In aging adults, the vocal cords grow weaker, resulting in presbylarynx, a change in the pitch of the voice.1 A senior woman’s voice may become lower in pitch and huskier, while a higher pitch and thinner voice may be produced by senior men. As the vocal cords weaken in older adults, it becomes more common for hoarseness to accompany colds or excessive voice use.1 The potential significance of hoarseness, particularly when persistent or progressive, should be appreciated by all health care practitioners. Hoarseness is caused by abnormal vocal fold (cord) vibration. The quality of the voice may be breathy, harsh, rough, or low-pitched. When more than 2 to 3 weeks of hoarseness persists, evaluation of the patient by an otolaryngologist, commonly referred to as an ear, nose, and throat (ENT) specialist, is required; the examination should include laryngoscopy to rule out malignancy or other serious conditions.2,3
Serious causes of hoarseness include
tumors, nodules, and lung cancer, especially in patients with a history
of tobacco use. Additionally, functional causes (e.g., muscle tension
dysphonia, spasmodic dysphonia) should be considered. Gastroesophageal
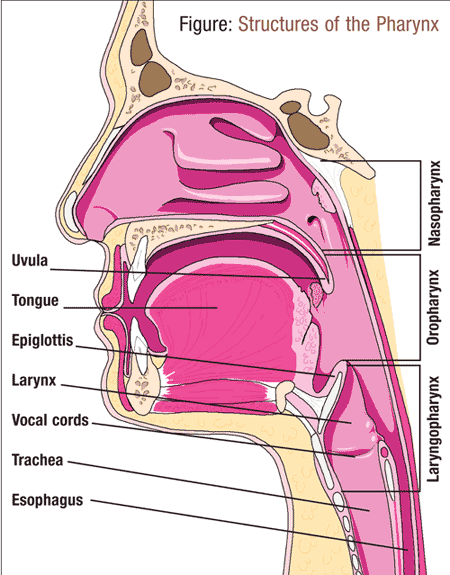
reflux into the larynx (located between the trachea and the base of the
tongue; see FIGURE), referred to as laryngopharyngeal reflux
(LPR), is also considered a cause of chronic hoarseness when other
causes of abnormal vocal fold vibration have been excluded via
laryngoscopy.2
Examination of the larynx is especially important in patients with suspected LPR since there appears to be an association of LPR and upper aerodigestive tract cancer.4,5 Of note, laryngitis is a nonspecific designation referring to inflammation of the larynx that is typically mild and resolves spontaneously; persistent laryngitis must be further defined based on the most likely etiologic factors, which include infection (viral or bacterial), allergy, vocal trauma, postnasal discharge, and LPR.3
Symptoms
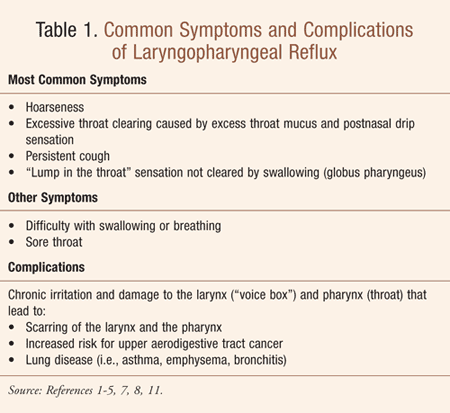
The most common LPR symptoms (TABLE 1) are hoarseness, throat clearing, persistent cough, and sensation of a lump in the throat.6 Other symptoms and complications are listed in TABLE 1. LPR differs from gastroesophageal reflux disease (GERD) in that it is frequently not associated with heartburn and regurgitation.7 Fewer than 50% of patients with laryngeal acid exposure have typical symptoms of heartburn and regurgitation; thus, the term silent reflux has been used to refer to LPR. Lack of such symptoms, however, should not give rise to the elimination of this cause of hoarseness.2
Since most patients with symptomatic LPR
do not meet criteria for GERD by pH probe testing, clinicians are
advised to consider these conditions as separate entities.2
However, it should be noted that GERD has been suggested as a
contributing factor to symptoms such as throat clearing and discomfort,
persistent cough, postnasal drip sensation, esophageal spasm, and
certain cases of asthma.2
Diagnosis
LPR is harder to diagnose than GERD; a combination of history, physical examination, and one or more tests (i.e., endoscopy exam, 24-hour pH monitoring) is required.8 Testing is important to confirm a diagnosis of LPR and to assess the magnitude of the problem.3
Twenty-four-hour pH monitoring of the pharynx, which should best identify LPR, is advocated by some as the initial management step, but is costly, more difficult, and less readily available than lower esophageal monitoring alone (lower esophageal monitoring does not correlate well with symptoms of LPR).2 Double esophageal pH probe (proximal and distal) testing is currently considered the standard of care for evaluation of LPR (see Resource).1 While a practical alternative to an initial pH study consists of placing patients on an empirical trial of a proton pump inhibitor (PPI; see Pharmacologic Treatment below), this trial should not precede excluding other causes of hoarseness through the visualization of the vocal cords.2

Management
While some LPR patients will respond to conservative behavioral management in conjunction with pharmacologic therapy, as seen with the treatment of GERD, most patients with LPR, unlike those with GERD, require more aggressive and prolonged treatment to reach regression of symptoms and laryngeal tissue changes.3 In selected refractory cases (i.e., with laxity of gastroesophageal sphincter), surgical intervention is useful, by either laparoscopic or traditional open surgery fundoplication.3,8
Conservative Behavioral Management: Also known as lifestyle modification, conservative behavioral management is a self-care intervention. Recommended behavioral changes for LPR (TABLE 2) appear to be an independently significant variable in determining response to medical management.3,9

Pharmacologic Treatment: Suppression of gastric acid is best accomplished with a PPI (omeprazole, lansoprazole, rabeprazole, pantoprazole, dexlansoprazole, or esomeprazole); these agents are the mainstay of empirical and medical treatment, although there is controversy regarding their efficacy.3,10,11 The American Academy of Otolaryngology—Head and Neck Surgery recommends full-strength, twice-daily PPI therapy (e.g., omeprazole 40 mg orally twice daily, or equivalent) for a minimum of 3 months.3 While improvement may be subjectively noted by patients after 3 months, it often requires 6 months for changes in the larynx to resolve.12 If a patient shows improvement with subsequent return of symptoms after cessation of therapy, reintroduction of a PPI is warranted at the lowest dose shown effective for remission (typically daily); but the PPI may be used intermittently on a demand basis.2 Compared with GERD, LPR usually requires more aggressive and prolonged treatment to achieve resolution.7,13 Adverse effects of PPIs need to be considered, including an increased risk of gastrointestinal infections, osteoporosis-related bone fractures of the hip, spine, or wrist, and hypomagnesemia.11 Histamine2-receptor antagonists, while considered an alternative to PPIs, are generally less clinically effective and less cost-effective.2 Patients who do not respond to medical management should undergo pH testing and manometry.
Prokinetic agents may be used to increase peristalsis and increase the pressure of the lower esophageal sphincter; their utility is limited due to the risk for adverse effects such as cardiac arrhythmias and diarrhea. Sucralfate, a mucosal cytoprotectant, may be used to protect injured mucous membranes.8 While antacids are more commonly used for symptoms of heartburn, they may be employed to help neutralize acid.
Conclusion
It is important for clinicians to understand the potential significance of persistent hoarseness and not overlook other symptoms of LPR, such as excessive throat clearing, persistent cough, and a “lump in the throat” sensation. Pharmacists should raise awareness of the behavioral modifications and pharmacologic interventions that improve symptoms and resolve changes in the larynx.
REFERENCES
1. Beers MH, Jones TV, Berkwits M, et al, eds. The Merck Manual of Health & Aging. Whitehouse Station, NJ: Merck Research Laboratories; 2004:483-486.
2. Lustig LR, Schindler JS. Ear, nose, & throat disorders. In: McPhee SJ, Papadakis MA, Rabow MW, eds. 2012 Current Medical Diagnosis & Treatment. 51st ed. New York, NY: McGraw Hill Medical; 2012:230-231.
3. Ford C. Evaluation and management of laryngopharyngeal reflux. JAMA. 2005;294(12):1534-1540.
4. Reavis KM, Morris CD, Gopal DV, et al.
Laryngopharyngeal reflux symptoms better predict the presence of
esophageal adenocarcinoma than typical gastroesophageal reflux symptoms.
Ann Surg. 2004;239:849-856.
5. Morrison MD. Is chronic gastroesophageal
reflux a causative factor in glottis carcinoma? Otolaryngol Head Neck Surg. 1988;993:370-373.
6. Book DT, Rhee JS, Toohill RJ, et al. Perspectives in laryngopharyngeal reflux: an international survey. Laryngoscope. 2002;112:1399-1406.
7. Koufman JA, Aviv JE, Casiano R, Shaw GY.
Laryngopharyngeal reflux: position statement of the Committee on Speech,
Voice, and Swallowing Disorders of the American Academy of
Otolaryngology—Head and Neck Surgery. Otolaryngol Head Neck Surg. 2002;127(1):32-35.
8. Laryngopharyngeal reflux (silent reflux). WebMD. Reviewed June 15, 2010. www.webmd.com/heartburn-gerd/laryngopharyngeal-reflux-silent-reflux. Accessed July 30, 2012.
9. Steward DL, Wilson KM, Kelly DH, et al. Proton pump
inhibitor therapy for chronic laryngo-pharyngitis: a randomized
placebo-control trial. Otolaryngol Head Neck Surg. 2004;131:342-350.
10. Epocrates, Version 4.5. Epocrates, Inc. www.epocrates.com. Accessed October 22, 2012.
11. Semla TP, Beizer JL, Higbee MD. Geriatric Dosage Handbook. 17th ed. Hudson, OH: Lexi-Comp, Inc; 2012.
12. Hanson DG, Jiang JJ. Diagnosis and management of chronic laryngitis associated with reflux. Am J Med. 2000;108(suppl 4a):112S-119S.
13. Park W, Hicks DM, Khandwala F, et al.
Laryngopharyngeal reflux: prospective cohort study evaluating optimal
dose of proton-pump inhibitor therapy and pretherapy predictors of
response. Laryngoscope. 2005;115:1230-1238.
To comment on this article, contact rdavidson@uspharmacist.com.





