US Pharm. 2013;38(7):37-39.
Gas exchange, necessary for life, is the essential function of the lung. By virtue of this exchange, there are potential insults arising from environmental agents—both infectious and noninfectious—that jeopardize this function. Upon insult, if the normal inflammatory and/or repair response is dysregulated, a chronic alveolar or interstitial remodeling process ensues; inflammation and fibrosis manifest in varying degrees.1 Ultimately, gas-exchange abnormalities and restrictive physiology constitute the characteristic pathology of diffuse interstitial lung disease. This term refers to a heterogeneous group of diseases sharing common clinical, radiographic, and physiological characteristics.1,2
Further, insults may arise via the circulation; for example, from a systemic connective tissue disease such as rheumatoid arthritis or systemic sclerosis, or from drugs and treatments. Rheumatologists and other physicians often underestimate the impact of the disorders associated with interstitial lung disease and diagnose respiratory impairment when it has reached an irreversible fibrotic stage.3 In conjunction with the rising median age of the U.S. population, an increase in the use of pneumotoxic drugs to treat malignancies and cardiovascular diseases in the elderly contributes to an increased incidence of interstitial lung disease.1 It is difficult to assess the incidence of true drug-induced pulmonary disease due to pulmonary nonspecificity and the interaction between the current underlying disease and the drugs.4 Alternative names for diffuse interstitial lung disease that may appear in the medical record include diffuse parenchymal lung disease; alveolitis; and idiopathic pulmonary pneumonitis.
Etiology and Risk Factors
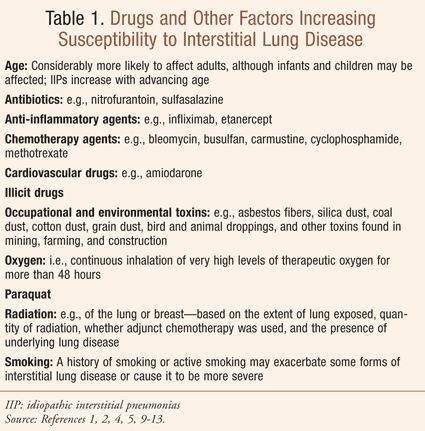
As noted above, the causes of diffuse interstitial lung disease are many and include occupational and environmental factors, medical conditions, drugs and treatments (TABLE 1, RESOURCE). Lung damage may be caused by long-term exposure to various toxins and pollutants, including asbestos fibers, silica dust, coal dust, grain dust, and bird and animal droppings.2 Examples of medical conditions that can result in damage to the lung include rheumatoid arthritis, systemic lupus erythematosus, sarcoidosis, and systemic sclerosis and scleroderma.2,5,6 Chemotherapeutic agents, antibiotics, antiarrhythmic drugs, and immunosuppressive agents can cause drug-induced interstitial lung disease; diagnosis is commonly made when a patient with interstitial lung disease is exposed to a drug that is known to induce lung disease and other causes have been excluded.7 When the cause of diffuse interstitial lung disease cannot be determined, which happens to be the situation in most cases of this condition, it is termed idiopathic interstitial lung disease. Idiopathic pulmonary fibrosis (IPF), a progressively worsening condition characterized by inflammation and fibrosis, is the most prevalent and devastating of all the diffuse interstitial lung diseases.1,5,8 TABLE 2 addresses the potential reasons why the elderly are particularly susceptible to IPF.


Symptoms and Complications
Irreversible lung damage often has already manifested by the time symptoms appear; the primary signs and symptoms of diffuse interstitial lung disease are shortness of breath aggravated by exertion and a dry cough.2 As the disease progresses, patients may develop clubbing (abnormal enlargement of the base of the fingernails) and blue coloring of the lips, skin, or fingernails secondary to cyanosis.5 Patients should not ignore breathing difficulties, since early and accurate diagnosis is important for appropriate treatment and management. TABLE 2 offers guidance for patients regarding when to seek medical attention. Complications include progressive pulmonary hypertension, right-sided heart failure (cor pulmonale), and respiratory failure.2
Diagnostic Testing
Diagnostic testing is imperative, since differential diagnosis is challenging given the variety of disorders that fall under the category of diffuse interstitial lung disease and the spectrum of medical conditions that share their symptomatology.
Examples of testing procedures used to reach a definitive diagnosis include2
• Imaging tests: chest x-ray, CT scan, and echocardiogram
• Pulmonary function tests: spirometry, oximetry, exercise stress test
• Lung tissue analysis: bronchoscopy, bronchoalveolar lavage, surgical biopsy.
Management
Medications and Treatment: Lung scar tissue is irreversible and there are no current treatments that prevent the ultimate disease progression that ensues. However, the goal of medications and treatment is to improve symptoms temporarily and potentially slow the current progress to some degree in an attempt to improve quality of life.2 Primary treatment of interstitial lung disease involves discontinuation of an offending agent and avoidance of further exposure; suppression of active inflammation with the use of systemic corticosteroids (e.g., prednisone) in patients with symptoms or with progressive or disabling disease; and treatment of complications and provision of supportive care.1,4,7 Sometimes the corticosteroid is coadministered with an immunosuppressant (e.g., cyclosporine) as initial therapy; however, long-term effectiveness has not been proven.2 Oxygen therapy is palliative for breathing and exercise; it also prevents or reduces the likelihood of complications secondary to hypoxia.2 In addition to other benefits, the patient may report improvement in sleep and sense of well-being; 24-hour oxygen may be required in some individuals.2 Families should be guided regarding proper oxygen storage and safety.
Pulmonary Rehabilitation: In order to improve and maximize daily functioning, pulmonary rehabilitation focuses on improving endurance of physical exercise, emotional support, and nutritional counseling to ensure adequate calories and nutrients.2,5
Organ Transplantation: For younger people with severe interstitial lung disease who have been refractory to therapy, lung transplantation may be an option of last resort.2,5
Lifestyle Modifications: Participatory health care by the patient is essential to living with diffuse interstitial lung disease. Patients should be counseled regarding options for quitting smoking, i ncluding smoking cessation therapies and programs; avoidance of harmful secondhand smoke requires the patient to disallow others to smoke in their presence.2 A nutritionally rich diet containing adequate calories is imperative, since patients with lung disease are prone to weight loss secondary to burning extra calories just to breathe; nutritional counseling is recommended. Immunizations offer protection against respiratory infections that are capable of worsening the symptoms of interstitial lung disease; the pneumonia vaccination and annual flu vaccination are recommended. Of note, avoidance of illicit drug use may prevent a number of drug-induced lung diseases.9
Patient and Caregiver Coping and Support
The physical and emotional challenges associated with living with chronic lung disease often require adjustments in the patient’s daily routines and activities to accommodate progressive breathing problems and other health care needs. Support groups or psychological counseling may provide comfort in coping with the fear, anger, and sadness associated with the grieving process that one experiences when transitioning from one’s previous active lifestyle to one of a more debilitated state. Furthermore, assigning a health care proxy, planning for and understanding hospice services, including the provision of palliative and end-of-life care, are all important issues to be discussed at appropriate times so that comfort and care of the patient, and support and resources for the family, are readily available at the time of need.
Conclusion
Genetics, age, and the environment contribute to impaired regenerative capacity and fibrosis of lung tissue. Occupational and environmental factors, medical conditions, drugs, and treatments are all culprits. Diffuse interstitial lung disease describes a large group of disorders, most of which cause progressive, generally irreversible scarring of lung tissue; early diagnosis is important. Discontinuation of the offending agent, use of systemic corticosteroids, and supportive care is the primary treatment and is best achieved through a multifaceted approach.
REFERENCES
1. Thannickal VJ, Toews GB. Diffuse parenchymal lung disease. In: Halter JB, Ouslander JG, Tinetti ME, et al, eds. Hazzard’s Geriatric Medicine and Gerontology. 6th ed. New York, NY: McGraw-Hill; 2009:1003-1008.
2. Interstitial lung disease.
MayoClinic.com. Published July 9, 2011.
www.mayoclinic.com/health/interstitial-lung-disease/DS00592. Accessed
June 17, 2013.
3. Marigliano B, Soriano A, Margiotta D,
et al. Lung involvement in connective tissue diseases: a comprehensive
review and a focus on rheumatoid arthritis. Autoimmun Rev. 2013 May 15. Epub ahead of print.
4. Raissy H, Harkins M, Marshik PL. Drug-induced pulmonary diseases. In: DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 8th ed. New York, NY: McGraw-Hill; 2011:511-523.
5. Diffuse interstitial lung disease. MedlinePlus.
U.S. National Library of Medicine. National Institutes of Health.
Updated March 3, 2012.
www.nlm.nih.gov/medlineplus/ency/article/000128.htm. Accessed June 17,
2013.
6. Kobayashi A, Okamoto H. Treatment of interstitial lung diseases associated with connective tissue diseases. Expert Rev Clin Pharmacol. 2012;5:219-227.
7. Schwaiblmair M, Behr W, Haeckel T, et al. Drug induced interstitial lung disease. Open Respir Med J. 2012;6:63–74. www.ncbi.nlm.nih.gov/pmc/articles/PMC3415629. Accessed June 19, 2013.
8. de Lauretis A, Veeraraghavan S,
Renzoni E. Review series: aspects of interstitial lung disease:
connective tissue disease-associated interstitial lung disease: how does
it differ from IPF? How should the clinical approach differ? Chron Respir Dis. 2011;8:53-82.
9. Drug-induced pulmonary disease. MedlinePlus. U.S. National Library of Medicine. National Institutes of Health. Updated June 2, 2011.
www.nlm.nih.gov/medlineplus/ency/article/000104.htm. Accessed June 19, 2013.
10. Cooper JA, White DA, Matthay RA. State of the art: drug-induced pulmonary disease, Part I: Cytotoxic drugs. Am Rev Respir Dis. 1986;133:321-340.
11. Kehrer JP, Kacew S. Systematically applied chemicals that damage lung tissue. Toxicology. 1985;35:251-293.
12. Epocrates, Version 4.5. Epocrates, Inc. www.epocrates.com. Accessed June 19, 2013.
13. Harvey RA, Champe PC, eds. Pharmacology. 4th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2009:205.
To comment on this article, contact rdavidson@uspharmacist.com.





