US Pharm. 2008;33(3):22-25.
Some illnesses are found to
take varied courses in geriatric patients.1 In the elderly, more
complications in gastrointestinal diseases are to be expected and the presence
of comorbidities often make diagnosis and management more difficult.1
For example, initial symptoms and signs of diverticulitis may be less
pronounced in senior patients who have a diminished sensorium, allowing
pathology to advance to a dangerous point prior to symptom development.2,3
They are also less likely to respond to therapy, have more frequent free
perforation, and greater postoperative morbidity and mortality.2
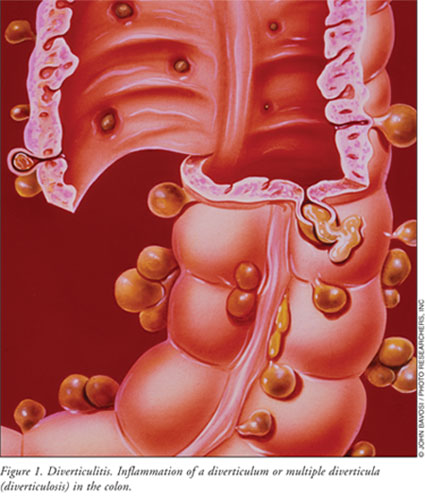
In the colon, the presence of
multiple diverticula (FIGURE 1), protruding pouch-like mucosal sacs
occurring normally or as a result of herniation, is known as diverticulosis
.4 Diverticula are thought to form when pressure inside the colon
builds, usually because of constipation.5 While the exact mechanism
involved is still unclear, this condition is thought to be a result of a
lifelong, low-fiber diet. While colonic diverticulosis is usually
asymptomatic, symptoms may include bloating, mild cramps, and constipation.
5 Dietary interventions (TABLE 1) are geared toward the
prevention of complications such as bleeding and inflammation. Contrary to
common belief, there are no scientific data supporting recommendations to
avoid seeds (e.g., sesame, sunflower, pumpkin, poppy, tomato) or other dietary
substances (e.g., popcorn) that may impact a diverticulum.4,5 In
the United States, approximately 10% of people over the age of 40 have
diverticulosis; frequency increases as age advances, and by age 60 and older,
this disease appears in about 50% of individuals.5
When a micro- or
macroperforation develops in a diverticulum and releases intestinal bacteria
(e.g., aerobic and anaerobic gram-negative bacilli), it is referred to as
diverticulitis.2,4 Inflammation resulting from this perforation
remains localized in most patients (75%), while others (25%) develop
complications (TABLE 1).4 Diverticulitis develops in 10% to
25% of patients with diverticulosis; its incidence increases the longer the
existence of diverticulosis.5,6 Diagnosis is preferably made by
abdominal CT scan with oral and IV contrast. The differential diagnosis
includes appendicitis and cancer of the colon and ovaries. Diverticular
disease (i.e., diverticulosis and diverticulitis) is commonly found in
industrialized or developed nations where low-fiber diets are prevalent (e.g.,
Australia, England, and the U.S.) and rarely in Asia and Africa, where
high-fiber vegetable diets predominate.5

Clinical Features
The most common
signs and symptoms in a patient with diverticulitis are abdominal pain and
tenderness in the left lower quadrant of the abdomen and fever.4,5,7
These may be accompanied by cramps, constipation, and chills.5
Nausea, vomiting, and abdominal distension may indicate bowel obstruction,
which may occur with repeated episodes of diverticulitis.2,4,5
Bleeding is uncommon and usually indicates complications of the disorder.
5 The most serious cases of diverticulitis are usually seen in geriatric
patients, particularly in those taking medications that increase the
likelihood of infection (e.g., prednisone).4 Almost all serious
cases are discovered in the sigmoid region of the colon.4
Treatment
Mild
Diverticulitis: For
mild diverticulitis, in patients that can tolerate oral hydration, treatment
involves rest, a liquid diet, and oral antibiotics.4,8 A course of
broad-spectrum antimicrobial therapy should include coverage targeting
anaerobic microorganisms (i.e., ciprofloxacin plus metronidazole or
amoxicillin/clavulanate plus metronidazole). In the elderly, the lower end of
metronidazole adult dosing guidelines is recommended; ciprofloxacin and
amoxicillin/clavulanate adult dosing should be adjusted carefully based on
renal function.9 Generally, symptoms subside and disappear rapidly
with treatment. After a few days, the patient can start a soft, low-fiber diet
and use a psyllium seed preparation (e.g., Metamucil and Citrucel) daily to
keep the stool soft; after one month, patients can begin a high-fiber diet.
8
Severe Diverticulitis
: People with more severe symptoms, including abdominal pain, fever >101F
(38.3C), marked leukocytosis, inadequate response to oral antibiotics, and
other evidence of serious infection or complications should be hospitalized.
4,8 Treatment involves IV fluids and IV antibiotics (e.g., ceftazidime
sodium plus metronidazole dosed according to renal function), bed rest, and
eating nothing by mouth until symptoms subside.8 Meperidine for
severe pain, titrated to analgesic effect, is preferred to morphine sulfate,
which can cause colonic spasm.2 Approximately 80% of patients can
be successfully treated without surgery.4
Surgery
About 20% of people
with diverticulitis require surgery because their condition does not improve.
8 In recurrent and complicated diverticulitis, the treatment of choice
is surgical resection of the inflamed bowel.10 If an abscess is
discovered, CT-guided percutaneous draining may be attempted before surgery is
considered.8 Emergency surgery may be required for the presence of
a large abscess, perforation, peritonitis, or ongoing bleeding; this usually
requires a colostomy procedure as well, to allow normal nutritional intake and
bowel movements.5 It has been found that among patients with
diverticulitis who are younger than 50 and who require surgery, men outnumber
women three to one; among those over 70 years, women outnumber men three to
one.8
Dietary Measures
During flare-up
periods of diverticulitis, a low-residue diet (<10 g fiber/day) is recommended
to decrease bowel volume and allow the infection to heal.11 Vitamin
and mineral supplementation may be necessary if a low-residue diet is required
for an extended period of time.11 The "Low-Residue Diet for
Diverticulitis" includes the following categories: grain products, fruit,
vegetables, meats and protein, and dairy. Additional fiber is gradually added
to the diet as symptoms of diverticulitis improve with concomitant increase in
fluid intake.11 Recommended maintenance high-fiber foods include:
whole grain breads and cereals; fruit such as apples and peaches; vegetables
including broccoli, cabbage, spinach, carrots, asparagus, and squash; and
starchy vegetables such as kidney beans and lima beans.5 The goal
of a high-fiber diet is to keep the stool soft and lower pressure inside the
colon so that bowel contents move through it easily.
Conclusion
While most patients
with diverticulosis are symptom free, it may result in bleeding or rupture,
causing inflammation or infection, known as diverticulitis. In the
elderly, since initial signs and symptoms of diverticulitis may be less
pronounced and postoperative morbidity and mortality are greater, it is
essential that prompt referral for medical attention and intervention is
sought. Patients with mild symptoms are treated with rest, a liquid diet, and
oral antibiotics, whereas those with severe symptoms are hospitalized and
treated with IV antibiotics and sometimes surgery.8 Pharmacists are
often in a unique position to guide patients to prompt interventional care
when they are informed about the recognition and treatment of this
gastrointestinal condition.
REFERENCES
1. L¸hrs H, Melcher R. Special gastrointestinal problems of elderly patients. MMW Fortschr Med. 2007;149:29-32.
2. Bharucha AE, Camilleri M. Common Large Intestinal Disorders. In: Hazzard WR, Blass JP, Halter JB, et al. Principles of Geriatric Medicine and Gerontology. 5th ed. New York, NY: McGraw-Hill, Inc.; 2003:646-648.
3. Bryan ED. Abdominal pain in elderly persons. Emedicine.com. Available at: www.emedicine.com/EMERG/topic931.htm. Accessed February 15, 2008.
4. Beers MH, Porter RS, Jones TV, et al. The Merck Manual of Diagnosis and Therapy. 18th ed. Whitehouse Station, NJ: Merck Research Laboratories; 2006:159-161.
5. Diverticulosis and diverticulitis. National Institute of Diabetes and Digestive and Kidney Diseases, National Institutes of Health of the U.S. Department of Health and Human Services. Available at: http://digestive.niddk.nih.gov/diseases/pubs/diverticulosis/. Accessed February 14, 2008.
6. Beers MH, Berkow R, eds. The Merck Manual of Geriatrics. 3rd ed. Whitehouse Station, NJ: Merck & Co.; 2000:1054-1057.
7. Dipiro JT, Howdieshell TR. Intraabdominal Infections. In: DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 6th ed. New York, NY: McGraw-Hill; 2005:2056-2059.
8. Diverticulitis. The Merck Manuals Online Library. Available at: www.merck.com/mmhe/sec09/ch128/ch128c.html?qt=intestinal%20bleeding&alt=sh. Accessed February 13, 2008.
9. Semla TP, Beizer JL, Higbee MD. Geriatric Dosage Handbook. 12th ed. Hudson, OH: Lexi-Comp, Inc.; 2007:309-314,1011-1013.
10. Zapletal C, Woeste G, Bechstein WO, Wullstein C. Laparoscopic sigmoid resections for diverticulitis complicated by abscesses or fistulas. Int J Colorectal Dis. 2007;22:1515-1521.
11. Diverticulitis Diet. Health
Castle Nutrition. vailable at: www.healthcastle.com/diverticulitis_diet.shtml.
Accessed January 31, 2008.
To comment on this article, contact
editor@uspharmacist.com.





