ABSTRACT: Organ transplantation has become a well-known treatment in end-stage organ failure. Although organ transplantation is now a routine medical procedure in many countries, patients and their families still face challenges before, during, and after the process; the emotional aspects may be underestimated. Overall, an estimated 50% of transplant patients experience at least one episode of substantial anxiety or depression within the first 2 years post transplantation. Posttransplant depression may impact adherence to treatment. The treatment of depression may sometimes be complex owing to the potential of multiple drug interactions with posttransplant drugs and complex drug regimens. In general, the most commonly prescribed antidepressants for transplant patients are the selective serotonin reuptake inhibitors.
US Pharm. 2017;42(4)(Specialty & Oncology suppl):Epub.
Organ transplantation has become a well-known treatment in end-stage organ failure. In 2016, more than 33,600 organ transplants were performed in the United States, which represented an 8.5% increase from 2015.1 Although organ transplantation is now a routine medical procedure in many countries, patients still face many challenges before, during, and after the process.2 Generally, when thinking about organ transplants, people tend to focus on the physical challenges of the illness itself, the transplant procedure, and the recovery process. They may be less likely to take into consideration the psychological challenges and emotional toll this life-changing surgery can have on patients and their families.
Transplant patients and their families are often faced with emotional trials before, during, and after the transplant process. According to the American Psychological Association, an estimated 50% of transplant patients experience at least one episode of substantial anxiety or depression within the first 2 years of the posttransplant period.3 Symptoms of posttraumatic stress disorder (PSTD) are also prevalent, with one study reporting nearly 25% of transplant patients displaying PTSD symptoms.4
Because organ transplantation is a serious and life-altering surgery, it is critical that the patient and the patient’s family understand the long-term compliance necessary to improve patient outcomes, as well as the surgical risks involved.5 The United Network for Organ Sharing (UNOS) mandates a psychological assessment for transplant patients before they are added to the transplant list.5 The psychosocial evaluation is used to assess the patient’s understanding of the procedure itself as well as the patient’s acceptance of the requirements for maintaining a positive surgical outcome, such as compliance with immunosuppressive therapy, laboratory tests, and routine office visits to transplant healthcare providers.5
In addition, the psychosocial evaluation usually includes an assessment of the support person who will be the primary caregiver for the transplant patient after the surgery. Since the primary caregiver role requires a considerable time commitment, the psychosocial evaluation enables the clinician to assess whether the primary caregiver is aware of and accepts the commitments essential for the care of the transplant patient.5
Depression and anxiety disorders may manifest during the transplant process owing to psychosocial factors, medications, and physiological disturbances.6,7 Mood and anxiety disorders may occur in organ-transplant candidates—as many as 25% of patients with advanced pulmonary disease, 40% of patients with advanced hepatic disease, and 50% of patients with advanced cardiac disease—as well as in posttransplant patients, with up to 20% of kidney recipients, 30% of liver recipients, and 63% of heart recipients affected, especially in the first year.7 A systematic review and meta-analysis, conducted by Dew and colleagues, of studies that examined whether depression and anxiety impacted mortality risk after transplant concluded that there was a 65% increased risk of mortality with depression; however, anxiety did not show a significant association.8 Results of research examining whether depression or anxiety predicts transplant-related outcomes are mixed.8,9
Psychosocial Factors
A retrospective study involving 47,889 subjects based upon Medicare claims reported collective incidences of depression of 5%, 7.3%, and 9.1% at 1, 2, and 3 years post renal transplant, respectively.10 Diabetes, female gender, obesity, and younger age at time of transplantation (age <65 years) were linked to greater rates of depression.10 In other studies, patients without a regular income, those who lived alone, those without a support system, those who did not receive the desired organ transplant, and those who experienced a rejection episode were more likely to develop depression.11,12 Posttransplant complications, changes in family and caregiver dynamics, and the stress of the illness and hospitalizations may also contribute to depression and anxiety.7 Common psychosocial issues experienced by patients and families may be found in Table 1.13
Physiological Factors and Medications
Allograft rejection and complications of immunosuppressive therapy are a source of considerable stress and may contribute to depression and anxiety.14 Other contributing medical factors may include medication adverse effects, rapid taper of steroids, metabolic derangements, and central nervous system events.7 Medication-induced mood disturbances, especially depression, may be more frequently observed in the first year post transplantation; some illness-related psychiatric disorders may abate postoperatively.14 A 2007 study of depression in lung transplantation, as well as a 2015 meta-analysis of posttransplant depression and anxiety, found that depression symptoms may negatively influence the patient’s capacity to adjust during the posttransplant process, impacting adherence to rehabilitation and pharmacologic therapy, as well as quality of life.8,15
Coping
During the transplant process, psychological consultation can be beneficial since it may enable patients to develop coping strategies.2 Patients are sometimes directed to employ educational and supportive therapy, as well as cognitive-behavioral interventions.2
Studies have shown that early identification and initiation of treatment for depression are associated with improved outcomes.16,17 Transplant patients who are able to return to work after transplantation reported better quality of life and lower incidence of depression.18 Many clinicians would agree that the use of antidepressants represents the best-established treatment for patients with a diagnosis of depression; pharmacists are in a position to identify patients at risk for depression and to make clinical recommendations regarding available therapies.17,19
Drug Therapy in Organ-Transplant Patients
Successfully supporting transplant patients as they transition from hospital to home is of critical importance.20 Posttransplant patients must adhere to a challenging regimen that often includes taking as many as 20 medications daily to prevent rejection.21,22 This complex drug regimen can be intimidating and may cause anxiety and stress. Managing comorbid disease states in conjunction with these medication regimens can be overwhelming for patients and family members.20 Consequently, patient education is vital to improving adherence. Pharmacists are key in identifying other factors that may lead to depression, such as the adverse effects associated with the use of immunosuppressive medication, including high-dose glucocorticoid therapy and antihypertensive treatment with agents such as beta-blockers.20
Posttransplant Regimens
The typical posttransplant regimen may consist of antirejection medications and anti-infectives—including antibacterials, antifungals, and antivirals—as well as other medications needed to treat adverse effects of antirejection drugs, drugs for other medical conditions, or supplements as needed.20,22
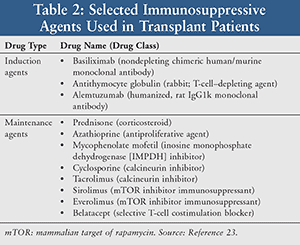
Immunosuppressive drugs (Table 2) may be classified as induction therapies and maintenance or antirejection therapies.23 Induction therapy is prescribed for intense early postoperative immune suppression; maintenance therapy is used throughout the patient’s life to prevent both acute and chronic organ rejection.23,24 Maintenance immunosuppressive therapies include small-molecule drugs such as calcineurin inhibitors and antiproliferatives, fusion proteins, and glucorticorticoids.23 There are also special agents including IV immunoglobulin, rituximab, leflunomide, eculizumab, and bortezomib.23 Induction immunosuppressive agents consist of depleting and non-depleting protein drugs (polyclonal and monoclonal antibodies).23 There is no consensus as to which immunosuppressive protocol is superior, and each transplant program has individualized protocols and employs various combinations of agents somewhat differently.
Unfortunately, the same medications that help improve transplant outcomes may cause or contribute adversely to other health conditions, such as diabetes, hypertension, and hyperlipidemia.22 Complicating matters more, up to 70% of transplant patients do not take their medications correctly, owing to difficulty keeping track of the medication regimen, lack of proper patient education about medications, and the high costs of the medications.22,24 These frustrations may contribute to anxiety and depression in transplant patients as well.
Antidepressant Medications
The antidepressants most commonly prescribed for transplant patients are the selective serotonin reuptake inhibitors (SSRIs) such as citalopram, escitalopram, fluoxetine, paroxetine, sertraline, and vilazodone.25-27 Because of adverse effects and potential for drug interactions, tricyclics and monoamine oxidase inhibitors are rarely used in posttransplant patients.25 In addition to SSRIs, serotonin-norepinephrine reuptake inhibitors (SNRIs) are commonly prescribed in this patient population, mainly because of their relative lack of adverse effects and their high therapeutic index.25-27
Patients should be monitored for the possibility of drug interactions between SSRIs/SNRIs and immunosuppressant medications.25-27 Particular caution should be taken with the use of fluoxetine and paroxetine, both of which inhibit the CYP4503A4 enzyme metabolism of the calcineurin inhibitors (cyclosporine and tacrolimus) and the mammalian target of rapamycin (mTOR) inhibitor sirolimus, thereby increasing their plasma concentrations when coadministered.26 Citalopram, escitalopram, sertraline, venlafaxine, mirtazapine and bupropion appear to have fewer adverse effects on CYP4503A4 and consequently would not be expected to extensively modify metabolism of these immunosuppressants.26
Results of one study involving transplant patients with depression revealed that 92% were taking an antidepressant medication (79% SSRIs; 8% SNRIs; the remainder were taking other antidepressants); 8% also received psychotherapy weekly.17
Role of the Pharmacist
Pharmacists play a major role in the multidisciplinary transplant team. In the U.S., UNOS administers the Organ Procurement and Transplantation Network; it is responsible for setting standards for all U.S. transplant programs, and it requires that all transplant programs identify at least one pharmacist to be accountable for providing pharmaceutical care to solid-organ transplant recipients.28
Pharmacists have an integral role in monitoring drug therapy, given that transplant patients generally have complex drug regimens. Transplant clinical pharmacists have expertise in patient education, detecting major drug adverse events and interactions, and in developing strategies to improve adherence to immunosuppressants, antimicrobials, and other essential posttransplant medications.28
Because numerous drug-drug interactions are associated with antirejection medications, pharmacists are key in identifying drug-drug interactions in posttransplant patients. For example, calcineurin inhibitors (tacrolimus and cyclosporine) and mTOR inhibitors (sirolimus and everolimus) are substrates of CYP isoenzyme 3A and P-glycoprotein and are subject to several drug interactions with commonly used posttransplant medications.28 Additionally, pharmacists should monitor for interactions with anti-infectives, protease inhibitors, statins, psychiatric medications, antiseizure medications, and some antihypertensive agents as well.28 It is also important to note that patients should be monitored for mental status changes such as alterations in behavior, mood swings, and depression that may manifest because of the use of immunosuppressants such as prednisone, cyclosporine, and tacrolimus; these may adversely affect patients, particularly those with preexisting mental-health issues.28
Pharmacists can be a source of information and support for transplant patients with regard to proper administration and storage of medications, as well as counseling on potential adverse effects. Pharmacists can provide tips for medication schedules, medication reminders, and reordering of medications. Pharmacists can also remind patients to wear a MedicAlert bracelet indicating that they are transplant recipients and to always maintain a current list of all medications. Through patient education, pharmacists and other clinicians on the transplant team can help patients understand what to expect before, during, and after the transplant process. They can also ease patients’ fears and stresses and provide them with pertinent information (see Resources) as they heal and recover not only physically, but also emotionally, from this life-altering process.25,29-32
Conclusion
Depression is treatable, and early identification and treatment of patients experiencing the symptoms of this disorder can greatly improve quality of life and reestablish more normal functioning in daily routines. With support and empathy from their healthcare providers, transplant patients and their family members can start a new chapter with the knowledge that there is a team of clinicians working together to improve their overall quality of life. Patients should be encouraged to be active team players and to always discuss issues of concern with their transplant team, including symptoms of depression and anxiety, since they may impact patient outcomes.
REFERENCES
1. United Network for Organ Sharing. U.S. organ transplants, decreased donors set record in 2016. January 9, 2017. www.unos.org/us-organ-transplants-set-record-in-2016/. Accessed October 12, 2017.
2. Schulz K. Kroencke S. Psychosocial challenges before and after organ transplant. Transplant Res Risk Manage. 2015;7:45-58.
3. Colis I, Burroughs A, Rolles K, Lloyd G. Psychiatric and social outcome of liver transplantation. Br J Psychiatry;1995;166(4):521-524.4. Rothenhäusler HB, Ehrentraut S, Kapfhammer HP, et al. Psychiatric and psychosocial outcome of orthotopic liver transplantation. Psychother Psychosom, 2002;71:285-297.
5. National Register of Health Service Psychologists. Organ transplantation issues in assessment and treatment. www.nationalregister.org/pub/the-national-register-report-pub/the-register-report-spring-2010/organ-transplantation-issues-in-assessment-and-treatment/. Accessed October 12, 2017.
6. Crone CC, Gabriel GM. Treatment of anxiety and depression in transplant patients: pharmacokinetic considerations. Clin Pharmacokinet. 2004;43(6):361-394.
7. DiMartini A, Crone C, Fireman M, Dew MA. Psychiatric aspects of organ transplantation in critical care. Crit Care Clin. 2008;24(4):949-981.
8. Dew MA, Rosenberger EM, Myaskovsky L, et al. Depression and anxiety as risk factors for morbidity and mortality after organ transplantation: a systematic review and meta-analysis. Transplantation. 2015;100(5):988-1003.
9. Corruble E, Barry C, Varescon I, et al. Report of depressive symptoms on waiting list and mortality after liver and kidney transplantation: a prospective cohort study. BMC Psychiatry. 2011;11:182.
10. Dobbels F, Skeans MA, Snyder JJ, et al. Depressive disorder in renal transplantation: analysis of Medicare claims. Am J Kidney Dis. 2008;51:819-828.
11. Tsunoda T, Yamashita R, Kojima Y, Takahara S. Risk factors for depression after kidney transplantation. Transplant Proc. 2010;42(5):1679-1681.
12. Jana AK, Sircar D, Waikhom R, et al. Depression and anxiety as potential correlates of post-transplantation renal function and quality of life. Indian J Nephrol. 2014;24(5):286-290.3. Dew MA, Manzetti J, Goycoolea JR, et al. Psychosocial aspects of transplantation. Medscape. June 17, 2002. www.medscape.com/viewarticle/436541. Accessed October 12, 2017.
14. Kalra G, Desousa A. Psychiatric aspects of organ transplantation. Int J Organ Transplant Med. 2011;2(1):9-19.
15. Fusar-Poli P, Lazzaretti M, Ceruti M, et al. Depression after lung transplantation: causes and treatment. Lung. 2007;185(2):55-65.
16. Kupfer DJ, Frank E, Perel JM. The advantage of early treatment intervention in recurrent depression. Arch Gen Psychiatry. 1989;46(9);771-775.
17. Okwuosa I, Pumphrey D, Puthumana J, et al. Impact of identification and treatment of depression in heart transplant patients. Cardiovasc Psychiatry Neurol. 2014; 2014:747293.
18. White-Williams C, Wang E, Rybarczyk B, Grady KL. Factors associated with work status at 5 and 10 years after heart transplantation. Clin Transplant. 2011;25(6):E599-E605. Accessed October 12, 2017.
19. Fournier JC, DeRubeis RJ, Hollon SD, et al. Antidepressant drug effects and depression severity: a patient-level meta-analysis. JAMA. 2010;303(1):47-53.
20. Vella J. Psychiatric aspects of organ transplantation. UpToDate. March 20, 2017. www.uptodate.com/contents/psychiatric-aspects-of-organ-transplantation#H2.
21. de la Vega A, Luong D. Post-transplant patient education and medication adherence. Texas Kidney Foundation. April 28, 2017. http://txkidney.org/wp-content/uploads/2017/03/Post-Transplant-Patient-Education-and-Compliance-v.pdf?x15235.
22. Berry Z. Organ transplant specialized pharmacies; providing care to improve adherence and outcomes. Specialty Pharmacy Times. December 17, 2013. www.specialtypharmacytimes.com/publications/specialty-pharmacy-times/2013/nov_dec-2013/organ-transplant-specialized-pharmacies-providing-patient-care-to-improve-adherence-and-outcomes. Accessed October 12, 2017.
23. Pellegrino B. Immunosuppression. Medscape. Updated January 4, 2016. http://emedicine.medscape.com/article/432316-overview#a5. Accessed October 12, 2017.
24. Tschida S, Aslam S, Khan TT, et al. Managing specialty medication services through a specialty pharmacy program: the case of oral renal transplant immunosuppressant medications. J Manage Care Pharm. 2013;19(1):26-41.
25. Mullish BH, Kabir MS, Thursz MR, Dhar A. Review article: depression and the use of antidepressants in patients with chronic liver disease or liver transplantation. Aliment Pharmacol Ther. 2014;40(8):880-892.
26. Rogal SS, Dew MA, Fontes P, DiMartini AF. Early treatment of depressive symptoms and long-term survival after liver transplantation. Am J Transplant. 2013;13:928-935.
27. Surman OS, Cosimi AB, DiMartini A. Psychiatric care of patients undergoing organ transplantation. Transplantation. 2009;87:1753-1761.
28. Wiegel JJ, Olyaei AJ. The role of the pharmacist in the management of kidney transplant recipients. Ind J Urol. 2016;32(3):192-198.
29. U.S. Department of Health and Human Services. Partnering With Your Transplant Team: The Patient’s Guide to Transplantation. Rockville, MD: Health Resources and Services Administration, Healthcare Systems Bureau, Division of Transplantation; 2008. www.unos.org/wp-content/uploads/unos/PartneringWithTransplantTeam.pdf. Accessed October 12, 2017.
30. United Network for Organ Sharing. UNOS Transplant Living. https://transplantliving.org/index.php. Accessed October 12, 2017.
31. LifeLink.org. Organ donation. www.lifelinkfoundation.org/organ-donation/. Accessed October 12, 2017.
32. Organdonor.gov. U.S. Government information on organ donation and transplantation. https://organdonor.gov/index.html. Accessed October 12, 2017.
To comment on this article, contact rdavidson@uspharmacist.com.