US Pharm. 2016;41(6)(Generic Drug Review suppl):29-33.
ABSTRACT: Appropriate medication use can reduce morbidity and mortality among patients and lead to an increased quality of life. Most prescriptions filled in the United States are for generic medications. As drug costs surge, generic drug substitution will continue to play a crucial role in reducing healthcare costs and improving access to healthcare. Although generic substitutions generally are cheaper, there are situations in which they are inappropriate. Healthcare providers should consider a drug’s classification and state substitution laws prior to generic substitution. Additionally, education of patients and providers is essential to improving the use and perception of generic medications.
Appropriate medication use can reduce morbidity and mortality among patients and lead to increased quality of life. Approximately eight in 10 prescriptions filled in the United States are for generic medications. On average, generic medications cost 80% to 85% less than their brand counterparts, saving consumers $158 billion—an average of $3 billion per week—in 2010.1 As healthcare costs continue to increase both nationally and globally, cost-containment methods such as generic-drug substitution will continue to be an essential part of efforts to lower healthcare costs.2
In the past, generic-drug manufacturers were required to conduct costly preclinical and clinical trials to prove that their drugs were effective and safe. As a result, generics constituted a marginal fraction of the prescription-drug market.3 In 1984, the Drug Price Competition and Patent Term Restoration Act (also known as the Hatch-Waxman Act) provided a less challenging path to market for generic-drug manufacturers by creating the Abbreviated New Drug Application (ANDA) drug-approval process. The ANDA requires that generic-drug manufacturers demonstrate the generic drug’s pharmaceutical equivalence (i.e., identical active ingredient[s], dosage form and route, and strength and/or concentration) and bioequivalence to the innovator (brand) drug while adhering to the FDA’s Current Good Manufacturing Practices.3 Bioequivalence studies evaluate the rate and extent of absorption of a generic drug compared with the brand medication.4 Two drugs are considered bioequivalent if the 90% confidence interval (CI) of the mean AUC and maximum concentration of drug (Cmax) of the tested product is within 80% to 125% of that of the other product.4 This assumes that a generic drug has the same rate and extent of absorption as the brand drug and can produce an equivalent clinical effect.3 Since the ANDA does not require clinical trials to demonstrate efficacy and safety, generics are generally—but not always—less expensive than their brand counterparts. Additionally, competition among manufacturers and the reduced need for extensive advertising, marketing, and promotion of their generic products provide additional opportunities to pass savings to the patient.1
Although a substantial number of generic substitutions occur in the U.S., patients’, physicians’, and pharmacists’ perceptions of generics are important factors in the success of generic substitution.5 The generally lower cost associated with generic drugs is sometimes incorrectly interpreted as inferiority, creating a barrier to effective generic substitution. In an evaluation of 2,070 human studies, the FDA determined that the average difference in in vivo absorption between brand and generic drugs was 3.5%. This finding highlights the similarity between generic and brand drugs, since this percentage is acceptable even among different batches of brand drugs.6 There are some situations, however, in which generic drug substitution should be avoided or employed with caution. Healthcare providers should be knowledgeable about the process in order to improve cost-containment efforts while optimizing health outcomes.
Narrow Therapeutic Index Drugs and Antiepileptic Drugs
In several classes of medications, generic substitution is controversial. Narrow therapeutic index (NTI) drugs are medications with a small threshold between effective and toxic doses. This means that minor variations in the percentage of drug exposure may lead to serious adverse outcomes.4,7 Several medical associations have issued statements discouraging automatic generic substitution for brand NTI drugs.3,8-10 There is no comprehensive list of NTI drugs; however, the FDA has categorized warfarin, levothyroxine, carbamazepine, digoxin, lithium carbonate, phenytoin, and theophylline as NTI drugs.11,12 Several medications used in organ transplantation (e.g., cyclosporine, tacrolimus, sirolimus) have been categorized as NTI drugs by other resources.13 The European Medicine Agency (EMA) recommends that the accepted CI for the Cmax and AUC be narrowed to 90% to 111.11% for NTI drugs.3 In 2010, the FDA began working on recommendations for bioequivalence studies in certain medications. Among other changes, the FDA advisory committee has suggested reducing the CI to match the EMA’s recommendation and developing a public list of NTI drugs. Bioequivalence-study recommendations have been completed for some medications; however, a number of recommendations are in draft status.3,12
Generic substitution is also of particular concern with antiepileptic drugs (AEDs). Bioequivalence may be compromised in AEDs with low water solubility (e.g., phenytoin, carbamazepine), narrow therapeutic ranges (e.g., phenytoin, carbamazepine), and/or nonlinear pharmacokinetics (e.g., phenytoin, valproate), further complicating appropriate substitution.14 Case reports have described breakthrough seizures occurring with generic substitution for brand AEDs in previously stabilized patients.14 A case series found that breakthrough seizures occurred in patients switched from brand lamotrigine to generic lamotrigine; most patients experienced seizure control when switched back to brand lamotrigine.15 Additionally, physicians report that they are likely to discourage generic substitution for brand AEDs because of concerns about seizures.5,16-18 The American College of Neurology recommends against mandatory substitution of AEDs without the approval of the patient and the prescribing physician.
One concern about generic substitution of NTI medications and AEDs is that switching a stable patient to a medication that may not produce the same effects could potentially cause the patient harm, thereby outweighing the possible cost savings associated with these medications. Because of the serious conditions being treated and the adverse-effect profiles, generic substitution should be done with caution or avoided in the absence of approval from the patient and the healthcare provider.
Biosimiliars
Biologics are medications that are developed from living organisms (e.g., insulin, vaccines, erythropoietin).4 These medications, which are expensive, provide additional challenges for substitution owing to their large, complex structure and their manufacturing process. Because of the difficulty of creating a true generic, off-patent versions of brand biologic products are called biosimilar or follow-on products. A biologic product is considered to be biosimiliar if it is highly similar to its reference product and there are no clinically meaningful differences in safety, purity, and potency between the products.19 The safety of biosimiliars is a key concern owing to the immune-response issues associated with these drugs.20 The Biologics Price Competition and Innovation Act of 2009 (BPCIA) introduced an abbreviated licensure process for biosimiliars that requires analytical, animal, and clinical studies as proof that the product is biosimilar to or interchangeable with the reference product.19 Several biosimiliars (e.g., hyaluronidase [Hylenex, Hydase], somatropin [Omnitrope], glucagon [GlucaGen]) were approved prior to the new approval process for biosimiliars and are not rated as therapeutically equivalent. The first biosimiliar to receive FDA approval through the BPCIA was Zarxio (filgrastim-sndz), on March 6, 2015.21 Inflectra (infliximab-dyyb), the second biosimilar approved through the BPCIA (on April 5, 2016), is biosimilar to Remicade (infliximab).22 Pharmacists should be aware that biosimiliars approved through the BPCIA are not interchangeable at this time; however, this may change in the future.23
The Orange Book
The FDA provides guidance for substitution with its publication Approved Drug Products With Therapeutic Equivalence Evaluations (commonly known as the Orange Book), first published in 1980.4 This resource, which is available on the Internet, lists the bioequivalence standards of all FDA-approved medications. It should be noted that the Orange Book excludes some older medications that were brought to market prior to the implementation of FDA standards requiring drugs to be proven both safe and effective (Drug Efficacy Study Implementation drugs); medications that have not been evaluated for therapeutic equivalence; and medications that lack a reference drug (e.g., phenobarbital).3,4 Additionally, once a generic drug gains OTC status, it is removed from the Orange Book.
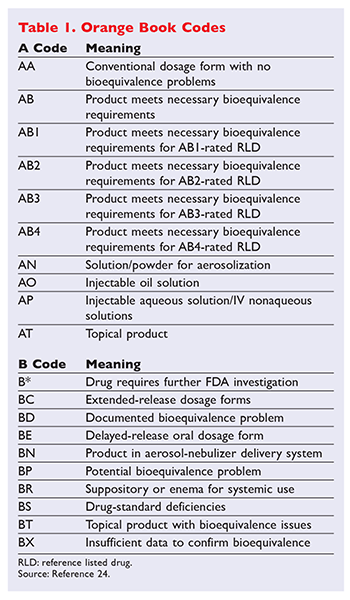
The Orange Book provides ratings for therapeutic equivalence between medications via a coding system indicating bioequivalence of the generic drug to the reference listed drug (RLD) used to gain FDA approval (TABLE 1). Codes start with the letter A or B and contain at least two letters. A-rated drugs (e.g., AB) have been determined to be bioequivalent to the brand drug, and B-rated drugs (e.g., BX) are considered not to be bioequivalent.4 A generic medication with an AB rating has in vivo or in vitro study results proving that it is therapeutically equivalent (displaying bioequivalence and pharmaceutical equivalence). Other A codes specify the dosage form when no issue is known or suspected (e.g., AA, AN). The B codes identify the suspected bioequivalence issue or provide the dosage forms. Since these medications are not considered to be therapeutically equivalent, they should not be substituted. Updated daily, the Orange Book is searchable by active ingredient, brand name, patent, or applicant.4
It is imperative that pharmacy personnel be familiar with the generic-substitution laws in their state. A B-rated generic should not be automatically substituted for its RLD. In these cases, prescriber authorization is needed, and details of the conversation should be noted on the prescription (e.g., date and time of contact, name of person providing authorization, etc).4 States guide and regulate generic product selection differently. For example, most states rely on the Orange Book for substitution, whereas some states have formularies that compile either a list of drugs approved for substitution or a list of drugs prohibited for substitution.4 Other states allow the pharmacist to determine substitution as long as the drug is pharmaceutically equivalent. Determining appropriate substitution for AB-rated drugs can prove difficult for medications with multiple brand names and generics. There are situations in which a generic is AB-rated to one brand medication, but not to other brand medications with the same active ingredient. For example, nifedipine has two extended-release brand drugs that are RLDs.24 Accordingly, the FDA adds a number to the end of the AB code (i.e., AB1, AB2) to minimize confusion between the RLDs. Drugs rated as AB1 are bioequivalent and pharmaceutically equivalent to each other, as are drugs that are AB2-rated, and so on. The electronic Orange Book provides guidance that is beneficial for pharmacy personnel to review.24
Education
Although the use of generic medications has become more prevalent, some patients and healthcare providers harbor negative perceptions of generic substitution that continue to challenge its acceptance. Dunne and Dunne conducted a systematic review of the opinions of physicians, pharmacists, and patients regarding generic medications and found a general improvement in the perception of generic drugs, but continued mistrust about the quality of generic medications.5 Skepticism about generic drugs was especially prevalent in patients, owing to the perception that lower cost signified lower quality. The review discovered that patients often poorly understood the information on substitution. Factors that influenced acceptance of generic medications included patient involvement in decisions, age, income, and severity of illness. Patients with less education and a lower income tended to distrust generics more.5 Physicians’ concerns centered on a lack of confidence in foreign manufacturers, doubts about equivalence, and the preference of brand drugs for personal use. Concerns with specific drug therapies (e.g., AEDs) were also noted. Pharmacists’ perspectives were mainly positive; however, safety concerns—especially in the elderly—were discussed owing to changes in the physical appearance of generic medications.5
In addition to being a more affordable alternative to brand drugs, generics also have been shown to contribute to medication adherence.25 Education of prescribers and consumers remains a key to improving acceptance of generic substitution. Patients’ willingness to approve a switch to a generic has been shown to increase after a short discussion.26 Physicians’ inclusion of patients in substitution decisions can increase patients’ confidence in generics.5 Pharmacists should inform patients about changes in manufacturer (which may cause packaging changes) and about the comparable effectiveness of generics and brand drugs. Pharmacists can also guide physicians on questions regarding bioequivalence, changes in regulation, and situations in which generic substitution is appropriate and when substitution should be made with caution or avoided.
Conclusion
Generic substitution can lead to improved medication adherence. Several factors, including a generic medication’s equivalence rating, should be taken into consideration prior to generic substitution. Healthcare providers play an essential role in imparting guidance for appropriate generic-drug use to optimize patient outcomes.
REFERENCES
1. FDA.gov. Facts about generic drugs. www.fda.gov/drugs/resourcesforyou/consumers/buyingusingmedicinesafely/understandinggenericdrugs/ucm167991.htm. Accessed February 1, 2016.
2. Basak SC, Sathyanarayana D. Exploring knowledge and perceptions of generic medicines among drug retailers and community pharmacists. Indian J Pharm Sci. 2012;74:571-575.
3. Pierini D, Anderson KV. How generic drugs are made. US Pharm. 2013;38(6)(Generic Drugs suppl):26-31.
4. Demystifying generic substitution: knowing the law. Hosp Pharm Lett. 2013:130307.
5. Dunne SS, Dunne CP. What do people really think of generic medicines? A systematic review and critical appraisal of literature on stakeholder perceptions of generic drugs. BMC Med. 2015;13:173.
6. Davit BM, Nwakama PE, Buehler GJ, et al. Comparing generic and innovator drugs: a review of 12 years of bioequivalence data from the United States Food and Drug Administration. Ann Pharmacother. 2009;43:1583-1597.
7. Paveliu MS, Bengea S, Paveliu FS. Generic substitution issues: brand-generic substitution, generic-generic substitution, and generic substitution of narrow therapeutic index (NTI)/critical dose drugs. Maedica (Buchar). 2011;6:52-58.
8. Gordon J, Schachter SC. Generic and brand name AEDs—considerations for clinicians and patients. www.epilepsy.com/information/professionals/diagnosis-treatment/therapeutic-and-generic-substitutions/article-generic. Accessed February 1, 2016.
9. Alloway RR, Isaacs R, Lake K, et al. Report of the American Society of Transplantation conference on immunosuppressive drugs and the use of generic immunosuppressants. Am J Transplant. 2003;3:1211-1215.
10. AACE, TES, and ATA joint position statement on the use and interchangeability of thyroxine products. www.aace.com/files/position-statements/aace-tes-ata-thyroxineproducts.pdf. Accessed February 1, 2016.
11. Yu LX. Quality and bioequivalence standards for narrow therapeutic index drugs. www.fda.gov/downloads/Drugs/DevelopmentApprovalProcess/HowDrugsareDevelopedandApproved/ApprovalApplications/AbbreviatedNewDrugApplicationANDAGenerics/UCM292676.pdf. Accessed February 1, 2016.
12. Tamargo J, Le Heuzey JY, Mabo P. Narrow therapeutic index drugs: a clinical pharmacological consideration to flecainide. Eur J Clin Pharmacol. 2015;71:549-567.
13. Johnston A. Equivalence and interchangeability of narrow therapeutic index drugs in organ transplantation. Eur J Hosp Pharm Sci Pract. 2013;20:302-307.
14. Generic substitution of antiepileptic drugs. Pharm Lett. 2007;23:230712.
15. Makus KG, McCormick J. Identification of adverse reactions that can occur on substitution of generic for branded lamotrigine in patients with epilepsy. Clin Ther. 2007;29:334-341.
16. Ngo SN, Stupans I, McKinnon RA. Generic substitution in the treatment of epilepsy: patient attitudes and perceptions. Epilepsy Behav. 2013;26:64-66.
17. Berg MJ, Gross RA, Haskins LS, et al. Generic substitution in the treatment of epilepsy: patient and physician perceptions. Epilepsy Behav. 2008;13:693-699.
18. Dunne SS, Shannon B, Cullen W, Dunne CP. Beliefs, perceptions and behaviours of GPs towards generic medicines. Fam Pract. 2014;31:467-474.
19. Christl L. FDA’s overview of the regulatory guidance for the development and approval of biosimilar products in the US. www.fda.gov/downloads/Drugs/DevelopmentApprovalProcess/HowDrugsareDevelopedandApproved/ApprovalApplications/TherapeuticBiologicApplications/Biosimilars/UCM428732.pdf. Accessed February 1, 2016.
20. Woodcock J. Assessing the impact of a safe and equitable biosimilar policy in the United States. www.fda.gov/NewsEvents/Testimony/ucm154017.htm. Accessed February 1, 2016.
21. FDA approves first biosimilar ZarxioTM (filgrastim-sndz) from Sandoz. www.sandoz.com/media_center/press_releases_news/global_news/2015_03_06_fda_approves_first_biosimilar_zarxio_from_sandoz.shtml. Accessed February 1, 2016.
22. FDA approves Inflectra, a biosimilar to Remicade. www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm494227.htm. Accessed April 26, 2016.
23. FDA.gov. Implementation of the Biologics Price Competition and Innovation Act of 2009. www.fda.gov/Drugs/GuidanceComplianceRegulatoryInformation/ucm215089.htm. Accessed February 1, 2016.
24. FDA.gov. Orange Book preface. www.fda.gov/Drugs/DevelopmentApprovalProcess/ucm079068.htm. Accessed February 1, 2016.
25. Sanchez CK, Farrell N, Lapp E. Generic drugs, cost, and medication adherence. US Pharm. 2015;40(6)(Generic Drugs suppl):14-19.
26. Roman B. Patients’ attitudes towards generic substitution of oral atypical antipsychotics: a questionnaire-based survey in a hypothetical pharmacy setting. CNS Drugs. 2009;23:693-701.
To comment on this article, contact rdavidson@uspharmacist.com.






