US Pharm. 2017;42(1):29-32.
ABSTRACT: Insomnia is a disorder due to inadequate sleep quantity and/or quality caused by impaired sleep initiation, maintenance, or duration. Understanding potential nonpharmacologic and pharmacotherapeutic treatment options for insomnia is a vitally important role for pharmacists. Many practitioners and patients are avoiding benzodiazepine receptor agonists (BZDRAs) due to their significant adverse-effect profiles, so pharmacists should understand the appropriate utility of the five FDA-approved non-BZDRA options. Diphenhydramine and doxylamine are generally not recommended due to efficacy and safety concerns, while doxepin, ramelteon, and suvorexant all appear to be efficacious options in the management of insomnia.
Insomnia, the most common sleep-wake disorder, is generally defined as a lack of sleep due to insufficient sleep quality or quantity. It can be characterized by difficulty initiating sleep (also known as sleep latency), difficulty maintaining sleep, or inappropriate duration of sleep.1 The natural history of insomnia often changes with time; some patients initially have difficulty initiating sleep but later have difficulty maintaining sleep, or vice versa.2 Inadequate sleep is often accompanied by impaired daytime functioning, which can lead to performance difficulties at work and/or school.3
Insomnia is commonly characterized as a disorder of nocturnal hyperarousal. This hyperarousal is a consequence of activation of the neuroendocrine system’s stress response.4 High levels of cortisol and adrenocorticotropic hormones have been recorded in those with insomnia. Dysregulation of corticotropin-releasing factor also plays a role, and increased blood pressure, body temperature, heart rate, metabolic rate, and high-frequency electroencephalographic (EEG) activity during sleep may be present in insomniacs as well.5
The American Psychiatric Association’s Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition ( DSM-5) criteria for a diagnosis of insomnia specify that symptoms must cause clinically significant functional distress or impairment and be present for at least 3 nights per week for at least 3 months. In addition, this must occur despite an adequate opportunity for appropriate sleep and cannot be explained via another sleep-related disorder.1
Epidemiology
Several comorbid medical conditions may contribute to insomnia such as obstructive sleep apnea (OSA), fibromyalgia, and chronic pain. Treatment of these underlying conditions may or may not resolve insomnia. Of these concomitant disease states, insomnia is most strongly associated with neuropsychiatric illness, including mood disorders, posttraumatic stress disorder (PTSD), and anxiety. Additionally, insomnia is a strong predictor of relapsing depression and substance abuse. Smoking may lead to shortened sleep duration (<6 hours), while chronic alcohol consumption will most likely increase sleep disruption and ultimately have a negative effect on sleep initiation.6
Numerous epidemiologic studies have been conducted to determine the prevalence of insomnia with worldwide rates varying from 5% to 50%.7 This variation may be due to different definitions being used for insomnia or various methods being used for assessing insomnia.7 In population-based studies, about one-third of adults report at least one nocturnal insomnia symptom weekly.8 When using the DSM-5 diagnostic criteria, insomnia prevalence rates from multiple countries have consistently been between 6% and 10%.1,9 Insomnia is found to be more prevalent among women, older adults, shift workers, and those with aforementioned comorbid medical and/or psychiatric disorders.7,9
Nonpharmacologic Treatment
The management of insomnia is dependent on a number of variables, including classification of insomnia, comorbid conditions, and patient-specific factors. Appropriate treatment of coexisting medical, psychiatric, or other sleep disorders is essential for the proper management of insomnia.2 It is also recommended that treatment of insomnia include at least one behavioral intervention.10 Potential components of nonpharmacologic therapy for insomnia include proper sleep hygiene, stimulus control, sleep restriction, relaxation training, and/or cognitive-behavioral therapy (CBT).11
One hallmark of insomnia treatment is CBT. This approach uses a combination of cognitive therapy, stimulus control, and sleep restriction therapy with or without relaxation therapy. Various trials have shown that CBT has a significant effect on the short- and long-term treatment of chronic insomnia, especially in patients with a psychiatric or medical comorbidity.6 In two separate trials, cognitive behavioral therapy was shown to sustain patients’ sleep improvements at 12 and 24 months when compared to pharmacotherapy alone.12,13
During a CBT session, patients are educated about good sleep practices, how to complete a sleep diary, and dysfunctional beliefs and misconceptions about insomnia. Patients are also taught principles of stimulus control and sleep restriction. Stimulus control teaches patients to eliminate distractions and associate the bedroom only with sleep and sex. It also involves going to bed only when tired and leaving the room if not asleep within 15 to 20 minutes. Patients are asked to estimate their total time asleep by using diaries, and to restrict their time in bed to the average necessary sleep time. Time in bed must not be <5 hours, and morning wake time should be consistent throughout treatment.10,11
FDA-Approved Pharmacotherapy
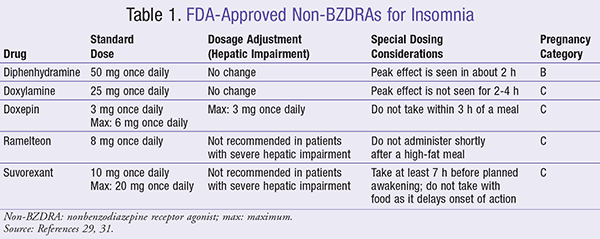
Treatment goals of insomnia should center on improving sleep quality and quantity and minimizing insomnia-related impairments.14 Knowledge of potential pharmacotherapeutic options is pertinent for every pharmacist. Previous guidelines mentioned benzodiazepine receptor agonists (BZDRAs; i.e., temazepam, zolpidem, eszopiclone, zaleplon) as potential first-line options for the management of insomnia.14 However, other guidelines suggest only short-term use of these agents on a case-by-case basis due to their significant adverse-effect profiles.15 BZDRAs are controlled substances and can lead to significant adverse effects that include but are not limited to cognitive impairment, falls/fractures, delirium/dementia, anterograde amnesia, altered sleep activities (e.g., sleep-eating, sleep-driving, sleep-walking), and carryover sedation.2,11,15 Because of these concerns, many clinicians and patients prefer options that work outside the BZDRA mechanism of action. The following is a review of agents that work via non-BZDRA mechanisms and are FDA-approved for the management of insomnia. Dosing recommendations for each agent are contained in TABLE 1.
Diphenhydramine and Doxylamine: It is estimated that >60% of pharmacotherapy for insomnia is via nonpre-scription medications.2 Diphenhydramine (e.g., Sominex) and doxylamine (e.g., Unisom SleepTabs) are first-generation antihistamines that work via competition with histamine at H1 receptors as inverse agonists. They exert their mechanism centrally, which leads to drowsiness and their potential effectiveness in the management of insomnia. Both OTC agents have carried historical FDA approval as safe and effective options for the management of insomnia for over 25 years, but their utility in this patient population is still controversial due to a dearth of large, well-designed trials.11,16 Additionally, rapid tolerance to their sedative effects renders them ineffective for chronic use. Small studies of diphenhydramine have suggested significant improvements in overall sleep time, efficacy, latency, and nighttime awakenings, while others contradict these findings.17-20
Contrary to diphenhydramine, doxylamine lacks even small studies directly confirming its efficacy in the management of insomnia. From an adverse-effect stand-point, these agents can cause confusion, carryover sedation, urinary retention, and multiple other anticholinergic effects due to muscarinic receptor antagonism.21 These effects are particularly concerning in the elderly, and the 2015 Beers criteria update gave a “strong” recommendation to avoid both agents in elderly patients.22 Additionally, patients with glaucoma, thyroid disorders, chronic respiratory diseases, cardiovascular disease, benign prostatic hyperplasia (BPH), or significant urinary retention should use these agents cautiously or completely avoid their use. Due to the relative lack of efficacy data and significant adverse-effect profiles, diphenhydramine and doxylamine are not currently recommended as routine options in the management of insomnia.14,15,21
Doxepin: Doxepin (Silenor) is a tricyclic antidepressant with central H1-receptor antagonism that produces a sedative effect. While it has been utilized as an antidepressant for over 50 years, it only gained FDA approval for the treatment of insomnia in 2010.23 The ability to use low doses (≤6 mg) for insomnia is derived from its high selectivity for histamine receptors.21 Multiple studies evaluating doxepin’s safety and efficacy in the management of insomnia have summarized that doxepin significantly improves Insomnia Severity Index (ISI) scores and also improves sleep duration, maintenance, and efficiency when compared to placebo.11,21,23,24
Regarding adverse effects, somnolence was the most commonly noted, with dizziness, nausea, upper respiratory tract infections, nasopharyngitis, hypertension, and head-ache all also being documented.23,24 Additionally, doxepin is contraindicated in patients with glaucoma or severe urinary retention and should be used cautiously in patients with concomitant depression, cardiovascular disease, diabetes, seizures, chronic respiratory disease, or OSA. Of particular note is that anticholinergic effects are not seen frequently with ≤6 mg of doxepin, which provides a treatment benefit when compared to diphenhydramine, doxylamine, or the significantly higher doses of doxepin used to treat depression.15,21,22 Doxepin could potentially cause a decrease in next-day psychomotor function, although a meta-analysis suggested no significant difference when compared to placebo.23,24 Of note, neither rebound insomnia nor withdrawal symptoms seem to be of concern upon discontinuation of doxepin.23 In summary, doxepin appears to be a safe and effective option for the management of insomnia at low doses.11,15
Ramelteon: Ramelteon (Rozerem) is a melatonin receptor agonist (MT1 and MT2) that gained FDA approval for the treatment of insomnia in 2005.25 Ramelteon’s activity at the MT1 receptor is thought to induce sleep, while its activity at the MT2 receptor is thought to influence the circadian rhythm. It is significantly more selective for these receptors when compared to melatonin itself. Clinical trials have primarily supported ramelteon’s efficacy in improving sleep latency. Additional benefits on sleep quality, efficiency, and duration have been noted but are relatively minor when compared to placebo and may not carry clinical relevance.26
Ramelteon’s adverse-effect profile includes somnolence, dizziness, nausea, myalgias, and upper respiratory tract infections. Interestingly, some patients (roughly 3%) reported a worsening of insomnia symptoms when using ramelteon. Other concomitant disease states that may be of concern are OSA, chronic obstructive pulmonary disease (COPD), severe hepatic impairment, and depression. Ramelteon does not appear to have any abuse potential and has a limited ability to cause carryover sedation, rebound insomnia, or withdrawal upon discontinuation. In summary, ramelteon appears to be a safe and effective option for the management of insomnia caused by difficulty falling asleep.11,14,15
Suvorexant: Suvorexant (Belsomra) is a schedule IV con-trolled substance and is the most recently FDA-approved agent for the management of insomnia, having garnered approval in 2014.27 It works through inhibition of the binding of orexin-A and -B to the orexin receptors (OX1R and OX2R). Orexins are thought to be wake-promoting neurotransmitters, so that by blocking OX1R and OX2R, suvorexant essentially “turns off” wakefulness. Clinical trial data have summarized that suvorexant significantly improves sleep latency, sleep maintenance, sleep duration, and ISI scores when compared to placebo.11,28
Somnolence/excessive daytime sleepiness was the most commonly noted adverse effect (and was dose-dependent), with abnormal dreams and dry mouth also being documented more frequently than placebo.27 Interestingly, most adverse effects appear more commonly in females (particularly obese females) due to higher drug exposure in this population. Suvorexant is contraindicated in patients with narcolepsy due to its unique ability to “turn off” wakefulness.27
Similar to ramelteon, concomitant OSA, COPD, or depression may be of concern when using suvorexant. Additionally, certain trials have suggested that suvorexant may cause impaired driving performance or balance deficits the morning after use.27 However, no difference in rebound insomnia rates or withdrawal symptoms has been seen when compared to placebo.28 In summary, clinical trial data support suvorexant as a safe and effective option for the management of insomnia.28
Other Therapies: Guidelines have also discussed other pharmacotherapeutic options that may have utility in the treatment of insomnia. Mirtazapine and trazodone may be beneficial in certain patient populations, particularly those with concomitant depression or unintentional weight loss.14,15,21 Trazodone has little to no anticholinergic activity but may cause excessive daytime sleepiness and psychomotor impairment, while mirtazapine can lead to anticholinergic adverse effects and significant weight gain.2,15,21,29 Because these medications do not have quality clinical trial data backing their efficacy and are not FDA-approved for the management of insomnia, they are not currently recommended for that purpose and should only be considered in patients who have concomitant diseases that may also benefit from their usage.
Summary
In summary, insomnia affects many patients worldwide. Nonpharmacologic treatment is considered first-line management of insomnia. Due to significant adverse-effect profiles, the BZDRAs may not be appropriate options for the management of insomnia in many patients. The non-BZDRAs doxepin, ramelteon, and suvorexant have scenarios where each may be the most appropriate selection and should currently be considered first-line pharmacotherapeutic options. Follow-up evaluation should take place within 3 weeks of therapy initiation to evaluate efficacy and safety of the agent selected.30
REFERENCES
1. American Psychiatric Association. Sleep-wake disorders. Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5). Arlington, VA: American Psychiatric Publishing; 2013.
2. Winkelman JW. Insomnia disorder. N Engl J Med. 2015;373:1437-1444.
3. Roth T, Jaeger S, Jin R, et al. Sleep problems, comorbid disorders, and role functioning in the National Comorbidity Survey Replication (NCSR). Biol Psychiatry. 2006;60(12):1364-1371.
4. Basta M, Chrousos GP, Vela-Bueno A, et al. Chronic insomnia and stress system. Sleep Med Clin. 2007;2(2):279-291.
5. Bonnet MH, Arand DL. Hyperarousal and insomnia: state of the science. Sleep Med Rev. 2010;14:9-15.
6. Hofmann G, Asnaani A, Vonk I, et al. The efficacy of cognitive behavioural therapy: a review of meta-analyses. Cognit Ther Res. 2012;36(5):427-440.
7. Ohayon MM. Epidemiology of insomnia: what we know and what we still need to learn. Sleep Med Rev. 2002;6(2):97-111.
8. Sivertsen A, Kokstad S, Øverland S, et al. The epidemiology of insomnia: associations with physical and mental health. The HUNT-2 study. J Psychosom Res. 2009;67:109-116.
9. Morin CM, Jarrin DC. Epidemiology of insomnia. Prevalence, course, risk factors, and public health burden. Sleep Med Clin. 2013;8:281-297.
10. Maness DL, Khan M. Nonpharmacologic management of chronic insomnia. Am Fam Physician. 2015;92(12):1058-1064.
11. Qaseem A, Kansagara D, Forciea MA, et al. Management of chronic insomnia disorder in adults: a clinical practice guideline from the American College of Physicians. Ann Intern Med. 2016;165:125-133.
12. Morin CM, Colecchi C, Stone J, et al. Behavioral and pharmacological therapies for late-life insomnia: a randomized controlled trial. JAMA. 1999;281(11):991-999.
13. Sivertsen B, Omvik S, Pallesen S, et al. Cognitive behavioral therapy vs zopiclone for treatment of chronic primary insomnia in older adults: a randomized controlled trial. JAMA. 2006;295(24):2851-2858.
14. Schutte-Rodin S, Broch L, Buysse D, et al. Clinical guideline for the evaluation and management of chronic insomnia in adults. J Clin Sleep Med. 2008;4:487-504.
15. Baker S, Bhatta S, Bowden E, et al; National Guideline Clearinghouse. Clinical guideline for the treatment of primary insomnia in middle-aged and older adults. Guideline summary NGC-10414. Rockville, MD: Agency for Healthcare Research and Quality; May 2014.
16. Labeling of diphenhydramine-containing drug products for over-the-counter human use. Final rule. Fed Regist. 2002;67:72555-72559.
17. Morin CM, Koetter U, Bastien C, et al. Valerian-hops combination and diphenhydramine for treating insomnia: a randomized placebo-controlled clinical trial. Sleep. 2005;28:1465-1471.
18. Glass JR, Sproule BA, Herrmann N, et al. Effects of 2-week treatment with temazepam and diphenhydramine in elderly insomniacs: a randomized, placebo-controlled trial. J Clin Psychopharmacol. 2008;28:182-188.
19. Rickels K, Morris RJ, Newman H, et al. Diphenhydramine in insomniac family practice patients: a double-blind study. J Clin Pharmacol. 1983;23:234-242.
20. Meuleman JR, Nelson RC, Clark RL Jr. Evaluation of temazepam and diphen-hydramine as hypnotics in a nursing-home population. Drug Intell Clin Pharm. 1987;21:716-720.
21. Vande Griend JP, Anderson SL. Histamine-1 receptor antagonism for treatment of insomnia. J Am Pharm Assoc. 2012;52:e210-e219.
22. American Geriatrics Society 2015 Beers Criteria Update Expert Panel. American Geriatrics Society 2015 updated Beers criteria for potentially inappropriate medication use in older adults. J Am Geriatr Soc. 2015;63:2227-2246.
23. Silenor (doxepin) package insert. Morristown, NJ: Pernix Therapeutics, LLC; 2010.
24. Yeung WF, Chung KF, Yung KP, et al. Doxepin for insomnia: a systematic review of randomized placebo-controlled trials. Sleep Med Rev. 2015;19:75-83.
25. Rozerem (ramelteon) package insert. Deerfield, IL: Takeda Pharmaceuticals America, Inc; 2005.
26. Kuriyama A, Honda M, Hayashino Y. Ramelteon for the treatment of insomnia in adults: a systematic review and meta-analysis. Sleep Med. 2014;15:385-392.
27. Belsomra (suvorexant) package insert. Whitehouse Station, NJ: Merck & Co, Inc; 2014.
28. Kishi T, Matsunaga S, Iwata N. Suvorexant for primary insomnia: a systematic review and meta-analysis of randomized placebo-controlled trials. PLoS One. 2015;28:e0136910.
29. Lie JD, Tu KN, Shen DD, et al. Pharmacological treatment of insomnia. P T. 2015;40(11):759-771.
30. Dopp JM, Phillips BG. Chapter 41: Sleep disorders. In: Chisholm-Burns MA, Schwinghammer TL, Wells BG, et al, eds. Pharmacotherapy Principles & Practice. 4th ed. New York, NY: McGraw-Hill Education; 2016.
31. Lexi-Drugs Online. Hudson, OH: Lexi-Comp, Inc. https://online.lexi.com. Accessed September 19, 2016.
To comment on this article, contact rdavidson@uspharmacist.com.





