US Pharm. 2007;32(8):HS26-HS37.
Iron deficiency anemia, a microcytic anemia, is the most prevalent deficiency condition in the world. It occurs when iron deficiency is so severe that it diminishes erythropoiesis (production of red blood cells), causing anemia. In healthy people, absorptive cells in the proximal small intestine, which changes iron absorption to match loss of iron in the body, carefully regulate iron concentration in the body.1
Iron deficiency anemia affects an individual's ability to perform physical activities and impairs growth and learning in children. In general, iron imbalance leads to either iron deficiency anemia or hemosiderosis; both are disorders with potential adverse consequences.
Diet and socioeconomic factors have an important role in iron deficiency, and, as a result, it is more commonly observed in people of various racial backgrounds living in poorer areas of the world.
Chronic iron deficiency anemia is rarely a direct cause of death; however, moderate or severe iron deficiency anemia can produce sufficient hypoxia to aggravate underlying pulmonary and cardiovascular disorders.1
Pharmacists have an important role in consulting with patients about different OTC iron products and can refer patients to a clinician to further diagnose the underlying causes if signs and symptoms of severe anemia are observed.
Pathophysiology
Iron deficiency develops in
several stages. In the first stage, body iron requirement exceeds iron intake,
causing progressive depletion of bone marrow iron stores. As iron reservoirs
decrease, compensatory increases in absorption of dietary iron occur. During
later stages, deficiency is severe enough to impair red blood cell
biosynthesis, leading to anemia. Iron deficiency, if severe and prolonged, may
cause dysfunction of iron-containing cellular enzymes, which may contribute to
fatigue and loss of stamina via mechanisms independent of the anemia itself.
2
Iron deficiency anemia must be differentiated from other types of microcytic anemia, such as anemia caused by deficient erythropoiesis or decreased red blood cell production due to other underlying causes. If tests exclude iron deficiency in a patient with microcytic anemia, then anemia of chronic disease, structural hemoglobin abnormalities (e.g., hemoglobinopathies), and congenital red blood cell membrane abnormalities are considered. Clinical laboratory studies of hemoglobin electrophoresis and HbA 2, as well as genetic testing (e.g., alpha-thalassemia), may help distinguish these entities.2
Diagnosis
When iron deficiency anemia is
suspected in patients with chronic blood loss or microcytic anemia, complete
blood count (CBC), serum iron, iron-binding capacity (transferrin), and serum
ferritin are measured. Serum iron concentration is typically low in patients
with iron deficiency or chronic diseases and elevated in patients with
hemolytic disorders and iron-overload syndromes. Usually, serum iron and
iron-binding capacity are both tested, because their relationship is
important; iron-binding capacity increases in iron deficiency. Iron deficiency
in the absence of anemia is asymptomatic.2
Among healthy individuals, serum iron levels are 75 to 150 mcg/dL in men and 60 to 140 mcg/dL in women; total iron-binding capacity is 250 to 450 mcg/dL. Patients taking oral iron may have normal serum iron despite a deficiency; in these cases, a valid test requires cessation of iron therapy for 24 to 48 hours. Serum ferritin concentrations closely correlate with total body iron stores. The normal range in most laboratories is 30 to 300 ng/mL; the mean serum ferritin level is 88 ng/mL in men and 49 ng/mL in women. Low concentrations (<12 ng/mL) are specific for iron deficiency.
Iron deficiency anemia is primarily a laboratory diagnosis, and, therefore, a carefully obtained patient history will normally lead to its recognition. The history can be useful in establishing the etiology of the anemia and estimating its duration.
Vegetarians are more likely to develop iron deficiency, unless their diet is supplemented with iron. National programs of dietary iron supplementation are initiated in many areas of the world where meat is sparse and iron deficiency anemia is prevalent.
In addition to the usual manifestations of anemia, some uncommon symptoms occur in severe iron deficiency; a patient may have pica, a compulsive eating of or craving for nonnutritive substances (e.g., ice, dirt, paint). Clay eating, specifically, may help the diagnosis.3
Body Iron Requirement
Total body iron is about 3.5 g in
healthy men and 2.5 g in healthy women; the difference between men and women
relates to body size, lower androgen levels, and the dearth of stored iron in
women due to menses- and pregnancy-associated iron loss. The distribution of
body iron in an average man is 2,100 mg in hemoglobin, 200 mg in myoglobin,
150 mg in tissue (heme and nonheme) enzymes, and 3 mg in transport-iron
compartment. Iron is stored in cells and plasma as ferritin (700 mg) and
hemosiderin (300 mg).4
It is important to maintain equilibrium between iron absorption and iron loss in the body to ensure multiple metabolic processes, such as oxygen transport, DNA synthesis, and electron transport. On a day-to-day basis, the body absorbs more iron than it loses; therefore, loss of body iron is a more passive process than absorption. It is important to remember that consistent errors in maintaining this equilibrium lead to either iron deficiency or iron overload.
The average American diet, which contains 6 mg of elemental iron per kcal of food, is adequate for iron homeostasis. Of about 15 mg per day of dietary iron, adults absorb only 1 mg, which is the approximate amount lost daily by cell destruction. In iron depletion, absorption increases, although the exact signaling mechanism is unknown; however, absorption rarely increases to more than 6 mg per day unless supplemental iron is added. Children have a greater need for iron and appear to absorb more to meet this need.
Iron is absorbed in the proximal small intestine. Iron uptake occurs by three separate pathways: the heme pathway and two separate pathways for ferric and ferrous iron. Ferric iron utilizes a different pathway to enter cells than does ferrous iron. Which pathway transports the most nonheme iron in humans is unknown. Most nonheme dietary iron is ferric iron. Heme and nonheme iron uptake by intestinal absorptive cells is noncompetitive.
Iron from the intestinal mucosal cell is transferred to transferrin, an iron-transport protein synthesized in the liver; transferrin can transport iron from cells (intestinal, macrophages) to specific receptors on erythroblasts, placental cells, and liver cells. For heme synthesis, transferrin transports iron to the erythroblast mitochondria, which insert the iron into protoporphyrin for it to become heme. Transferrin (plasma half-life, eight days) is recycled for reutilization. Synthesis of transferrin increases with iron deficiency but decreases with any type of chronic disease.
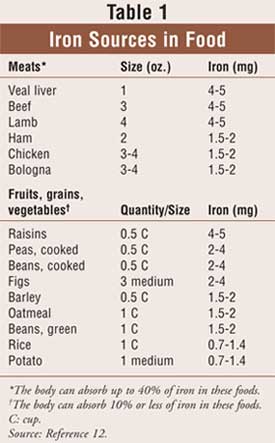
Absorption of iron is determined by the type of iron molecule and by other substances that are ingested. Iron absorption is best when food contains heme iron (e.g., meat). Dietary nonheme iron must be reduced to the ferrous state and released from food binders by gastric secretions. Nonheme iron absorption is reduced by other food items (e.g., vegetable fiber phytates and polyphenols; tea tannates, including phosphoproteins; bran) and certain antibiotics (e.g., tetracycline). Table 1 lists common food sources of iron. Ascorbic acid is the only common food element known to increase nonheme iron absorption. Heme and nonheme iron are absorbed into the enterocyte noncompetitively.4,5
Because iron absorption is so limited, the body recycles and conserves iron. Transferrin grasps and recycles available iron from aging red blood cells undergoing phagocytosis by mononuclear phagocytes. This mechanism provides about 97% of the daily iron needed (~25 mg iron). Iron stores tend to increase as age increases, because iron elimination slows down.
Causes of Iron Deficiency
Two thirds of body iron is
present in circulating red blood cells as hemoglobin. One gram of hemoglobin
contains 3.47 mg of iron; thus, 1 mL of blood lost from the body (hemoglobin,
15 g/dL) results in a loss of 0.5 mg of iron. Bleeding is the most common
cause of iron deficiency in the UnitedStates and Europe.6
Iron deficiency caused solely by diet is uncommon in adults in countries where meat is an important part of the diet. Depending upon the criteria used for the diagnosis of iron deficiency, approximately 4% to 8% of premenopausal women are iron deficient. In countries where little meat is consumed, iron deficiency anemia is six to eight times more prevalent than in the UnitedStates and Europe. This occurs despite consumption of a diet that contains an equivalent amount of total dietary iron, because heme iron is absorbed better from the diet than nonheme iron. In certain geographic areas, intestinal parasites, particularly hookworm, worsen iron deficiency due to blood loss in the gastrointestinal tract. Anemia is more profound among children and premenopausal women in these environs.1,6
Because the average woman eats less than the average man does, she must be more than twice as efficient in absorbing dietary iron in order to maintain equilibrium and avoid developing iron deficiency anemia. A woman loses about 500 mg of iron with each pregnancy. Menstrual iron loss is highly variable, ranging from 10 to 250 mL (4-100 mg of iron) per period. Menstrual iron loss doubles the need for women to absorb iron, compared with men.
Healthy men lose body iron in sloughed epithelium, in secretions from the skin and gut lining, and from small, daily loss of blood from the gastrointestinal tract (0.7 mL of blood daily); cumulatively, this amounts to 1 mg of iron. Men with severe siderosis from blood transfusions can lose a maximum of 4 mg daily via these routes without additional blood loss.
Healthy newborn infants have a total body iron level of 250 mg (80 ppm), which is obtained from maternal sources. Infants consuming cow's milk have a greater incidence of iron deficiency, because bovine milk has a higher concentration of calcium, which competes with iron for absorption. Subsequently, growing children must obtain approximately 0.5 mg more iron than is lost daily in order to maintain a normal body concentration of 60 ppm.
Prolonged achlorhydria may produce iron deficiency because acidic conditions are required to release ferric iron from food. Then, it can be chelated with mucins and other substances (e.g., sugars, amino acids, amides) to keep it soluble and available for absorption in the more alkaline duodenum.6,7
Laboratory Tests
The severity of the anemia can be
documented by a CBC. In chronic iron deficiency anemia, the cellular indices
show a microcytic and hypochromic erythropoiesis; both the mean corpuscular
volume (MCV) and mean corpuscular hemoglobin concentration (MCHC) have values
below the normal range for the laboratory performing the test. Reference range
values for the MCV and MCHC are 83 g/dL to 97 g/dL and 32 g/dL to 36 g/dL,
respectively. Often, the platelet count is elevated (>450,000/mcL); this
normalizes following iron therapy. The white blood cell count is usually
within reference ranges (4,500-11,000/mcL).8
If a CBC is obtained after blood loss, the cellular indices do not enter the abnormal range until most of the erythrocytes produced before the bleeding are destroyed at the end of their normal lifespan (120 days).
Examination of the peripheral smear is an important part of the workup of patients with anemia. Examination of the erythrocytes shows microcytic and hypo chromic red blood cells in chronic iron deficiency anemia. The microcytosis is apparent in the smear long before the MCV is decreased following an event that produces iron deficiency. Platelets are usually increased in this disorder.
A bone marrow aspirate can be used to diagnose iron deficiency. The absence of stainable iron in a bone marrow aspirate that contains spicules and the presence of stainable iron in a simultaneous control specimen permit establishment of a diagnosis of iron deficiency without other laboratory tests.
Other laboratory tests are useful to establish the etiology of iron deficiency anemia and to exclude or establish a diagnosis of one of the other microcytic anemias.9
Pharmacotherapy
Iron therapy without pursuit of
the cause of iron deficiency is a poor practice. The response to treatment is
assessed by serial hemoglobin measurements until normal red blood cell values
are achieved. Hemoglobin rises slightly for two weeks, then rises by 0.7 to 1
g per week until near normal, at which time rate of increase tapers. The
normal range is 3.0 mcg/mL to 8.5 mcg/mL. Normally, anemia should be corrected
within two months. A subnormal response suggests continued hemorrhage,
underlying infection or malignancy, insufficient intake of iron, or very
rarely, malabsorption of oral iron. The most sensitive and specific criterion
for iron-deficient erythropoiesis, however, is absent marrow stores of iron,
although a bone marrow examination is rarely needed. During iron therapy, the
anemia and iron panels need to be monitored.8
Iron supplements are used to provide adequate iron for hemoglobin synthesis and to replenish body stores of iron. Recommended dosages of iron are administered prophylactically during pregnancy due to anticipated requirements of the fetus and iron loss that occurs during delivery.10
Oral Iron Products
The most economical and effective
medication in the treatment of iron deficiency anemia is oral ferrous iron
salts. Among the various iron salts, ferrous sulfate is used most commonly.
However, claims have been made that other iron salts are absorbed better and
have less morbidity. Generally, the toxicity is proportional to the amount of
iron available for absorp tion. If the quantity of iron in the test dose is
decreased, the percentage of the test dose absorbed is increased, but the
quantity of iron absorbed is diminished.
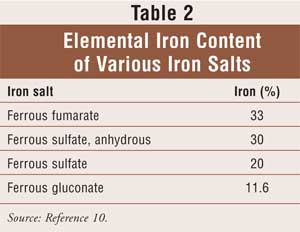
Iron can be provided by various iron salts (e.g., ferrous sulfate, gluconate, fumarate) or by saccharated iron given 30 minutes before meals (food or antacids may reduce absorption). A typical initial dosage is 60 mg of elemental iron (i.e., 325 mg of ferrous sulfate) given one or two times per day. Larger doses are unabsorbed and increase the occurrence of adverse effects, especially dark stool, constipation, and nausea. Ascorbic acid, in the form of a pill (500 mg) or orange juice, enhances iron absorption without increasing gastric distress when taken with iron.10 The elemental iron content of various iron salts is listed in Table 2.
For adults, the recommended daily dosage of oral iron products is 2 to 3 mg/kg of elemental iron (divided into three doses). For slow-release tablets, the recommended dosage is 50 to 100 mg of elemental iron per day.
Recommended dosages in infants and children vary according to age. For premature infants, the recommended dosage is 2 to 4 mg/kg per day of elemental iron (one dose; if not tolerated, then divided into two doses), with a maximum dosage of 15 mg per day. For full-term infants and children, the recommended dosage is 3 to 6 mg/kg per day of elemental iron (one dose; if not tolerated, then divided into two or three doses). When it is used as prophylaxis, premature infants should receive 2 mg/kg elemental iron (one dose; if not tolerated, then divided into two or three doses), with a maximum dosage of 15 mg per day; full-term infants should receive 1 to 2 mg/kg of elemental iron per day (one dose; if not tolerated, then divided into two or three doses), with a maximum of 15 mg per day.
The recommended dietary allowance is 8 mg per day in men, 18 mg per day in women ages 19 to 50, 8 mg per day in women ages 51 and older, 27 mg/day in women who are pregnant, and 9 mg per day in women ages 18 and older who are lactating.
Parenteral Iron Products
Parenteral iron causes the same
therapeutic response as oral iron but can cause adverse effects, such as
anaphylactoid reactions, serum sickness, thrombo phle bitis, and pain. It is
reserved for patients who cannot tolerate or will not take oral iron or for
patients who steadily lose large amounts of blood because of capillary or
vascular disorders. A hematologist can determine the proper dosage of
parenteral iron. To replenish tissue stores, oral or parenteral iron therapy
should continue for six months or longer after correcting hemoglobin levels.
It is important to remember that parenteral iron therapy is expensive and has
greater morbidity than oral preparations of iron.
Iron Dextran (Dexferrum, Infed; 50 mg/mL): The recommended daily dose of iron dextran for adults who weigh more than 50 kg is 100 mg per day. The recommended daily dose of iron dextran for children between 5 to 15 kg is 50 mg per day and for those 15 to 50 kg is 100 mg per day.11
A test dose of 0.5 mL (25 mg) is required prior to the first therapeutic dose. At least one hour should elapse after the test dose before the therapeutic dose is given intravenously. The test dose must be administered slowly over at least five minutes. Hemoglobin, hematocrit, serum iron, total iron-binding capacity, saturation percentage of transferrin, reticulocyte count, and blood pressure should be carefully monitored. Iron dextran is a complex of ferric oxyhydroxide and a polyglucose that restores hemoglobin and depleted iron through the action of its iron component, which forms hemosiderin or ferritin and transferrin by binding to protein moieties.
Iron Sucrose (Venofer, 20 mg/mL): The dosage of iron sucrose for adults with chronic renal impairment who are receiving erythropoietin is 100 mg per consecutive hemodialysis session. The bolus dose is given as an undiluted solution of 100 to 200 mg over two to five minutes. The infusion is given as 100 mg diluted in 0.9% normal saline (100 mL) over 15 minutes.10,11
Hemoglobin, hematocrit, serum ferritin, transferrin saturation, and blood pressure should be monitored. Iron sucrose dissociates to its iron and sucrose components where it increases iron and ferritin levels and decreases total iron-binding capacity. Transfusion of packed red blood cells should be reserved for patients with significant acute bleeding or for those in danger of hypoxia and/or coronary insufficiency.
Summary
Iron deficiency is the most
common cause of anemia. Iron is needed by the human body to form hemoglobin.
Iron deficiency can usually be corrected with proper diet, iron supplementation, and pharmacotherapy. Oral iron ferrous salts and, in severe cases, parenteral iron complexes can be given to provide adequate iron for hemoglobin synthesis. Sometimes, additional treatments are necessary, especially if there are other reasons for iron deficiency anemia.
References
1. Centers for
Disease Control and Prevention. Iron deficiency-United States, 1999-2000.
MMWR Morb Mortal Wkly Rep. 2002;51:897-899.
2. Cook JD. Diagnosis
and management of iron-deficiency anaemia. Best Pract Res Clin Haematol
. 2005;18:319-332.
3. Cook JD. Newer
aspects of the diagnosis and treatment of iron deficiency. American Society of
Hematology Educational Program Book. 2003:40-61.
4. Looker AC, Dallman
PR, Carrol MD, et al. Prevalence of iron deficiency in the United States.
JAMA. 1997;277:973-976.
5. Hallberg L, Brune M,
Rossander L. Effect of ascorbic acid on iron absorption from different types
of meals. Studies with ascorbic-acid-rich foods and synthetic ascorbic acid
given in different amounts with different meals. Hum Nutr Appl Nutr.
1986;40:97-113.
6. Duffy T. Microcytic
and hypochromic anemias. In: Cecil RL, Goldman L, Ausiello DA. Cecil
Textbook of Medicine. 22nd ed. Philadelphia, Pa: Saunders; 2004:1008.
7. Iron-deficiency
anemia. In: Hillman RS, Ault KA. Hematology in Clinical Practice. 3rd
ed. New York, NY: McGraw-Hill; 2002:51-61.
8. Conrad ME. Iron
deficiency anemia. Availble at: www.emedicine.com/med/topic1188.htm. Accessed
June 10, 2007.
9. The Merck Manuals
Online Medical Library. Iron Deficiency Anemia. Available at:
www.merck.com/mmpe/sec11/ch130/ch130b.html. Accessed May 27, 2007.
10. Micromedex
Healthcare Series, 2007. Thomson Healthcare Inc.
11. Barton JC, Barton
EH, Bertoli LF, et al. Intravenous iron dextran therapy in patients with iron
deficiency and normal renal function who failed to respond to or did not
tolerate oral iron supplementation. Am J Med. 2000;109:27-32.
12. Ohio State
University Extension fact sheet: human nutrition. Available at:
ohioline.osu.edu/hyg-fact/5000/5559.html. Accessed July 13, 2007.
To comment on this article, contact editor@uspharmacist.com






