US Pharm. 2021;46(2):29-35.
ABSTRACT: The COVID-19 pandemic has presented the global research community with the greatest challenge of its generation. Safe and effective therapeutic agents are limited, and there are hundreds of ongoing clinical trials. Remdesivir is the only antiviral that is currently FDA approved for the management of COVID-19. This article discusses the mode of action of current investigational antiviral agents, the evidence of their effectiveness, and clinical trials that are currently being conducted in the United States.
The coronavirus disease 2019 (COVID-19) pandemic continues to present an unprecedented challenge to identify effective drugs for prevention and treatment. The disease is caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), a beta-coronavirus that is genetically similar to the SARS-CoV and Middle East respiratory syndrome coronavirus (MERS-CoV).1 Current management of patients is mainly based on the controlling the symptoms and the experiences of therapies for similar viruses. There are hundreds of ongoing clinical trials investigating new and repurposed agents, primarily focusing on antivirals and immunomodulators. Some antivirals under investigation are reviewed here.
Pathophysiology
The SARS-CoV-2 virus is a single-stranded RNA-enveloped virus with three kinds of proteins on its envelope, including spike protein (S-protein), envelope protein, and membrane protein.2 The S-protein is instrumental in host-cell recognition and binding, as well as mediating the fusion of the virus envelope with the cell membrane. Its cleavage activation is mediated by the transmembrane protease serine subfamily member 2 (TMPRSS2). The S-protein in the SARS-CoV and SARS-CoV-2 both recognize and bind to the same host receptor, the angiotensin-converting enzyme 2 (ACE 2) receptor.1 These receptors are commonly expressed on the epithelial cells of alveoli, trachea, bronchi, and bronchial serous glands of the respiratory tract.3 As such, TMPRSS2 inhibitors or ACE inhibitors are potential therapeutic agents for COVID-19.
Once the S-protein binds to the host cell, the virus enters the cell via endocytosis, where lysosomes are formed and the RNA is released and translated into viral polymerase proteins regulated by related protease and pH.2 Endosomal acidification inhibitors, such as chloroquine, and membrane fusion inhibitors, such as arbidol, may prove useful in blocking this step.2
The RNA completes the transcription and translation of virus proteins, and RNA replication occurs in the cytoplasm. Nucleoside analogues such as remdesivir, protease inhibitors such lopinavir/ritonavir (LPVr), and SARS-CoV-2 3CLpro protease (for processing of polyproteins translated from the viral RNA) inhibitors, such as pyridine-containing ketoamides, can block this process. Lastly, RNA combines with the protein shells to generate new coronavirus particles that are released from the host through the Golgi apparatus to infect new cells.2
Antiviral Drug Candidates for Treating Covid-19
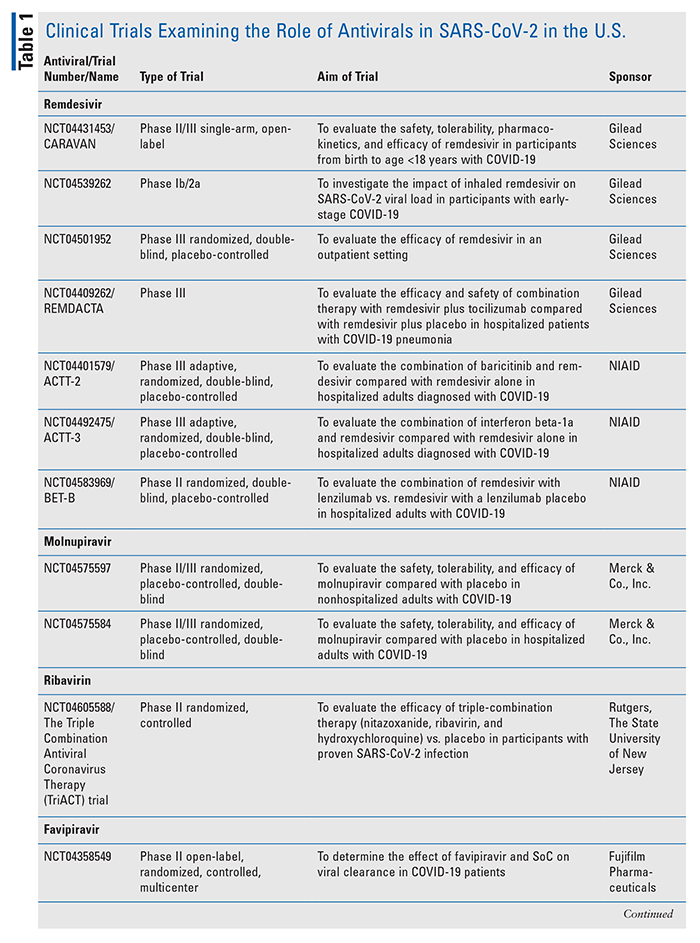
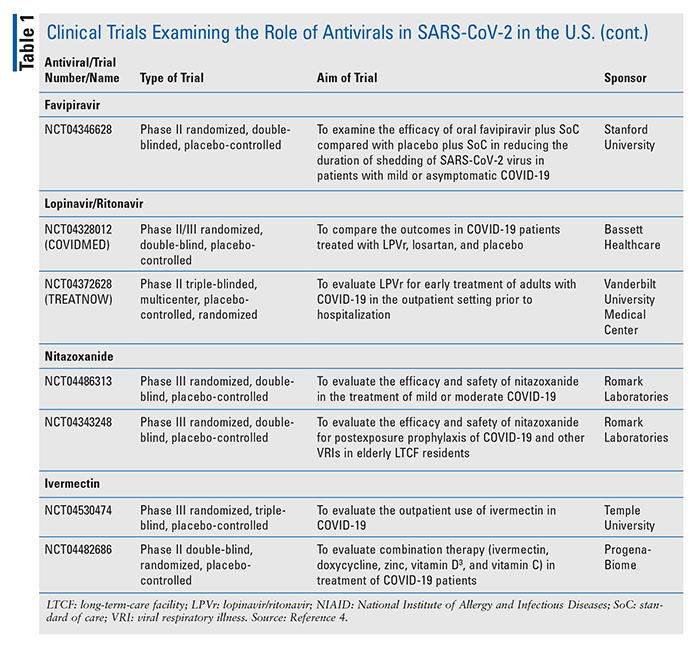
Several ongoing clinical trials are currently underway, many focusing on repurposing established antiviral therapies, especially those that showed prior efficacy against MERS-CoV and SARS-CoV. TABLE 1 provides a snapshot of some of ongoing U.S. trials.4
Nucleoside Analogues
Remdesivir (Veklury): Remdesivir is a broad-based antiviral drug originally designed to target Ebola. It inhibits viral replication through premature termination of RNA transcription, thereby disrupting the reproductive ability of the virus.3 In May 2020, remdesivir was FDA approved under emergency-use authorization (EUA) for the treatment of hospitalized patients with COVID-19. The EUA was later expanded to cover patients with nonsevere disease too.5
A randomized, double-blinded, placebo-controlled trial was performed to examine the time to recovery in hospitalized COVID-19 patients treated with remdesivir (200-mg loading dose on Day 1 and 100 mg daily for up to 9 additional days).6 The results showed that remdesivir had a shorter time to recovery than placebo (P <.001) and that remdesivir may have prevented the progression to more severe respiratory disease. Data were also obtained from a randomized, open-label trial evaluating different durations of remdesivir and an open-label trial evaluating different durations of remdesivir compared with standard of care (SoC).7,8 These trials did not record a significant difference between a 5-day course and a 10-day course.
Based upon these findings, remdesivir has since been approved by the FDA to treat COVID-19 in adults and pediatric patients aged 12 years and older weighing at least 40 kg and requiring hospitalization.9 The recommended dose is a single loading dose of remdesivir 200 mg on Day 1 followed by once-daily maintenance doses of remdesivir 100 mg from Day 2 infused over 30 to 120 minutes. The use of remdesivir is contraindicated in patients with a history of clinically significant hypersensitivity reactions to remdesivir or any components of the product. The most common adverse effects noted with remdesivir are nausea and increased alanine aminotransferase (ALT) and aspartate aminotransferase (AST) test results. Remdesivir is being tested for use in expanded populations as well as in combination therapy (TABLE 1).
Molnupiravir: Molnupiravir (MK-4482 [previously EIDD-2801]; Merck) is a prodrug of the ribonucleoside analogue EIDD-1931. It is a clinical-stage oral antiviral agent that exerts its effect by introducing copying errors during viral RNA replication of the SARS-CoV-2 virus.10 It is an investigational molecule not commercially available in the U.S. The drug has been tested in a phase I randomized, double-blind, placebo-controlled, first-in-human study designed to evaluate its safety, tolerability, and pharmacokinetics following oral administration to healthy volunteers. Two phase II/III randomized, placebo-controlled, double-blind clinical studies are being conducted to evaluate the efficacy and safety of molnupiravir in adult participants with COVID-19 (TABLE 1).
Ribavirin: Ribavirin is a guanosine analogue that interferes with polymerases, leading to RNA degradation.11 It has broad-spectrum antiviral activity against both RNA and DNA viruses. Ribavirin is FDA approved for the treatment of chronic hepatitis C (CHC) virus infection in combination with peginterferon alfa-2a (PEGASYS) in patients aged 5 years and older with compensated liver disease not previously treated with interferon alpha and in adult CHC patients coinfected with HIV.12 The recommended dose is 800 mg by mouth daily for a total of 48 weeks. It is contraindicated in pregnant women and in men whose female partners are pregnant, in patients with hemoglobinopathies, and during coadministration of didanosine. The most common adverse effects associated with the use of ribavirin include fatigue/asthenia, pyrexia, myalgia, and headache. Ribavirin may interact with other nucleoside analogues and azathioprine.
One study suggested the effectiveness of ribavirin as a potential agent against SARS-CoV-2.13 Ribavirin is currently undergoing trials to evaluate its efficacy as a component of triple therapy (TABLE 1).
Favipiravir (Avigan): Favipiravir triphosphate is a purine nucleoside analogue that competitively inhibits viral RNA-dependent RNA polymerase, halting viral replication.14 It has activity against influenza A and B as well as several agents of viral hemorrhagic fever and SARS-CoV-2 in vitro.14
Favipiravir is not commercially available in the U.S. but is approved for novel epidemic influenza strains that are unresponsive to standard antiviral therapies in Japan.14
In the early stages of the pandemic, a small open-label, nonrandomized, controlled study was performed on COVID-19 patients in China comparing favipiravir with controls treated with LPVr. The study noted a significant reduction in the time to SARS-CoV-2 viral clearance in patients treated with favipiravir compared with controls.15 Another open-label, prospective, randomized, multicenter study in China compared the effect of favipiravir with umifenovir on the clinical recovery rate at 7 days in adults with COVID-19 pneumonia. It was found that the group taking favipiravir had a higher 7-day clinical recovery rate than the group taking umifenovir.16 The most common adverse events were liver enzyme abnormalities, psychiatric symptoms, gastrointestinal symptoms, and serum uric acid elevations, and it is associated with QT prolongation and teratogenic effects.
Protease Inhibitors
Lopinavir and Ritonavir (Kaletra): The replication of SARS-CoV-2 involves the cleavage of polyproteins into an RNA-dependent RNA polymerase and a helicase. This is achieved through two proteases: 3-chymotrypsin-like protease (3CLpro) and papain-like protease (PLpro).17 Lopinavir is a protease inhibitor of 3CLpro in vitro but is rapidly metabolized by the cytochrome P450 enzyme system. As such, is does not achieve sufficient bioavailability when administered orally.18 Ritonavir, another protease inhibitor, inhibits this metabolic effect and is therefore given concomitantly to boose the half-life of lopinavir.
LPVr is commercially available as Kaletra. It is FDA approved for the treatment of HIV type 1 in adult and pediatric patients.19 The recommended daily dose in adults is 800/200 mg in one or two divided doses. The use of Kaletra is contraindicated in patients with a known hypersensitivity to any of its components. There is a potential for drug interactions with drugs that are highly dependent on CYP3A for clearance or with CYP3A inducers. Commonly reported adverse effects include diarrhea, nausea, vomiting, hypertriglyceridemia, and hypercholesterolemia. The use of Kaletra is not recommended during lactation.
LPVr has previously shown a favorable clinical response with a decreased incidence of adverse clinical outcomes at Day 21, reduced viral load at 48 hours, decreased steroid use, and reduced incidence of nosocomial infections in SARS-CoV.20
On the basis of this, it has been tested in the management of SARS-CoV-2. A series of open-label trials, however, have shown no significant clinical benefit. The LOTUS China trial was the first reported randomized, controlled trial of LPVr.21 A moderately sized trial, it investigated the combination of lopinavir and ritonavir in SARS-CoV-2. A total of 199 patients were given either LPVr 400/100 mg twice daily for 14 days, in addition to SoC, or SoC alone. The study found no significant differences in time to clinical improvement or 28-day mortality.21 However, patients in the study group had a shorter stay in the ICU (median difference of 5 days) and shorter duration from randomization to hospital discharge (median difference of 1 day).21 The study did not find any significant differences for other outcomes such as duration of oxygen therapy, duration of hospitalization, and time from randomization to death. The authors concluded that LPVr treatment did not have a significant beneficial effect in the management of SARS-CoV-2 patients.21
The Randomised Evaluation of COVID-19 Therapy (RECOVERY) trial is a randomized, controlled, open-label trial investigating whether treatment with LPVr, hydroxychloroquine, corticosteroids (low-dose dexamethasone), azithromycin, convalescent plasma, synthetic neutralizing antibodies, or tocilizumab prevent death in patients with COVID-19. The LPVr arm of this trial was halted as it showed no improvement in outcomes of patients admitted to the hospital with COVID-19 in terms of 28-day mortality, duration of hospital stay, or risk of progressing to invasive mechanical ventilation or death.22
The SOLIDARITY trial is an international randomized clinical trial evaluating the effect of COVID-19 treatments on three important outcomes in COVID-19 patients: mortality, need for assisted ventilation, and duration of hospital stay. Interim published results show that remdesivir, hydroxychloroquine, LPVr, and interferon had little or no positive effect on the measured outcomes in hospitalized patients.23
It is possible that the typical doses of LPVr do not achieve the plasma drug concentrations required to inhibit SARS-CoV-2 replication.24 Furthermore, none of the studies with published results were blinded.
Endosomal Acidification Inhibitors
Chloroquine and Hydroxychloroquine (Plaquenil): Chloroquine and its analogue hydroxychloroquine are endosomal acidification inhibitors that increase the endosomal pH and, therefore, inhibit the fusion of SARS-CoV-2 and the host cell membranes.2,4 Additionally, chloroquine inhibits the glycosylation of the cellular ACE-2 receptor and, consequently, inhibits the binding of SARS-CoV-2 to the host cell.
Both of these agents are FDA-approved antimalarials; hydroxychloroquine is also FDA approved for the treatment of rheumatoid arthritis and lupus erythematosus.25 They have a narrow therapeutic window and toxicologic outcomes, including retinopathy, neuromyopathy, and cardiomyopathy after long-term use.26
In vitro studies have suggested a beneficial effect of chloroquine and hydroxychloroquine against SARS-CoV-2.27 This effect was observed clinically in a large retrospective cohort study conducted to evaluate the role of hydroxychloroquine therapy alone and in combination with azithromycin in hospitalized COVID-19 patients.28 However, many randomized clinical trials have shown otherwise.29 Bearing in mind the potential toxicities associated with the use of these agents, chloroquine and hydroxychloroquine are not recommended for use in COVID-19 patients.17,30-33 The TriACT trial is investigating the use of hydroxychloroquine in combination with ribavirin and nitazoxanide in COVID-19 patients (TABLE 1).
Nitazoxanide (Alinia): Nitazoxanide is a broad-spectrum antimicrobial prodrug that is rapidly converted to the active metabolites tizoxanide and tizoxanide conjugates.34 It is effective against various helminthic, protozoal, bacterial, and viral infections approved by the FDA for the oral treatment of diarrhea caused by Cryptosporidium parvum or Giardia lamblia.35 The recommended dose in adults is 500 mg of nitazoxanide every 12 hours for 3 days with food. Its use is contraindicated in patients with a known hypersensitivity to nitazoxanide or any of its components. The use of nitazoxanide is associated with abdominal pain, headache, chromaturia, and nausea.
Nitazoxanide has been shown to inhibit the replication of a broad range of respiratory viruses in cell cultures, including SARS-CoV-2.36 An early-stage, multicenter, randomized, double-blind, placebo-controlled trial examining the resolution of COVID-19 symptoms in patients receiving 500 mg of nitazoxanide three times daily for 5 days found no difference in resolution of symptoms between the test and control groups.37 However, the research team noted that nitazoxanide significantly reduced viral load and was safe in the dosages administered.
Membrane Fusion Inhibitors
Umifenovir (Arbidol): Umifenovir is a nonnucleoside antiviral drug that inhibits the contact, adhesion, and fusion of the viral lipid envelope by binding to and activating hemagglutinin protein in the host. It also demonstrates an immunomodulatory effect by inducing the body to produce interferon.2
Umifenovir is used is China and Russia to treat influenza and is associated with mild adverse effects, such as nausea, abdominal discomfort, and headache. Early studies have shown that umofenovir may inhibit SARS-CoV-2 infection in vitro; however, further studies have had conflicting results.38
While one retrospective study was unable to demonstrate an improvement in the prognosis of COVID-19 patients, another study revealed that umifenovir had a tendency to improve the discharging rate and decrease the mortality rate.39,40
A retrospective study to evaluate the antiviral effects and safety of LPVr and umifenovir in COVID-19 patients found that the umifenovir groups had a shorter viral load than the LPVr group (P <.01).38 However, another study comparing LPVr or umifenovir monotherapy with SoC in patients with mild-to-moderate COVID-19 showed no statistical difference between the treatment groups.41 Stronger randomized trials are needed to establish the place of umifenovir therapy in COVID-19 patients; however, there are currently no such studies being conducted in the U.S.
Ivermectin (Stromectol): Ivermectin is a broad-spectrum macrolide endectocide macrocyclic lactone isolated from the fermentation products of Streptomyces avermitili. It is FDA approved as an oral anthelmintic for strongyloidiasis of the intestinal tract and onchocerciasis.42 Ivermectin is known to have in vitro antiviral activity by inhibiting importin a/b-mediated nuclear transport and, therefore, preventing entry of viral proteins into the host nucleus to alter host-cell function. Recently, it demonstrated in vitro activity against SARS-CoV-2 by producing a 5,000-fold reduction in the viral-RNA at 48 hours of its single addition.43 A retrospective observational cohort study found that ivermectin was associated with a lower mortality during the treatment of COVID-19 than SoC (15% vs. 25.2%; P = .03), especially in patients with severe pulmonary involvement (38.8% vs. 80.7%; P = .001).34 The rate of successful extubation did not differ significantly.44
Conclusion
Pharmacists play a significant part not only in ensuring a regular supply of medications that are approved or under trials but also in managing individual patient therapies as more agents gain approval for use in COVID-19 patients. A considerable amount of work remains to be done to establish safe and effective therapies for the management of patients. In the meantime, pharmacists can continue to educate themselves by keeping abreast of the new developments in the field and build upon the information provided in this article.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
REFERENCES
1. Sanders JM, Monogue ML, Jo
2. Wang D, Li Z, Liu Y. An overview of the safety, clinical application and antiviral research of the COVID-19 therapeutics. J Infect Public Health. 2020;13(10):1405-1414.
3. Abd El-Aziz TM, Stockand JD. Recent progress and challenges in drug development against COVID-19 coronavirus (SARS-CoV-2)–an update on the status. Infect Genet Evol. 2020;83:104327.
4. NIH. ClinicalTrials.gov. http://www.clinicaltrials.gov. Accessed November 19, 2020.
5. FDA News Release. COVID-19 Update: FDA broadens emergency use authorization for Veklury (remdesivir) to include all hospitalized patients for treatment of COVID-19. www.fda.gov/news-events/press-announcements/covid-19-update-fda-broadens-emergency-use-authorization-veklury-remdesivir-include-all-hospitalized. August 28, 2020. Accessed November 18, 2020.
6. Beigel JH, Tomashek KM, Dodd LE, et al. Remdesivir for the treatment of Covid-19–final report. N Engl J Med. 2020;383(19):1813-1826.
7. Goldman JD, Lye DCB, Hui DS, et al. Remdesivir for 5 or 10 days in patients with severe Covid-19. N Engl J Med. 2020;383(19):1827-1837.
8. Spinner CD, Gottlieb RL, Criner GJ, et al. Effect of remdesivir vs standard care on clinical status at 11 days in patients with moderate COVID-19: a randomized clinical trial. JAMA. 2020;324(11):1048-1057.
9. Veklury [package insert]. Foster City, CA: Gilead Sciences; 2020. www.accessdata.fda.gov/drugsatfda_docs/label/2020/214787Orig1s000lbl.pdf. Accessed November 18, 2020.
10. Cennimo D. Coronavirus disease 2019 (COVID-19) treatment and management. Medscape. November 16, 2020. Accessed November 17, 2020. https://emedicine.medscape.com/article/2500114-treatment#showall.
11. Khalili JS, Zhu H, Mak NSA, et al. Novel coronavirus treatment with ribavirin: groundwork for an evaluation concerning COVID-19. J Med Virol. 2020;92(7):740-746.
12. Copegus [package insert]. South San Francisco, CA: Genentech USA; 2011. www.accessdata.fda.gov/drugsatfda_docs/label/2011/021511s023lbl.pdf. Accessed November 17, 2020.
13. Elfiky AA. Anti-HCV, nucleotide inhibitors, repurposing against COVID-19. Life Sci. 2020;248:117477.
14. Coomes EA, Haghbayan H. Favipiravir, an antiviral for COVID-19? J Antimicrob Chemother. 2020;75(7):2013-2014.
15. Cai Q, Yang M, Liu D, et al. Experimental treatment with favipiravir for COVID-19: an open-label control study. Engineering (Beijing). 2020;6:1192-1198.
16. Chen C, Huang J, Zhang Y, et al. Favipiravir versus arbidol for COVID-19: a randomized clinical trial. www.medrxiv.org/content/medrxiv/early/2020/04/15/2020.03.17.20037432.full.pdf. medRxiv; 2020. Accessed November 10, 2020.
17. NIH. COVID-19 treatment guidelines. www.covid19treatmentguidelines.nih.gov/. Accessed November 10, 2020.
18. Lythgoe MP, Mid
19. Kaletra [package insert]. North Chicago, IL: AbbVie Inc.; 2016. www.accessdata.fda.gov/drugsatfda_docs/label/2016/021251s052_021906s046lbl.pdf. Accessed November 13, 2020.
20. Chu CM, Cheng VC, Hung IF, et al. Role of lopinavir/ritonavir in the treatment of SARS: initial virological and clinical findings. Thorax. 2004;59(3):252-256.
21. Cao B, Wang Y, Wen D, et al. A trial of lopinavir-ritonavir in adults hospitalized with severe Covid-19. N Engl J Med. 2020;382(19):1787-1799.
22. RECOVERY Collaborative Group. Lopinavir-ritonavir in patients admitted to hospital with COVID-19 (RECOVERY): a randomised, controlled, open-label, platform trial. Lancet. 2020;396(10259):1345-1352.
23. Pan H, Peto R, Karim QA, et al. WHO Solidarity trial consortium. Repurposed antiviral drugs for COVID-19–interim WHO SOLIDARITY trial results. medRxiv. Preprint. www.medrxiv.org/content/10.1101/2020.10.15.20209817v1. Accessed November 11, 2020.
24. Schoergenhofer C, Jilma B, Stimpfl T, et al. Pharmacokinetics of lopinavir and ritonavir in patients hospitalized with coronavirus disease 2019 (COVID-19). Ann Intern Med. 2020;173(8):670-672.
25. Aralen [package insert]. Bridgewater, NJ: Sanofi-Aventis; 2017. www.accessdata.fda.gov/drugsatfda_docs/label/2017/006002s044lbl.pdf. Accessed November 2, 2020.
26. Plaquenil [package insert]. Oakville, Ontario, Canada: Concordia Pharmaceuticals; 2017. www.accessdata.fda.gov/drugsatfda_docs/label/2017/009768s037s045s047lbl.pdf. Accessed November 3, 2020.
27. Liu J, Cao R, Xu M, et al. Hydroxychloroquine, a less toxic derivative of chloroquine, is effective in inhibiting SARS-CoV-2 infection in vitro. Cell Discov. 2020;6:16.
28. Arshad S, Kilgore P, Chaudhry ZS, et al. Treatment with hydroxychloroquine, azithromycin, and combination in patients hospitalized with COVID-19. Int J Infect Dis. 2020;97:396-403.
29. Horby P, Mafham M, Linsell L, et al. Effect of hydroxychloroquine in hospitalized patients with COVID-19: preliminary results from a multi-centre, randomized, controlled trial. medRxiv. 2020; Preprint. www.medrxiv.org/content/10.1101/2020.07.15.20151852v1. Accessed November 10, 2020.
30. Cavalcanti AB, Zampieri FG, Rosa RG, et al. Hydroxychloroquine with or without azithromycin in mild-to-moderate Covid-19 [published correction in N Engl J Med. 2020 Nov 19;383(21):e119]. N Engl J Med. 2020;383(21):2041-2052.
31. Furtado RHM, Berwanger O, Fonseca HA, et al. Azithromycin in addition to standard of care versus standard of care alone in the treatment of patients admitted to the hospital with severe COVID-19 in Brazil (COALITION II): a randomised clinical trial. Lancet. 2020;396(10256):959-967.
32. Geleris J, Sun Y, Platt J, et al. Observational study of hydroxychloroquine in hospitalized patients with Covid-19. N Engl J Med. 2020;382(25):2411-2418.
33. Rosenberg ES, Dufort EM, Udo T, et al. Association of treatment with hydroxychloroquine or azithromycin with in-hospital mortality in patients with COVID-19 in New York State. JAMA. 2020;323(24):2493-2502.
34. Kelleni MT. Nitazoxanide/azithromycin combination for COVID-19: a suggested new protocol for early management. Pharmacol Res. 2020;157:104874.
35. Alinia [package insert]. Tampa, FL: Romark Pharmaceuticals; 2016. Accessed November 12, 2020. https://www.accessdata.fda.gov/drugsatfda_docs/label/2016/021497s001,021498s004lbl.pdf.
36. Al-Horani RA, Kar S. Potential anti-SARS-CoV-2 therapeutics that target the post-entry stages of the viral life cycle: a comprehensive review. Viruses. 2020;12(10):1092.
37. Rocco PRM, Silva PL, Cruz FF, et al. Early use of nitazoxanide in mild Covid-19 disease: randomized, placebo-controlled trial. medRxiv. 2020; Preprint. www.medrxiv.org/content/10.1101/2020.10.21.20217208v1. Accessed November 10, 2020.
38. Wang X, Cao R, Zhang H, et al. The anti-influenza virus drug, arbidol is an efficient inhibitor of SARS-CoV-2 in vitro. Cell Discov. 2020;6:28.
39. Lian N, Xie H, Lin S, et al. Umifenovir treatment is not associated with improved outcomes in patients with coronavirus disease 2019: a retrospective study. Clin Microbiol Infect. 2020;26(7):917-921.
40. Wang Z, Yang B, Li Q, et al. Clinical features of 69 cases with coronavirus disease 2019 in Wuhan, China. Clin Infect Dis. 2020;71(15): 769-777.
41. Li Y, Xie Z, Lin W, et al. Efficacy and safety of lopinavir/ritonavir or arbidol in adult patients with mild/moderate COVID-19: an exploratory randomized controlled trial [published online ahead of print, 2020 May 19]. Med (N Y). 2020;10.1016.
42. Stromectol [package insert]. Kenilworth, NJ: Merck & Co., Inc. www.accessdata.fda.gov/drugsatfda_docs/label/2008/050742s022lbl.pdf. Accessed November 14, 2020.
43. Caly L, Druce JD, Catton MG, et al. The FDA-approved drug ivermectin inhibits the replication of SARS-CoV-2 in vitro. Antiviral Res. 2020;June(178):104787.
44. Rajter JC, Sherman MS, Fatteh N, et al. Use of ivermectin is associated with lower mortality in hospitalized patients with coronavirus disease 2019: The ICON Study [published online ahead of print, 2020 Oct 13]. Chest. 2020;S0012-3692(20)34898-4.
To comment on this article, contact rdavidson@uspharmacist.com.






