal
necrolysis (TEN), exfoliative dermatitis, and anaphylaxis.6
Etiology
While causes of SJS include a
variety of drugs (TABLE 1), infections (viral, bacterial, fungal,
protozoal), and malignancies (e.g., various carcinomas, lymphomas), up to 50%
of cases have no identified etiology.7 More than 50% of patients
with SJS report a recent upper respiratory tract infection.8 In
adults and the elderly, drugs and malignancies are the etiologies most often
implicated; infections most often cause SJS in pediatric patients.7
Most SJS reactions induced by anticonvulsants occur in the first 60 days of
therapy.9 Exposure to corticosteroids has been associated with an
increased rate of SJS occurrence.10 SJS occurs predominately in
Caucasians; there is a male-to-female ratio of 2:1 and a propensity for the
reaction to manifest in the early spring and winter.7 SJS can occur
at any age; however, most patients are in the second to fourth decade of their
lives. Cases have been reported in children as young as 3 months.7

Pathophysiology
While certain
categories of drug reactions involve immunologic mechanisms, there may also be
underlying nonimmunologic mechanisms involved (e.g., dose relationship).6
The most frequent of all cutaneous drug reactions are exanthem-like (macular
and papular) eruptions.6 The drugs most commonly responsible for
exanthematous eruptions include penicillins, cephalosporins, sulfonamides,
carbamazepine, phenytoin, allopurinol, and gold.6
Symptoms, Signs, and
Diagnosis
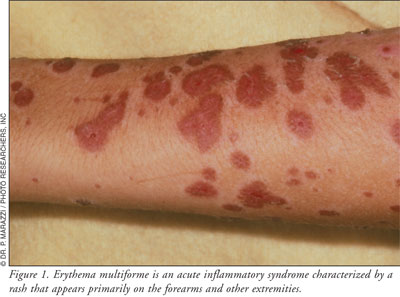
Erythema multiforme
is an acute inflammatory syndrome characterized initially by a macropapular
eruption that may progress to irregular lesions with a central clearing,
referred to as target or iris skin lesions.11 The
rash appears mostly on the extremities (e.g., hands, palms, wrists, forearms,
feet, elbows, knees) and may be accompanied by bullous lesions that break down
into erosions.1 The more extensive syndrome, referred to as
erythema multiforme major or SJS, is characterized by a spread to
more areas of the body and particularly involves the mucous membranes. SJS is
usually associated with fever and extensive purpura.1 In the course
of the illness, the significant involvement of mucous membranes includes
nasal, ocular, oral, gastrointestinal (GI), lower respiratory tract, urethral,
and vaginal.1,7 Diagnosis of SJS is clinical, and a dermatologist
is the clinician most often making the determination of SJS, with or without
biopsy.7
Separation of the epidermis
from the dermis may progress to sloughing of significant areas of the skin
that is attributable to pathologic cell death; some have also linked
inflammatory cytokines to the pathogenesis.7 Sloughing resembles
third-degree burns, and at this stage the condition is referred to as TEN
.1 Progression to necrosis may occur with GI and respiratory
mucous membrane involvement as well.7 There is a simple
classification used to describe the relationship of SJS to TEN: SJS may be
considered a mild form of TEN, with less than 10% body surface area (BSA)
detachment; overlapping SJS-TEN presents with detachment of 10% to 30% BSA;
and the diagnosis of TEN is used when detachment reaches more than 30% BSA.
12
Treatment, Prognosis, and
Prevention
While topical
steroids are an appropriate outpatient treatment for individuals with erythema
multiforme minor, patients with erythema multiforme major must
be hospitalized.7 Furthermore, due to the seriousness of the
condition, the facility should have critical care capabilities in the event
they are necessary. Management typically consists of discontinuing the
offending drug and administering symptomatic therapy until the reaction has
resolved.6 There is no treatment specifically for SJS.7
Severe reactions may require treatment in a burn center.6 While
consultation with an ophthalmologist is mandatory for the treatment of
patients with ocular involvement, consultation with other organ specialists
(e.g., pulmonologists, gastroenterologists, nephrologists) may be appropriate
in some cases.7
Saline compresses can be
applied to the eyelids, lips, and nose.7 Antimicrobials are
indicated in cases of cutaneous or urinary tract infections, as either may
result in bacteremia; the prophylactic use of systemic antibiotics is not
useful, particularly because of the risk of resistance to multiple drugs.
7 While systemic corticosteroids may be useful early in the reaction to
prevent visceral involvement and reduce intensity and duration, their overall
use in patients with SJS has been associated with an increase in morbidity and
mortality, rendering their utility controversial to date.7,10
Intravenous immunoglobulins and cyclosporine have also been used as treatments
for SJS.8
Unless a secondary infection
occurs, lesions usually heal within one to two weeks and most patients recover
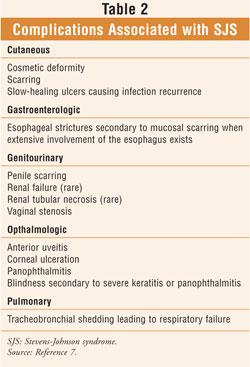
from SJS without sequelae.7 The development of complications (
TABLE 2) will ultimately determine prognosis; up to 15% of SJS cases
result in death.7 Mortality associated with TEN can reach as high
as 30%.1 Because there is the potential for recurrences, patients
must avoid any future exposure to the agents that were implicated in the
manifestation of SJS.7 Prophylactic treatment with human
intravenous immunoglobulin for recurrent SJS has been described in the
literature.7,13 Patients with skin conditions that are potentially
drug-induced should be evaluated by pharmacists and primary care providers
using an organized and thorough approach.8 Based on an
understanding of the mechanisms involved in adverse drug reactions, this
process should begin with a comprehensive medication history and documentation
of episodes of all medication allergies.8
Conclusion
There is a
potential risk of adverse events in response to the administration of any
drug, and cutaneous reactions may span a spectrum ranging from mild,
self-limiting occurrences to severe and life-threatening eruptions.
Stevens-Johnson syndrome, an immune complexñmediated hypersensitivity
disorder, is one of the most dangerous conditions that can be induced by a
drug. Associated with significant morbidity and mortality, SJS should be well
understood by pharmacists who can assist in its recognition and prevention.
REFERENCES
1. DiPiro JT, Qwnby DR. Allergic and pseudoallergic drug reactions. In: DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 6th ed. New York, NY: McGraw-Hill; 2005:1599-1611.
2. Svensson CK, Cowen EW, Gaspari AA. Cutaneous drug reactions. Pharmacol Rev. 2000;53:357-379.
3. Hunziker T, Kunzi U, Braunschweig S, et al. Comprehensive hospital drug monitoring: adverse drug reactions--a 20-year survey. Allergy. 1997;52:388-393.
4. Mockenhaupt M, Schopf E. Epidemiology of drug-induced severe skin reactions. Semin Cutan Med Surg. 1996;15:236-243.
5. Stern RS, Steinberg LA. Epidemiology of adverse cutaneous reactions to drugs. Dermatoepidemiology. 1995;13:681-688.
6. Osberg LA, Nesbitt LT. Urticaria and drug eruptions. American Academy of Dermatology. www.aad.org/education/students/_doc/UrticariaandDrugEruptions.doc. Accessed March 13, 2008.
7. Parrillo SJ. Stevens-Johnson Syndrome. emedicine.com. WebMD. Updated January 23, 2008. www.emedicine.com/emerg/TOPIC555.HTM. Accessed March 11, 2008.
8. Cheigh NH. Dermatologic drug reactions, self-treatable skin disorders, and skin cancer. In: DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic Approach . 6th ed. New York, NY: McGraw-Hill; 2005:1741-1753.
9. Mockenhaupt M, Messenheimer J, Tennis P, et al. Risk of Stevens-Johnson syndrome and toxic epidermal necrosis in new users of antiepileptics. Neurology. 2005;64:1134-1138.
10. Amerson AB. Allergic and drug-induced skin diseases. In: Herfindal ET, Gourley DR, eds. Textbook of Therapeutics: Drug and Disease Management. 7th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2000:973-988.
11. Beers MH, Porter RS, Jones TV, et al. The Merck Manual of Diagnosis and Therapy. 18th ed. Whitehouse Station, NJ: Merck Research Laboratories; 2006:809,974-975.
12. French LE. Toxic epidermal necrolysis and Stevens-Johnson syndrome: our current understanding. Allergol Int. 2006;55:9-16.
13. Hebert AA, Bogle MA. Intravenous
immunoglobulin prophylaxis for recurrent Stevens-Johnson Syndrome. J Am
Acad Dermatol. 2004;50:286-288.





