US Pharm. 2011;37(3):58-60.
With the advent and progression of new vaccines in the pharmaceutical market, some may come to believe that varicella-zoster virus (VZV), also known as chickenpox, has been eradicated and therefore is no longer a health care concern. Since the release of the varicella vaccine in 1995, there has been a significant decrease in infection rates. Deaths and the number of hospitalizations due to infection with VZV have decreased by 90% since 1996.1 However, the CDC reports that from 2001-2005, there were outbreaks in schools that reported vaccination coverage of 96% to 100%. In this population, approximately 11% to 17% of children vaccinated for VZV had a breakthrough infection. Most adults prior to the establishment of the varicella vaccine were thought to have acquired immunity as a consequence of having VZV as a child.1 The CDC states that most breakthrough infections occurred in adolescence; however, adults who received the vaccination in childhood may be at possible risk.1
VZV is extremely contagious.1 Transmission of VZV relies on human vectors that expose one another to infected respiratory secretions or direct contact with lesions.1,2 Clinical manifestations include malaise, headache, and low-grade fever.3 Children typically develop a rash prior to these symptoms; however, adults develop a rash 1 or 2 days after.1 Purulent lesions occur mostly on the face and trunk of the body, and they may also appear on various mucous membranes.1 The rash evolves over several days with multiple stages of the lesions in development.1 Breakthrough infections typically have fewer lesions and are mild, resolving in a few days.4
VZV is typically self-limiting in healthy children; however, complications include secondary bacterial super infection, central nervous system involvement, and Reye’s syndrome.1,2 Pneumonia is a complication that often occurs in adults.5 A person’s age correlates with the risk of developing possible complications. Those younger than 1 year of age or greater than 20 years of age develop these complications more frequently.1
Treatment
Primary infection of VZV is usually self-limiting in healthy children, often only requiring symptomatic treatment for relief of itching. Although no studies exist evaluating the effectiveness of calamine lotion in patients with itching due to VZV, it may be recommended owing to its safety profile and patient or caregiver reported relief.6 Other symptomatic treatments include antipruritic lotions such as those containing camphor and menthol (e.g., Sarna Anti-Itch), oatmeal baths, cool or wet compresses, and tepid baths.2,7 Oral antihistamines including hydroxyzine, loratadine, cetirizine, fexofenadine, and diphenhydramine may help with itching and prevent excoriation from occurring.2,7 Ensuring fingernails are kept short also will help to prevent excoriation. Several reports of topical diphenhydramine toxicity exist in patients with varicella; therefore, it should not be recommended for use, especially in combination with oral diphenhydramine.8-10 Use of salicylates during a varicella infection increases the risk of acquiring Reye’s syndrome; thus acetaminophen and other antipyretics, not including aspirin, should be recommended for fever.2,7
While VZV is usually self-limiting, there are several instances in which antiviral treatment is indicated. Both the Advisory Committee on Immunization Practices (ACIP) and American Academy of Pediatrics (AAP) do not recommend antiviral therapy for healthy children without complications. The AAP does suggest, however, that those at increased risk of moderate-to-severe VZV primary infection be considered for antiviral treatment with acyclovir. These groups include healthy individuals ≥12 years old, pregnant women with serious, viral-mediated complications such as pneumonia, those with chronic cutaneous or pulmonary disorders (e.g., asthma), and persons receiving long-term salicylate therapy or short, intermittent, or aerolized courses of corticosteroids. For best results, antiviral therapy should begin within 24 hours of rash onset (TABLE 1).11
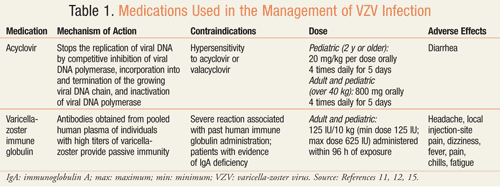
Varicella zoster immune globulin (VZIG) is a varicella-specific immune globulin used to produce passive immunization for the treatment of exposed, susceptible individuals who are at risk of complications from VZV.12 The CDC recommends VZIG within 96 hours of exposure for pregnant women, neonates, and immunocompromised persons at high risk of developing VZV and complications.1 Persons who received two doses of varicella vaccine and then became immunocompromised are not candidates for VZIG.1
Prevention
Two varicella-containing vaccines are available in the
United States for use in children 12 months and older to prevent the
occurrence of VZV (TABLE 2). Varivax (Merck) is a single-agent
vaccine, while ProQuad (Merck) is a combination measles-mumps-rubella
and varicella (MMRV) vaccine. Also available in the U.S. is Zostavax
(Merck), a herpes zoster vaccine FDA approved for persons aged 50 or
older to prevent postherpetic neuralgia caused by the reactivation of
VZV. Although this product is approved for use in those ≥50 years, ACIP
recommendations only recommend it for those ≥60 years.12,13
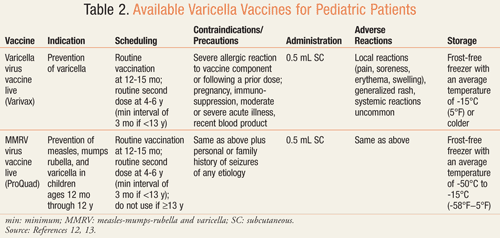
All three varicella-containing vaccines contain live attenuated virus derived from the Oka strain of VZV but in varying amounts. Single-agent varicella vaccine has a lower VZV titer than the titer in the MMRV product, and the herpes zoster vaccine contains the highest titer of all three products. The Oka strain of VZV was isolated in the early 1970s from blister fluid in a healthy child infected with VZV. The varicella single-agent vaccine has been available for use in Asia since 1988 and in the U.S. since 1995. In 2005, the combination MMRV vaccine was approved for use in the U.S. Following the approval of the MMRV vaccine was the herpes zoster vaccine, which was approved in 2006.13
The varicella vaccine has a seroconversion rate of 97% in children ages 12 months to 12 years after one dose with 90% of those maintaining antibody 7 to 10 years after receiving the vaccination. The seroconversion rate is estimated to be 78% in persons 13 years of age or older after one dose and 99% after two doses (second dose given 4-8 weeks after initial dose), with 97% of those receiving two doses maintain antibody for at least a year. The vaccine is 70% to 90% effective against VZV infection, and 90% to 100% effective against moderate or severe disease.13 Even with these positive seroconversion rates, breakthrough VZV infection has been reported. Data from Merck’s routine global postmarketing surveillance system and the Varicella Zoster Virus Identification Program over a 10-year time frame indicate approximately one breakthrough per 10,000 distributed doses occurred, with 51 cases meeting the regulatory definition of serious (1%). Breakthrough VZV infections occurring 142 days after vaccination were associated with wild-type VZV; however, 99% of the reports were not serious in nature, according to regulatory definition.14
Despite the effectiveness of the varicella vaccine, there are adverse effects associated with its use. The 10-year data discussed previously suggests there were 3.4 reports of adverse events for every 10,000 doses administered. It is estimated that approximately 55.7 million single-agent varicella vaccine doses were distributed worldwide during this time.14 The most common adverse reactions following administration of the vaccine include local reactions and generalized rash. Systemic adverse reactions are uncommon with the varicella vaccine. Local reactions, mostly of mild and self-limiting nature, include pain, soreness, erythema, and swelling at the injection site, which are reported by 19% of children and 24% (33% after the second dose) of adolescents and adults.13 Varicella-like rash, both injection site and generalized rash, have been reported following vaccination. Most rashes are maculopapular instead of the usual characteristic vesicular varicella rash. The injection-site rash has been reported by 3% of children and 1% of adolescents and adults (after second dose), while the generalized rash has been reported by 4% to 6% of those receiving the varicella vaccine. The injection-site rash has a median of two lesions present and the generalized rash occurs with an average of five lesions. Injection-site lesions usually appear within 2 weeks after vaccine administration while generalized rashes are typically seen within 3 weeks.13
Although systemic reactions are uncommon, fever is reported by 15% of children and 10% of adolescents and adults within 42 days after receiving the varicella vaccine.13 However, most of these reported fevers have been associated with concurrent illness and not the vaccine itself. Postmarketing surveillance also reported neurologic adverse events including 12 reports of encephalitis, 5 reports of meningitis, and 5 reports of cerebellar ataxis.14 Because varicella is an attenuated live vaccine, the potential for secondary transmission to household contacts is a concern.13
Adverse reactions are similar in patients receiving the MMRV vaccine.13
In 2006, the CDC implemented a routine two-dose childhood varicella vaccination program.1 The CDC decided to change from the one-dose program to two doses after reviewing epidemiologic data from the one-dose program. When comparing the one-dose to two-dose schedules, it was noticed that the two-dose schedule was more effective at preventing VZV disease. Catch-up vaccinations for children and adolescents who only received one dose of varicella are recommended, as well as two doses for adolescents and adults without evidence of varicella immunity.1
Although live attenuated vaccines are not routinely recommended for immunocompromised patients, the CDC recommends varicella vaccine be administered to those with isolated humoral immunodeficiency and patients with leukemia, lymphoma, or other malignancies whose disease is in remission and who are ≥3 months post-chemotherapy treatment. Varicella vaccination should also be considered in HIV-infected children if their CD4+ T-lymphocyte percentage is ≥15%. If children meet these criteria, they should receive two doses of single-antigen varicella vaccine 3 months apart. Varicella vaccination may also be considered in HIV-infected persons with CD4+T-lymphocyte counts ≥200 cells/mL.1
Conclusion
Though the VZV vaccine is available, there is still a very small occurrence of breakthrough infection. In comparison to prevaccination statistics, the incidence of infection has decreased significantly. Therefore, importance lies in parents maintaining updated vaccinations for their children. This not only prevents the spread of infection, but also decreases the severity of those who may be infected.4 A person who experiences a breakthrough infection after receiving varicella vaccine may still infect a healthy person with wild-type virus.14 It has been established that the VZV vaccine is approximately 95% effective in clinical practice.4 However, should a patient experience a primary or breakthrough infection, there are treatments available to reduce the course of the disease and treat symptoms.
REFERENCES
1. CDC. Prevention of varicella: recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR Recomm Rep. 2007;56(No. RR-4):1-40.
2. Carrasco DA, Straten MV, Tyring SK. Treatment of varicella-zoster virus and postherpetic neuralgia. Dermatol Ther. 2000;13:258-268.
3. Whitely R. Varicella-zoster virus. In: Galasso G, Whitely R, Merigan T, eds. Antiviral Agents and Viral Disease in Man. New York, NY: Raven Press; 1990:235.
4. Vazquez M, LaRussa P, Gershon A, et al. The effectiveness of the varicella vaccine in clinical practice. N Engl J Med. 2001;344:955-960.
5. McKendall R, Klawans H. Nervous system complications of the varicella-zoster virus. In: Vinken P, Bruyn G, eds. Handbook of Clinical Neurology. Vol. 34. Amsterdam, Netherlands: Elsevier; 1978:161.
6. Tebruegge M, Kuruvilla M, Margarson I. Does the use of
calamine or antihistamine provide symptomatic relief from pruritus in
children with varicella zoster infection? Arch Dis Child. 2006;91:1035-1036.
7. Habif TP. Warts, herpes simplex and other viral infections. In: Clinical Dermatology. 5th ed. New York, NY: Mosby Elsevier; 2010. www.mdconsult.com. Accessed December 27, 2011.
8. Chan CY, Wallander KA. Diphenhydramine toxicity in three children with varicella-zoster infection. DICP. 1991;25:130-132.
9. Woodward GA, Baldassano RN. Topical diphenhydramine toxicity in a five year old with varicella. Pediatr Emerg Care. 1988;4:18-20.
10. McGann KP, Pribanich S, Graham JA, Browning DG. Diphenhydramine toxicity in a child with varicella. A case report. J Fam Pract. 1992;35:210, 213-214.
11. Chickenpox (varicella). Managing persons at risk for
severe varicella. CDC. www.cdc.gov/chickenpox/index.html. Accessed
December 27, 2011.
12. Facts & Comparisons. Facts & Comparisons eAnswers
[online]. Wolters Kluwer Health, Inc.; 2011.
www.factsandcomparisons.com/facts-comparisons-online.aspx. Accessed
January 2, 2012.
13. CDC. Varicella. In: Atkinson W, Wolfe S, Hamborsky J, ed. Epidemiology and Prevention of Vaccine-Preventable Diseases. 12th ed. Washington, DC: CDC; 2011.
14. Galea SA, Sweet A, Beninger P, et al. The safety profile of varicella vaccine: a 10-year review. J Infect Dis. 2008;197(suppl 2):S165-S169.
15. Lexi-Comp [iPhone app]. Hudson, OH: Lexi-Comp, Inc.; 2010. Accessed January 2, 2012.
To comment on this article, contact rdavidson@uspharmacist.com.





