US Pharm. 2011;36(6):39-43.
A urinary tract infection (UTI), defined as an inflammatory response resulting from the presence of microorganisms in the urinary tract, is one of the most common bacterial infections for which patients seek treatment.1 Overall, UTIs account for over 7 million health care provider visits each year, and acute uncomplicated cystitis is one of the most common reasons that antibiotics are prescribed to otherwise healthy women.1,2 It is estimated that 11% of women in the United States who are 18 years of age and older have a UTI each year, with the highest incidence of infection among those between 18 and 24 years of age.3 Pyelonephritis (UTI that spreads to the kidneys) occurs at a rate of approximately 59 episodes per 10,000 women each year.4
Although UTIs encompass a variety of syndromes ranging from asymptomatic bacteriuria to pyelonephritis with bacteremia or sepsis,1 this article focuses on the recently updated guidelines for the treatment of acute uncomplicated cystitis and pyelonephritis in women. It is important to note that these guidelines are applicable to the management of premenopausal, nonpregnant women with no known urologic abnormalities or comorbid medical conditions. This article reviews the current antimicrobial treatment recommendations from the 2010 guidelines published through the collaboration of the Infectious Diseases Society of America and the European Society for Microbiology and Infectious Diseases.2
Clinical Presentation
Signs and symptoms of uncomplicated cystitis include increased frequency and urgency of urination, dysuria (pain on urination), bacteriuria (the presence of bacteria in the urine), pyuria (the presence of pus or white blood cells in the urine), and pain or pressure around the bladder.4-6 Hematuria (blood in the urine) can be present microscopically, and less often is present macroscopically.4 If vaginal discharge or irritation is present, an alternative diagnosis should be considered. In addition, women with acute uncomplicated cystitis typically do not have fever or flank pain; if a patient presents with these symptoms, an alternate diagnosis such as pyelonephritis or complicated UTI should be considered.2,4 Pyelonephritis should be suspected if the patient experiences nausea, vomiting, flank pain, fever, and/or costovertebral angle tenderness in addition to urinary symptoms.4
Diagnosis
Urine samples obtained through the midstream clean-catch technique can be used to provide more conclusive evidence in patients suspected of having an infection. Urine cultures and sensitivity tests are typically considered unnecessary in acute uncomplicated cystitis unless the patient experiences treatment failure or recurrent infection; in these patients, a urinalysis is commonly performed.4,7 Components of a urinalysis include bacteria count and Gram stain; pyuria (with counts of >10 leukocytes per mm3 suggesting infection); the leukocyte esterase dipstick test (a rapid-screening test for pyuria since leukocyte esterase is found in neutrophils and its presence indicates white blood cells); and the nitrite test (which detects an enzyme found in bacteria that reduce nitrate).7
In addition to the situations previously mentioned, urine culture and susceptibility tests are recommended for patients with suspected pyelonephritis.2,7 The presence of >105 colony-forming units of bacteria per mL of urine is suggestive of infection, and the microbiology laboratory will test pathogens for antimicrobial susceptibility.7
Etiology
The most common microbial etiology of acute uncomplicated cystitis is Escherichia coli, which causes 80% to 85% of cases.4,5 The second most common pathogen is Staphylococcus saprophyticus, which is responsible for approximately 5% to 15% of cases. Other less common microbial etiologies of acute cystitis include Klebsiella pneumoniae, Proteus mirabilis, and Streptococcus agalactiae.4,5 These organisms may also cause uncomplicated pyelonephritis, while complicated cases in hospitalized patients may be caused by additional organisms such as Enterobacter species (spp), Pseudomonas aeruginosa, Enterococcus spp, or Staphylococcus spp.1
Approach to Treatment
The authors of the updated guidelines point out several changes since the guidelines were previously published in 1999.2 The first is that there has been an increase in antimicrobial resistance of urinary pathogens. There has also been an increased understanding of the importance of minimizing “collateral damage,” which has been more commonly associated with the use of third-generation cephalosporins and the fluoroquinolones. “Collateral damage” has been defined as the ecologic adverse effects of antimicrobial therapy in terms of the selection of drug-resistant organisms, unwanted effects (such as Clostridium difficile infection), or the development of colonization or infection with drug-resistant organisms.8 Finally, there have been additional clinical studies with various antimicrobial agents and durations of therapy since the publication of the previous guidelines. These factors were taken into account in the updated recommendations.2
Additional factors that the clinician should take into account when deciding the most appropriate antimicrobial regimen for a patient with a UTI include availability of the medication, ability of the patient to tolerate oral medications, the patient’s allergy history, and local antimicrobial resistance patterns.2
Treatment of Acute Uncomplicated Cystitis
The updated guidelines recommend nitrofurantoin, trimethoprim-sulfamethoxazole (TMP-SMZ), or fosfomycin as the first-line treatment for acute uncomplicated cystitis.2 The recommended dosing regimen, duration of therapy, and therapeutic considerations for each agent are included in TABLE 1. If the clinician is uncertain as to whether a patient’s diagnosis is cystitis or pyelonephritis, nitrofurantoin and fosfomycin should be avoided because adequate drug levels in renal tissues are not achieved with these agents.2
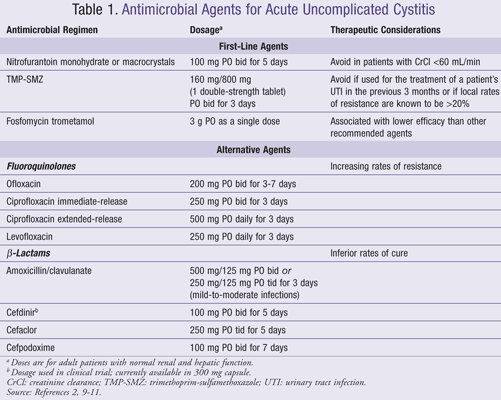
If one of the first-line agents cannot be used, a fluoroquinolone or b-lactam agent may be considered (TABLE 1).2,9-11 Although fluoroquinolones are highly efficacious, the guidelines consider this class of agents as alternatives in order to preserve their use for other indications. There has been an increasing prevalence of resistance of uropathogens and other microorganisms to the fluoroquinolones, potentially causing infections at other body sites that are more difficult to treat. If an agent in this class is used to treat a patient for cystitis in a geographic area of high resistance, close follow-up is warranted.2
Although several b-lactam options are available for the treatment of uncomplicated cystitis, most studies have demonstrated inferior rates of cure with b-lactams as compared to fluoroquinolones. It is believed that these lower rates of cure are a result of lower rates of eradication of vaginal uropathogens, so that the vaginal reservoir remains a potential source of continued infection. One randomized, single-blind study showed that a 3-day regimen of amoxicillin-clavulanate was less effective than a 3-day course of ciprofloxacin for the treatment of uncomplicated cystitis in women, even when the source of infection was a susceptible strain of bacteria.12 Although cefdinir is recommended as an option in the guidelines based upon results of a study that found comparable clinical and microbiologic cure rates with cefdinir 100 mg twice daily as compared to cefaclor 250 mg three times daily for 5 days,11 cefdinir is not FDA approved for this indication and is currently available in a 300-mg capsule dosage form.9
Finally, cefpodoxime 100 mg twice daily for 3 days was found to be comparable in safety and efficacy to a 3-day course of therapy with one double-strength tablet of TMP-SMZ in a randomized, multicenter study13; however, it is important to note that the current recommendation is to use cefpodoxime for a 7-day course of therapy if it is used.9 Overall, the guidelines recommend avoiding b-lactams as empiric therapy for uncomplicated cystitis, unless none of the first-line recommended agents are appropriate for use.2
It is important for the clinician to note that the guidelines recommend to avoid ampicillin or amoxicillin monotherapy because of the increasing prevalence of resistance to these agents, resulting in lower efficacy.2 If these agents are used for treatment, the patient should be followed closely to assess for response to therapy.
Monitoring Response to Treatment
For patients with an uncomplicated UTI whose symptoms do not respond to therapy or recur after a course of treatment, a urine culture may be obtained to identify the infecting pathogen(s) and assist the clinician with selecting the most appropriate antimicrobial agent.2
Approximately 20% of recurrent episodes of a UTI are a relapse, defined as a UTI occurring within 2 weeks of a previous episode that represents persistence of infection by the same microorganism.1 For patients who relapse after short-course therapy, it is recommended to treat with a different agent for a 2-week duration of therapy. Eighty percent of recurrent episodes of a UTI are considered to be reinfections, defined as a UTI that occurs >2 weeks after completion of therapy for a previous UTI; reinfections usually represent infection by a different microorganism. If the patient has fewer than three infections per year, each episode should be treated as a separately occurring infection, typically with a short course of antibiotic therapy. If the patient has three or more infections per year, it is important to assess if there is an identified risk factor, such as sexual activity. If so, the patient should be counseled to void after intercourse and may be prescribed to take a single dose of TMP-SMZ after each occasion of intercourse. If there is no identified precipitating event, the patient should be treated for each event, followed by prophylactic daily therapy (with either one-half of a single-strength tablet of TMP-SMZ, trimethoprim 100 mg, or nitrofurantoin 50 mg to 100 mg).1
Treatment of Pyelonephritis
It is recommended to obtain a urine culture and sensitivity report in all patients with suspected pyelonephritis.2 In addition, it is recommended to obtain blood cultures in patients who are hospitalized. Once laboratory results return, antimicrobial treatment can be directed toward the infecting pathogen(s).2
There are several treatment options for patients who are not hospitalized.2 The first is a fluoroquinolone-based regimen, which is only recommended for use if the prevalence of fluoroquinolone resistance is <10%. Recommended regimens include oral ciprofloxacin 500 mg twice daily for 7 days, ciprofloxacin 1,000 mg extended-release daily for 7 days, or levofloxacin 750 mg daily for 5 days. These regimens may be preceded by an initial one-time IV dose of either a fluoroquinolone, ceftriaxone, or a consolidated 24-hour dose of an aminoglycoside.
Another treatment option for uncomplicated pyelonephritis in patients who are not hospitalized is oral TMP-SMZ 160 mg/800 mg (1 double-strength tablet) twice daily for 14 days; however, this agent should only be used if the infected pathogen is known to be susceptible. It is recommended to give an initial IV dose of ceftriaxone or an aminoglycoside if sensitivity results are not initially known. Finally, oral b-lactams are considered to be less effective than other agents for the treatment of pyelonephritis. If used, an initial one-time IV dose of ceftriaxone or an aminoglycoside is recommended, followed by a 10- to 14-day course of therapy with a b-lactam agent.2
For patients who are hospitalized, the initial antimicrobial treatment regimen should be given via the IV route of administration.1,2 Several regimens may be used, with the choice of agents based on local patterns of resistance. Recommended options for empiric antimicrobial regimens include a fluoroquinolone; an aminoglycoside, with or without ampicillin; an extended-spectrum cephalosporin; an extended-spectrum penicillin; or one of the carbapenems. Once culture and sensitivity results are available, therapy should be directed toward the infecting pathogen(s). After clinical improvement, patients may be transitioned to an oral agent or regimen that has activity against the infecting pathogen(s).1,2
Antimicrobial Monitoring Parameters and Drug Interactions
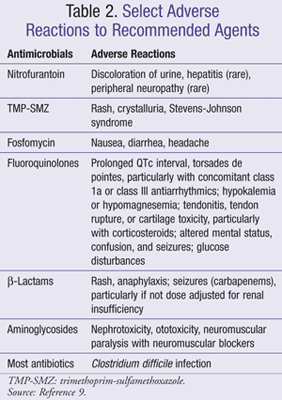
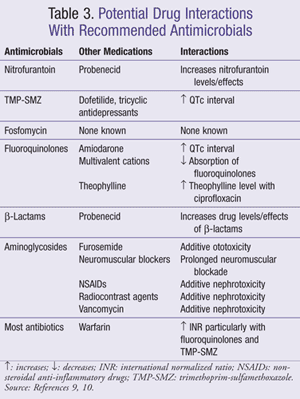
It is important for the clinician to be aware of appropriate monitoring parameters and drug interactions based on the recommendation for a particular antimicrobial agent or regimen. Common adverse reactions to specific medications or medication classes covered in this article are listed in TABLE 2 and interactions between antimicrobials and commonly used medications are included in TABLE 3.
Conclusion
Pharmacists should actively engage with other clinicians to select the most suitable antimicrobial agent or regimen for the treatment of acute uncomplicated cystitis and pyelonephritis in women. Pharmacists are in a key position to appropriately dose antimicrobial regimens and to monitor for adverse reactions and drug interactions. They also play an important role in educating health care providers and patients about the appropriate use of antimicrobials to limit the spread of antimicrobial resistance. Pharmacists must work with patients and other health care providers to ensure the proper treatment of these infections.
REFERENCES
1. Coyle E, Prince R. Urinary tract infections and prostatitis. In: DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 7th ed. New York, NY: McGraw Hill; 2008.
2. Gupta K, Hooton T, Naber K, et al. International clinical practice guidelines for the treatment of acute uncomplicated cystitis and pyelonephritis in women: a 2010 update by the Infectious Diseases Society of America and the European Society for Microbiology and Infectious Diseases. Clin Infect Dis.
3. Barbosa-Cesnik C, Brown M, Buxton M, et al. Cranberry juice fails to prevent recurrent urinary tract infection: results from a randomized placebo-controlled trial. Clin Infect Dis. 2011;52:23-30.
4. Guay D. Contemporary management of uncomplicated urinary tract infections. Drugs.
5. Hooton T, Besser R, Foxman B, et al. Acute uncomplicated cystitis in an era of increasing antibiotic resistance: a proposed approach to empirical therapy. Clin Infect Dis. 2004;39:75-80.
6. Nazarko L. Urinary tract infection: diagnosis, treatment and prevention. Br J Nurs. 2009;18:1170-1174.
7. Wilson M, Gaido L. Laboratory diagnosis of urinary tract infections in adult patients. Clin Infect Dis.
8. Paterson D. “Collateral damage” from cephalosporin or quinolone antibiotic therapy. Clin Infect Dis.
9. Lexi-Comp Online [Internet database]. Hudson, OH: Lexi-Comp, Inc; 2011.
www.lexi.com. Accessed April 4, 2011.
10. Micromedex Healthcare Series [Internet database]. Greenwood Village, CO: Thomson Healthcare; 2011.
www.thomsonhc.com/micromedex2/ 2011;52:e103-e120. 2008;68:1169-1205. 2004;38:1150-1158. 2004;38(suppl 4):S341-S345.
11. Leigh A, Nemeth M, Keyserling C, et al. Cefdinir versus cefaclor in the treatment of uncomplicated urinary tract infection. Clin Ther. 2000;22:818-825.
12. Hooton T, Scholes D, Gupta K, et al. Amoxicillin-clavulanate vs. ciprofloxacin for the treatment of uncomplicated cystitis in women: a randomized trial. JAMA. 2005;293:949-955.
13. Kavatha D, Giamarellou H, Alexiou Z, et al. Cefpodoxime-proxetil versus trimethoprim-sulfamethoxazole for short-term therapy of uncomplicated acute cystitis in women. Antimicrob Agents Chemother. 2003;47:897-900.
To comment on this article, contact rdavidson@uspharmacist.com.





