US Pharm. 2020;45(1):25-29.
ABSTRACT: Falls in geriatric patients cost the United States billions of dollars each year and contribute to morbidity and mortality in this population. Polypharmacy can significantly contribute to the fall risk, especially those medications that are on the Beers Criteria list. Skeletal muscle relaxants are on this list, and an increased risk of falls is associated with their use. These medications are inappropriately used as an alternative to conventional pain medications and can be as harmful as opioids in the geriatric population. Education of patients and prescribers is necessary in order to prevent inappropriate muscle-relaxant use and to lessen the risk of falls.
In the United States, an estimated 29 million falls occurred in 46 million people older than age 65 years in 2014, and 7 million of those falls resulted in injuries.1 In 2015, estimated medical costs related to fatal and nonfatal falls totaled more than $49 billion.2 It is estimated that the U.S. geriatric population will increase to 74 million in 2030, and 49 million falls are predicted (with 12 million of these falls incurring injuries).1 Well-known risk factors for falls in geriatric patients are polypharmacy and adverse effects of medications. Community pharmacists are uniquely positioned to reduce costs related to falls and increase patient safety by scrutinizing prescriptions for high-risk medications before these drugs are given to their patients. One class of medications with the potential for inappropriate prescribing in geriatric patients is skeletal muscle relaxants. Most skeletal muscle relaxants appear in both the National Committee for Quality Assurance’s list of high-risk medications in the elderly and the Beers Criteria list of potentially inappropriate medications in older adults.3,4 In 2017, cyclobenzaprine, diazepam, tizanidine, baclofen, and carisoprodol appeared on the top-200 list of medications dispensed to patients.5
Although these medications may be useful for treating acute low back pain, evidence for safe and effective prolonged use is limited.6,7 These agents may be inappropriately prescribed on a long-term basis, as an alternative to opioids or nonsteroidal anti-inflammatory drugs (NSAIDs), based on a mistaken belief that they are safer. Carisoprodol and diazepam are the only skeletal muscle relaxants that carry a risk of addiction, but all of them have some risk of central nervous system depression, which can be problematic in geriatric patients.7-9
Types of Skeletal Muscle Relaxants
Skeletal muscle relaxants, also called muscle relaxers, may be divided into two classes: antispasmodics and antispastics. Antispasmodics are agents that specifically treat muscle spasms. Muscle spasm occurs as a result of injury to muscles, tendons, or ligaments and is often synonymous with low back sprain or strain.10,11 Antispastics (sometimes referred to as spasmolytics) are agents that specifically treat muscle spasticity. Muscle spasticity is a condition in which the patient experiences continuous muscle spasms as a result of spinal motor neuron overactivity. This overexcitation manifests as clonus; stiffness; rigidity and tightness; and difficulty with walking, movement, and, occasionally, talking.12,13 A systematic review of studies on leg spasticity epidemiology reported a prevalence of 28% to 38% in stroke patients, 41% to 66% in multiple sclerosis patients, and 13% in patients with traumatic brain injury.13 TABLE 1 highlights key differences between antispasmodic and antispastic agents. A summary of available antispasmodics and antispastics is presented in TABLE 2.
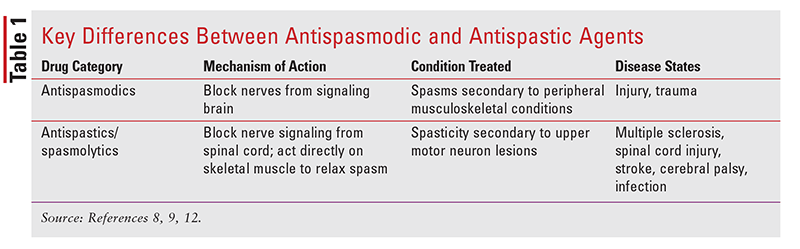
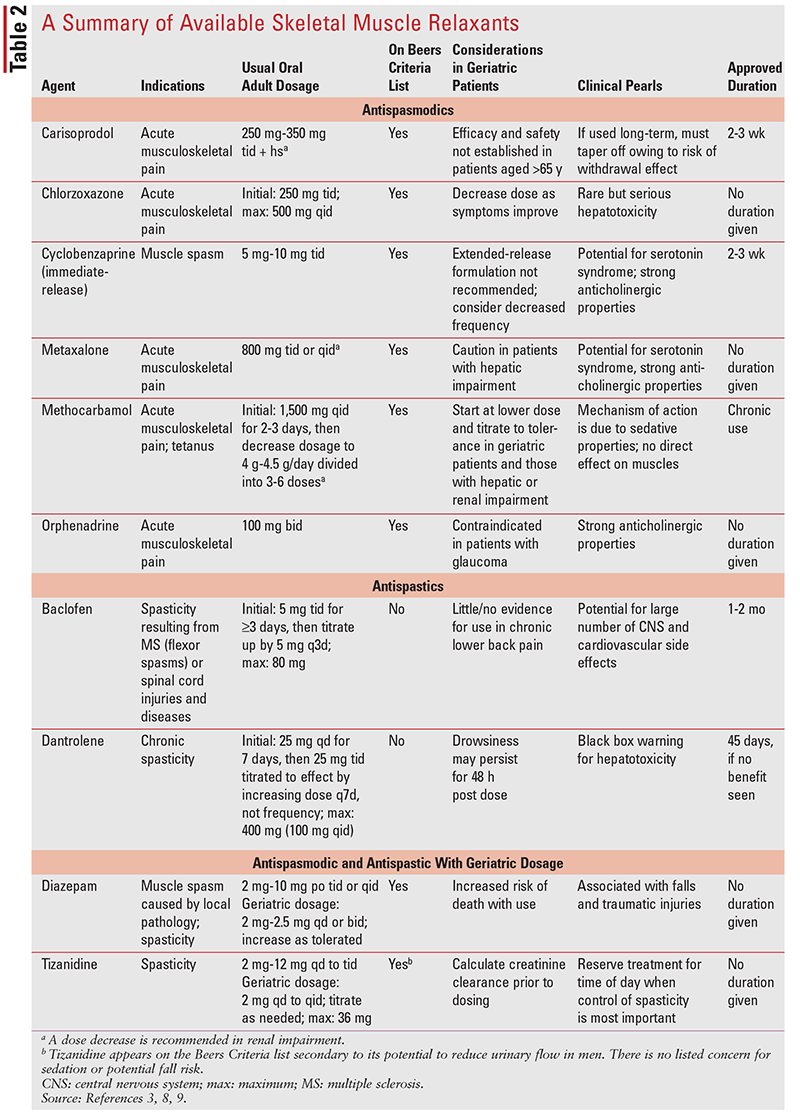
According to the American College of Physicians (ACP), first-line therapy for acute low back pain (pain lasting <4 wk) consists of nonpharmacologic measures such as stretching, heat, and physical therapy. Antispasmodics, antispastics, and NSAIDs are all considered second-line therapy.14 Patient characteristics will influence the drug choice. Unlike NSAIDs, however, skeletal muscle relaxants do not have any disease-modifying properties for low back pain and provide only symptomatic improvement.14 Chronic use of these medications is not recommended because little to no data exist on their safety and efficacy with long-term use.6 The ACP does not recommend skeletal muscle relaxants in patients with chronic low back pain (pain lasting >12 wk) because of a lack of efficacy and safety data.14
The Geriatric Lexi-Drugs database recommends the avoidance of muscle relaxants other than diazepam and tizanidine in patients older than age 65 years because efficacy and safety have not been established in geriatric patients.9 However, all muscle relaxants, including tizanidine and diazepam, are on the Beers Criteria list.3
Potential for Harm in Geriatric Patients
Because antispastics and antispasmodics work within the central nervous system, their side effects can pose a unique risk for geriatric patients. Compared with the average adult, geriatric patients are at increased risk for falls because of unsteady gait, loss of coordination or muscle strength, and other age-related declines in mobility and cognition. Common side effects of antispastic and antispasmodic medications include dizziness, drowsiness, and hypotension; therefore, a geriatric patient’s risk for falls and fractures can increase when skeletal muscle relaxants are used. One study showed that geriatric patients who took muscle relaxants were 2.25 times more likely to visit the emergency department for a fall or fracture and 1.56 times more likely to be hospitalized for a fall or fracture than patients who did not take these medications.15 Another study found that skeletal muscle relaxant users older than age 65 years were 1.32 times more likely to have an injury than patients who did not use skeletal muscle relaxants. More specifically, patients who took carisoprodol, cyclobenzaprine, and methocarbamol, respectively, were 1.73 times, 1.22 times, and 1.42 times more likely to have experienced injury compared with patients without a history of skeletal muscle relaxant use.16
Possible Alternative Therapies
There are several alternative therapies to skeletal muscle relaxants, depending on the reason for use. TABLE 3 gives a summary of possible alternatives.17 For patients with lower back pain, it is important to understand that most pain resolves on its own and does not require medical treatment. Nonpharmacologic therapies such as superficial heat, transcutaneous electrical nerve stimulation, and massage may be employed, along with rest.14,18 If pharmacologic therapy is deemed appropriate, ibuprofen may be used instead of skeletal muscle relaxants in patients without heart failure, renal dysfunction, or a history of gastrointestinal issues.19 Recommendations for ibuprofen should be made cautiously in patients with cardiovascular history because of potential drug-disease interactions.6 Bleeding risk should also be evaluated because older adults have an increased risk of gastrointestinal bleeds.20 The patient’s profile should be assessed prior to initiation, with particular attention paid to aspirin, clopidogrel, warfarin, and factor Xa inhibitors.21 Recommendation of a trial of short-term pharmacologic therapy on an as-needed basis, along with nonpharmacologic options and physical therapy, can reduce polypharmacy and increase positive health outcomes in many patients.

Guidelines from the National Institute for Health and Care Excellence (NICE) for the management of multiple sclerosis, the most common cause of spasticity, recommend physical therapy for the management of spasticity in all patients. Pharmacotherapy is recommended only when spasticity causes pain, significant discomfort, loss of independence, or limitations in activities.13 For patients who experience adverse effects with muscle relaxants, it may be beneficial to discuss alternative options, such as physical therapy, physiotherapy, or as-needed dosing with a muscle relaxant. Patients should be educated about the potential for falls and other adverse events and encouraged to weigh the pros and cons of taking a skeletal muscle relaxant. Another option to reduce medication burden, and therefore reduce fall risk, would be to tailor therapy to the time of day that muscle relaxation is needed. Patients often do not need medication when walking and being active, but they may require relaxation when going to bed because changing positions can aggravate spasticity. The first-line therapy (baclofen) and one second-line therapy (dantrolene), according to the NICE guidelines, are not on the Beers Criteria list, but both medications can increase the risk of falls.13 Tizanidine, the other second-line therapy, is on the Beers list owing to potential urinary retention, and it can also increase the risk of falls.3,12
The Pharmacist’s Role
Community pharmacists spend a significant amount of time ensuring that their patients receive medications that are both safe and effective for their medical conditions. Often, this involves contacting the prescriber after receiving a new prescription to verify the drug choice or dosing information. Pharmacists use clinical judgment every day to determine whether interventions necessitate calling the provider or counseling the patient. By educating patients and prescribers on the alternative pharmacologic and nonpharmacologic therapeutic options to skeletal muscle relaxants, the use of these medications can be drastically reduced. Also, patients should be educated on the risks associated with muscle relaxants, particularly falls.
If an older patient has a genuine need for one of these high-risk medications, it is important that the duration of medication use be kept as short as possible. Patients should also be educated about nonpharmacologic measures that can help prevent falls.22 Patients with vision difficulties should avoid areas that are not well lit and should remove any tripping hazards, including rugs.23 Assistive devices, particularly those with nonskid rubber ends, should be used if the patient feels unsteady while walking.24 While taking skeletal muscle relaxants, patients should be particularly careful to avoid ingesting alcohol because coadministration increases the risk of central nervous system depression and falls.8
Conclusion
Skeletal muscle relaxants are a sedating class of medications used to treat spasticity and pain. Their sedative properties can pose a risk for geriatric patients who are predisposed to falls. It is important for the pharmacist to assess the patient before dispensing medications. Short-term use of skeletal muscle relaxants may be appropriate for certain conditions but should not be used long-term, regardless of interaction. Alternative pharmacologic options exist, but most have drawbacks. Nonpharmacologic therapy may be a better option in both the short term and the long term. Nonpharmacologic education on fall prevention is essential in patients being given skeletal muscle relaxants, regardless of duration of therapy. Not only will appropriate use of skeletal muscle relaxants improve patient outcomes, it can also improve star ratings for both insurance providers and pharmacies.
REFERENCES
1. CDC. Take steps to prevent older adult falls. www.cdc.gov/steadi/pdf/STEADI_ClinicianFactSheet-a.pdf. Accessed October 1, 2019.
2. Florence CS, Bergen G, Atherly A, et al. Medical costs of fatal and nonfatal falls in older adults. J Am Geriatr Soc. 2018;66:693-698.
3. 2019 American Geriatrics Society Beers Criteria® Update Expert Panel. American Geriatrics Society 2019 updated AGS Beers Criteria® for potentially inappropriate medication use in older adults. J Am Geriatr Soc. 2019;67:674-694.
4. National Committee for Quality Assurance. HEDIS 2019 final NDC lists. www.ncqa.org/hedis/measures/hedis-2019-ndc-license/hedis-2019-final-ndc-lists. Accessed August 25, 2019.
5. Kane SP. The top 200 drugs of 2019. ClinCalc DrugStats Database, Version 19.1. https://clincalc.com/DrugStats. Accessed September 12, 2019.
6. Chou R, Qaseem A, Snow V, et al. Diagnosis and treatment of low back pain: a joint clinical practice guideline from the American College of Physicians and the American Pain Society. Ann Intern Med. 2007;147:478-491.
7. University of Illinois at Chicago, Drug Information Group. Muscle relaxers: a list of prescription medications. Healthline. www.healthline.com/health/muscle-relaxers. Accessed October 1, 2019.
8. Clinical Pharmacology [online database]. Tampa, FL: Elsevier/Gold Standard; 2019. www.clinicalpharmacology.com. Accessed September 24, 2019.
9. Geriatric Lexi-Drugs [online database]. Riverwoods, IL: Lexicomp, Inc. http://online.lexi.com. Accessed September 28, 2019.
10. Roland J. Understanding and treating lower back spasms. Healthline. www.healthline.com/health/back-pain/lower-back-spasms. Accessed October 1, 2019.
11. Engstrom JW. Back and neck pain. In: Jameson JL, Fauci AS, Kasper DL, et al, eds. Harrison’s Principles of Internal Medicine. 20th ed. New York, NY: McGraw Hill Education; 2018.
12. Cleveland Clinic. Spasticity. https://my.clevelandclinic.org/health/diseases/14346-spasticity. Accessed October 1, 2019.
13. Nair KPS, Marsden J. The management of spasticity in adults. BMJ. 2014;349:g4737.
14. Qaseem A, Wilt TJ, McLean RM, et al. Noninvasive treatments for acute, subacute, and chronic low back pain: a clinical practice guideline from the American College of Physicians. Ann Intern Med. 2017;166:514-530.
15. Alvarez CA, Mortensen EM, Makris UE, et al. Association of skeletal muscle relaxers and antihistamines on mortality, hospitalizations, and emergency department visits in elderly patients: a nationwide retrospective cohort study. BMC Geriatr. 2015;15:2.
16. Spence MM, Shin PJ, Lee EA, Gibbs NE. Risk of injury associated with skeletal muscle relaxant use in older adults. Ann Pharmacother. 2013;47:993-998.
17. Humana. Medications to avoid in the elderly. http://apps.humana.com/marketing/documents.asp?file=3128346. Accessed October 1, 2019.
18. Chou R, Huffman LH. Nonpharmacologic therapies for acute and chronic low back pain: a review of the evidence for an American Pain Society/American College of Physicians clinical practice guideline. Ann Intern Med. 2007;147:492-504.
19. Hanlon JT, Semla TP, Schmader KE. Alternative medications for medications in the use of high-risk medications in the elderly and Potentially Harmful Drug–Disease Interactions in the Elderly quality measures. J Am Geriatr Soc. 2015;63:e8-e18.
20. Bhatt DL, Scheiman J, Abraham NS, et al. ACCF/ACG/AHA 2008 expert consensus document on reducing the gastrointestinal risk of antiplatelet therapy and NSAID use: a report of the American College of Cardiology Foundation Task Force on Clinical Expert Consensus Documents. J Am Coll Cardiol. 2008;52:1502-1517.
21. Hamrick JW, Nykamp D. Drug-induced bleeding. US Pharm. 2015;40(12):HS17-HS21.
22. Jeon MY, Jeong H, Petrofsky J, et al. Effects of a randomized controlled recurrent fall prevention program on risk factors for falls in frail elderly living at home in rural communities. Med Sci Monit. 2014;20:2283-2291.
23. Gillespie LD, Robertson MC, Gillespie WJ, et al. Interventions for preventing falls in older people living in the community. Cochrane Database Syst Rev. 2012;(9):CD007146.
24. National Institute on Aging. Prevent falls and fractures. www.nia.nih.gov/health/prevent-falls-and-fractures. Accessed November 27, 2019.
To comment on this article, contact rdavidson@uspharmacist.com.





