US Pharm. 2015;40(9):39-44.
ABSTRACT: Polycystic ovarian syndrome (PCOS), which is a complex disease, is the most common endocrine disorder affecting females of reproductive age. Left untreated, PCOS can increase the risk of various comorbidities, including obstructive sleep apnea, metabolic syndrome, hypertension, dyslipidemia, cardiovascular disease, glucose intolerance, and type 2 diabetes. PCOS is associated with menstrual disorders such as oligomenorrhea, amenorrhea, menorrhagia, and infertility, and it confers an increased risk of endometrial hyperplasia and carcinoma. Because patients with PCOS typically present with more than one medical issue, treatment often requires a multifaceted approach involving the use of pharmacologic agents and lifestyle and dietary modifications in order to effectively manage and treat the signs and symptoms of PCOS.
Polycystic ovarian syndrome (PCOS), also known as Stein-Leventhal syndrome, is considered the most prevalent endocrine disorder, affecting 5% to 10% of reproductive-age women (or, an estimated 5-7 million) in the United States.1-4 The clinical manifestations of PCOS vary from mild menstrual disorders to severe disturbances of reproductive and metabolic functions.3 The majority of PCOS patients are diagnosed in their 20s or 30s, but PCOS can affect young girls as well.4
COMORBIDITIES OF PCOS
The impact that PCOS has on a patient’s health and overall quality of life varies from patient to patient. Many PCOS patients commonly present with signs of hyperandrogenism and ovulatory dysfunction.3,5 PCOS is also associated with obesity (although not all patients with PCOS have weight problems), insulin resistance, menstrual disorders, and infertility.3,5
According to the PCOS Foundation, only 50% of women with PCOS have been diagnosed, and PCOS is responsible for approximately 70% of infertility problems.6 Moreover, if left untreated, insulin resistance—which occurs in 50% to 70% of women with PCOS—can result in several comorbidities, including metabolic syndrome, hypertension, dyslipidemia, cardiovascular disease (CVD), glucose intolerance, type 2 diabetes, obstructive sleep apnea (OSA), and endometrial cancer.1,7 Early diagnosis of PCOS is critical for affected patients, since the disorder is associated with an increased risk of these comorbidities.8
Common Comorbidities
Details of common comorbidities of PCOS are discussed in the following sections.
Insulin Resistance and Diabetes: Many PCOS patients are insulin-resistant. For this reason, the American College of Endocrinology and the American Association of Clinical Endocrinologists advocate diabetes screening by age 30 years in PCOS patients, whether obese or not.9 In patients at greater risk for diabetes, screening before age 30 years is frequently recommended, and patients who initially test negative for diabetes should be periodically reassessed throughout their lifetime.9,10
Endometrial Hyperplasia and Carcinoma: PCOS patients are at increased risk for endometrial hyperplasia and endometrial carcinoma.10 The chronic anovulation characteristic of PCOS results in constant endometrial stimulation by estrogen in the absence of progesterone; as a result, the risk of developing endometrial hyperplasia and carcinoma is augmented.10 The Royal College of Obstetricians and Gynaecologists (United Kingdom) recommends that progestogens be used for induction of withdrawal bleeding at least every 3 to 4 months in PCOS patients, when warranted, to prevent or minimize risks.10
Reproductive Disorders: During the reproductive years, there is a greater incidence of first-trimester miscarriage and pregnancy complications, such as gestational diabetes and pregnancy-induced hypertension, in females with PCOS.11,12
The menstrual disturbances usually observed in PCOS include oligomenorrhea, amenorrhea, and prolonged erratic menstrual bleeding.7,13 However, clinical studies indicate that some PCOS patients have normal monthly menses.7,13 An estimated 85% to 90% of females presenting with oligomenorrhea also have PCOS, and 30% to 40% of those with amenorrhea have PCOS.7,13
Hyperandrogenism: More than 80% of women presenting with symptoms of androgen excess also have PCOS.7 Hirsutism, a frequent clinical presentation of hyperandrogenism, occurs in an estimated 70% of PCOS patients.7
ETIOLOGY OF PCOS
Although the exact cause of PCOS is unknown, environmental and genetic factors have been implicated in the development of PCOS.14 Recent research conducted in animal models suggests that, in some cases, PCOS may be caused by genetic or chemical changes that occur in the womb.10,15 Research has also shown that PCOS patients typically have abnormalities in androgen and estrogen metabolization and in the control of androgen production.10-15
CLINICAL FEATURES OF PCOS
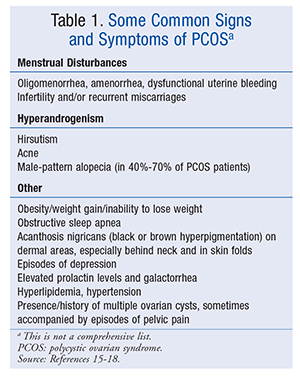
The major presenting features of PCOS include menstrual dysfunction, anovulation, and signs of hyperandrogenism.15 The intensity of symptoms will vary from patient to patient. Some common signs and symptoms of PCOS are given in TABLE 1.15-18
DIAGNOSING PCOS
In 2013, the Endocrine Society released a practice guideline for the diagnosis and treatment of PCOS.19 Highlights of the practice guideline include the following points:
• For diagnosing PCOS, the Rotterdam criteria should be used; i.e., at least two of the following clinical signs should be present: androgen excess, ovulatory dysfunction, and polycystic ovaries
• In adolescents with PCOS, hyperandrogenism is central to the presentation, and treatment options in the absence of contraindications include hormonal contraceptives and metformin
• Postmenopausal women do not have a consistent PCOS phenotype
• Alternative androgen-excess disorders and risk factors for CVD, diabetes, endometrial cancer, mood disorders, and OSA should be excluded
• Oral contraceptives (OCs) are first-line treatment for menstrual abnormalities and hirsutism/acne
• Clomiphene is first-line treatment for infertility in PCOS patients
• Metformin is beneficial for metabolic/glycemic abnormalities and for improving menstrual irregularities
• Metformin is of limited or no benefit for managing acne, hirsutism, or infertility
• More investigation is needed to determine the roles of weight loss and statins in PCOS19
There are several diagnostic guidelines for PCOS, all of which agree that three major factors should be considered for diagnosis: ovulatory dysfunction, ovarian morphology, and hyperandrogenism.20 The National Institutes of Health and the Androgen Excess Society criteria stress the critical nature of androgen excess in diagnosis, stating that this is a means of identifying those patients at greater risk for developing metabolic complications.20
PCOS TREATMENTS
Because PCOS patients typically present with more than one medical problem, a multifaceted approach is usually required to effectively manage and treat symptoms. Signs and symptoms include oligomenorrhea, hirsutism, insulin resistance, ovulatory infertility, OSA, weight problems, and risk factors for diabetes.18-20
According to the Endocrine Society’s practice guideline, general goals of selected therapy include elimination of hyperandrogenic signs such as hirsutism, acne, and alopecia; management of underlying metabolic abnormalities; reduction of risk factors for type 2 diabetes and CVD; and prevention of endometrial hyperplasia and carcinoma.19 Other goals include contraception (for those not wishing to conceive) and ovulation induction (for those pursuing pregnancy).19
Lifestyle Modifications
PCOS treatment typically starts with a proper diagnosis and implementation of certain lifestyle modifications, such as diet and exercise, which are first-line therapy for the majority of PCOS patients. However, in many cases, the use of pharmacologic agents is necessary to effectively treat and manage metabolic issues, anovulation, hirsutism, and menstrual irregularities.1,20 The American College of Obstetricians and Gynecologists (ACOG) and the Society of Obstetricians and Gynaecologists of Canada (SOGC) believe that lifestyle modifications such as weight loss and increased exercise, in conjunction with dietary modifications, decrease the incidence of diabetes.10 Various clinical studies have demonstrated that lifestyle modifications are comparable to or better than treatment with medication and should therefore be considered first-line treatment in managing PCOS.10,20 Lifestyle modifications have been effective in restoring ovulatory cycles and achieving pregnancy in obese women with PCOS.10,20 Weight loss also improves many hyperandrogenic features in obese women with PCOS.10
For many PCOS patients, lifestyle interventions such as dietary modifications and exercise also resulted in weight loss. To date, these interventions remain the foundation of effective long-term health improvement in PCOS patients who are overweight or obese.10,21
Drug Therapy
If drug therapy is warranted, selection of therapy is often based on the patient’s symptoms, medical history, age, and future pregnancy plans. Drugs used to treat PCOS include metformin (off-label use), spironolactone, eflornithine (topical cream for treating hirsutism), and OCs.10,22
First-line medical therapy usually includes the use of an OC to induce regular menses.20,22 OCs not only inhibit ovarian androgen production, but also increase production of sex hormone–binding globulin.10,22 The ACOG recommends the use of combination low-dose hormonal contraceptive agents for long-term management of menstrual dysfunction.10,22 OCs are often considered the mainstay of pharmacologic therapy for PCOS in terms of managing hyperandrogenism and menstrual dysfunction and providing contraception.10,22
Insulin-Sensitizing Agents
Insulin-sensitizing agents, such as metformin, are often used in PCOS patients. In the past two decades, metformin has been used off-label for PCOS.19,23 Clinical studies have shown that it is an effective ovulation agent for nonobese women with PCOS and offers some advantages over other first-line treatments for anovulatory infertility, such as clomiphene.10,19 The use of metformin is associated with increased regular cycles, improved ovulation, and a decrease in circulating androgen levels.19,20,23 Metabolic benefits associated with metformin are enhanced in the presence of weight loss, and weight loss itself may be increased by the use of metformin.23
Metformin’s primary clinical action is to inhibit hepatic glucose production, although it also decreases intestinal glucose uptake and increases insulin sensitivity in peripheral tissues.23 Metformin also improves ovulation induction in PCOS patients in a variety of ways, including reducing insulin levels and altering insulin’s effect on ovarian androgen biosynthesis, theca cell proliferation, and endometrial growth.23 In addition, metformin inhibits ovarian gluconeogenesis, thus reducing ovarian androgen production.23
Treatment of Androgen-Related Signs
The most common androgen-related signs associated with PCOS are acne, hirsutism, and alopecia.7 These signs vary in severity from woman to woman, but some patients present with only one or two of them, and a minority experience all three.
Eflornithine is a topical cream that can be used to slow hair growth.10 This agent works by inhibiting ornithine decarboxylase, which is essential for the rapidly dividing cells of hair follicles.10 Eflornithine used adjunctively with laser therapy is considered superior to laser therapy alone in treating hirsutism.10 Weight reduction decreases androgen production in women who are obese; therefore, weight loss may improve hirsutism as well.
Patients who do not want to become pregnant can be successfully treated for hirsutism with OCs.10 OCs slow hair growth in 60% to 100% of women with hyperandrogenemia.10 Prescribers often initiate therapy with a formulation containing a low dose of estrogen and a nonandrogenic progestin.10 Preparations containing norgestrel and levonorgestrel should be avoided because of their androgenic activity.10 Since there is a risk of thrombotic complications in obese women taking OCs, it is imperative to use caution when prescribing these agents to prevent such events.10
Other agents, such as antiandrogens (e.g., spironolactone), are also considered effective for treating hirsutism.10 Because of the potential teratogenic effects of spironolactone, it is important that PCOS patients taking this agent also use an effective form of contraception.10 Adverse effects of spironolactone include gastrointestinal discomfort and irregular menstrual bleeding, which can be managed by adding an oral contraceptive to prevent pregnancy.10
In addition, some patients may elect to use laser hair removal and other mechanical hair-removal products instead of pharmacologic agents, owing to the adverse effects of drugs.
Treatments for Infertility
Lifestyle changes such as losing weight can trigger bodily changes that facilitate conception in women with PCOS.24 In one study of 11 PCOS patients who had menstrual dysfunction and lost more than 5% of their initial weight, nine either became pregnant or experienced menstrual-cycle regulation.24,25
The ACOG and SOGC recommend clomiphene citrate as first-line therapy to stimulate ovulation when fertility is desired.26-28 For patients who are not responsive to clomiphene citrate, second-line therapy is exogenous gonadotropins or laparoscopic ovarian surgery.25,26 If gonadotropins are used, a low-dose regimen is recommended, and the patient should be monitored with ultrasonography and laboratory studies.25,26 Gonadotropin therapy is expensive, and its use is associated with an increased risk of multiple pregnancy and ovarian hyperstimulation syndrome.25
Clinical studies report that metformin improves ovulation rates and increases pregnancy rates in some PCOS patients, especially those who are obese.10
While clomiphene is the current first-line infertility treatment in women with PCOS, clinical studies indicate that aromatase inhibitors, including letrozole, might increase pregnancy outcomes.29 Letrozole transiently slows estrogen production and causes the body to make more follicle-stimulating hormone.21,28 Studies in animals have shown that letrozole causes birth defects if used during pregnancy, but to date there have been no studies in pregnant women.23,29 The National Institute of Child Health and Human Development is currently conducting research to compare the safety and effectiveness of letrozole with clomiphene for treating infertility related to PCOS.26
Surgical management of PCOS is aimed mainly at restoring ovulation. Ovarian wedge resection is no longer a commonly used method because of postoperative adhesion formation and the successful introduction of ovulation-inducing medications.26 However, various laparoscopic methods, including electrocautery, laser drilling, and multiple biopsies, have been used to create focal areas of damage in the ovarian cortex and stroma.10
CONCLUSION
PCOS is often underdiagnosed, but with the growing trend toward increasing awareness about this common endocrine disorder, more women are being diagnosed earlier. As a result, early treatment reduces or prevents the comorbidities associated with PCOS. It is imperative that all healthcare professionals, including pharmacists, be aware of the clinical signs of PCOS, because if it is not treated, PCOS can cause multiple long-term complications. Indeed, PCOS is a complex endocrine condition that often requires both the incorporation of lifestyle modifications and the implementation of pharmacologic agents to effectively manage its symptoms. While a standard treatment plan does not exist, clinicians should be familiar with the most common treatments to effectively manage PCOS. Since weight loss and diet modifications are pivotal components of PCOS control, patients should be encouraged to take an active role in their health and maintain routine follow-up medical care to enable their primary healthcare provider to monitor their progress, as well as to prevent long-term complications. Although currently there is no cure for PCOS, the promising news is that there are effective treatments for managing PCOS and reducing the serious complications that occur if it is untreated. Treatment of PCOS should be individualized to address the patient’s specific symptoms.
In working with patients struggling with the many facets of PCOS, healthcare professionals should stress the significance of adhering to the chosen treatment regimen to successfully manage PCOS, as well as provide these patients with the necessary information to make informed decisions about their health. Through patient education, increasing awareness, and ongoing investigation into the complexities of this syndrome, the millions of women affected by PCOS can improve their health and overall quality of life.
REFERENCES
1. National Institutes of Health. Evidence-based methodology workshop on Polycystic ovary syndrome. https://prevention.nih.gov/docs/programs/pcos/FinalReport.pdf. Accessed July 30, 2015.
2. PCOS Foundation. About PCOS Foundation—outreach. http://pcosfoundation.org/about. Accessed July 30, 2015.
3. Badawy A, Elnashar A. Treatment options for polycystic ovary syndrome. Int J Womens Health. 2011;3:25-35.
4. National Institute of Child Health and Human Development (NICHD). How many people are affected by PCOS? www.nichd.nih.gov/health/topics/PCOS/conditioninfo/Pages/risk.aspx. Accessed July 30, 2015.
5. Berger JJ, Bates GW Jr. Optimal management of subfertility in polycystic ovary syndrome. Int J Womens Health. 2014;6:613-621.
6. PCOS Foundation. What is PCOS? www.pcosfoundation.org/what-is-pcos. Accessed July 30, 2015.
7. Sirmans SM, Pate KA. Epidemiology, diagnosis and management of polycystic ovary syndrome. Clin Epidemiol. 2014;6:1-13.
8. PCOS Foundation. About polycystic ovarian syndrome. www.pcosfoundation.org/about-pcos. Accessed July 30, 2015.
9. Polycystic Ovary Syndrome Writing Committee. American Association of Clinical Endocrinologists position statement on metabolic and cardiovascular consequences of polycystic ovary syndrome. Endocr Pract. 2005;11:125-134.
10. Lucidi RS. Polycystic ovarian syndrome. Medscape. http://emedicine.medscape.com/article/256806-overview#aw2aab6b2b5. Accessed July 30, 2015.
11. NICHD. What is PCOS? www.nichd.nih.gov/health/topics/PCOS/conditioninfo/Pages/default.aspx#f2. Accessed July 30, 2015.
12. Womenshealth.gov. Polycystic ovary syndrome (PCOS) fact sheet: how does PCOS affect a woman while pregnant? www.womenshealth.gov/publications/our-publications/fact-sheet/polycystic-ovary-syndrome.html#i. Accessed July 30, 2015.
13. Pinkerton JV. Polycystic ovary syndrome (PCOS). www.merckmanuals.com/professional/gynecology-and-obstetrics/menstrual-abnormalities/polycystic-ovary-syndrome-pcos. Accessed July 30, 2015.
14. NICHD. What causes PCOS? www.nichd.nih.gov/health/topics/PCOS/conditioninfo/Pages/causes.aspx. Accessed July 30, 2015.
15. Goodarzi MO, Dumesic DA, Chazenbalk G, Azziz R. Polycystic ovary syndrome: etiology, pathogenesis and diagnosis. Nat Rev Endocrinol. 2011;7:219-231.
16. MedlinePlus. Polycystic ovary syndrome. www.nlm.nih.gov/medlineplus/ency/article/000369.htm. Accessed July 30, 2015.
17. Womenshealth.gov. Polycystic ovary syndrome (PCOS) fact sheet: what are the symptoms of PCOS? www.womenshealth.gov/publications/our-publications/fact-sheet/polycystic-ovary-syndrome.html#d. Accessed July 30, 2015.
18. Sheehan MT. Polycystic ovarian syndrome: diagnosis and management. Clin Med Res. 2004;2:13-27.
19. Legro RS, Arslanian SA, Ehrmann DA, et al. Diagnosis and treatment of polycystic ovary syndrome: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 2013;98:4565-4592.
20. Setji TL, Brown AJ. Polycystic ovary syndrome: update on diagnosis and treatment. Am J Med. 2014;127:912-919.
21. Barbieri RL. Polycystic ovary syndrome: diagnosis and management. NEJM Journal Watch. www.jwatch.org/na35755/2014/10/08/polycystic-ovary-syndrome-diagnosis-and-management#sthash.CA6PTDxm.dpuf. Accessed July 30, 2015.
22. NICHD. What are the treatments for PCOS? www.nichd.nih.gov/health/topics/PCOS/conditioninfo/Pages/treatments.aspx. Accessed July 30, 2015.
23. Johnson NP. Metformin use in women with polycystic ovary syndrome. Ann Transl Med. 2014;2:56.
24. NICHD. Treatments for infertility resulting from PCOS. www.nichd.nih.gov/health/topics/PCOS/conditioninfo/Pages/infertility.aspx. Accessed July 30, 2015.
25. Kiddy DS, Hamilton-Fairley D, Bush A, et al. Improvement in endocrine and ovarian function during dietary treatment of obese women with polycystic ovary syndrome. Clin Endocrinol (Oxf). 1992;36:105-111.
26. Vause TD, Cheung AP, Sierra S, et al. Ovulation induction in polycystic ovary syndrome. J Obstet Gynaecol Can. 2010;32:495-502.
27. American College of Obstetricians and Gynecologists (ACOG). Polycystic ovary syndrome. Washington, DC: ACOG; 2009. ACOG Practice Bulletin; No. 108.
28. Thessaloniki ESHRE/ASRM-Sponsored PCOS Consensus Workshop Group. Consensus on infertility treatment related to polycystic ovary syndrome. Fertil Steril. 2008;89:505-522.
29. Legro RS, Brzyski RG, Diamond MP, et al. Letrozole versus clomiphene for infertility in the polycystic ovary syndrome. N Engl J Med. 2014;371:119-129.
To comment on this article, contact rdavidson@uspharmacist.com.





