US Pharm. 2012;37(6):HS-2-HS-5.
Interstitial cystitis (IC), also known as painful bladder syndrome (PBS), is more common than was previously thought; however, the disorder is difficult to diagnose and treat. IC/PBS is part of a group of conditions that fall under the umbrella of chronic pelvic pain syndrome.1 In the past, a number of other names were used to describe IC/PBS, including urethral syndrome, trigonitis, and bladder pain syndrome. In 1987, the National Institute of Diabetes and Digestive and Kidney Diseases developed the first criteria for the diagnosis of IC. In 2002, the International Continence Society proposed changing the name from IC to IC/PBS and defined the condition as “the complaint of suprapubic pain related to bladder filling, accompanied by other symptoms such as increased daytime and night time frequency, in the absence of a proven urinary infection and other obvious pathology.”2 IC/PBS has been associated with other chronic pain syndromes, such as fibromyalgia, irritable bowel syndrome, and chronic fatigue syndrome. Some experts believe that IC/PBS may be a bladder manifestation of a more general condition, such as fibromyalgia or irritable bowel syndrome, that causes inflammation in various organs and areas of the body.
Although IC/PBS was initially considered to be a rare condition, its prevalence has significantly increased. IC/PBS is more common in women than in men. The only definitive risk factor for IC/PBS is female gender, with a female:male ratio of 10:1.1 In the United States, an estimated 3.3 million women aged 18 years and older have experienced pelvic pain or other urinary symptoms. An estimated 1.6 million men aged 30 years and older have persistent symptoms that are associated with PBS, such as pain upon bladder filling and pain relieved by bladder emptying.3 In 2000, the estimated medical expenditures associated with IC/PBS totaled $66 million.2
PATHOPHYSIOLOGY
IC/PBS is a chronic disease of unknown etiology; however, several theories exist, and the pathophysiology of IC/PBS is considered to be multifactorial.4 The proposed mechanism for the pathogenesis of IC/PBS is shown in FIGURE 1.
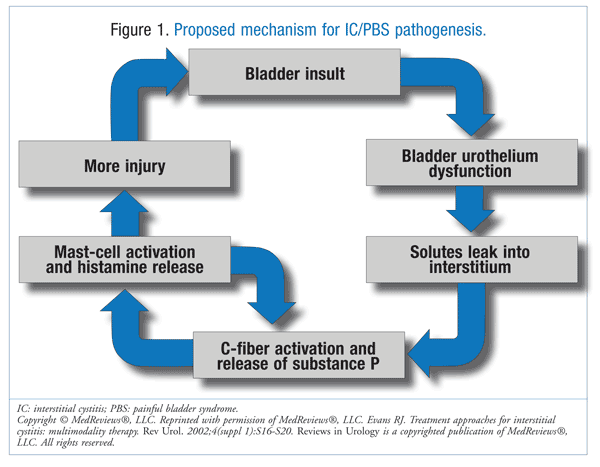
Although the underlying pathophysiology of IC/PBS is not completely understood, it is thought to involve changes in the bladder urothelium, mast-cell activation, and neurogenic inflammation. The normal bladder urothelium is highly impermeable to urinary solutes and irritants such as urea, ammonia, and potassium. The glycosaminoglycan (GAG) layer is responsible for protecting the bladder surface from irritants. Deficiency of the GAG layer results in increased urothelial permeability, which allows irritants to leak from the urine into the bladder tissue. This results in symptoms of IC/PBS, such as pelvic pain and irritative voiding symptoms. In addition to the changes in the bladder urothelium, mast-cell activation is increased, which can lead to more mast-cell upregulation, inflammation of the bladder wall, injury to the GAG layer, and eventually fibrotic changes within the bladder wall.4
CLINICAL EVALUATION AND DIAGNOSIS
The clinical presentation of IC/PBS is variable. However, most patients present with urgency, frequency, and/or pain. IC/PBS should be considered if a patient experiences any of the following symptoms: pelvic pain, dyspareunia, frequent urinary tract infections, frequent vaginitis (women) or prostatitis (men), nocturia, and urinary frequency and urgency.4-6
Pain during sexual activity is common in both men and women with IC/PBS. Women may also experience a flare of symptoms during the premenstrual week. The clinical evaluation of IC/PBS should begin with a thorough medical history and physical examination if the patient is experiencing pain, nocturia, frequency, and/or urgency. In addition, the history should include inquiry regarding urinary tract infections, pelvic surgeries, and central nervous system or autoimmune disorders. Even though there are no specific physical-examination findings in IC/PBS, a pelvic examination is important to rule out vaginitis, vulvar lesions, urethral diverticula, and pelvic-floor dysfunction.4-6
Questionnaires are another useful screening tool. The most commonly employed screening tools in IC/PBS are the Pelvic Pain and Urgency/Frequency Patient Symptom Scale and the O’Leary-Sant Interstitial Cystitis Symptom Index and Problem Index. These surveys include questions pertaining to pain, urinary urgency and frequency, and nocturia. A high score on both surveys warrants further evaluation for possible IC/PBS. Physicians often recommend that patients keep a voiding diary to document frequency and volume. This diary is used not only for screening purposes, but also to monitor response to treatment.4-6
Laboratory tests such as urinalysis can help differentiate IC/PBS from other conditions. Urinalysis also may be used to rule out hematuria. In addition, a urine culture is required to exclude urinary tract infection. If hematuria is present and the patient is older than 40 years of age and has a history of smoking, cytology and CT scan are typically performed to rule out urinary tract malignancies.4-6
In addition, cystoscopy should be performed routinely in patients with gross hematuria and a history of smoking. This procedure may be performed on an outpatient basis in the physician’s office or in the hospital under general anesthesia. In cystoscopy, the physician inserts a thin telescope containing a camera and a light into the bladder via the urethra. The purpose of the procedure is to examine the lining of the bladder to detect any abnormalities. The bladder of a patient with IC/PBS may be normal or abnormal; if any abnormalities are seen on cystoscopy, however, further testing and examination may be warranted.4-6
Other diagnostic procedures include the potassium sensitivity test and urodynamic studies. The potassium sensitivity test uses sterile water and potassium chloride solution as an irritant to detect dysfunction of the bladder urothelium. Increased pain when the solution is instilled into the bladder denotes a positive result. Urodynamics (a series of tests to determine lower urinary tract function) remain controversial, but they are useful for excluding overactive bladder syndrome and evaluating bladder dysfunction in men.4-6
TREATMENT
The goals of therapy for IC/PBS are to alleviate stress and anxiety, treat and relieve current symptoms, restore bladder-surface integrity, modulate neuronal dysfunction, and reduce coexisting inflammation.7
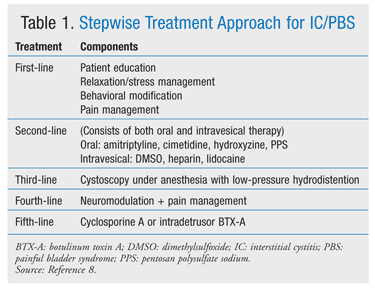
According to the guidelines developed by the American Urological Association (AUA), the treatment of IC/PBS involves a stepwise approach—more conservative therapies are tried first, with more aggressive therapies reserved for when symptom control is inadequate or not achieved (TABLE 1).8 Initial treatment depends upon several factors: patient preference, symptom severity, and physician judgment or recommendation. The simultaneous use of multiple treatment approaches may be considered in patients who do not achieve symptom relief upon initial treatment. First-line treatment should be initiated in all patients.
Nonpharmacologic Therapy
Behavioral therapy is considered the mainstay of treatment for patients with IC/PBS. IC/PBS may be worsened by stress, anxiety, and depression. Behavioral therapy involves not only education about symptoms, but also behavior-modification techniques for symptoms such as urinary frequency and urgency, physical therapy for trigger-point release, stress reduction, and diet and lifestyle modification. Patients with IC/PBS should learn to identify foods and beverages that trigger or aggravate their symptoms. Avoiding foods that irritate the bladder (e.g., those that are rich in potassium) and foods with a high acid content (e.g., tomatoes, chocolate, citrus fruits/juices, coffee, alcohol, and carbonated beverages) can minimize or prevent symptoms. Patients are encouraged to keep a diary of foods consumed and to identify any resultant symptoms.4,7
Pharmacologic Therapy
Pharmacologic treatment options for patients with IC/PBS can be categorized into three different approaches: intravesical drug instillation, systemic (oral) treatment, and surgery.9 The following treatment options should not be considered in patients with IC/PBS because of a lack of evidence or efficacy and an increased risk of adverse effects: long-term antibiotics, intravesical instillation of resiniferatoxin or bacillus Calmette-Guérin, high-pressure hydrodistention, and long-term systemic (oral) glucocorticoid use.8
Intravesical Drug Instillation: Also called bladder bath or bladder wash, bladder instillation is used to reduce IC/PBS symptoms and pain. Dimethylsulfoxide (DMSO), the only drug approved by the FDA for this procedure, is used for instillation and has been shown to provide good-to-excellent symptom relief in at least 50% of patients.6 The mechanism of action is uncertain, but DMSO is thought to work by depleting substance P and reducing mast-cell degranulation.1 In this treatment, a catheter is placed into the bladder, after which DMSO is passed through the catheter and held in the bladder for an average of 10 to 15 minutes before normal voiding and urination. DMSO may be administered every week or two for up to 6 to 8 weeks. The advantage of DMSO treatment is that patients can be taught to catheterize themselves and administer the solution at home. The most common adverse effect of DMSO is a bothersome garlicky taste and odor on the breath and skin that can last up to 7 hours after treatment. CBC and kidney- and liver-function tests should be performed every 6 months.
Several other intravesical therapies have been tried in patients with IC/PBS; however, data are limited.3 Heparin has been used in combination with lidocaine and sodium bicarbonate to relieve IC/PBS symptoms by restoring barrier function of the epithelial mucous layer of the urothelium. This treatment may be offered as an alternative to DMSO.9
Systemic (Oral) Treatment: This therapy consists of cimetidine, amitriptyline, hydroxyzine, and pentosan polysulfate sodium (PPS). Evidence supporting the use of cimetidine to relieve painful bladder symptoms is weak. The recommended dosage of cimetidine that was found to relieve symptoms is 400 mg daily.9 Amitriptyline is a tricyclic antidepressant that is commonly used in patients with IC/PBS to regulate bladder pain and urgency. Although the exact mechanism of action is unknown, amitriptyline is believed to work by modulating neuronal dysfunction. In one study, amitriptyline provided mild-to-moderate central pain relief in 60% to 90% of patients.10 The dosage of amitriptyline used to treat chronic pain is much lower than that used to treat depression. The typical starting dose is 25 mg at bedtime (because of the incidence of drowsiness), with an increase to 50 mg daily after 1 to 2 months. Common adverse effects associated with amitriptyline use are dry mouth, blurred vision, and constipation. Pain relief may not occur for up to 3 weeks.
The addition of hydroxyzine, an oral antihistamine, to the treatment regimen is usually recommended to suppress mast-cell degranulation and therefore decrease the inflammatory response associated with IC. The recommended starting dose is 25 mg at bedtime, with an increase to 50 to 100 mg daily during allergy season. The most common adverse effect associated with hydroxyzine use is drowsiness.6,7
PPS, the only oral medication currently approved by the FDA for the treatment of IC/PBS, recently has become the cornerstone of therapy. The approved dosage is 100 mg three times daily, administered 1 hour before or 2 hours after a meal. Patients typically are slow to respond to PPS therapy, and symptom relief may not occur for 3 to 4 months. However, PPS treatment should continue for at least 6 months so that the medication has sufficient time to relieve urinary symptoms. The adverse effects of PPS are limited primarily to gastrointestinal discomfort (e.g., diarrhea, nausea, dyspepsia, and abdominal pain). Additional adverse effects include alopecia, headache, and rash. Liver function should be monitored in patients taking PPS. In addition, because PPS has not been tested in pregnant women, the drug is not recommended for use in this patient population. PPS should also be discontinued prior to surgery because of its mild blood-thinning effects. PPS is usually added to amitriptyline or hydroxyzine in patients with severe or advanced IC/PBS.3,6,7
Evidence supporting the use of cyclosporine and botulinum toxin A is limited, and currently neither of these treatment options is approved by the FDA. The AUA recommends that the use of these treatment options be limited and administered only by a practitioner experienced in managing patients with IC/PBS.8
Surgery: Procedures such as cystoplasty and urinary diversion with or without cystectomy may be considered in IC/PBS patients in whom all other therapies have failed to provide symptom relief.
CONCLUSION
IC/PBS is a chronic disease of unknown etiology that is often difficult to diagnose and treat. For this reason, the management of patients with IC/PBS can be challenging. It is important to remember that treatment must be individualized and that not all therapies will be effective in every patient. Combination therapy may be necessary in order to achieve symptom relief. Currently, therapeutic evidence is limited, and few randomized, controlled trials exist in the area of IC/PBS. Additional clinical trials and evidence-based therapies are essential for optimizing the treatment of patients who have this ongoing condition.
REFERENCES
1. McDermott P. Painful bladder syndrome/interstitial cystitis (history, epidemiology, symptoms, diagnosis and treatments). Int J Urol Nurs. 2009;3:16-23.
2. Persu C, Cauni V, Gutue S, et al. From interstitial cystitis to chronic pelvic pain. J Med Life. 2010;3:167-174.
3. National Kidney & Urologic Diseases Information Clearinghouse.
Interstitial cystitis/painful bladder syndrome.
http://kidney.niddk.nih.gov/kudiseases/pubs/interstitialcystitis.
Accessed February 18, 2012.
4. Butrick CW, Howard FM, Sand PK. Diagnosis and treatment of interstitial cystitis/painful bladder syndrome: a review. J Womens Health (Larchmt). 2010;19:1185-1193.
5. Moutzouris DA, Falagas ME. Interstitial cystitis: an unsolved enigma. Clin J Am Soc Nephrol. 2009;4:1844-1857.
6. Rosenberg M, Parsons CL, Page S. Interstitial cystitis: a primary care perspective. Cleve Clin J Med. 2005;72:698-704.
7. Rosenberg MT, Newman DK, Page SA. Interstitial cystitis/painful
bladder syndrome: symptom recognition is key to early identification,
treatment. Cleve Clin J Med. 2007;74:S54-S62.
8. Hanno PM, Burks DA, Clemens JQ, et al. Diagnosis and treatment of
interstitial cystitis/bladder pain syndrome. American Urological
Association (AUA) Guideline.
www.auanet.org/content/guidelines-and-quality-care/clinical-guidelines/main-reports/ic-bps/diagnosis_and_treatment_ic-bps.pdf.
Accessed February 18, 2012.
9. Dasgupta J, Tincello DG. Interstitial cystitis/bladder pain syndrome: an update. Maturitas. 2009;64:212-217.
10. Hanno PM. Amitriptyline in the treatment of interstitial cystitis. Urol Clin North Am. 1994;21:89-91.
To comment on this article, contact rdavidson@uspharmacist.com.





