US Pharm. 2015:40(6):9-11.
The foot is composed of 26 bones and 33 joints, and is layered with a matrix of more than 120 muscles, ligaments, and nerves.1 Functionality of this complex structure involves weight bearing, shock absorption, mobility, and balance. With age, however, changes in the foot place the elderly at very high risk for foot problems. Chronic morbidity may impinge upon foot health, and senescence, physical disability, and obesity can make older adults especially vulnerable to podiatric conditions.2 Pain due to foot problems can become especially distressing for an older adult who may already be experiencing interference with activities of daily living (ADL), leisure pursuits, domestic chores, and restorative sleep owing to multiple chronic conditions (MCCs) commonly seen in this population.
Since feet are the body parts most distant from the heart and central nervous system, early clues of cardiovascular and neurologic illness may initially appear there.3 Foot problems may develop from age-related changes in neurologic and cardiopulmonary function and metabolic and cell-mediated responses. Skeletal and skin structure changes cause the skin to become drier, the foot to become wider and flatter, and the adipose padding on the sole of the foot to wear down.1,2 Ultimately, foot problems in older adults have the potential to impair balance and function, contributing to altered independence and quality of life. Age-related changes and MCCs not only contribute to foot problems, but may also affect the treatment of these conditions.2
Foot-pain etiologies are often grouped under one of the following categories: 1) Ill-fitting shoes (e.g., pointed-toe, high-heeled); 2) certain medical conditions (e.g., diabetes, Parkinson’s disease, cerebral palsy); and 3) high-impact exercise (e.g., jogging, strenuous aerobics).1 Injuries include muscle cramps, acute knee and ankle injuries, pain and inflammation of the plantar fascia, and pain and inflammation in the ball of the foot; corns, calluses, and blisters are also common and cause patients to seek remedies and relief. Of note, the presence of calluses in a diabetic patient is a strong predictor of ulceration, particularly in those who have a history of foot ulcers.1
Foot Pain
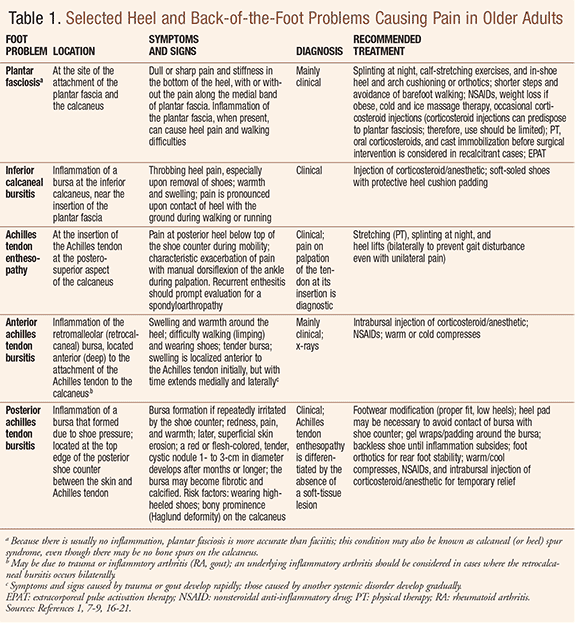
Foot pain generally appears in one of three anatomical areas: the toes, the forefoot, or the back of the foot.1 This column will focus on a brief overview of common problems of the heel (calcaneus) and back of the foot (TABLE 1), noting that pain originating in the heel can potentially extend across the sole (plantar surface) to the ball of the foot (metatarsophalangeal joint).
A tenet of geriatric healthcare is that pain should not be considered a normal consequence of aging and is always due to pathology, even if not easily identified or fully appreciated by the clinician.4 Since pain continues to remain undertreated in the geriatric population for a variety of reasons, pharmacists providing care for this specialty population need never underestimate that persistent pain interferes with the enjoyment of life and is associated with harmful effects on mood, function, and social interaction.
Importantly, nonpharmacologic approaches to pain will avoid drug-drug and drug-disease interactions, which are especially problematic in older adults with MCCs. Overemphasis on pharmacologic approaches ignores the potential benefits of physical and cognitive behavioral strategies.4 Furthermore, failure to employ nonpharmacologic strategies for pain often accounts for treatment failure.4 Nonpharmacologic treatment interventions (TABLE 1)—such as night splints, heel cups, arch cushions, and gel wraps—for heel and back-of-the-foot problems are usually considered initial treatment and are available OTC in pharmacies.
NSAIDs may be necessary; however, they are considered to be potentially inappropriate in the geriatric population (Beers Criteria—quality of evidence: moderate; strength of recommendation: strong).5 If necessary, NSAIDs should be used in the lowest possible dose for the shortest period possible, bearing in mind that they can compromise existing renal function, particularly when creatinine clearance (CrCl) is <30 mL/min.5 Of note, the elderly may exhibit NSAID-related central nervous system adverse effects, such as confusion, agitation, and hallucinations, at lower doses than in younger adults.
In light of the risk for adverse effects, corticosteroids should be used cautiously in the elderly, in the smallest possible dose and for the shortest possible time. These agents should be used with caution in patients who have thyroid disease, hepatic and/or renal impairment, cardiovascular disease, diabetes, or myasthenia gravis, and are at risk for osteoporosis or seizures.5 Additionally, there is corticosteroid-associated risk of perforation in those patients at risk for gastrointestinal diseases such as diverticulosis, peptic ulcer, and ulcerative colitis.5
Heel and Back-of-the-Foot Pain in Older Adults
Up to 10% of people will experience heel pain.6 Most often, heel pain is the result of strain of the plantar fascia on the bottom of the foot and has been referred to as plantar fasciitis; plantar-fascia pain syndromes are usually not associated with inflammation; therefore, the term plantar fasciosis is more accurate. Another term, calcaneal (or heel) spur syndrome, is often used since plantar fasciosis was thought to be caused by a heel spur, although there may be no bone spurs on the calcaneus; research has found that on x-ray, heel spurs are seen in people with and without plantar fasciosis.7,8 Plantar fasciosis is one of the most common orthopedic foot complaints. While this condition is seen in both men and women, it most often affects active men age 40 to 70 years.8
Selected risk factors for the development of this condition include occupations requiring sitting or prolonged walking on hard surfaces; very high or low foot arches; wearing high-heeled shoes; sudden weight gain; sedentary lifestyle; and running. These factors increase risk by leading to contracted or shortened calf muscles and plantar fascia.8
Other key points regarding plantar fasciosis include:9,10
• Plantar fasciosis involves various syndromes causing pain in the plantar fascia
• Disorders such as rheumatoid arthritis and psoriatic arthritis; obesity may be associated with this condition
• Pain at the bottom of the heel worsens with weight bearing, especially upon pushing off at the heel
• Initial treatment should be with in-shoe heel and arch cushioning, calf-stretching exercises, and splinting devices worn at night
• A newer treatment for recalcitrant types of plantar fasciosis is called extracorporeal pulse activation therapy (EPAT). This modality delivers low-frequency pulse waves locally via a handheld applicator; this is a safe, noninvasive technique that stimulates metabolism and enhances blood circulation, thus assisting in the regeneration of damaged tissue and accelerating healing.
TABLE 1 discusses this condition and other selected heel and back-of-the-foot problems encountered by older adults, including inferior calcaneal bursitis, Achilles tendon enthesopathy and Achilles tendon bursitis.
A pharmacist’s referral for podiatric assessment may assist in addressing whether a foot problem may be having an impact on the patient’s functional ability. Referral to a healthcare provider is necessary when there is pain in the heel around the Achilles tendon that becomes worse with activity.11
Achilles Rupture: Quinolones
The Achilles tendon connects the calf muscles to the calcaneus. Patients with an Achilles tendon rupture often present with complaints of a sudden snap in the lower calf associated with acute, severe pain.12 Rupture of the Achilles tendon and other tendon sites (rotator cuff, biceps) has been reported with quinolone antibiotics. Pharmacists should be aware of the potential for increased risk among patients >60 years of age, those with concurrent corticosteroid use, and among solid-organ transplant recipients.5 Independent risk factors for tendinitis may include renal impairment, rheumatoid arthritis, and strenuous physical activity. Of note, inflammation and rupture may occur bilaterally; cases have been reported within the first 48 hours, during, and up to several months after discontinuation of therapy.5
Obesity: Functional Ability and Pain
Each step an individual takes exerts a force upon the feet that is about 50% greater than the person’s body weight.1 Obesity may exacerbate foot discomfort and pain by adding to the tremendous force that each step contains. Obesity not only contributes to a variety of medical problems that are commonly seen in the elderly, including arthritis and gout, but may also make physical rehabilitation and the independent performance of ADL difficult.13 Functional ability may be especially impaired in morbidly obese seniors with cognitive impairment and MCCs such as heart failure or chronic obstructive pulmonary disease (COPD).13
Conclusion: Maintaining Mobility
Retaining the ability to be mobile is an important factor in an older adult’s ability to remain a vital part of society.14 As one ages, the ability to retain ambulation is directly related to foot health. When ambulation is impaired secondary to local foot problems and focal complications of systemic diseases, active seniors can be transformed into individuals who become dependent on family and other caregivers. Interventions aimed at sustained mobility often enable older adults to maximize their independence and the ability to socialize. Of note, falling, especially recurrent falling, is an indication that health and function are failing in older adults.15 Pharmacists, whether being approached for advice or actively identifying a foot problem associated with pain, can provide guidance regarding pharmacologic and lifestyle interventions to ameliorate pain and help improve functional ability.
REFERENCES
1. The New York Times. Foot pain in-depth report. www.nytimes.com/health/guides/symptoms/foot-pain/print.html. Accessed May 6, 2015.
2. McIntosh I. The vulnerable ageing foot. GM. www.gmjournal.co.uk/gm/default.aspx. April 2014:12-15.
3. Medscape.com. Evaluating foot pain in elderly patients. 2008. www.medscape.org/viewarticle/583760. Accessed May 6, 2015.
4. Bruckenthal P. Pain in the older patient. In: Fillit HM, Rockwood K, Woodhouse K, eds. Brocklehurst’s Textbook of Geriatric Medicine and Gerontology. 7th ed. Philadelphia, PA: Saunders Elsevier; 2010:965-972.
5. Semla TP, Beizer JL, Higbee MD. Geriatric Dosage Handbook. 19th ed. Hudson, OH: Lexicomp; 2014:934,1368.
6. Wrobel JS, Fleischer A, Crews RT, et al. A randomized controlled trial of custom foot orthoses for the treatment of plantar heel pain: a return to spontaneous physical activity. J Am Podiatr Med Assoc. May 5, 2015. [Epub ahead of print.]
7. Beers MH, Porter RS, Jones TV, et al. The Merck Manual of Diagnosis and Therapy. 19th ed. Whitehouse Station, NJ: Merck Research Laboratories; 2011:400-401.
8. U.S. National Library of Medicine. Plantar fasciitis. Updated March 8, 2014. http://www.nlm.nih.gov/medlineplus/ency/article/007021.htm. Accessed May 11, 2015.
9. Whitney KA. Plantar fasciosis (plantar fasciitis). Updated October 2014. www.merckmanuals.com/professional/musculoskeletal-and-connective-tissue-disorders/foot-and-ankle-disorders/plantar-fasciosis. Accessed May 19, 2015.
10. Gollwitzer H, Saxena A, DiDomenico LA, et al. Clinically relevant effectiveness of focused extracorporeal shock wave therapy in the treatment of chronic plantar fasciitis: a randomized, controlled multicenter study. J Bone Joint Surg Am. 2015;97(9):701-708.
11. U.S. National Library of Medicine. MedlinePlus. Achilles tendinitis. Updated August 11, 2012. www.nlm.nih.gov/medlineplus/ency/article/001072.htm. Accessed May 11, 2015.
12. Saglimbeni AJ, Fulmer CJ. Achilles tendon injuries. Medscape.com. Updated June 3, 2014. http://emedicine.medscape.com/article/309393-overview. Accessed May 11, 2015.
13. Zagaria ME. Obesity: reality and relevance to health. US Pharm. 2009;34(9):20-24.
14. Helfand AE. Primary considerations in managing the older patient with foot problems. In: Halter JB, Ouslander JG, Tinetti ME, et al, eds. Hazzard’s Geriatric Medicine and Gerontology. 6th ed. New York, NY: McGraw-Hill; 2009:1479-1490.
15. Studenski SA. Falls. In: Fillit HM, Rockwood K, Woodhouse K, eds. Brocklehurst’s Textbook of Geriatric Medicine and Gerontology. 7th ed. Philadelphia, PA: Saunders Elsevier; 2010:901-902.
16. Chu NK, Lew HL, Chen CP. Ultrasound-guided injection treatment of retrocalcaneal bursitis. Am J Phys Med Rehabil. 2012;91(7):635-637.
17. Foye PM, Rispoli L, Patibanda V. Retrocalcaneal bursitis. Medscape. Updated November 26, 2014. http://emedicine.medscape.com/article/86297-overview. Accessed May 19, 2015.
18. Whitney KA. Inferior calcaneal bursitis. Last full review/revision October 2014. www.merckmanuals.com/professional/musculoskeletal-and-connective-tissue-disorders/foot-and-ankle-disorders/inferior-calcaneal-bursitis. Accessed May 19, 2015.
19. Whitney KA. Achilles tendon enthesopathy. Last full review/revision October 2014. http://www.merckmanuals.com/professional/musculoskeletal-and-connective-tissue-disorders/foot-and-ankle-disorders/achilles-tendon-enthesopathy. Accessed May 19, 2015.
20. Whitney KA. Anterior achilles tendon bursitis (Albert disease; retromalleolar bursitis). Last full review/revision October 2014. www.merckmanuals.com/professional/musculoskeletal-and-connective-tissue-disorders/foot-and-ankle-disorders/anterior-achilles-tendon-bursitis. Accessed May 19, 2015.
21. Whitney KA. Posterior achilles tendon bursitis. Last full review/revision October 2014. www.merckmanuals.com/professional/musculoskeletal-and-connective-tissue-disorders/foot-and-ankle-disorders/posterior-achilles-tendon-bursitis. Accessed May 19, 2015.
To comment on this article, contact rdavidson@uspharmacist.com.





