US Pharm. 2020;45(11)(Specialty&Oncology suppl):9-12.
ABSTRACT: Over 5.5 million children in the United States have a diagnosis of asthma, but children have high rates of poor inhaler technique. Inhaled therapy is the backbone of asthma treatment, necessitating that inhaler-technique education be incorporated at all points of care. Children require individualized teaching to meet appropriate developmental needs. The teach-back method, print and video resources, and interactive technology are options to meet individual learning needs. Dispensing pharmacists are often the last healthcare provider to come in contact with a child before independent inhaler administration, consequently making it imperative for pharmacists to take responsibility for providing developmentally targeted inhaler-technique education.
Pharmacists dispense lifesaving medications routinely; however, some medications require more effort than others to provide their lifesaving value. Arguably, inhalers are among the most challenging medication-delivery devices. Inhalers require multiple administration steps, often with coordinated movements, to obtain a therapeutic dose of medication. Over 5.5 million children in the United States have asthma and likely require mastery of inhaler technique for management.1,2 To that end, the National Heart, Lung, and Blood Institute Guideline on diagnosing and managing asthma recommends reviewing inhaler technique at each healthcare-visit touch point.3 When it comes to counseling children, the U. S. Pharmacopeia recommends that health professionals ensure that the information that is taught is developmentally appropriate.4 Pharmacists are critical members of the healthcare team who can deploy multiple teaching modalities to provide pediatric patients with proper inhaler-technique education.
Metered-Dose Inhaler
Metered-dose inhalers (MDIs) consist of a metal canister that holds liquid medication with a propellant under pressure and a plastic holder that helps to release the medication. When the user presses the canister, the medication particles are propelled toward the throat to be inhaled.5 A 2016 systematic review of inhaler technique in children with asthma found a wide range of proper inhaler use; anywhere from zero to about 57% of children were properly using their MDIs.2 Factors that increased the likelihood of proper inhaler technique included older age, receiving instruction from a family member, reading asthma publications, and receiving more training.2 Directions for proper administration of MDIs can be found in TABLE 1.6,7

Common steps performed incorrectly include inhaling slowly and deeply for 3 to 4 seconds (step 7), holding the breath for 10 seconds (step 8), and waiting in between puffs (step 9).2
MDI Spacer
Medication is propelled from an MDI at a speed of about 60 miles an hour, allowing medication to be lost in the air, stuck inside the mouth or back of the throat, or swallowed.8 The goal of the MDI is to have the medication delivered deep into the lungs, which requires an intricate balance of coordination and timing. The spacer is a device that will modify the complicated administration technique of an MDI and maximize the amount of medication reaching the lungs. Any patient can use a spacer; however, anyone who has difficulty with the complicated administration steps of an MDI should use a spacer to maximize drug delivery. Spacers can be used with either a mouthpiece or a mask. Younger children, specifically those under age 5 years, may need a mask because they are unable to seal their lips around the mouthpiece properly.7 TABLE 2 highlights how to use the spacer with a mask versus a mouthpiece.9,10

Dry-Powder Inhaler
According to a systematic review by Gillette and colleagues, children with asthma used dry-powder inhalers (DPIs) correctly anywhere from zero to 35% of the time.2 As opposed to MDIs, where the medication is propelled into the lungs, DPIs require the user to take a fast, deep breath to activate the medication.11 DPIs are typically not recommended until children are about age 8 years and capable of performing the forceful breath required.12 DPIs come in multiple shapes, including the Diskus, Twisthaler, Flexhaler, and Ellipta. TABLE 3 includes general instructions for using the various devices.13-16 The DPIs each have a unique way of opening the device and activating the dose; however all require the patient to exhale away from the inhaler, place the mouthpiece in the mouth, take a quick deep breath, and hold the breath for 10 seconds. Common steps performed incorrectly include exhaling away from the inhaler (step 4) and holding the breath for 10 seconds (step 6).2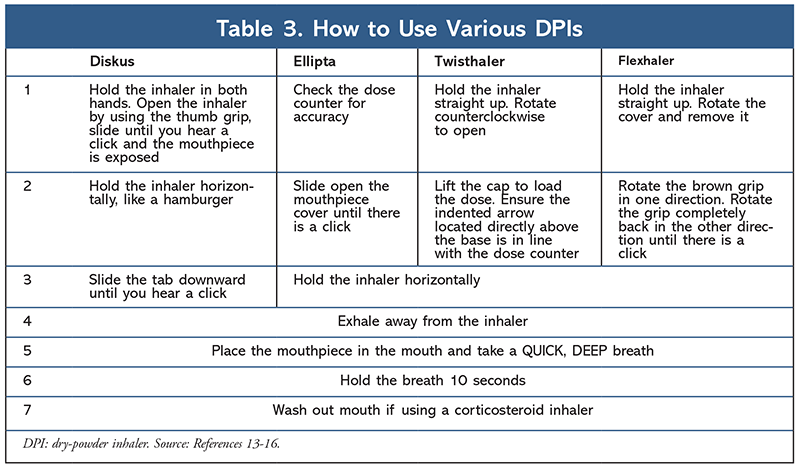
Soft-Mist Inhaler
One of the newer drug-delivery devices used for the treatment of asthma is the soft-mist inhaler (SMI), Respimat. SMIs produce a mist with a smaller particle size, lower velocity, and longer duration of aerosol cloud, implying there would be improved coordination of inhalation with actuation, higher lung deposition, and lower oropharyngeal deposition compared with MDIs.17 Few medications are currently formulated into SMIs; the youngest age indicated for use is 6 years.18 The most common error is not pressing the dose-release button while taking a slow, deep breath (step 7).19 TABLE 4 reviews the teaching points of a Respimat.20,21

Selecting a Delivery Device
Various inhaler delivery devices are available, resulting in prescribers individualizing the asthma regimen to the child. The age of the child plays a vital role in the selection process. Very young children must use an MDI with a spacer, and the caregiver needs to ensure the facemask on the spacer has a good seal for optimal medication delivery.22 As the child ages to about 8 years, the child will have an inspiratory flow rate that is sufficient to inhale through all the different inhaler types.22 In addition to age, it is important to consider the child’s ability to follow directions prior to inhaler selection.23
If the child is unable to follow complex directions, an MDI with a spacer would be the most appropriate therapy. Some children might be able to master one inhaler type, such as an MDI, but get confused when they need to use multiple, different inhaler types such as an MDI and a DPI. If multiple-inhaler-device mastery is of concern, providers can choose a drug regimen that uses one type of delivery device. To account for patient comfort and preference, prior to prescribing, the device should be discussed to ensure an adequate comfort level, because the inhaler is ineffective if it is not used correctly.23 Overall, delivery-device selection is just as important as the drug itself when choosing asthma treatment therapy.
Inhaler Teaching Techniques
Teaching methods for inhaler education include the teach-back method, print, and video resources, and interactive technology. Regardless of what type of teaching technique is used, developmentally appropriate information should be provided.4 Counseling for infants is exclusively directed to the caregiver’s level of health literacy.24 In toddlerhood, counseling is still focused on the caregiver, but the child can understand simple explanations.24 For example, the educator can state that the inhaler will help make it easier to breathe.24 Exhibiting a nonintimidating, nonthreatening, reassuring demeanor while at the child’s eye level allows for a relaxed teaching session. Providers can incorporate a stuffed animal into the inhaler demonstration to make the child feel more comfortable.24 At preschool age, where education is still primarily directed to the caregiver, the child can be involved by allowing him or her to demonstrate how to use the inhaler with the stuffed animal. In early school age, children’s cognitive and logical skills expand.2 Their thinking becomes more concrete, critical, and advanced, allowing understanding of concepts surrounding inhaled therapy.24 Adolescents can be counseled like adults; however, possible social stigma that may be attached to taking medication should be considered.24 Although caregivers still have the overall responsibility for medication administration, pharmacists can direct some counseling to pediatric patients of all ages.24
Teach-Back Method
The teach-back method is recommended by the Global Initiative for Asthma guidelines for inhaler education.25 This method necessitates that the healthcare provider demonstrate the inhaler to the patient and that the patient demonstrate it back.26 Having the patient show the provider how to use the device allows the provider to correct any mistakes or address areas of uncertainty and ensure all information is understood.27 Patients have superior inhaler technique, improved asthma control, and greater adherence when instructed with the teach-back method versus just watching a demonstration by the provider.26
Print/Video Materials
Print resources are readily available from multiple sources, the most common being the package insert. Though easily accessible, when patients read the package insert, there is no statistically significant improvement in inhaler technique.26 Videos are also easily available from sources such as YouTube or the CDC homepage. When compared, there was no statistically significant difference between the two video sources on patient competency with inhaler technique.26 When comparing print with video materials on inhaler technique, video watchers outperformed print participants immediately after seeing the materials; however, a week later the two groups’ performance did not differ.28 The use of the take-home material predicted marginally better recall, which is the major benefit of using print or easily available video resources.28 When employing print or video materials, health literacy of the child and caregiver along with the child’s developmental level must be considered. For younger children, it is important to use more pictures than words. When using words, it is important to choose words the child is able to read and understand. A comic-book education program, Iggy and the Inhalers, designed based on the National Asthma Education and Prevention Program guidelines for children aged 7 to 12 years was designed to improve inhaler technique while factoring in the health literacy of the child.29 Print and video resources are available from a wide variety of locations and when selected appropriately can provide significant added value to the inhaler teaching session.
Interactive Technology
Current technology has allowed application (app) developers to design child-friendly apps for asthma education. The app Wizdy Pets allows children to learn to manage asthma by adopting an asthmatic fire-breathing dragon. The user administers the dragon’s MDI in such a way that each step is reviewed from opening the cap and attaching the spacer to following the appropriate breathe-and-hold technique.30 MySpira is an app designed for children aged 6 to 13 years that uses “aliens” in combination with tactile interactions to teach children good inhaler technique.31 Research showed that children could retain the information 26% better by using this app compared with videos, and 70% better compared with leaflets.31 Other game-style asthma apps designed for slightly older children include The Amazings, where a superhero completes levels to learn about asthma, and ASTHMAXcel Adventures, which includes videos, game play, and multiple-choice questions to test the child’s knowledge.32,33 In addition to asthma game-based apps, symptom-tracking apps such as My Asthma Pal are available. This app allows children and caregivers to track, understand, and manage a child’s asthma by including educational materials, symptom trackers, and medication reminders.34
Conclusion
Delivery of respiratory medications by inhalation achieves a high drug concentration in the airways, more rapid onset of action, and fewer systemic adverse effects than systemic delivery. However, using an inhaler is a skill that must be learned and maintained in order for the medication to be delivered effectively. Multiple teaching techniques are available that can be mixed and matched to individualize teaching to children of all ages. Pharmacists are an excellent resource to help achieve optimal therapy in children, and they have a responsibility to ensure that proper inhaler-technique education is dispensed along with every inhaler prescription.
Disclaimer: The views expressed herein are those of the author and do not reflect the official policy of the Department of the Army, Department of Defense, or the U.S. Government.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
REFERENCES
1. CDC. Most recent national asthma data. www.cdc.gov/asthma/most_recent_national_asthma_data.htm. Accessed April 22, 2020.
2. Gillette C, Rockich-Winston N, Kuhn JA, et al. Inhaler technique in children with asthma: a systematic review. Acad Pediatr. 2016;16(7):605-615.
3. National Heart, Lung, and Blood Institute. Guidelines from the National Asthma Education and Prevention Program. Updated September 2012. www.nhlbi.nih.gov/files/docs/guidelines/asthma_qrg.pdf. Accessed April 24, 2020.
4. Abraham O, Alexander DS, Schleiden LJ, Carpenter DM. Identifying barriers and facilitators that affect community pharmacists' ability to engage children in medication counseling: a pilot study. J Pediatr Pharmacol Ther. 2017;22(6):412-422.
5. How to Use Inhalers Interactive Guidance and Management. How does metered dose inhaler work? Understand your medicine before you inhale. Updated 2013. http://use-inhalers.com/how-does-metered-dose-inhaler-work. Accessed April 22, 2020.
6. How to Use Inhalers Interactive Guidance and Management. Handouts and flyers. Updated 2013. https://use-inhalers.com/patients-handouts. Accessed April 24, 2020.
7. About Kids Health. Asthma: using a a metered dose inhaler (MDI) with a spacer. Updated 2009. www.aboutkidshealth.ca/article?contentid=1476&language=english. Accessed April 24, 2020.
8. Allergy and Asthma Network. Holding chambers/spacers. www.allergyasthmanetwork.org/education/asthma/management-tools/holding-chambers-spacers. Accessed April 24, 2020.
9. American College of Chest Physicians. Using your MDI with a spacer and mask—pediatric patient education guide. www.vapg.com/docs/asthma-mdi-and-spacer-instructions.pdf. 2006.
10. Allergan. Learning how to use your AeroChamber Plus Flow-Vu. Updated 2018. www.aerochambervhc.com/instructions-for-use. Accessed April 24, 2020.
11. American Academy of Allergy, Asthma, and Immunology. Dry powder inhaler definition. www.aaaai.org/conditions-and-treatments/conditions-dictionary/dry-powder-inhalers. Accessed April 24, 2020.
12. About Kids Health. Asthma: using a Diskus inhaler. www.aboutkidshealth.ca/article?contentid=1479&language=english. Accessed April 22,2020.
13. How to Use Inhalers Interactive Guidance and Management. How to use Diskus patient education guide. Updated 2013. https://use-inhalers.com/patients-handouts. Accessed April 24, 2020.
14. How to Use Inhalers Interactive Guidance and Management. How to use Ellipta patient education guide. Updated 2013. https://use-inhalers.com/patients-handouts. Accessed October 5, 2020.
15. How to Use Inhalers Interactive Guidance and Management. How to use Twisthaler patient education guide. Updated 2013. https://use-inhalers.com/patients-handouts. Accessed October 5, 2020.
16. How to Use Inhalers Interactive Guidance and Management. Updated 2013. How to use Flexhaler patient education guide. https://use-inhalers.com/patients-handouts. Accessed October 5, 2020.
17. Anderson P. Use of Respimat Soft Mist inhaler in COPD patients. Int J Chron Obstruct Pulmon Dis. 2006;1(3):251-259.
18. Spiriva. Spiriva for kids. www.spiriva.com/asthma/spiriva-for-kids. Accessed April 24, 2020.
19. How to Use Inhalers Interactive Guidance and Management. Respimat common mistakes. https://use-inhalers.com/common-mistakes-when-using-respimat. Accessed April 24, 2020.
20. How to Use Inhalers Interactive Guidance and Management. How to use Respimat patient education guide. https://use-inhalers.com/patients-handouts. Accessed April 24, 2020.
21. American Association for Respiratory Care. A patient’s guide to aerosol medication delivery. 2017. www.aarc.org/wp-content/uploads/2018/01/aerosol-guides-for-patients-3rd.pdf. Accessed April 24, 2020.
22. van Aalderen WM, Garcia-Marcos L, Gappa M, et al. How to match the optimal currently available inhaler device to an individual child with asthma or recurrent wheeze. NPJ Prim Care Respir Med. 2015;25:14088.
23. Allergy and Asthma Network. Choosing the right asthma delivery device. Updated 2015. www.allergyasthmanetwork.org/choosing-the-right-delivery-device. Accessed April 24, 2020.
24. El-Rachidi S, LaRochelle JM, Morgan JA. Pharmacists and pediatric medication adherence: bridging the gap. Hosp Pharm. 2017;52(2):124-131.
25. Global Initiative for Asthma. Global strategy for asthma management and prevention, 2019. www.ginasthma.org. Accessed April 24, 2020.
26. Axtell S, Haines S, Fairclough J. Effectiveness of various methods of teaching proper inhaler technique. J Pharm Pract. 2017;30(2):195-201.
27. Teachbacktraining.org. Always use teach-back! Using the Teach-back toolkit. www.teachbacktraining.org/using-the-teach-back-toolkit. Accessed April 24, 2020.
28. Wilson EA, Park DC, Curtis LM, et al. Media and memory: the efficacy of video and print materials for promoting patient education about asthma. Patient Educ Couns. 2010;80(3):393-398.
29. Mickel CF, Shanovich KK, Evans MD, Jackson DJ. Evaluation of a school-based asthma education protocol. J Sch Nurs. 2017;33(3):189-197.
30. MassDiGl. Wizdy Pets. https://apps.apple.com/us/app/wizdy-pets/id1499398928. Accessed April 22, 2020.
31. Postelnicu L. New app uses gamification, augmented reality to help children with asthma. August 23, 2019. www.mobihealthnews.com/news/europe/new-app-uses-gamification-augmented-reality-help-children-asthma. Accessed April 24, 2020.
32. Mistry N. App reviews pediatric asthma. https://practicalapps.ca/topics/pediatric-asthma/#the-amazings-noScroll. Accessed April 22, 2020.
33. Montefiore Applications, LLC. ASTHMAXcel Adventures. https://apps.apple.com/us/app/asthmaxcel-adventures/id1424390741. Accessed April 22, 2020.
34. Pai A. Children's Health launches asthma tracking app. 2015. www.mobihealthnews.com/47184/childrens-health-launches-asthma-tracking-app. Accessed April 22, 2020.
To comment on this article, contact rdavidson@uspharmacist.com.





