US Pharm. 2016;41(12):30-34.
ABSTRACT: Drug-induced liver injury (DILI) is an uncommon, but potentially fatal, cause of liver disease that is associated with prescription medications, OTC drugs, and herbal and dietary supplements (HDS). DILI has two types: intrinsic and idiosyncratic. Patient, environmental, and drug-related factors may play a role in the pathogenesis of DILI. In the United States, antibiotics and antiepileptic drugs are the most common drug classes associated with DILI, but HDS are on the rise as a cause. Management of DILI involves the removal of the offending agent and the use of N-acetylcysteine for acetaminophen-induced liver injury. Outcomes vary depending on the drug used and type of liver injury sustained. Pharmacists can play an essential role in the evaluation of DILI, especially in patients taking multiple medications and supplements.
Drug-induced liver injury (DILI; also known as drug-induced hepatotoxicity) is caused by medications (prescription or OTC), herbal and dietary supplements (HDS), or other xenobiotics that result in abnormalities in liver tests or in hepatic dysfunction that cannot be explained by other causes.1 There are two types of DILI: intrinsic and idiosyncratic. Intrinsic DILI refers to liver toxicity induced by a drug in a predictable and dose-related manner (e.g., acetaminophen [APAP]); idiosyncratic DILI, which occurs less frequently, is associated with a less consistent dose-toxicity relationship and a more varied presentation.2
The true prevalence of DILI is hard to ascertain because premarketing clinical trials are underpowered to detect the presence of idiosyncratic DILI.3 However, DILI is estimated to have an annual incidence of 10 to 15 per 10,000 to 100,000 persons exposed to prescription medications. Therefore, about 44,000 people in the United States will experience DILI annually, making it costly in terms of not only its toll on humans, but also healthcare expenditures. This prevalence is expected to increase with the widespread use of HDS.4,5 Of the 2,000 cases of acute liver failure (ALF) that occur in the U.S. each year, medications account for >50%, with 37% of cases attributable to APAP and 13% attributable to idiosyncratic adverse drug reactions.6
Mechanisms of DILI
DILI is thought to occur via several different mechanisms. Among these are direct impairment of the structural (e.g., mitochondrial dysfunction) and functional integrity of the liver; production of a metabolite that alters hepatocellular structure and function; production of a reactive drug metabolite that binds to hepatic proteins to produce new antigenic drug-protein adducts, which are targeted by hosts’ defenses (the hapten hypothesis); and initiation of a systemic hypersensitivity response (i.e., drug allergy) that damages the liver.7-9
Drugs Associated With DILI
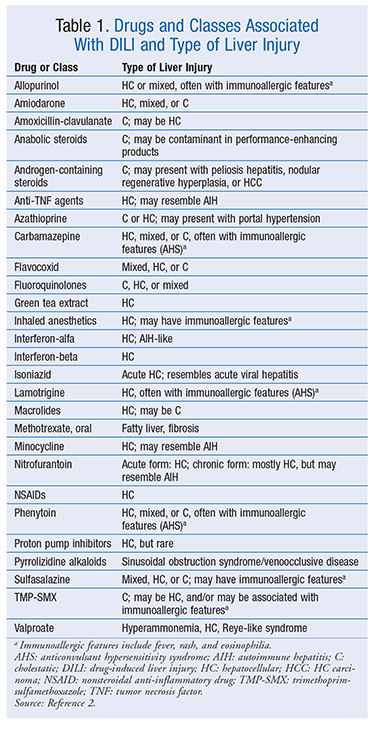
More than 60% of cases of DILI are attributed to antibiotics and antiepileptic agents. The American College of Gastroenterology (ACG) clinical guidelines on idiosyncratic DILI have identified the most common and well-described DILI-associated agents, as well as their pattern of liver injury (TABLE 1).2
LiverTox (https://livertox.nih.gov) is a clinical and research database developed by the National Institute of Diabetes and Digestive and Kidney Diseases, the National Library of Medicine, and the Drug-Induced Liver Injury Network (DILIN) study group to provide up-to-date, comprehensive clinical information on DILI. LiverTox includes an overview of medications (their chemical nature, indications, recommended dosages, and frequency of use), a description of the pattern and course of liver injury, case histories with laboratory data, and a comprehensive list of references.10 Pharmacists should routinely consult LiverTox for the most current information on DILI because there is much variation in standard drug compendia and published reports regarding the potential hepatotoxicity of medicinal products.11-14 Another drug reference list, DILIrank, contains information on 1,036 FDA-approved medications ranked according to their potential to cause DILI.15 Additionally, the FDA has developed a software program, eDISH (evaluation of drug-induced serious hepatotoxicity), to scan large numbers of participants in clinical trials for signs of DILI (i.e., elevated serum alanine aminotransferase [ALT] or total bilirubin).16,17
HDS-Induced Liver Injury
There has been a dramatic increase in the number of cases of DILI caused by HDS. Data from the DILIN study showed an increase from 7% to 20% between 2004 and 2013. The most common HDS associated with the development of DILI in the U.S. are bodybuilding and weight-loss supplements. Bodybuilding HDS produced prolonged jaundice, but no fatalities, in otherwise healthy young men. Nonbodybuilding HDS produced hepatocellular DILI primarily in middle-aged women and were more likely (in 13%) to result in death or in the need for liver transplant.18 Unlike prescription and nonprescription medications in which both the active and inactive ingredients are well characterized, HDS often contain variable substances (i.e., differing potencies of the main ingredient, adulterants). They also lack regulatory oversight, which makes an assessment of DILI very difficult to perform.2,19,20 HDS associated with a positive rechallenge for DILI include green tea extract, senna glycosides, centella asiatica, greater celandine, isabgol, and Venencapsan.21
Risk Factors
DILI is rare, but predisposing factors have been identified that may place a patient at greater risk for developing it. Patient risk factors that may contribute to DILI include genetics, age (older or younger), gender (female), race, pregnancy, malnutrition, gut microbiome, hormonal status, obesity, diabetes mellitus, comorbidities including preexisting liver disease or HIV, and indications for therapy (e.g., hepatitis C).2,3,22-25 Environmental factors that may increase the risk of DILI are smoking, alcohol consumption, and infections or inflammatory episodes.2
Drug-related factors may also contribute to the development of DILI, including the daily dose (i.e., >50 mg/day), metabolic profile (i.e., the more extensively metabolized, the greater the risk), class effect and cross-sensitization (as seen with anticonvulsants), and drug interactions or polypharmacy. Daily doses of >50 to 100 mg of drugs with greater lipophilicity (i.e., octanol-water partition coefficient ≥3) appear to be more inducive of DILI compared with doses <50 mg/day of less lipophilic agents. Higher doses may lead to increased intrahepatic levels of the parent drug or metabolite; greater lipophilicity may require more extensive metabolism, which can lead to covalently bound haptens that produce an adverse immune response in genetically susceptible individuals.26-31 Drug-induced autoimmune hepatitis occurs more commonly with drugs that undergo extensive hepatic metabolism.32 Ninety percent of ALF cases occurred in patients receiving ≥50 mg/day.33 Further, drugs that are metabolized via CYP2C9 or CYP2C19 appear to be associated with a greater risk of DILI than medications metabolized by CYP3A or CYP2D6.34
Assessment of Causality
DILI is a diagnosis of exclusion based on a careful history, including information about prescription and nonprescription agents and HDS, appropriate laboratory testing, hepatobiliary imaging, and liver biopsy, when indicated.2 Elevations of ALT without signs of liver dysfunction are not considered serious because the liver frequently adapts and becomes tolerant to the drug. In adaptation, continued exposure to the drug (e.g., statins) leads to normalization or stabilization of the liver enzymes.35 In performing a pharmaceutical-intake assessment, it is essential to develop an accurate timeline regarding the use of a substance and the onset and course of liver-chemistry abnormalities.2 Although the time to onset of signs and symptoms of DILI may vary, most cases occur within the first 6 months of exposure to a medicinal product.2
Besides DILI, other conditions to rule out include viral hepatitis (i.e., hepatitis A, B, C, and possibly E) and other viral infections (e.g., cytomegalovirus, Epstein-Barr or herpes simplex), autoimmune hepatitis, ischemic liver injury, Budd-Chiari syndrome (thrombotic or nonthrombotic obstruction of hepatic venous outflow),36 and Wilson disease (autosomal recessive inherited disorder of copper metabolism).37 In general, liver biopsy is not necessary because it only infrequently yields a definitive diagnosis of DILI. Cholestatic DILI takes longer to resolve than hepatocellular DILI. A significant decrease in ALT should occur within 30 to 60 days in hepatocellular DILI, whereas in cholestatic DILI a significant decrease in serum alkaline phosphatase (ALP) and bilirubin may take up to 180 days.2
Clinical chemistry criteria for the presence of DILI include any of the following: ≥5-fold elevation above the upper limit of normal (ULN) for ALT; ≥2-fold elevation above the ULN for ALP; and ≥3-fold elevation in ALT with simultaneous elevation of bilirubin exceeding two times the ULN.38 The R value is used to define the pattern of liver injury. It is equal to ALT/ULN divided by ALP/ULN. An R value ≥5 indicates a hepatocellular pattern of liver injury, whereas a value <2 refers to a cholestatic-type pattern; a value of 2 <R <5 represents a mixed hepatocellular and cholestatic-type pattern of DILI. However, patterns of injury and clinical features may vary for the same drug.2
Although the gold standard for diagnosing idiosyncratic DILI remains expert consensus opinion,2 several tools can assist in the assessment.39 Among these are RUCAM (Roussel Uclaf Causality Assessment Method), which was developed by the Council for International Organizations of Medical Sciences (CIOMS), and the Maria and Victorino (M&V) scale.40-42 Based on scores calculated for RUCAM, the likelihood of a drug-induced event is rated as follows: <0, drug excluded; 1-2, unlikely; 3-5, possible; 6-8, probable; and >8, highly probable. RUCAM is widely used by clinicians, the pharmaceutical industry, and regulatory agencies to assess the risk of DILI.2 The M&V scale42 (also known as the Clinical Diagnostic Scale) is a modified version of the CIOMS/RUCAM scale, but it has limitations, including its focus on hypersensitivity features of DILI, which are not always present; reliance on a small number of expert opinions; poor performance in cases involving atypical presentation or long latency; and inadequate concordance with the CIOMS/RUCAM scale.3,32,43 Electronic files of these causality-assessment tools are available on the LiverTox website.44 The clinical practice guidelines on DILI advise that consensus expert opinion (following a thorough evaluation of possible etiologies for hepatotoxicity) is the current gold standard for determining causality, but that, for practical reasons, it is not widely used and cannot be recommended for clinical practice.2 Therefore, the method of choice for causality assessment of suspected DILI is the CIOMS/RUCAM scale.32,43
Treatment
The mainstay of management for DILI is withdrawal of the offending agent as early as possible. Although it has not been proven, quick discontinuation is believed to minimize progression to ALF. Corticosteroids are beneficial for alcoholic hepatitis and autoimmune hepatitis, but they have not been adequately studied in DILI.2 Nonetheless, it has been recommended to manage drug-induced autoimmune-like hepatitis with drug withdrawal and corticosteroids.45 Corticosteroid therapy may also be considered if laboratory abnormalities do not resolve after 6 to 8 weeks, especially if the suspected drug is associated with an immune basis for DILI.46
N-acetylcysteine (NAC) has an established use in APAP toxicity, but its role is being explored in non–APAP-related DILI. According to the ACG clinical practice guidelines, NAC may be considered in adults with early-stage ALF, but it is not recommended in children with severe DILI because of its association with lower survival in non–APAP-induced ALF.2 A review of published data from 2003 to 2012 found that NAC conferred marginal benefit in non–APAP-induced ALF with coma grades I or II and that its routine use cannot be recommended.47 A systematic review of NAC for non-APAP DILI is currently being conducted.48 NAC is not FDA-approved for non–APAP-induced ALF.
Ursodeoxycholic acid has been used to manage patients with cholestatic DILI; however, data supporting this use are limited. Carnitine has been administered in valproate-induced liver injury.49 Natural products such as silymarin, resveratrol, curcumin, and ginkgo are being investigated for possible hepatoprotective effects, although data are preliminary.50 Plasma exchange, molecular adsorbents recirculatory systems, and fractionated plasma separation and adsorption have been used in ALF.51
Outcomes
Hy’s law refers to the likelihood of developing ALF following exposure to a hepatotoxic drug.52 According to Hy’s law, for every 10 patients who develop jaundice secondary to hepatocellular injury during a clinical trial, one patient will develop ALF involving coagulopathy or encephalopathy.53,54 Further, Temple’s corollary states that for every 10 cases of ALT >10 times the ULN in a clinical trial, there will be one instance of Hy’s law.55 In its guidance for industry on the premarketing clinical evaluation of drug-induced liver injury, the FDA has defined the risk of developing severe DILI based on Hy’s law.56
DILI, which is the leading cause of ALF in the U.S., results in ALF more often than viral hepatitis does.32 The type of DILI plays a role in outcome. APAP-induced liver injury has a better prognosis and a more self-limited duration of injury because of faster hepatocyte regeneration compared with idiosyncratic DILI; the liver-transplantation rate is 9%, with 70% overall short-term survival for APAP-induced liver injury.2,57 Acute hepatocellular DILI is the most common form of idiosyncratic DILI, accounting for about 90% of cases, and is associated with a 10% to 50% mortality rate.58 Mortality rates are as high as 60% to 80% in ALF secondary to idiosyncratic DILI when liver transplantation is not performed.54
The rate of chronic DILI is increasing, and the condition may be more common than previously thought, occurring in up to 15% to 20% of patients with acute DILI. Antibiotics (e.g., amoxicillin-clavulanate, trimethoprim-sulfamethoxazole, azithromycin) are the drug class most often associated with the development of chronic DILI. Risk factors for the development of chronic DILI include cholestatic-type DILI, age ≤65 years, and a latency period of >365 days since last drug exposure.2,59
The Registry of Hepatotoxicity in southern Spain revealed that 5.7% of cases of idiosyncratic DILI resulted in chronic hepatotoxicity, which was defined as a persistent biochemical abnormality of hepatocellular pattern of damage >3 months after drug withdrawal or >6 months after cholestatic or mixed damage. Although cardiovascular and central nervous system agents accounted for 9.8% and 13%, respectively, of overall causes of DILI, these drug classes were associated with chronic hepatotoxicity in 28.5% and 25% of patients, respectively.60
Rechallenge with the suspected hepatotoxin should not be attempted, unless there is no suitable alternative for a life-threatening condition. A more rapid and severe—and possibly fatal—reaction may occur upon subsequent reexposure, especially if liver-function tests were initially greater than five times the ULN, patients met the criteria for Hy’s law, or jaundice was present.2
Conclusion
The number of cases of DILI is expected to rise because of the increased availability of prescription medications resulting from changes in insurance coverage and the burgeoning HDS market. Pharmacists can play an integral role in helping prevent DILI and in identifying DILI when it does occur so that the offending agent can be discontinued, if possible. In order to best protect their patients, pharmacists must be knowledgeable about the drugs associated with DILI, as well as their clinical features and the disease course. It is essential to perform a thorough medication history in a patient suspected of experiencing DILI. Once DILI is confirmed, patients should be followed for a minimum of 6 months to assess for the development of chronic injury. Medication therapy management is one tool pharmacists can use to help identify patients who have DILI or are at risk for it.
REFERENCES
1. Suk KT, Kim DJ. Drug-induced liver injury: present and future. Clin Mol Hepatol. 2012;18:249-257.
2. Chalasani NP, Hayashi PH, Bonkovsky HL, et al; Practice Parameters Committee of the American College of Gastroenterology. ACG Clinical Guideline: the diagnosis and management of idiosyncratic drug-induced liver injury. Am J Gastroenterol. 2014;109:950-966.
3. Andrade RJ, Robles M, Fernández-Castañer A, et al. Assessment of drug-induced hepatotoxicity in clinical practice: a challenge for gastroenterologists. World J Gastroenterol. 2007;13:329-340.
4. Bell LN, Chalasani N. Epidemiology of idiosyncratic drug-induced liver injury. Semin Liver Dis. 2009;29:337-347.
5. Larson AM. Drug-induced liver injury. UptoDate. www.uptodate.com/contents/drug-induced-liver-injury. Accessed July 8, 2016.
6. Pandit A, Sachdeva T, Bafna P. Drug-induced hepatotoxicity: a review. J Appl Pharm Sci. 2012;2:233-243.
7. O’Donnell JT, Marks DH, Danese P, O’Donnell JJ III. Drug-induced liver disease: primer for the primary care physician. Dis Mon. 2014;60:55-104.
8. Holt MP, Ju C. Mechanisms of drug-induced liver injury. AAPS J. 2006;8:e48-e54.
9. Yuan L, Kaplowitz N. Mechanisms of drug-induced injury. Clin Liver Dis. 2013;17:507-518.
10. LiverTox. Introduction. https://livertox.nih.gov/intro.html. Accessed July 24, 2016.
11. Guo JJ, Wigle PR, Lammers K, Vu O. Comparison of potentially hepatotoxic drugs among major US drug compendia. Res Social Adm Pharm. 2005;1:460-479.
12. Teschke R, Frenzel C, Wolff A, et al. Drug induced liver injury: accuracy of diagnosis in published reports. Ann Hepatol. 2014;13:248-255.
13. Agarwal VK, McHutchison JG, Hoofnagle JH, et al. Important elements for the diagnosis of drug-induced liver injury. Clin Gastroenterol Hepatol. 2010;8:463-470.
14. Björnsson ES, Hoofnagle JH. Categorization of drugs implicated in causing liver injury: critical assessment based on published case reports. Hepatology. 2016;63:590-603.
15. Chen M, Suzuki A, Thakkar S, et al. DILIrank: the largest reference drug list ranked by the risk for developing drug-induced liver injury in humans. Drug Discov Today. 2016;21:648-653.
16. Senior JR. Evolution of the Food and Drug Administration approach to liver safety assessment for new drugs: current status and challenges. Drug Saf. 2014;37(suppl 1):S9-S17.
17. Senior JR. Alanine aminotransferase: a clinical and regulatory tool for detecting liver injury—past, present, and future. Clin Pharmacol Ther. 2012;92:332-339.
18. Navarro VJ, Barnhart H, Bonkovsky HL, et al. Liver injury from herbals and dietary supplements in the U.S. Drug-Induced Liver Injury Network. Hepatology. 2014;60:1399-1408.
19. Seeff LB, Bonkovsky HL, Navarro VJ, Wang G. Herbal products and the liver: a review of adverse effects and mechanisms. Gastroenterology. 2015;148:517-532.
20. Teschke R, Frenzel C, Glass X, et al. Herbal hepatotoxicity: a critical review. Br J Clin Pharmacol. 2013;75:630-636.
21. Björnsson ES. Drug-induced liver injury: an overview over the most critical compounds. Arch Toxicol. 2015;89:327-334.
22. Chen M, Suzuki A, Borlak J, et al. Drug-induced liver injury: interactions between drug properties and host factors. J Hepatol. 2015;63:503-514.
23. Ortega-Alonso A, Stephens C, Lucena MI, Andrade RJ. Case characterization, clinical features and risk factors in drug-induced liver injury. Int J Mol Sci. 2016;17:e714.
24. Fromenty B. Drug-induced liver injury in obesity. J Hepatol. 2013;58:824-826.
25. Corsini A, Bortolini M. Drug-induced liver injury: the role of drug metabolism and transport. J Clin Pharmacol. 2013;53:463-474.
26. Fontana RJ. Pathogenesis of idiosyncratic drug-induced liver injury and clinical perspectives. Gastroenterology. 2014;146:914-928.
27. Chen M, Borlak J, Tong W. High lipophilicity and high daily dose of oral medications are associated with significant risk for drug-induced liver injury. Hepatology. 2013;58:388-396.
28. Chalasani N, Björnsson E. Risk factors for idiosyncratic drug-induced liver injury. Gastroenterology. 2010;138:2246-2259.
29. Aithal GP. Pharmacogenetic testing in idiosyncratic drug-induced liver injury: current role in clinical practice. Liver Int. 2015;35:1801-1808.
30. Russmann S, Jetter A, Kullak-Ublick GA. Pharmacogenetics of drug-induced liver injury. Hepatology. 2010;52:748-761.
31. Tarantino G, Di Minno MN, Capone D. Drug-induced liver injury: is it somehow forseeable? World J Gastroenterol. 2009;15:2817-2833.
32. Fisher K, Vuppalanchi R, Saxena R. Drug-induced liver injury. Arch Pathol Lab Med. 2015;139:876-887.
33. Ghabril M, Chalasani N, Björnsson E. Drug-induced liver injury: a clinical update. Curr Opin Gastroenterol. 2010;26:222-226.
34. Stine JG, Sateesh P, Lewis JH. Drug-induced liver injury in the elderly. Curr Gastroenterol Rep. 2013;15:299.
35. Au JS, Navarro VJ, Rossi S. Review article: drug-induced liver injury—its pathophysiology and evolving diagnostic tools. Aliment Pharmacol Ther. 2011;34:11-20.
36. Roy PK. Budd-Chiari syndrome. Medscape. http://emedicine.medscape.com/article/184430-overview. Accessed August 31, 2016.
37. Gilroy RK. Wilson disease. Medscape. http://emedicine.medscape.com/article/183456-overview. Accessed August 31, 2016.
38. Aithal GP, Watkins PB, Andrade RJ, et al. Case definition and phenotype standardization in drug-induced liver injury. Clin Pharmacol Ther. 2011;89:806-815.
39. Garcia-Cortes M, Stephens C, Lucena MI, et al; Spanish Group for the Study of Drug-Induced Liver Disease. Causality assessment methods in drug induced liver injury: strengths and weaknesses. J Hepatol. 2011;55:683-691.
40. Danan G, Benichou C. Causality assessment of adverse reactions to drugs—I. A novel method based on the conclusions of international consensus meetings: application of drug-induced liver injuries. J Clin Epidemiol. 1993;46:1323-1330.
41. Benichou C, Danan G, Flahault A. Causality assessment of adverse reactions to drugs—II. An original model for validation of drug causality assessment methods: case reports with positive rechallenge. J Clin Epidemiol. 1993;46:1331-1336.
42. Maria VA, Victorino RM. Development and validation of a clinical scale for the diagnosis of drug-induced hepatitis. Hepatology. 1997;26:664-669.
43. Teschke R, Frenzel C, Schulze J, Eickhoff A. Herbal hepatotoxicity: challenges and pitfalls of causality assessment methods. World J Gastroenterol. 2013;19:2864-2882.
44. LiverTox. Causality. https://livertox.nih.gov/Causality.html. Accessed July 24, 2016.
45. Czaja AJ. Review article: the management of autoimmune hepatitis beyond consensus guidelines. Aliment Pharmacol Ther. 2013;38:343-364.
46. Mitchell SJ, Hilmer SN. Drug-induced liver injury in older adults. Ther Adv Drug Saf. 2010;1:65-77.
47. Sales I, Dzierba AL, Smithburger PL, et al. Use of acetylcysteine for non-acetaminophen-induced acute liver failure. Ann Hepatol. 2013;12:6-10.
48. Chughlay MF, Kramer N, Werfalli M, et al. N-acetylcysteine for non-paracetamol drug-induced liver injury: a systematic review protocol. Syst Rev. 2015;4:84.
49. Leise MD, Poterucha JJ, Talwakar JA. Drug-induced liver injury. Mayo Clin Proc. 2014;89:95-106.
50. Singh D, Cho WC, Upadhyay G. Drug-induced liver toxicity and prevention by herbal antioxidants: an overview. Front Physiol. 2016;6:363.
51. Khoury T, Rmeileh AA, Yosha L, et al. Drug induced liver injury: review with a focus on genetic factors, tissue diagnosis, and treatment options. J Clin Transl Hepatol. 2015;3:99-108.
52. Zimmerman HJ. The spectrum of hepatotoxicity. Perspect Biol Med. 1968;12:135-161.
53. Temple R. Hy’s law: predicting serious hepatotoxicity. Pharmacoepidemiol Drug Saf. 2006;15:241-243.
54. Robles-Diaz M, Lucena MI, Kaplowitz N, et al; Spanish DILI Registry; SLatinDILI Network; Safer and Faster Evidence-based Translation Consortium. Use of Hy’s Law and a new composite algorithm to predict acute liver failure in patients with drug-induced liver injury. Gastroenterology. 2014;147:109-118.
55. Maddur H, Chalasani N. Idiosyncratic drug-induced liver injury: a clinical update. Curr Gastroenterol Rep. 2011;13:65-71.
56. FDA. Guidance for industry: drug-induced liver injury: premarketing clinical evaluation. www.fda.gov/downloads/Drugs/GuidanceComplianceRegulatoryInformation/Guidances/UCM174090.pdf. Accessed July 24, 2016.
57. Lee WM. Drug-induced acute liver failure. Clin Liver Dis. 2013;17:575-586.
58. Wang YM, Chai SC, Brewer CT, Chen T. Pregnane X receptor and drug-induced liver injury. Exp Opin Drug Metab Toxicol. 2014;10:1521-1532.
59. Stine JG, Chalasani N. Chronic liver injury induced by drugs: a systematic review. Liver Int. 2015;35:2343-2353.
60. Andrade RJ, Lucena MI, Kaplowitz N, et al. Outcome of acute idiosyncratic drug-induced liver injury: long-term follow-up in a hepatotoxicity registry. Hepatology. 2006;44:1581-1588.
To comment on this article, contact rdavidson@uspharmacist.com.





