US Pharm. 2012;37(12):36-39.
ABSTRACT: Prescriptions for opioid analgesics have been steadily increasing over the past decade. While these medications have the potential to provide optimal pain relief for many patients, they do not come without risk of side effects. The main effects limiting the use of opioid medications are those associated with the gastrointestinal tract, especially nausea and constipation. Several treatment options exist to help manage these side effects, but prevention is the key component for patients taking opioid analgesics. Nonpharmacologic methods are just as important as pharmacologic methods for the prevention and management of side effects. Pharmacists play an important role in educating patients about the side effects associated with these medications and the options available for preventing and managing them.
One in four Americans has experienced pain lasting more than 24 hours in the previous month, and 42% of those reporting pain indicated that it had lasted for more than a year, according to the National Health and Nutrition Examination Survey.1 The estimated annual pain-related cost to the United States is in the billions of dollars.1 Pain control has become a major focus for clinics and hospitals around the country, in part because of regulatory standards; as a result, physicians are prescribing more pain medications, including opioid analgesics.2 Prescriptions for opioid analgesics have increased by 700% from 1997 to 2007.3 Along with the increased use of opioids comes an increased risk of side effects. Side effects of opioids can be quite troublesome and may lead to drug discontinuation, if severe enough. Major reasons for discontinuing opioid medications are gastrointestinal (GI) side effects such as nausea, vomiting, and constipation, along with central nervous system (CNS) effects.2 This article will focus on side effects involving the GI tract.
OPIOID PHARMACOLOGY
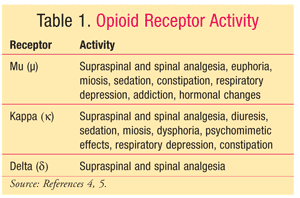
Opioids produce their analgesic effects by activating G protein–coupled receptors located in the brain and spinal cord regions that are involved in the transmission and modulation of pain.4 There are three major opioid receptors: mu, delta, and kappa.4,5 These receptors are located in the brain, the spinal cord, and various peripheral tissues, including vascular, cardiac, lung, and gut.5 Effects caused by opioids that have a high affinity for mu receptors include analgesia, euphoria, sedation, respiratory depression, and constipation.4-6 Activation of kappa receptors produces milder analgesic effects and less respiratory depression, whereas activation of delta receptors produces analgesia with minimal to no side effects (TABLE 1).4,5
COMMON SIDE EFFECTS AND THEIR TREATMENT
Opioids are highly effective analgesics; however, their side-effect profile often limits their use.6,7 Because opioid receptors are widely distributed throughout the body, opioids have a broad range of effects.4,5 Factors that may influence the development of side effects include gender, race, and increasing age.7 Effects such as sedation, mental clouding, respiratory depression, and euphoria are caused by the activation of CNS receptors.3-5 Patients usually become tolerant (i.e., require a higher dose to produce the same response) to these CNS side effects and to the analgesic effects of opioids.4,7 Opioid receptors are also highly dense within the GI tract and therefore carry side effects such as nausea, vomiting, gastroesophageal reflux, and constipation.4-8 Nausea and vomiting are usually transient and experienced only during initial treatment.7,8 Tolerance to constipation occurs only rarely, and patients often require preventive treatment.6
Nausea and Vomiting
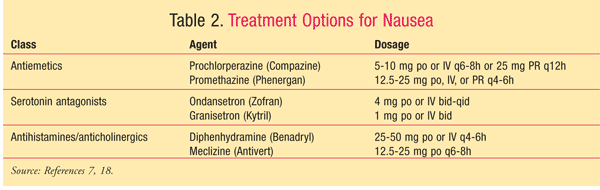
These common side effects are caused by opioid activity in the CNS and the GI tract.5,7 Nausea is estimated to occur in 25% of patients treated with opioids.7 Nausea can be induced by gastric upset caused by the reduction in gastric motility; other mechanisms include opioid activation of the chemoreceptor trigger zone (CTZ) and enhanced vestibular sensitivity.4,5,7 Vomiting is simply the motor consequence of nausea.5 Nausea associated with opioid use is usually temporary; however, if substantial nausea and vomiting occur, treatment may be required. In order to define the appropriate treatment, the mechanism of the nausea must be determined. Treatment options include antipsychotics, metoclopramide, serotonin antagonists, antihistamines, and steroids. These agents (TABLE 2) may be used alone or in combination, and the duration of therapy is based on patient-specific symptoms. Currently, data do not support one antiemetic over another.7 Other options include using an alternative opioid or using a low dosage of an opioid receptor antagonist.
Nonpharmacologic Therapies: Nonpharmacologic options for the treatment of opioid-induced nausea include adequate exposure to fresh air, relaxation techniques, limited dietary intake, and general distractions. General relaxation techniques such as rhythmic breathing may be beneficial. Patients should avoid foods that are spicy or excessively sweet or salty. Some patients may find relief by reading, listening to music, or engaging in other activities that distract them from the nausea.7,8
Antiemetics: Antiemetics, which are relatively inexpensive, work by blocking dopamine receptors within the CTZ.7 These agents have a risk of side effects. Patients should be counseled about the possibility of akathisia, dystonic reactions, sedation, or orthostatic hypotension. One agent, metoclopramide, blocks dopamine receptors in the CTZ and promotes peristalsis through the release of acetylcholine.8 The use of metoclopramide frequently is limited by the drug’s CNS effects, such as sedation and extrapyramidal effects.7,8 This drug also carries a black box warning for possible risk of tardive dyskinesia. Prolonged treatment (>12 weeks) is not recommended, except in rare and extreme cases. Based on these limitations and risks, metoclopramide is not considered an appropriate recommendation for the treatment of nausea and vomiting.9
Serotonin Antagonists: Serotonin antagonists are effective for preventing nausea and vomiting associated with CTZ stimulation. These agents block serotonin release, primarily within the GI tract. They are free of extrapyramidal effects and are generally well tolerated by patients. Although these medications are approved for the treatment of nausea and vomiting, they have not been approved specifically for opioid-induced nausea and vomiting.7,8
Antihistamines and Anticholinergics: Antihistamine agents and anticholinergic drugs may be beneficial for patients who experience nausea related to ambulation or vertigo. These agents reduce opioid-induced vestibular sensitivity. Side effects include constipation, xerostomia, confusion, and blurred vision; however, when they are used at low doses, these agents are generally well tolerated.7,8
Gastroesophageal Reflux
Gastroesophageal reflux occurs as a result of delayed gastric emptying time.5 Reflux may often be treated with OTC antacids or with alginate preparations such as Gaviscon. Low-dose histamine2 (H2) blockers may benefit patients with mild symptoms. In patients with more severe symptoms, a proton pump inhibitor may be appropriate.10
Constipation
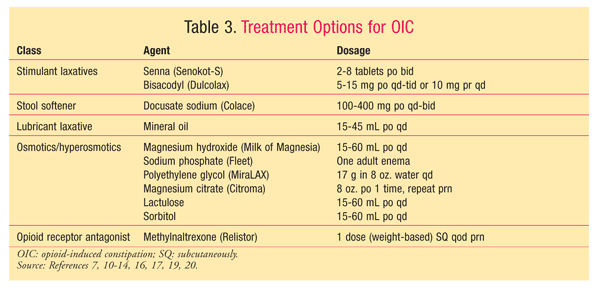
Opioid-induced constipation (OIC) is the most common and debilitating side effect of opioids.6 The concentration of opioid receptors in the GI tract is highly dense.4-6 Activation of these receptors, particularly mu receptors, inhibits gastric emptying, reduces mucosal secretions, and increases fluid reabsorption.6,7 These factors cause stools to become hard and dry, and constipation ultimately develops.6,7 The constipating effects of opioids are considered to be dose related and are more common with long-term use.7 However, even with acute dosing, approximately 45% to 95% of patients receiving opioids develop constipation.5 Prevention is a key component of OIC treatment, and a common goal of therapy is for the patient to have one bowel movement every 1 to 2 days.7 The following sections discuss nonpharmacologic methods and scheduled medication regimens that can be used for prevention. Often, a patient will discontinue the opioid if OIC is not managed appropriately. Agents that may be used are listed in TABLE 3. Duration of therapy depends upon the patient and his or her symptoms, but most patients will likely need to use a single agent or a combination of agents for the duration of opioid therapy.
Nonpharmacologic Therapies: The risk of constipation can be minimized by increasing fluid and dietary fiber intake, establishing a regular toileting routine, and increasing physical activity. These actions help stimulate the intestines. Patients should be cautioned that too much dietary fiber could lead to bowel obstruction, and they should discuss their current diet with their provider to determine whether any changes should be made. Patients should be encouraged to always speak with their provider before implementing a new exercise regimen. Patients should be advised that these measures alone often are insufficient to treat OIC and that they may also require pharmacologic therapy.7
Stimulant Laxatives: Stimulants are the most common type of laxative used to treat OIC. These agents work by triggering intestinal-wall muscles to tighten, squeezing the stool and allowing it to pass more easily. The limitations of these medications should be recognized. Side effects such as bloating, abdominal cramping, and incontinence may lead to poor patient adherence. Fluid and electrolyte imbalances may also occur; therefore, patient education on the proper use of these agents is very important.11
Stool Softeners: These medications reduce surface tension of the oil-water interface of the stool. The enhanced incorporation of water and fat results in stool softening. Side effects associated with these agents are minimal, with the most common one being bitter taste. Use of a stool softener alone is often not effective for OIC; therefore, the use of a scheduled stimulant laxative with or without a stool softener is usually recommended.10
Mineral Oil: Mineral oil produces its effects by reducing water absorption and lubricating the intestine. Patients should be counseled that this medication must be ingested while in an upright position and that they should remain upright for 30 to 60 minutes afterward to minimize the risk of aspiration. This agent has several drug interactions, so patients need to review their medications with their provider or pharmacist prior to use. Prolonged use of mineral oil also may result in decreased absorption of the fat-soluble vitamins A, D, E, and K.12
Osmotics and Hyperosmotics: An osmotic agent may be attempted if a patient does not have a sufficient response to stimulant laxatives. Bulk-forming laxatives are generally not recommended because they require ample fluid intake, which may not be appropriate for some patient populations. Bulk-forming laxatives may increase the risk of bowel obstruction in patients with impaired GI motility.7,10 Possible side effects of these agents include flatulence, bloating, stomach cramping, and nausea.13,14
Prescription Medications: Methylnaltrexone (Relistor) is a peripherally acting antagonist of the mu-opioid receptor. Methylnaltrexone targets binding sites in the tissues of the GI tract, which lessens OIC without compromising the analgesic effects in the CNS.15 It is indicated for the treatment of OIC in patients receiving palliative care who have failed standard laxative therapy. Methylnaltrexone is given subcutaneously, and dosing is weight based.16,17 Use of this agent for more than 4 months has not been studied. Patients should be advised about the possibility of dizziness, abdominal pain, flatulence, and diaphoresis.16
Opioid Rotation: Patients experiencing OIC from one opioid may benefit from opioid rotation. This includes using an alternative opioid agent or a different route of administration. Switching to a transdermal or parenteral route of administration, as opposed to the oral route, may partially alleviate symptoms if the opioid has a direct local effect.7
CONCLUSION: KEY POINTS FOR THE PHARMACIST
Opioids can be useful agents when managing acute and chronic pain, but they carry a risk of side effects. These effects can be debilitating and may result in discontinuation of the medication if they are not properly managed; therefore, patients should be counseled extensively about possible side effects and how to manage them properly. Side effects may be prevented or lessened if patients take appropriate nonpharmacologic measures such as proper hydration and dietary intake, physical activity, and establishment of a toileting routine. Pharmacists are an excellent resource for guiding patients to appropriate OTC medications. Proper education and preventive measures regarding possible side effects of opioid analgesics can lead to improved medication adherence and quality of life.
REFERENCES
1. Baumann TJ, Strickland JM, Herndon CM. Pain management. In: DiPiro JT, Talbert RL, Matzke GR, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 8th ed. New York, NY: McGraw-Hill Medical; 2011.
2. Volkow ND, McLellan TA. Curtailing diversion and abuse of opioid analgesics without jeopardizing pain treatment. JAMA. 2011;305:1346-1347.
3. Boyer EW. Management of opioid analgesic overdose. N Engl J Med. 2012;367:146-155.
4. Schumacher MA, Basbaum AI, Way WL. Opioid analgesics & antagonists. In: Katzung BG, Masters SB, Trevor AJ, eds. Basic & Clinical Pharmacology. 12th ed. New York, NY: McGraw-Hill Medical; 2012.
5. Yaksh TL, Wallace MS. Opioids, analgesia, and pain management. In: Brunton LL, Chabner BA, Knollman BC, eds. Goodman & Gilman’s The Pharmacological Basis of Therapeutics. 12th ed. New York, NY: McGraw-Hill Medical; 2011.
6. Satyavan K, Barna MM. Managing opioid-induced constipation. Pharmacy Times. www.pharmacytimes.com/publications/issue/2009/september2009/CounselingConstipation-0909. Accessed August 20, 2012.
7. Swegle JM, Logemann C. Management of common opioid-induced adverse effects. Am Fam Physician. 2006;74:1347-1354.
8. Porreca F, Ossipov MH. Nausea and vomiting side effects with
opioid analgesics during treatment of chronic pain: mechanisms,
implications, and management options. Pain Med. 2009;10:654-662.
9. Metoclopramide. Thomson Micromedex [online subscription database].
www.thomsonhc.com/micromedex2/librarian/ND_T/evidencexpert/ND_PR/evidencexpert/CS/802F50/ND_AppProduct/evidencexpert/DUPLICATIONSHIELDSYNC/26387C/ND_PG/evidencexpert/ND_B/evidencexpert/ND_P/evidencexpert/PFActionId/evidencexpert.DisplayDrugpointDocument?docId=373185&contentSetId=100&title=Metoclopramide+Hydrochloride&servicesTitle=Metoclopramide+Hydrochloride&topicId=dosingAndIndicationsSection&subtopicId=adultDosingSection.
Accessed October 24, 2012.
10. Panchal SJ, Müller-Schwefe P, Wurzelmann JI. Opioid-induced bowel dysfunction: prevalence, pathophysiology and burden. Int J Clin Pract. 2007;61:1181-1187.
11. Grasberger F, el Tahir KE, O’Reilly M. Senna. Thomson Micromedex
[online subscription database].
www.thomsonhc.com/micromedex2/librarian/ND_T/evidencexpert/ND_PR/evidencexpert/CS/C8C449/ND_AppProduct/evidencexpert/DUPLICATIONSHIELDSYNC/88D1F5/ND_PG/evidencexpert/ND_B/evidencexpert/ND_P/evidencexpert/PFActionId/evidencexpert.DisplayAltMedEvalDocument?docId=10&contentSetId=60&topicId=cautionsSection&subtopicId=adverseReactionsSection.
Accessed July 8, 2012.
12. Mineral oil. Thomson Micromedex [online subscription database].
www.thomsonhc.com/micromedex2/librarian/ND_T/evidencexpert/ND_PR/evidencexpert/CS/251906/ND_AppProduct/evidencexpert/DUPLICATIONSHIELDSYNC/A87BBA/ND_PG/evidencexpert/ND_B/evidencexpert/ND_P/evidencexpert/PFActionId/evidencexpert.DoIntegratedSearch?SearchTerm=mineral%20oil.
Accessed July 22, 2012.
13. Polyethylene glycol. Thomson Micromedex [online subscription
database].
www.thomsonhc.com/micromedex2/librarian/ND_T/evidencexpert/ND_PR/evidencexpert/CS/60CA22/ND_AppProduct/evidencexpert/DUPLICATIONSHIELDSYNC/5AE1CA/ND_PG/evidencexpert/ND_B/evidencexpert/ND_P/evidencexpert/PFActionId/evidencexpert.DisplayDrugpointDocument?docId=928045&contentSetId=100&title=Polyethylene+Glycol+3350&servicesTitle=Polyethylene+Glycol+3350&topicId=contraindicationsWarningsSection&subtopicId=precautionsSection.
Accessed July 22, 2012.
14. Lactulose. Thomson Micromedex [online subscription database].
www.thomsonhc.com/micromedex2/librarian/ND_T/evidencexpert/ND_PR/evidencexpert/CS/64D5C5/ND_AppProduct/evidencexpert/DUPLICATIONSHIELDSYNC/59044D/ND_PG/evidencexpert/ND_B/evidencexpert/ND_P/evidencexpert/PFActionId/evidencexpert.DisplayDrugpointDocument?docId=329396&contentSetId=100&title=Lactulose&servicesTitle=Lactulose&topicId=adverseEffectsSection&subtopicId=commonSection.
Accessed July 22, 2012.
15. Greenwood-Van Meerveld B, Standifer KM. Methylnaltrexone in the treatment of opioid-induced constipation. Clin Exp Gastroenterol. 2008;1:49-58.
16. Methylnaltrexone bromide. Thomson Micromedex [online subscription
database].
www.thomsonhc.com/micromedex2/librarian/ND_T/evidencexpert/ND_PR/evidencexpert/CS/D596AD/ND_AppProduct/evidencexpert/DUPLICATIONSHIELDSYNC/960848/ND_PG/evidencexpert/ND_B/evidencexpert/ND_P/evidencexpert/PFActionId/evidencexpert.DisplayDrugpointDocument?docId=929021&contentSetId=100&title=Methylnaltrexone+Bromide&servicesTitle=Methylnaltrexone+Bromide&topicId=dosingAndIndicationsSection&subtopicId=adultDosingSection.
Accessed July 22, 2012.
17. Relistor (methylnaltrexone bromide) product information. Raleigh,
NC: Salix Pharmaceuticals, Inc; February 2012.
http://www.salix.com/assets/pdf/prescribe_info/relistor-pi.pdf. Accessed
July 22, 2012.
18. DiPiro CV, Ignoffo RJ. Nausea and vomiting. In: DiPiro JT, Talbert RL, Matzke GR, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 8th ed. New York, NY: McGraw-Hill Medical; 2011.
19. Sharkey KA, Wallace JL. Treatment of disorders of bowel motility
and water flux; anti-emetics; agents used in biliary and pancreatic
disease. In: Brunton LL, Chabner BA, Knollman BC, eds. Goodman & Gilman’s The Pharmacological Basis of Therapeutics. 12th ed. New York, NY: McGraw-Hill Medical; 2011.
20. Powel PH, Fleming VH. Diarrhea, constipation, and irritable bowel
syndrome. In: DiPiro JT, Talbert RL, Matzke GR, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 8th ed. New York, NY: McGraw-Hill Medical; 2011.
To comment on this article, contact rdavidson@uspharmacist.com.





