US Pharm. 2014;39(9):51-54.
ABSTRACT: Coronary heart disease, which is the most common type of heart disease, is the number-one killer of women in the United States. Awareness of the prevalence of heart disease in women is increasing, but awareness is lower in younger women and in minorities. It has been suggested that women are being misdiagnosed because their symptoms may differ from those experienced by men. However, a recent study in which heart-attack diagnoses were made based on chest-pain characteristics (CPCs) such as location of pain/discomfort, onset and degree of pain, and pain radiation to other parts of the body concluded that these parameters alone are not powerful enough to confirm diagnosis. Sex-specific differences in CPC symptoms among women and men are subjective, and the exact differences remain unclear.
The term heart disease comprises numerous cardiovascular conditions, including coronary artery disease (CAD), cardiovascular disease, coronary heart disease (CHD), heart attack, and acute myocardial infarction (MI). Many of these conditions are related to atherosclerosis or blood clots in the coronary arteries.1 A woman having a heart attack is more likely than a man to die.2 It has been suggested that physicians may be misdiagnosing women more often because their symptoms may differ from those experienced by men. Although about 90% of patients with acute MI present with chest pain or discomfort, some patients present without typical chest pain. Sex-specific differences in symptoms are claimed and may be worth noting, but may not be reliable across the population.3 The purpose of this article is to examine literature reports on differences in heart-attack symptoms that may exist between men and women.
Epidemiology
According to the American Heart Association (AHA), about 600,000 people in the United States die of heart disease every year, and heart disease is the leading cause of death in both men and women.2 In 2009, most of these deaths were due to heart disease in men. CHD is the most common type of heart disease, killing more than 400,000 people annually.2 About 5.8% of white, 7.6% of black, and 5.6% of Mexican American women have CHD.4 Each year, about 720,000 Americans have a heart attack. Of these attacks, 515,000 are a first heart attack and 205,000 are in people who have previously had a heart attack. The overall annual cost of CHD in the U.S. is about $110 billion and includes costs for healthcare services, medications, and lost productivity.5
The commonly held notion that heart disease is primarily a man’s disease has been greatly challenged. According to a recent AHA study, women’s awareness of heart disease is increasing. The number of women aware that heart disease is the leading cause of death has significantly increased in the last 15 years, but this knowledge is still lacking in minorities and younger women. Awareness of CHD among U.S. women increased from 30% in 1997 to 54% in 2009 and 56% in 2012.2,4,6 Heart disease was identified as the top killer by 36% of both black women and Hispanic women. Women aged 25 to 34 years had the lowest awareness rate of any age group (44%). Earlier, most women had cited cancer as the leading killer. The first women-specific clinical recommendations for CHD prevention were published by the AHA in 1999.2
To promote increased social awareness of heart attacks in women, the Go Red For Women movement was launched, including the National Wear Red Day.7 In 2013, the AHA celebrated the 10th anniversary of this initiative with a national convention focusing on heart-healthy educational activities and health screenings. The intent is to arm women with facts about heart disease, dispel myths and folklore, identify specific heart-attack symptoms, offer tips on how to cope with heart disease, and provide the latest news and research on beating and treating heart disease.
CHD is now the most common type of heart disease and is recognized as the number-one killer of women.8 In the U.S., 1 in 4 women dies from heart disease. More women die from CHD than from cancer, chronic respiratory disease, Alzheimer’s disease, and accidents combined.2,8 Other types of heart disease in women include coronary microvascular disease (MVD) and broken heart syndrome (emotional stress-induced cardiomyopathy, or takotsubo cardiomyopathy). MVD affects the heart’s tiny arteries by damaging the artery walls.9 CHD death rates in women aged 35 to 54 years are increasing, possibly because of the obesity epidemic.10
CHD
In CHD, plaque forms on or within the inner lining of the coronary arteries, reducing the flow of oxygen-rich blood to the heart and causing fatigue.1,11 Plaque consists of fat, cholesterol, calcium, and other substances found in the blood. Over time, plaque hardens and may rupture. Hardening plaque deposits can partially or totally restrict blood flow to the heart, causing chest pain (angina), pressure, or discomfort. The most common cause of a heart attack is when plaque ruptures and a blood clot forms on its surface. A large blood clot can partially or totally block blood flow through an artery, causing heart tissue to die. A portion of the clot also can break loose and enter systemic blood circulation. The circulating clot may lodge in a smaller blood vessel and restrict blood flow to areas beyond the clot. Over time, ruptured plaque hardens and further narrows coronary arteries. In addition to angina and heart attack or MI, CHD can lead to heart failure, arrhythmias, and sudden cardiac arrest.
In CAD, blood-vessel lumen becomes narrowed and blood can no longer flow freely to the muscle cells.1 The narrowing of the vessels is caused by the development of atheromas (fatty tumors in the intimal lining of the vessels), attracting platelets and immune factors and causing swelling and the development of larger deposits in the intima. The lumen also loses its natural elasticity and becomes unable to respond to normal stimuli to dilate or constrict to meet the needs of the tissues.
The diseased heart may function without noticeable problems until increases in activity or other stresses place a demand on it to beat faster or harder.1 Normally, the heart would stimulate blood vessels to dilate and deliver more blood when this occurs, but the narrowed vessels are unable to respond and cannot supply the blood needed by the working heart. The heart muscle then becomes hypoxic. This imbalance between oxygen supply and demand manifests as pain or angina pectoris (meaning “suffocation of the chest”). Although the heart muscle does not contain pain fibers, a chemical called substance P is released from ischemic myocardial cells, and pain is felt whenever substance P reacts with pain receptors in the heart. This pain does not result in heart-muscle damage. If a coronary vessel becomes completely occluded and is unable to deliver blood to the cardiac muscle, the area of the heart muscle that depends on that vessel for oxygen becomes ischemic and then necrotic. This event is a myocardial infarction, and the pain associated with it can be excruciating.
CHD Risk Factors
Hypertension, elevated LDL cholesterol, and smoking are cardinal risk factors for heart disease (TABLE 1). About 50% of Americans have at least one of these risk factors.12 Other medical conditions and lifestyle choices confer a higher risk of heart disease, including diabetes, overweight and obesity, poor diet, physical inactivity, and excessive alcohol use. CHD incidence in the U.S. is significantly higher in black women than in white women (286/100,000 vs. 205/100,000). This correlates with the lower rates of awareness of heart disease and stroke in black women versus white women.7,8,13,14 Annually, 55,000 more women than men have strokes.7

Hypertension trends are higher in women than in men, and the likelihood appears to increase as women age, especially after age 65 years.2 The prevalence of hypertension in U.S. women is increasing, especially in black women. Prevalence in black women increased from about 36% in 1988–1994 to 41% in 1999–2002, the highest prevalence worldwide. One contributor is the ongoing increase in average body weight or BMI, with nearly two-thirds of U.S. women older than 20 years being overweight or obese.12 The increase in obesity appears to be a key factor in the burgeoning epidemic of type 2 diabetes, now present in more than 12 million U.S. women (6.5% of non-Hispanic white women and 12.7 % of Hispanic women).2 Diabetes is also a major risk factor for MI and stroke.15 Each year, about 55,000 more women than men die of stroke, and before age 75 years. To a great extent, CHD could be avoided or prevented by establishing a healthy lifestyle (TABLE 1) early in life and continuing this pattern throughout life. Not only should the risk of heart disease be lower, but the individual should have a better quality of life.
Cardiovascular Symptoms of Heart Attacks
Both men and women having a heart attack can experience chest pressure that feels like an elephant sitting on one’s chest. About 64% of women who die suddenly of CHD have no previous symptoms prior to the fatal attack.13 Others experience angina (dull, heavy-to-sharp chest pain/discomfort); neck, jaw, or throat pain; or pain in the upper abdomen or back. Anginal symptoms may occur during rest or physical activity or may be triggered by mental stress.16
Women reportedly are more likely to present with chest pain that is sharp or burning and more frequently have pain in the neck, jaw, throat, abdomen, or back. Sometimes heart disease is silent and not diagnosed until a woman experiences signs or symptoms of heart attack or acute MI (severe chest pain/discomfort, upper-back pain, indigestion, heartburn, nausea/vomiting, extreme fatigue, upper-body discomfort, shortness of breath, light-headedness, cold sweats); heart failure (shortness of breath, fatigue, swelling of feet/ankles/legs/abdomen); arrhythmia (fluttering feelings in chest, palpitations); or stroke (sudden weakness, paralysis or numbness of face/arms/legs, facial droop, especially on one side of the body).2 Other symptoms of stroke include confusion, trouble speaking or understanding speech, difficulty seeing in one or both eyes, shortness of breath, dizziness, loss of balance or coordination, loss of consciousness, or sudden and severe headache.13
Heart-Attack Symptoms and Treatment in Men Versus Women
Reportedly, men having a heart attack experience a crushing type of chest pain that radiates down the left arm, whereas women may complain of pressure or pain in the neck, jaw, lower chest, or abdomen that may spread to the shoulder or arm.14,17 Sex-specific differences in symptoms among women and men are subjective, and the claimed differences remain unclear. A recent study investigated differences in symptoms in 2,475 patients (796 women, 1,679 men) who presented at hospital emergency departments with acute chest pain between April 2006 and August 2012.3 Acute MI was diagnosed in 18% of women and 22% of men. Most of the 34 chest-pain characteristics (CPCs) identified were reported with similar frequency in women and men. There were no significant differences in the types of chest pain experienced by men and women. CHD treatment was reported as usually the same for both women and men and often included medication, medical and surgical procedures, lifestyle changes, and cardiac rehabilitation.
Data from this study confirm that CPCs (including location of pain/discomfort, onset and degree of pain, and pain radiation to other parts of the body) are not powerful enough to be used to confirm a diagnosis of acute MI; other less subjective measures are needed.3 Also, it was suggested that about 80% of patients who complained of chest pains and discomfort were not having a heart attack, but rather were suffering from indigestion, acid reflux, or another relatively benign disorder. See Case Study. The most important things that any person who suspects that he or she may be having an acute MI should know are the relevant signs and symptoms and when to call 911 or get to a hospital emergency department.

The Pharmacist’s Role
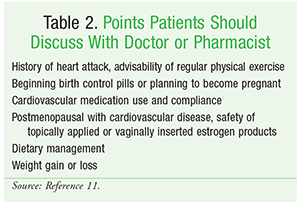
Pharmacists are the most accessible, knowledgeable, and trusted healthcare professionals in the local community. As such, pharmacists can play a key role in helping those with heart disease by actively interacting with male and female clients who regularly frequent the pharmacy, as well as consulting with other healthcare professionals in hospitals and clinics on cardiovascular issues. Pharmacists can be a readily available resource for clients with a history of heart disease and can reinforce information provided by physicians (TABLES 1 and 2) and cardiac rehabilitation therapists. Pharmacists can also participate in community health-information fairs and seminars focusing on various heart-disease issues and treatments in men and women—e.g., awareness of signs and symptoms, knowing when to call 911, cardiovascular medication use and compliance, nonprescription medication use, reversible and manageable risk factors, heart-healthy dietary considerations, lifestyle activity, and strategies to prevent heart attacks.
REFERENCES
1. Brunton L, Chabner BA, Knollmann BC, eds. Goodman and Gilman’s The Pharmacological Basis of Therapeutics. 12th ed. New York, NY: McGraw-Hill; 2011.
2. Go AS, Mozaffarian D, Roger VL, et al. Heart disease and stroke statistics—2014 update: a report from the American Heart Association. Circulation. 2014;129:e28-e92.
3. Rubini Gimenez M, Reiter M, Twerenbold R, et al. Sex-specific chest pain characteristics in the early diagnosis of acute myocardial infarction. JAMA Intern Med. 2014;174:241-249.
4. Mosca L, Hammond G, Mochari-Greenberger H, et al. Fifteen-year trends in awareness of heart disease in women: results of a 2012 American Heart Association national survey. Circulation. 2013;127:1254-1263.
5. Heidenreich PA, Trogdon JG, Khavjou OA, et al. Forecasting the future of cardiovascular disease in the United States: a policy statement from the American Heart Association. Circulation. 2011;123:933-944.
6. Mosca L, Mochari-Greenberger H, Dolor RJ, et al. Twelve-year follow-up of American women’s awareness of cardiovascular disease risk and barriers to heart health. Circ Cardiovasc Qual Outcomes. 2010;3:120-127.
7. American Heart Association. Go Red For Women. www.goredforwomen.org. Accessed June 9, 2014.
8. Roger VL, Go AS, Lloyd-Jones DM, et al; American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Heart disease and stroke statistics—2011 update: a report from the American Heart Association. Circulation. 2011;123:e18-e209. [Erratum in: Circulation. 2011;123:e240.]
9. National Heart, Lung, and Blood Institute (NHBL). How does heart disease affect women? www.nhlbi.nih.gov/health/health-topics/topics/hdw. Accessed June 10, 2014.
10. Mosca L, Benjamin EJ, Berra K, et al. Effectiveness-based guidelines for the prevention of cardiovascular disease in women—2011 update: a guideline from the American Heart Association. Circulation. 2011;123:1243-1262.
11. NHBL. How is heart disease treated? www.nhlbi.nih.gov/health/health-topics/topics/hdw/treatment.html. Accessed June 16, 2014.
12. CDC. Million hearts: strategies to reduce the prevalence of leading cardiovascular disease risk factors—United States, 2011. MMWR Morb Mortal Wkly Rep. 2011;60:1248-1251.
13. Kleindorfer D, Khoury J, Broderick JP, et al. Temporal trends in public awareness of stroke: warning signs, risk factors, and treatment. Stroke. 2009;40:2502-2506.
14. Ferris A, Robertson RM, Fabunmi R, et al. American Heart Association and American Stroke Association national survey of stroke risk awareness among women. Circulation. 2005;111:1321-1326.
15. Hertz RP, Unger AN, Cornell JA, Saunders E. Racial disparities in hypertension prevalence, awareness, and management. Arch Intern Med. 2005;165:2098-2104.
16. CDC. State-specific mortality from sudden cardiac death—United States, 1999. MMWR Morb Mortal Wkly Rep. 2002;51:123-126.
17. Pilote L. Chest pain in acute myocardial infarction: are men from Mars and women from Venus? JAMA Intern Med. 2014;174:249-250.
To comment on this article, contact rdavidson@uspharmacist.com.





