US Pharm. 2013;38(6):51-54.
ABSTRACT: Superficial fungal infections commonly affect the hands and feet. While various dermatophytes can lead to infection, Epidermophyton, Microsporum, and Trichophyton tend to cause the majority of infections. Tinea pedis, tinea unguium, and tinea manuum are common superficial fungal infections. Topical and oral antifungal agents, which are the mainstay of therapy, often need to be used for 1 week to 4 months, depending upon the type and severity of the infection. Pharmacists play an important role in educating patients about the proper treatment of, and prevention strategies for, superficial fungal infections.
Superficial fungal infections are caused by dermatophytes (pathogenic fungi on the skin), which can infect the skin, hair, and nails. Dermatophytes thrive on moist areas of the skin and may also be found on clothing and towels and in the soil. About 20% to 25% of the world population is infected with a dermatophyte.1 While various dermatophytes exist, three are known to cause the majority of fungal infections in humans: Epidermophyton, Microsporum, and Trichophyton.1
Two areas of the body commonly exposed to these pathogens are the hands and the feet. Tinea pedis (athlete’s foot) has a lifetime prevalence of approximately 70% and is often accompanied by tinea manuum (hands), tinea unguium (nails), or tinea cruris (groin).2 While tinea pedis, tinea manuum, and tinea cruris can be successfully treated with OTC medications, tinea unguium typically requires prescription medications. This article will focus on the clinical features of fungal infections of the hands and feet, along with potential preventive and treatment strategies.
TINEA PEDIS
Epidermophyton floccosum, Trichophyton mentagrophytes, and Trichophyton rubrum are common causes of tinea pedis. Although contact with infected people, animals, or fomites (inanimate objects capable of harboring infectious agents) are obvious sources of fungal transmission, several other factors promote the growth of tinea pedis: living in a warm or moist climate, occlusive footwear, excessive sweating, community showers or swimming pools, poor foot hygiene, and health conditions or medications that suppress the immune system.2
Tinea pedis generally affects the superficial layer of the skin and is often found between the toes, although it can infect the sides and soles of the feet as well. Tinea pedis may be categorized as chronic interdigital, moccasin, vesicular, or acute ulcerative. Chronic interdigital tinea pedis presents as macerations or fissures in the toe webs, with symptoms including malodor, pruritus, and burning of the feet. Moccasin tinea pedis is characterized by diffuse scaling plaques on the soles and sides of the feet and may be accompanied by mild inflammation and erythema. Vesicular tinea pedis presents as small vesicles between the toes or on the soles of the feet and tends to worsen in the summer. The presence of severe inflammation, skin discoloration, macerations, and/or weeping ulcerations may indicate acute ulcerative tinea pedis, which can be debilitating and lead to bacterial superinfections if not treated appropriately.2-5
With all four types, the risk of developing other superficial fungal infections (such as tinea unguium) increases if the condition is not properly treated. Beyond foot examination, diagnosis should be confirmed by a potassium hydroxide (KOH) preparation used to visualize the scales under a microscope, or (less commonly), by a fungal culture.3,4
Treatment Strategies
The goals of tinea pedis therapy include symptom relief, fungus eradication, and prevention of future infections. Topical antifungals, which are considered first-line treatment for fungal skin infections of the foot, are readily available as nonprescription products. Most of these agents are applied once or twice daily, with a treatment duration of 1 to 4 weeks.6 For more severe cases or if topical therapy has failed, oral prescription therapy may be employed. See TABLES 1 and 2 for a summary of products commonly used to treat tinea pedis.
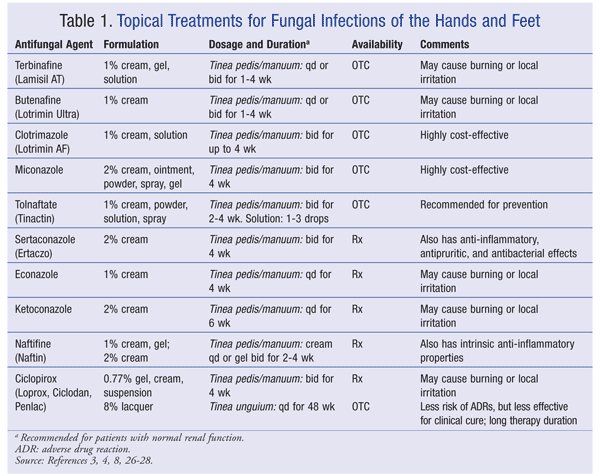
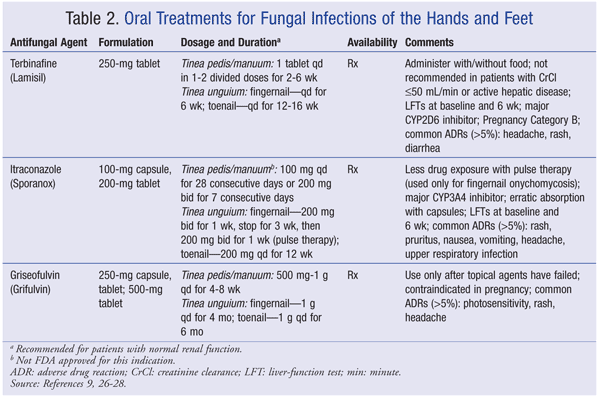
A literature review reveals strong evidence that topical terbinafine (an allylamine) and butenafine (an allylamine derivative) produce high cure rates.7 These agents are considered fungicides, since each inhibits squalene epoxidase, the enzyme responsible for synthesizing the fungal cell membrane. The topical azole antifungals clotrimazole and miconazole hinder fungal cell wall synthesis by blocking the formation of ergosterol. For the most part, these agents are fungistatic and, as a result, may be less effective than the allylamines.6,7 However, azole therapy cure rates increase with a longer treatment duration. In fact, azole treatment for 4 weeks has similar outcomes to allylamine therapy for 1 week.7,8 After an appropriate treatment duration, topical azoles and allylamines reach cure rates of about 72% and 80%, respectively.9
Prescription topical therapies include sertaconazole, econazole, ketoconazole, naftifine, and ciclopirox. As noted, systemic therapy may be needed for severe cases or if topical therapy has failed. Prescription oral terbinafine, itraconazole, and fluconazole have demonstrated efficacy for tinea pedis.3,10,11 Fluconazole, however, is not FDA approved for any type of tinea infection. Another oral agent that may be used to treat tinea pedis is griseofulvin.10 Nevertheless, terbinafine is more effective than griseofulvin, and the efficacies of terbinafine and itraconazole are comparable.12
Although self-treatment of tinea pedis is generally well tolerated and safe for most patients, patients with a history of diabetes, immunodeficiency, or signs of systemic infection should be referred to their primary care physician. It is important to note that tinea pedis presenting with inflammation or as the wet, soggy type may require the use of an astringent solution (e.g., Burow’s solution) prior to initiation of antifungal therapy.2 Burow’s solution may be applied to the affected area for 20 minutes two to three times daily, or as recommended. Although antifungal creams and solutions are better treatment options since they are rubbed directly into the skin, sprays and powders may be better formulations for prevention.2
Preventive Strategies
Preventive strategies may prove beneficial, especially since up to 70% of patients experience recurrences.13 Several nonpharmacologic strategies may be used to help prevent initial or recurring fungal foot infections. Because dermatophytes prefer a warm, moist environment, it is important to keep the feet cool and dry. Approaches include changing the socks more frequently, wearing cotton or wool socks, and using nonocclusive footwear (e.g., such as sandals) whenever possible. Because tinea pedis is transmittable from person to person, contact with infected individuals should be avoided, and protective footwear should be worn in public showers. The skin should be washed with soap and water on a daily basis and dried thoroughly.2 The feet should be dried last, or a separate towel should be used for the feet. Any potentially infected clothing should be washed in hot water. Another prevention strategy is to sprinkle nonmedicated powder inside the shoes to limit moisture.5 Currently, the only FDA-approved active ingredient for tinea pedis prevention is tolnaftate. Available as a cream, powder, solution, or spray, tolnaftate should be applied once or twice daily.2
TINEA UNGUIUM
Tinea unguium, often referred to as onychomycosis, is an infection of nail tissue of the hands or the feet. T rubrum and Trichophyton interdigitale are the common dermatophytes known to cause tinea unguium. Nondermatophytes account for the remainder of infections, notably yeasts from Candida species, as well as molds from Fusarium and Acremonium species.14 Risk factors for onychomycosis include older age, swimming, trauma to the nail, diabetes, immunosuppression, living with someone with onychomycosis, and tinea pedis.15
There are three forms of onychomycosis: distal subungual, superficial white, and proximal subungual. Distal subungual onychomycosis is the most common form, with the big toe usually the first nail to be affected. This form involves the end third of the nail farthest away from the cuticle and begins with a whitish, yellowish, or brownish discoloration of the nail. The discoloration eventually spreads to the entire nail and extends slowly to the cuticle. The discoloration is due in part to keratinous debris between the nail and the nail bed. A patient may present initially with hyperkeratosis of the nail bed, which may lead to onycholysis (separation of the nail from underlying tissue). Onycholysis causes pain, which may prevent the patient from being able to perform typical activities of daily living. Superficial white onychomycosis infects the entire top surface of the nail and has a flaky appearance. Proximal subungual onychomycosis, which is relatively rare, occurs mostly in immunocompromised patients; it presents with a seemingly deeper infection that occurs under the nail near the cuticle and extends distally.16 Unless treated properly, onychomycosis persists indefinitely.
Treatment Strategies
It is important to recognize the presence of fungus before antifungal therapy is initiated. A variety of presentations exist that could lead to a differential diagnosis, including psoriasis, iron deficiency, eczematous conditions, trauma, yellow nail syndrome, periungual squamous cell carcinoma, and lichen planus. Studies have indicated that onychomycosis is responsible for only 50% to 60% of abnormal-appearing nails.17 The examiner must take into account the number of affected nails, as well as symmetry, pain, and other nail characteristics.16 Onychomycosis is most readily confirmed using a KOH preparation for histologic examination.18 Treatment should be initiated upon confirmation.
Topical and systemic therapies for onychomycosis exist; however, studies indicate that systemic therapies are more effective.10 Topical antifungal creams do not adequately penetrate the nail bed and are not considered appropriate. However, an antifungal topical in the form of a nail lacquer (e.g., ciclopirox) is an option, especially in patients in whom oral therapy is contraindicated. The combination of oral terbinafine and topical ciclopirox has not been shown to provide greater efficacy.19,20 Evidence supports the use of oral terbinafine or itraconazole for 6 to 8 weeks for fingernail onychomycosis. Toenail onychomycosis requires a longer duration of therapy (12-16 weeks for terbinafine, or continuous daily dosing with itraconazole for 12 weeks).16 In patients with onychomycosis, fluconazole 150 mg to 300 mg once weekly has been effective, but less effective than terbinafine or itraconazole.21 Griseofulvin, another treatment option, has been associated with lower clinical cure rates—as well as with recurrence—compared with terbinafine.22 TABLES 1 and 2 include a summary of available treatment options for onychomycosis.
Prevention Strategies
Patients with onychomycosis should be educated about proper hygiene and lifestyle modifications in order to prevent relapse and recurrence. Patients should be encouraged to adequately trim the toenails directly across the toe with minimal curvature, as well as to avoid walking barefoot in damp areas.23 The feet should be kept clean and dry, and an emollient may be applied to areas of compromised dry skin where a fungal infection may be more probable. Adequate footwear that minimizes humidity should be worn, and should later be discarded upon significant wear and tear.16,23
TINEA MANUUM
Tinea manuum, sometimes referred to as two feet–one hand syndrome, is similar to moccasin tinea pedis and often develops after the occurrence of tinea pedis or tinea unguium.24,25 The same fungal species that cause tinea pedis and tinea unguium also can result in tinea manuum.25 Typically, the hand used to scratch the foot with the rash is affected. The palm appears hyperkeratotic, with a fine white scale emphasizing the normal lines of the hand. The dorsal surface of the hand may exhibit a classic ringworm appearance. Tinea manuum may mimic eczema, contact dermatitis, palmar psoriasis, or dryness of the hand. Overall, tinea manuum occurs less frequently than either tinea pedis or tinea unguium. Preventive and treatment strategies, which are the same as for tinea pedis, are summarized in TABLES 1 and 2.25
CONCLUSION
Superficial fungal infections of the hands and feet are manageable conditions with a favorable prognosis when treated appropriately. Topical and oral antifungals continue to be the mainstay of therapy and often need to be used for 1 week to 4 months, depending upon the type and severity of fungal infection. It is important to counsel the patient regarding the potential for recurrence despite adequate adherence and symptom resolution. Prevention strategies should be encouraged in order to minimize the risk of future infections.
REFERENCES
1. Havlickova B, Czaika VA, Friedrich M. Epidemiological trends in skin mycoses worldwide. Mycoses. 2008;51(suppl 4):2-15.
2. Newton GD, Popovich NG. Fungal skin infections. In: Krinsky DL, Berardi RR, Ferreri SP, et al, eds. Handbook of Nonprescription Drugs: An Interactive Approach to Self-Care. 17th ed. Washington DC: American Pharmacists Association; 2012.
3. Weinberg JM, Koestenblatt EK. Treatment of interdigital tinea pedis: once-daily therapy with sertaconazole nitrate. J Drugs Dermatol. 2011;10:1135-1140.
4. Weinstein A, Berman B. Topical treatment of common superficial tinea infections. Am Fam Physician. 2002;65:2095-2102.
5. Grin C. Tinea: diagnostic clues, treatment keys. Consultant. 2004;44:214-216.
6. Kiencke P, Korting HC, Nelles S, Rychlik R. Comparable efficacy
and safety of various topical formulations of terbinafine in tinea pedis
irrespective of the treatment regimen: results of a meta-analysis. Am J Clin Dermatol. 2007;8:357-364.
7. Crawford F, Hollis S. Topical treatments for fungal infections of the skin and nails of the foot. Cochrane Database Syst Rev. 2007;(3):CD001434.
8. Hart R, Bell-Syer SE, Crawford F, et al. Systematic review of
topical treatments for fungal infections of the skin and nails of the
feet. BMJ. 1999;319:79-82.
9. Markova T. What is the most effective treatment for tinea pedis (athlete’s foot)? J Fam Pract. 2002;51:21.
10. Gupta AK, Cooper EA. Update in antifungal therapy of dermatophytosis. Mycopathologia. 2008;166:353-367.
11. Gupta AK, Doncker PD, Heremans A, et al. Itraconazole for the
treatment of tinea pedis: a dosage of 400 mg/day given for 1 week is
similar in efficacy to 100 or 200 mg/day given for 2 to 4 weeks. J Am Acad Dermatol. 1997;36(5 Pt 1):789-792.
12. Bell-Syer SE, Khan SM, Torgerson DJ. Oral treatments for fungal infections of the skin of the foot. Cochrane Database Syst Rev. 2012;(10):CD003584.
13. Brown TE, Chin TW. Superficial fungal infections. In: DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 7th ed. New York, NY: McGraw-Hill Medical; 2008:1957-1972.
14. Ghannoum MA, Hajjeh RA, Scher R, et al. A large-scale North
American study of fungal isolates from nails: the frequency of
onychomycosis, fungal distribution, and antifungal susceptibility
patterns. J Am Acad Dermatol. 2000;34:641-648.
15. Sigurgeirsson B, Steingrímsson O. Risk factors associated with onychomycosis. J Eur Acad Dermatol Venereol. 2004;18:48-51.
16. deBerker D. Fungal nail disease. N Engl J Med. 2009;360:2108-2116.
17. Gupta AK, Jain HC, Lynde CW, et al. Prevalence and epidemiology
of onychomycosis in patients visiting physicians’ offices: a multicenter
Canadian survey of 15,000 patients. J Am Acad Dermatol. 2000;43(2 Pt 1):244-248.
18. Drake LA, Dinehart SM, Farmer ER, et al. Guidelines of care for superficial mycotic infections of the skin: onychomycosis. J Am Acad Dermatol. 1996;34:116-121.
19. Gupta AK; Onychomycosis Combination Therapy Study Group.
Ciclopirox topical solution, 8% combined with oral terbinafine to treat
onychomycosis: a randomized, evaluator-blinded study. J Drugs Dermatol. 2005;4:481-485.
20. Avner S, Nir N, Henri T. Combination of oral terbinafine and
topical ciclopirox compared to oral terbinafine for the treatment of
onychomycosis. J Dermatolog Treat. 2005;16:327-330.
21. Havu V, Heikkilä H, Kuokkanen K, et al. A double-blind,
randomized study to compare the efficacy and safety of terbinafine
(Lamisil) with fluconazole (Diflucan) in the treatment of onychomycosis.
Br J Dermatol. 2000;142:97-102.
22. Hofmann H, Bräutigam M, Weidinger G, Zaun H. Treatment of toenail
onychomycosis. A randomized, double-blind study with terbinafine and
griseofulvin. Arch Dermatol. 1995;131:919-922.
23. Tosti A, Hay R, Arenas-Guzmán R. Patients at risk of onychomycosis—risk factor identification and active prevention. J Eur Acad Dermatol Venereol. 2005;19(suppl 1):13-16.
24. Daniel CR III, Gupta AK, Daniel MP, Daniel CM. Two feet-one hand syndrome: a retrospective multicenter survey. Int J Dermatol. 1997;36:658-660.
25. Noble SL, Forbes RC, Stamm PL. Diagnosis and management of common tinea infections. Am Fam Physician. 1998;58:163-74,177-178.
26. Clinical Pharmacology. www.clinicalpharmacology.com. Accessed May 9, 2013.
27. Micromedex Healthcare Series 2.0. Truven Health Analytics. www.micromedexsolutions.com/home/dispatch. Accessed May 9, 2013.
28. Lexicomp Online. https://online.lexi.com/lco/action/home. Accessed May 9, 2013.
To comment on this article, contact rdavidson@uspharmacist.com.





