US Pharm. 2019:44(60):8-11.
The costs of prescription drugs continue to increase in the United States. Medicare prescription drug coverage—Medicare Part D, the major source of payment for prescription drugs for people aged 65 years and older—remains complex and dynamic.1,2 The estimated expenditure for Medicare Part D, made by the Congressional Budget Office, is expected to total $99 billion in 2019, accounting for 15% of net Medicare outlays.3 Overall, Medicare’s share of retail prescription-drug spending has increased from 18% in 2006 to 30% in 2017.4 As a major payer for retail prescription drugs, Medicare is second only to private insurance.
The average annual growth rate in per-beneficiary costs for Part D is projected to be higher in the next decade (4.6%) than it was between 2010 and 2017 (2.2%).3 Higher Part D program costs associated with expensive specialty drugs are partly to blame, and they are expected to be reflected in higher reinsurance payments from Medicare to Part D plans.3 Projections indicate Part D benefits spending will increase from 15% of net Medicare spending in 2017 to 18% in 2028.5 Furthermore, Medicare is highly regulated; Centers for Medicare and Medicaid oversight and approval are required for programs, fees, and reimbursement.2
In an effort to contain rising drug costs, government proposals could change some features of the Part D benefit and other aspects related to Medicare drug coverage and reimbursement.3 Whatever any future adjustments to Medicare drug coverage may bring, at present, cost concerns among older adults constitute a barrier to medication adherence. It has become clear that a “cost conversation” needs to take place with every patient so that out-of-pocket cost, cost and coverage, and cost of illness are addressed in light of their potential impact on cost-related medication nonadherence.6-9
Defining Adherence
Individuals are considered adherent to medication therapy when they take prescribed agents at the doses and times recommended by their healthcare provider and agreed to by the patient.10 The term medication persistence refers to the length of time from therapy initiation to discontinuation.10
One way researchers have measured adherence is in terms of hospitalization for selected high-prevalence chronic diseases, using adherence metrics derived from pharmacy-claims data and insurance-claims data.10 (For further discussion of adherence metrics, see Reference 10.) For example, one of the most common reasons for hospital admissions in patients aged 65 years and older is heart failure (1 million hospitalizations estimated annually); healthcare expenditures for heart failure in 2010 were approximately $32 billion.11 Medication nonadherence and lifestyle contribute to hospital admissions in up to one-third of patients.11
Pharmacist-Provided MTM
Unnecessary drug therapy and over-medication are common problems with drug use in older adults; projected estimates for elderly patient polypharmacy alone are $1.3 billion per year.12 Polypharmacy regimens can be complex, burdensome, and costly for patients, which may increase the risk for medication nonadherence.
Approximately 10% of initial prescriptions written by physicians are never filled.13 Despite evidence that medication therapy prevents death and improves quality of life, patients with chronic conditions adhere to only 50% to 60% of medications as prescribed.14-19 Poor adherence to cardiovascular-related medications has been noted to lead to considerable morbidity, mortality, and avoidable healthcare costs.20
Demonstrated improvements in medication adherence for patients taking drugs for cholesterol management, gastroesophageal reflux disease, and thyroid and benign prostatic hyperplasia have been noted, based on a study of pharmacist-provided comprehensive medication review to Medicare beneficiaries in community pharmacies.21
Several other studies underscore the benefit of pharmacist-provided medication therapy management (MTM) by demonstrating increased medication adherence, improved outcomes, and reduced overall medical costs.22,23 The high, and still rising, cost of prescription medications, however, often leads to cost-related medication nonadherence or underuse.
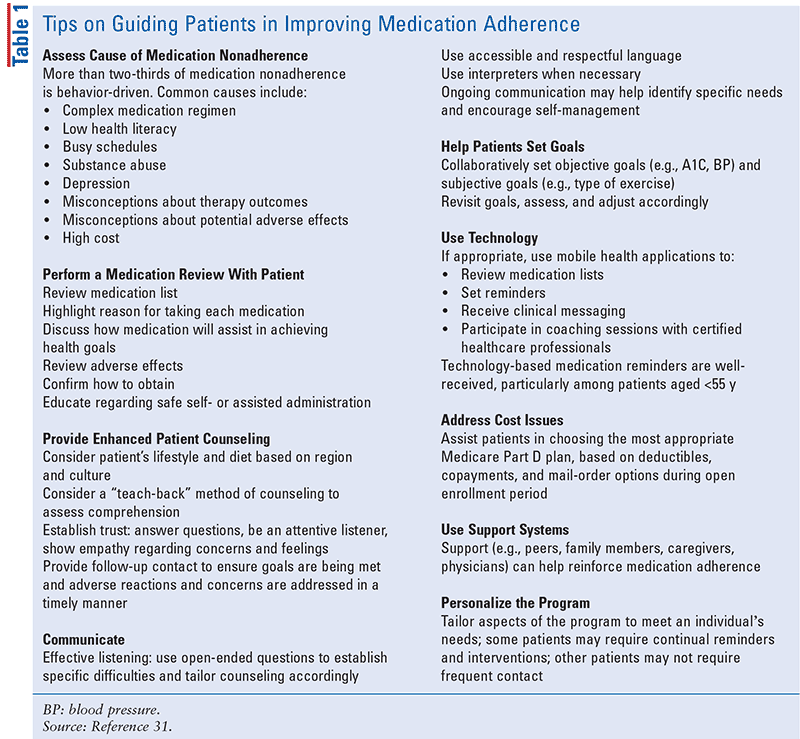
There are programs to support pharmacists with medication-adherence counseling and educational efforts: for example, the no-fee service available through the National Community Pharmacists Association called Simplify My Meds.24 Some companies have been developing and introducing patient-centric technology to streamline patient access to complex drug therapies, accurately train patients on how to administer treatment, and engage with patients through mobile applications.25 See TABLE 1 for adherence counseling guidance and SIDEBAR for examples of these platforms and technologies.
The Cost of Medication Underuse
Strategies for improving medication adherence at care transitions have recently been discussed by Miranda and colleagues as a means to address cost-related medication underuse (CRMU) by patients.6 Pharmacists should be aware that according to the research literature, the highest risk of CRMU appears to involve a range of patients including those with a high disease burden, low household income, no prescription drug coverage, and who are under age 65 years.26-28 The researchers indicate that although there is an absence of a specific definition in the literature, CRMU is a patient-centered, medication-related problem that exists in spite of commonly employed practices to limit medication cost.29
Through conducting medication-cost conversations, a patient-specific plan can be developed to address concerns and actual medication costs. An algorithm addressing patient-specific strategies to reduce CRMU for 1) all patients; 2) uninsured or underinsured patients; and 3) insured patients with government insurance or commercial insurance can be found in Reference 6. For example, the process for all patients regardless of insurance-coverage status includes:
• Recommend generic medications
• Practice deprescribing
• Help select an ideal outpatient pharmacy for the individual.6
Other recommended strategies, depending on insurance-coverage status, include referring the patient to a community health center or free pharmacy; helping him or her apply for manufacturer patient-assistance program(s); regularly reviewing the formulary; referring the patient to a State Health Insurance Assistance Program counselor; and helping the patient with accessing or applying for copay-assistance programs.6
Telepharmacy in the U.S. has advanced over the past decade, and its market is predicted to reach $3.2 billion by 2020—approximately 13% of the $22 billion telemedicine market.30 With regard to medication adherence, when telepharmacy is optimized—using remotely positioned pharmacists—it allows implementation and expansion of on-site clinical initiatives such as medication reconciliation and discharge management, underscoring a focus on medication-adherence support.
Conclusion
The program that pays for the largest share of prescription drug costs for older adults, Medicare Part D, is grappling with rising drug costs, as are the patients it insures. Older adults in the U.S. use more medications than other age groups. Medication nonadherence is an important public health consideration, affecting health outcomes and overall healthcare costs. Pharmacists can continue to guide patients to improve medication adherence with technology for education and counseling, with patient-centric mobile applications for reminders and adherence monitoring, and by optimizing telepharmacy where appropriate. Importantly, pharmacists need to raise awareness that a cost conversation needs to take place with every patient so that concerns and actual cost difficulties and impossibilities are preempted, and cost-related medication nonadherence is mitigated and prevented.
REFERENCES
1. Kesselheim AS, Avorn J, Sarpatwari A. The high cost of prescription drugs in the United States: origins and prospects for reform. JAMA. 2016;316(8):858-871.
2. Navarro R. Introduction to Medicare and Medicaid. In: Whalen K, Hardin HC. Medication Therapy Management: A Comprehensive Approach, 2nd ed. 1-19.
3. KFF. Henry J. Kaiser Family Foundation. The Medicare Part D prescription drug benefit. October 12, 2018. www.kff.org/medicare/fact-sheet/an-overview-of-the-medicare-part-d-prescription-drug-benefit/. Accessed May 6, 2019.
4. KFF. Henry J. Kaiser Family Foundation. 10 essential facts about Medicare and prescription drug spending. January 29, 2019. www.kff.org/infographic/10-essential-facts-about-medicare-and-prescription-drug-spending/. Accessed May 6, 2019.
5. Cubanski J, Neuman T. Issue brief: the facts on Medicare spending and financing. KFF. Henry J Kaiser Family Foundation. June 2018:1.
6. Miranda AC, Serag-Bolos ES, Cooper JB. Cost-related medication underuse: strategies to improve medication adherence at care transitions. Am J Health-Syst Pharm. 2019;76(8):560-565.
7. Alexander GC, Casalino LP, Meltzer DO. Physician strategies to reduce patients’ out-of-pocket prescription costs. J Health Care Poor Underserved. 2005;165:633-636.
8. Hunter WG, Zhang CZ, Hesson A, et al. What strategies do physicians and patients discuss to reduce out-of-pocket costs? Analysis of cost-saving strategies in 1,755 outpatient clinic visits. Med Decis Making. 2016;36:900-910.
9. Hunter WG, Hesson A, Davis JK, et al. Patient-physician discussions about costs: definitions and impact on cost conversation incidence estimates. BMC Health Serv Res. 2016;16:108.
10. Iuga AO, McGuire MJ. Adherence and health care costs. Risk Manag Healthc Policy. 2014;7:35-44.
11. Davis EM, Packard KA, Jackevicius CA. The pharmacist role in predicting and improving medication adherence in heart failure patients. J Manag Care Spec Pharm. 2014;20(7):741-755.
12. Karnon J, McIntosh A, Dean J, et al. Modeling the expected net benefits of interventions to reduce the burden of medication errors. J Health Serv Res Policy. 2008;13:85-91.
13. Aitken H, Valkova S. Exhibit 1: avoidable U.S. healthcare costs add up to $213 billion. Avoidable costs in U.S. healthcare: the $200 billion opportunity from using medicines more responsibly. Report by the IMS Institute for Healthcare Informatics. June 2013:3.
14. Benner JS, Glynn RJ, Mogun H, et al. Long-term persistence in use of statin therapy in elderly patients. JAMA. 2002;288(4):455-461.
15. Avorn J, Monette J, Lacour A, et al. Persistence of use of lipid-lowering medications: a cross-national study. JAMA. 1998;279(18):1458-1462.
16. Feldman R, Bacher M, Campbell N, et al. Adherence to pharmacologic management of hypertension. Can J Public Health. 1998;89(5):116-118.
17. Flack J, Novikov SV, Ferrario CM. Benefits of adherence to antihypertensive drug therapy. Eur Heart J. 1996;17(Suppl A):16-20.
18. Mallion JM, Baguet JP, Siche JP, et al. Compliance, electronic monitoring and antihypertensive drugs. J Hypertens Suppl. 1998;16(1):S75-S79.
19. Haynes RB, McKibbon KA, Kanani R. Systematic review of randomised trials of interventions to assist patients to follow prescriptions for medications. Lancet. 1996;348(9024):383-386.
20. Bosworth HB, Granger BB, Mendys P, et al. Medication adherence: a call for action. Am Heart J. 2011;162(3): 412–424.
21. Branham A, Moose J, Ferreri S, et al. Retrospective analysis of medication adherence and cost following medication therapy management. Innov Pharm. 2010;1(12):1-8.
22. Cranor CW, Bunting BA, Christensen DB. The Asheville project: long-term outcomes of a community pharmacy diabetes care program. J Am Pharm Assoc. 2003;43:183-194.
23. McClean DL, McAlister FA, Johnson JA, et al. A randomized trial of the effect of community pharmacist and nurse care on improving blood pressure management in patients with diabetes mellitus. Arch Intern Med. 2008;168:2355-2361.
24. Appold K. Nine ways to help patients better adhere to their medications. Drug Topics. March 5, 2019. www.drugtopics.com/article/nine-ways-help-patients-better-adhere-their-medications. Accessed May 6, 2019.
25. Shelley S. Improving medication adherence with technology: the longstanding adherence problem is yielding to new technology. Pharmaceutical Commerce. 2019;14(1):22-25.
26. Kennedy J, Morgan S. Health care access in three nations: Canada, insured America, and uninsured America. Int J Health Serv. 2006;36:697-717.
27. Zivin K, Ratliff S, Heisler MM, et al. Factors influencing cost-related nonadherence to medication in older adults: a conceptually based approach. Value Health. 2010;13:338-345.
28. Strickland WJ, Hansen CM. Coping with the cost of prescription drugs. J Health Care Poor Underserved. 1996;7:50-62.
29. Choudhry NK, Saya UY, Shrank WH, et al. Cost-related medication underuse prevalence among hospitalized managed care patients. J Hosp Med. 2012;7:104-109.
30. Duff BL. How pharmacy will change in 2019: four trends that will shape business and the profession. Drug Topics. 2019;163(1):14-18.
31. Zagaria MA. Addressing challenges of infection: antibiotic adverse drug events in older adults. US Pharm. 2019;44(4):6-12.
To comment on this article, contact rdavidson@uspharmacist.com.