US Pharm. 2009;34(6)(Generic Drug Review suppl):12-19.
The FDA defines narrow therapeutic range (NTR) drug products as “containing certain drug substances subject to therapeutic drug concentration or pharmacodynamic monitoring, and/or where product labeling indicates a narrow therapeutic range designation.”1 Other terms used to describe NTR drugs are narrow therapeutic index (NTI) and critical-dose drugs. This article will examine what is considered an NTI drug, various laws related to NTI drugs, and position statements of national associations.
What Is an NTI Drug?
In addition to the FDA definition of an NTI drug, there are many others. While the general definitions are similar, variations exist among organizations. TABLE 1 identifies examples of NTI drugs given by the FDA.
The North Carolina Board of Pharmacy defines an NTI drug as “those pharmaceuticals having a narrowly defined range between risk and benefit. Such drugs have less than a twofold difference in the minimum toxic concentration and minimum effective concentration in the blood or are those drug product formulations that exhibit limited or erratic absorption, formulation-dependent bioavailability, and wide intrapatient pharmacokinetic variability that requires blood-level monitoring.”2 As defined by the Therapeutic Products Directorate of Health Canada, an NTR drug is a drug wherein the ratio of the lowest concentration at which clinical toxicity occurs, to the median concentration providing a therapeutic effect, is less than or equal to two.3
Laws Concerning Bioequivalence and NTI Drugs
The FDA uses an average bioequivalence approach involving a comparison of means when it is determining a product’s bioequivalence. The core of the bioequivalence concept is an absence of a significant difference, which is considered to be less than 20% by the FDA.4 All data are expressed as a ratio of the average response (AUC and Cmax) for test and/or reference. The limit expressed in the second analysis is 125%, which is the reciprocal of 80%. Tests carried out using an analysis of variance and calculating a 90% confidence interval (CI) for the average of each pharmacokinetic parameter must be entirely within the 80% to 125% boundaries.5
In response to many reports appearing in the literature suggesting problems related to generic substitution, the FDA has conducted two large studies. One study was carried out on 224 bioequivalence studies submitted from 1985 to 1986. It found an average difference in AUC between reference and generic products to be 3.5%.6 The other study looked at 127 bioequivalence studies submitted in 1997. It found an average difference of 3.47% for AUC and 4.29% for Cmax.7
Based on this information, the FDA states “there are no documented examples of a generic product manufactured to meet its approved specifications that could not be used interchangeably with the corresponding brand-name drug.”8 Products evaluated as therapeutically equivalent can be expected to have an equivalent clinical effect whether the product is a brand name or a generic drug product.5
The FDA’s coding system for therapeutic equivalence consists of two or three characters.5 The first character is an “A” if the FDA considers the product to be therapeutically equivalent to other pharmaceutically equivalent products. The first character is a “B” if the FDA considers it not to be therapeutically equivalent. The second character gives other information about the product. Products coded “AA” contain active ingredients and dosage forms that do not have any actual or potential bioequivalence problems or drug quality or standards issues. If a study demonstrating bioequivalence is submitted for multisource drug products listed under the same active ingredients, dosage form, route of administration, and strength, the product is coded “AB.” A character can also represent the dosage form (e.g., a “T” would represent a topical product). In certain instances, a number is added to the end of the AB code to make a three-character code (i.e., AB1, AB2, AB3, etc.). Three-character codes are assigned only in situations when more than one reference listed drug of the same strength has been designated under the same heading, such as in the case of certain levothyroxine products that are discussed later in this article.
It is important for each pharmacist to be aware of the current laws of the state in which he or she practices. The following examples show the differences in laws governing the substitution of NTI drugs seen across the country at the state level.
In Texas, the Texas Board of Pharmacy was given the authority to create a list of NTI drugs, but to date the board has not added any drug to such a list.9 Substitution of drug products by a pharmacist is to be done with a product that is rated therapeutically equivalent in the FDA’s Orange Book, officially known as Approved Drug Products with Therapeutic Equivalence Evaluations.5 The substitution of NTI drugs is to get no special consideration over the substitution of any other drug.
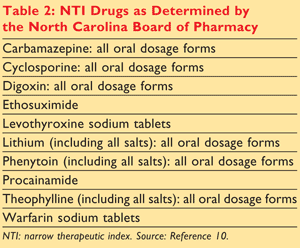
In North Carolina, General Statute (NCGS) 90-85.27 defines NTI drugs to mean those pharmaceuticals having a narrowly defined range between risk and benefit.2 Drugs identified as having NTIs (TABLE 2) are designated as NTI drugs by the Secretary of the North Carolina Department of Health and Human Services upon the advice of the State Health Director, the North Carolina Board of Pharmacy, and the North Carolina Medical Board, and are subject to the provisions of NCGS 90-85.28(b1).10 This law states that “A prescription for a narrow therapeutic index drug shall be refilled using only the same drug product by the same manufacturer that the pharmacist last dispensed under the prescription, unless the prescriber is notified by the pharmacist prior to the dispensing of another manufacturer’s product, and the prescriber and the patient give documented consent to the dispensing of the other manufacturer’s product.”2
California’s generic substitution section of The Pharmacy Law applies “to all prescriptions.” There is no legal classification of NTI drugs.11
Position Statements and Policies
At the 2007 Annual Meeting of the American Medical Association (AMA), the House of Delegates considered a report written in response to a resolution that called for “written notifications” to physicians from third-party payers and pharmacists prior to generic substitution of NTI drugs.4,12 It was concluded that a more stringent generic substitution process for NTI drugs was unnecessary. It was resolved that pharmacists and pharmacy organizations should be made aware of current AMA policy H-125.984 on generic drugs and AMA policy H-115.994 on prescription labeling.13,14
The Academy of Managed Care Pharmacy (AMCP) “opposes legislation that restricts the appropriate generic substitution of narrow therapeutic index (NTI) drugs…AMCP supports allowing pharmacists, in consultation with prescribers, to exercise professional judgment, based on scientific information, when determining whether a generic drug is an appropriate substitute for its brand name equivalent.”15
The American Society of Health-System Pharmacists (ASHP) supports “the current processes used by the Food and Drug Administration (FDA) to determine bio equivalence of generic drug products, including those with a narrow therapeutic index, and to recognize the authority of the FDA to decide if additional studies are necessary to determine equivalence.”16
The American Pharmacists Association (APhA) has helped facilitate excellent resources for pharmacists. A special feature in the Journal of the American Pharmacists Association presents tools and resources for pharmacists to use when considering prescription drug product substitution. An example is the Manolakis tool, which is a flow chart with 18 boxes. Within each box, a decision is to be made that will help the pharmacist make an appropriate dispensing decision that is patient-centered and evidence-based.17 A monograph published in 2000, entitled Substitution of Critical Dose Drugs: Issues, Analysis, and Decision Making, presents a thorough discussion of the issue of helping pharmacists navigate this controversial area.18 Both of these are excellent resources and should be added to every pharmacist’s library.
The National Community Pharmacists Association (NCPA) supports the continued right of the pharmacist to utilize his or her professional judgment when deciding whether to substitute a chemically equivalent generic product for a brand-name pharmaceutical product in all therapeutic categories, including NTI medications.19
NTI Drugs
Antiarrythmic Drugs: There have been case reports of potential clinical inequivalence for some antiarrhythmic agents, such as quinidine, procainamide, disopyramide, and amiodarone, with effects that include actual and possible recurrent supraventricular tachycardia and atrial fibrillation with a rapid ventricular response.20 The AMA still concludes that “it is possible to switch…products with minimal risk to the vast majority of patients.” They do feel that monitoring of drug concentrations is warranted.4
Levothyroxine: Levothyroxine substitution has been an issue for quite some time due to the variety of generics available. There are five brand-name marketed innovator products for the thyroid hormone replacement levothyroxine: Unithroid, Synthroid, Levoxyl, Levo-T, and Levothroid, in addition to generics made by multiple manufacturers. In addition to the FDA using the two- or three-character therapeutic equivalence (TE) codes for levothyroxine, it has specific explanations of certain therapeutically equivalent products due to the fact that the codes could be quite confusing.5
One common TE code between products indicates that they are therapeutically equivalent. Levo-T (Alara NDA 021342), Levothyroxine Sodium (Mylan ANDA 76187), Unithroid (Jerome Stevens NDA 021210), and Levothyroxine Sodium (Merck KGAA 76752) tablets have been determined to be therapeutically equivalent to corresponding strengths of Synthroid (Abbott NDA 021402) tablets with the TE code AB2.5
It has been demonstrated that the current FDA Guidance for establishing bioequivalence of levothyroxine is adequate, and, therefore, the FDA accepts products that are therapeutically equivalent. No generic approved by the FDA has been shown to result in safety or efficacy profiles different from its brand counterparts.21
Antiepileptic Drugs (AEDs): The AEDs (e.g., phenytoin, carbamazepine, lamotrigine, oxcarbazepine) have multiple factors that might increase the likelihood of problems with generic substitution, including low water solubility, NTR, and nonlinear pharmacokinetics.22 It has been questioned whether AEDs are switchable under all clinical circumstances.23 Examples include phenytoin toxicity after generic substitution and breakthrough seizures after carbamazepine generic substitution.
Warfarin: The success of warfarin therapy depends greatly on appropriate therapeutic blood concentrations. Cases of subtherapeutic international normalized ratio (INR) values reported have been reported after a switch from the brand-name drug Coumadin to the warfarin generic while all other variables were kept consistent.24 The authors concluded that any patient switching between Coumadin and generic warfarin should have their INR monitored more carefully.
Another study in a health maintenance organization (HMO) population was conducted to determine whether a generic warfarin could be added to formulary without concern about substitution.25 Milligan et al determined that substitution of a certain manufacturer’s warfarin for Coumadin did not significantly affect INR control, warfarin management, or adverse events. They concluded that HMOs can safely substitute at least one generic formulation of warfarin without extra monitoring.
Transplant Drugs or Anti-rejection Medications: A 1997 survey completed by 59 pharmacists via telephone and fax was used to assess pharmacists’ role at solid-organ transplant centers. Parameters included factors pharmacists considered important for generic product selection and pharmacists’ attitudes about the FDA guidelines on bioequivalence testing. Only 12% of the respondents of this survey said they thought that the FDA guidelines on bioequivalence testing were appropriate for NTI drugs (called critical-dose drugs in the study), and 92% thought that bioequivalence testing for NTI drugs should be conducted in actual patients.26 Efficacy, safety, the presence of an NTI, bioequivalence, and clinical consequences were identified by transplant pharmacists as important factors in decisions about generic product selection.
Conclusion
No matter what your views and opinions are regarding the generic substitution of NTI drugs, it is important to be educated on the matter. This article reviewed federal and state laws, policies and statements from federal authorities and national associations, and some of the drugs that are involved in this subject. All medications, not just NTI drugs, should be treated with respect and substituted appropriately.
REFERENCES
2. Pharmacy Laws of North Carolina. October 2008. Chapter 90. Medicine and Allied Occupations. North Carolina Pharmacy Practice Act. Article 4A. 90-85.28(b1). www.ncbop.org/LawsRules/
3. Palylyk-Colwell E, Jamali F, Dryden W, et al. Bioequivalence and interchangeability of narrow therapeutic range drugs. Canadian Society for Pharmaceutical Sciences Discussion. J Pharm Pharmaceut Sci. 1998;1:2-7.
4. Report 2 of the Council on Science and Public Health. Generic substitution of narrow therapeutic index drugs. June 2007. www.ama-assn.org/ama/no-index/
5. Approved Drug Products with Therapeutic Equivalence Evaluations. FDA Center for Drug Evaluation and Research; 2009. www.fda.gov/cder/orange/
6. Nightingale SL, Morrison JC. Generic drugs and the prescribing physician. JAMA. 1987;258:1200-1204.
7. Henney JE. Review of generic bioequivalence studies. JAMA. 1999;282:1995.
8. Therapeutic equivalence of generic drugs letter to health practitioners. FDA. January 28, 1998. www.fda.gov/cder/news/
9. Texas Administrative Code. Title 22, Part 15, Chapter 309, Rule §309.3 Generic Substitution. September 7, 2008. Texas State Board of Pharmacy. http://info.sos.state.tx.us/
10. Narrow therapeutic index drugs. North Carolina Medicaid Pharmacy Newsletter. Number 115. March 2004. www.dhhs.state.nc.us/DMA/
11. Business & Professions Code Article 4—Requirements for Prescriptions Section 4073. 2008 Lawbook for Pharmacy. California Board of Pharmacy. www.leginfo.ca.gov/cgi-bin/
12. Letter from Michael Maves, MD, MBA, Executive Vice President and CEO, American Medical Association to Mark Merritt, President and CEO, Pharmaceutical Care Management Association. August 30, 2007. www.pharmacist.com/AM/
13. Policy H-125.984. January 2008. American Medical Association PolicyFinder. www.ama-assn.org/ama/no-index/
14. Policy H-115.994. January 2008. American Medical Association PolicyFinder. www.ama-assn.org/ama/no-index/
15. Narrow therapeutic index (NTI) drugs, interchange of. Academy of Managed Care Pharmacy. January 28, 2004. www.amcp.org/amcp.ark?p=
16. Generic substitution of narrow therapeutic index drugs. 2003. ASHP Policy Positions. www.ashp.org/Import/
17. Manolakis P. Prescription drug product substitution decision support. J Am Pharm Assoc.
2007;47:328-347.
18. Alloway R, Barr WH, Flagstad M, Lake K. Substitution of critical dose drugs: issues, analysis, and decision making. 2000. American Pharmaceutical Association. www.pharmacist.com/AM/
19. E-mail communication with Michael Conlan, National Community Pharmacists Association (NCPA). NCPA 2009 Statement of Position: Narrow Therapeutic Index Medications. February 27, 2009.
20. Reiffel JA. Issues in the use of generic antiarrhythmic drugs. Curr Opin Cardiol. 2001,16:23-29.
21. Bolton S. Bioequivalence studies for levothyroxine. AAPS Journal. 2005;7:E47-E53. www.aapsj.org/view.asp?art=
22. Crawford P, Feely M, Guberman A, Kramer G. Are there potential problems with generic substitution of antiepileptic drugs? A review of issues. Seizure. 2006;15:165-176.
23. Gidal BE, Tomson T. Debate: substitution of generic drugs in epilepsy: is there cause for concern? Epilepsia. 2008;49(suppl 9):56-62.
24. Hope KA, Havrda DE. Subtherapeutic INR values associated with a switch to generic warfarin. Ann Pharmacother. 2001;35:183-187.
25. Milligan PE, Banet GA, Waterman AD, Gatchel SK. Substitution of generic warfarin for Coumadin in an HMO setting. Ann Pharmacother. 2002;36:764-768.
26. Vasquez EM, Min DI. Transplant pharmacists’ opinions on generic product selection of critical-dose drugs. Am J Health Syst Pharm. 1999;56:2246-2247.
To comment on this article, contact rdavidson@jobson.com.






