Hypertension is one of the most common chronic medical conditions in the United States, affecting 29% of people over the age of 18.1 Hypertension is an established risk factor for cardiovascular, cerebrovascular, and renal disease.2 Severe elevations in blood pressure (BP) can result in acute end-organ damage with significant morbidity or mortality.3
Hypertensive crises are encountered in a wide range of patients and occur with varying degrees of severity.4 Prompt recognition, evaluation, and appropriate treatment of these conditions are crucial for preventing permanent end-organ damage.5 This article reviews the current understanding of hypertensive crises, the evaluation of a patient's risk of end-organ damage, management strategies for BP reduction, and commonly used therapeutic agents.
Overview
The Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure does not specifically define hypertensive crisis.2 A crisis is generally considered to occur when the systolic BP (SBP) exceeds 180 mmHg or the diastolic BP (DBP) exceeds 120 mmHg.2 Hypertensive crises are further classified as either hypertensive emergency (acute end-organ damage is present) or hypertensive urgency (acute end-organ damage is absent).6 It is important to distinguish between hypertensive urgency and hypertensive emergency when formulating a therapeutic plan.
Despite increasing knowledge of and advances in the management of chronic hypertension, it is estimated that 1% to 2% of patients with hypertension will have a hypertensive emergency at some time in their life.4 The majority of patients presenting with hypertensive emergency have a previous diagnosis of hypertension and have been prescribed antihypertensive medications.7 It is common (more than 50% of the time) for patients who present with hypertensive emergency to have been poorly adherent to their antihypertensive regimen at some point during the preceding week.7,8 Rates of hypertensive-emergency episodes are highest among the elderly, African Americans, and individuals of lower socioeconomic status, and men are affected twice as often as women.8,9 Patients presenting with severe hypertension may represent as much as 25% of all visits to busy urban emergency departments (EDs).4
Pathophysiology
Most patients have persistent BP elevation--resulting from essential or secondary hypertension--for years before they manifest a hypertensive crisis.7 The cause of severe and rapid BP elevation is not fully understood, but it is postulated that an abrupt increase in systemic vascular resistance is precipitated by humoral vasoconstrictors.3 The subsequent rise in BP generates mechanical stress and endothelial injury, which leads to activation of the coagulation cascade and platelets; this results in a deposition of fibrin, and thus fibrinoid necrosis of the arterioles.3 This process induces end-organ ischemia and triggers the release of additional vasoactive mediators that generate a cycle of ongoing injury.3,10 In addition, the renin-angiotensin system often is activated, leading to further vasoconstriction and the production of proinflammatory cytokines.10 All of these mechanisms contribute to the rapidly progressing end-organ hypoperfusion, ischemia, and dysfunction that define a hypertensive emergency.
Evaluation and Management
The clinical symptoms observed in a patient with hypertensive emergency are directly related to the particular end-organ dysfunction that has occurred (TABLE 1).4-6 Patients often present for evaluation of a new complaint related to their elevated BP.7 The manifestations of end-organ dysfunction vary from patient to patient. Rapid patient triage and physician evaluation should take place in order to identify potential ongoing end-organ damage. A physical examination that includes assessment of pulses in all extremities, auscultation of the lungs for possible pulmonary edema, listening for heart gallops or murmurs, and thorough neurologic and fundoscopic testing should be performed.5 Pharmacists can assist in taking a medical account that focuses on the history of the hypertension. It is desirable to assess the patient's adherence to the current antihypertensive medication regimen and to know how much time has elapsed since the last dose was taken. A complete medication-history screening, including OTC usage, is imperative for identifying possible secondary causes of BP elevation.

The management of hypertensive urgency differs from that of hypertensive emergency since no acute end-organ damage is present. In these patients, the elevated BP may represent an acute recognition of chronic hypertension. Utilizing oral medications to lower the BP gradually over 24 to 48 hours (h) is the best approach to management.11 A rapid reduction in BP may be associated with significant morbidity in hypertensive urgency caused by sudden changes in perfusion pressure and a blunted autoregulatory response with long-standing hypertension.6
In a hypertensive emergency, end-organ damage is already present. Altered autoregulation exists in these patients; therefore, rapid and excessive correction of the BP can further reduce perfusion and propagate further injury.6 Hypertensive emergency is best managed with continuous infusion of a short-acting, titratable antihypertensive agent.5 The patient should be managed in an ICU with close monitoring, and consideration should be given to using an arterial line to obtain accurate BP readings. The goal is not to rapidly lower the BP to less than 140/90 mmHg; rather, a controlled reduction in mean arterial pressure (MAP = [2 x DBP + SBP]/3) of up to 25% within minutes to hours is the initial target. If the patient is stable, further reduction to 160/110 mmHg can be attempted over the next 2 to 6 h. If the patient remains stable with these reductions, normalization of BP to goal targets can be attempted slowly with oral agents over the next 24 to 48 h.2
Pharmacotherapy
A number of drugs are available for the management of hypertensive crisis.12 The agent of choice in a given situation will depend on the clinical scenario. Oral agents such as clonidine and captopril are useful in the management of hypertensive urgency; titratable parenteral agents are preferred in the treatment of hypertensive emergency.6,11 Immediate-release nifedipine is potentially dangerous in patients with hypertensive crises and is not recommended.13 Because of unpredictable pharmacodynamics, the sublingual and intramuscular routes should be avoided with all medications used to manage hypertensive crises. The following is a summary of recommended IV antihypertensive agents (see also TABLE 2).
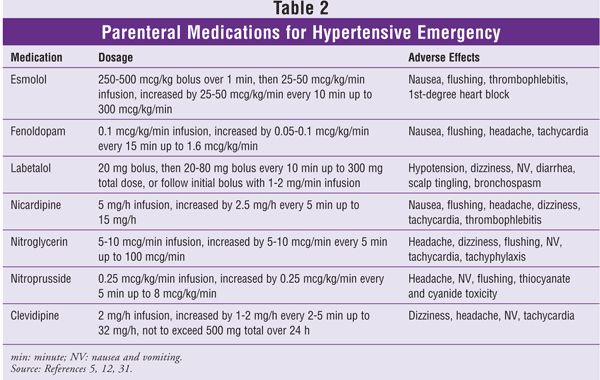
Esmolol: This is a rapid-acting, parenteral, cardioselective beta1-adrenergic receptor blocker. Its onset of action is within 60 seconds (s) and its duration of action is 10 to 20 minutes (min).14 Metabolism of esmolol is via rapid hydrolysis of ester linkages by red blood cell (RBC) esterases; it is not dependent on renal or hepatic function.14 Esmolol is administered at a 250- to 500-mcg/kg loading dose over 1 min, followed by an infusion starting at 25 to 50 mcg/kg/min and titrated by 25 to 50 mcg/kg/min up to 300 mcg/kg/min as needed. Esmolol is particularly useful in severe postoperative hypertension because of its rapid effect and titratability.15 Like other beta-blockers, esmolol is contraindicated in patients with asthma, severe bradycardia, worse than first-degree heart blockade, and uncontrolled heart failure.
Fenoldopam: Fenoldopam is a fast-acting, parenteral, peripheral dopamine-1 receptor agonist. Activation of dopamine-1 receptors causes vasodilation of the coronary, renal, mesenteric, and peripheral arteries.16 Fenoldopam's onset of action is within 5 min, with peak effect achieved by 15 min; its duration of action is 30 min.17 The recommended initial starting dose is 0.1 mcg/kg/min, and it can be titrated by 0.05 to 0.1 mcg/kg/min at 15-min intervals to a maximum of 1.6 mcg/kg/min. Fenoldopam improves creatinine clearance, urine flow rates, and sodium excretion in severely hypertensive patients with normal or impaired renal function, but these outcomes have not been documented to reduce morbidity and mortality.18,19 Adverse effects are minimal and may include tachycardia, flushing, dizziness, or headache.17 Because fenoldopam produces a dose-dependent increase in intraocular pressure, it should be used cautiously in patients with glaucoma.
Labetalol: This medication is a combined nonselective beta-adrenergic and selective alpha1-adrenergic receptor blocker. The beta:alpha antagonism of IV labetalol is approximately 7:1.20 The mixed adrenergic receptor antagonism manifests as a reduction in peripheral vascular resistance without causing reflex tachycardia and potentially causing bradycardia. Antihypertensive effects of labetalol begin within 2 to 5 min after IV administration, peak at 5 to 15 min, and last 3 to 6 h.20 Labetalol's lengthy duration of effect allows it to be administered at a loading dose of 20 mg, followed by repeated incremental doses of 20 to 80 mg at 10-min intervals until the desired BP is achieved, up to a maximum cumulative dose of 300 mg. Alternatively, after the initial bolus, an infusion of 1 to 2 mg/min titrated to the desired BP can be effective. Because of its potent nonselective beta-adrenergic effects, labetalol should be avoided in patients with asthma, uncontrolled heart failure, sinus bradycardia, or greater than first-degree heart block.
Nicardipine: This drug is a second-generation dihydropyridine calcium channel blocker with high vascular selectivity and strong cerebral and systemic vasodilatory activity. The onset of action of IV nicardipine is 5 to 15 min, with a duration of action of 40 to 60 min.21 The initial infusion rate is 5 mg/h, increasing by 2.5 mg/h every 5 min to a maximum of 15 mg/h. Nicardipine has few serious adverse effects. In clinical trials the most frequently reported adverse effects were thrombophlebitis, headache, flushing, tachycardia, dizziness, and nausea.22,23
Nitroglycerin: Nitroglycerin is a potent venous dilator, but it affects arterial tone only at high doses. Its onset of action is 1 to 2 min and its duration of action is 5 to 10 min.24 The initial infusion rate is 5 to 10 mcg/min, and it should be titrated to effect, up to a dose of 100 mcg/min. Nitroglycerin is limited by its adverse effects: tachyphylaxis, which develops with prolonged usage, and headache. Because of its favorable effects on collateral coronary flow, nitroglycerin should be considered for patients with hypertensive emergencies associated with myocardial ischemia.25
Nitroprusside: Sodium nitroprusside is a potent arterial and venous vasodilator that decreases both preload and afterload. This agent has an onset of action of seconds, a duration of action of 1 to 2 min, and a plasma half-life of 3 to 4 min.26 The initial dose is 0.25 mcg/kg/min, titrated by 0.25 mcg/kg/min every 5 min to a maximum dose of 8 mcg/kg/min. Patients may develop tachyphylaxis to nitroprusside with prolonged use; this requires higher doses than initially established for similar BP control.
A potential concern with nitroprusside is that it contains 44% cyanide by weight.27 Cyanide is released in a dose-dependent manner as nitroprusside degradation occurs. Cyanide is metabolized in the liver to thiocyanate--a reaction that requires the presence of adequate amounts of thiosulfate--and the thiocyanate is excreted by the kidneys.28 A healthy person can adequately eliminate the cyanide produced by an infusion of nitroprusside up to a rate of 2 mcg/kg/min. Higher rates, especially in patients requiring prolonged therapy or with concomitant renal or hepatic dysfunction, are associated with a greater risk of cyanide toxicity.27,28 This increase in potential toxicity can be offset by the addition of sodium thiosulfate.29,30
Current methods of monitoring cyanide levels are not sensitive. Therapy should be discontinued if the patient develops signs of cyanide toxicity, including tachycardia, metabolic acidosis, altered consciousness, coma, convulsions, and cardiac arrest.27,28 Thiocyanate toxicity, which occurs more frequently than cyanide toxicity, is of particular concern in patients with renal insufficiency who are receiving prolonged infusions. Thiocyanate toxicity may cause weakness, hyperreflexia, confusion, psychosis, tinnitus, seizures, and coma.26 Monitoring of thiocyanate levels is not recommended unless a patient has renal insufficiency and is receiving therapy for more than a couple of days. Nitroprusside should be discontinued if thiocyanate levels reach 12 mg/dL.26
Clevidipine: This agent is a third-generation dihydropyridine calcium channel blocker with an ultrashort-acting profile. A selective arteriolar vasodilator, clevidipine acts by selectively inhibiting the influx of extracellular calcium through the L-type channel, relaxing smooth muscle of the small arteries and reducing peripheral vascular resistance.31 It is rapidly metabolized by RBC esterases, with an initial half-life of 1 min, and it is not affected by altered renal or hepatic function.32 Several small trials have shown clevidipine to be effective for the control of postoperative hypertension and for severe hypertensive patients treated in the ED.33-36 No large randomized, controlled studies have investigated the role of clevidipine in hypertensive emergencies, but its pharmacokinetic properties have made it an agent of interest.
Clevidipine is available as a concentration of 0.5 mg/mL injectable emulsion. It is contraindicated in patients with soy or egg allergy. Because the lipid content is 2 kcal/mL, the drug should be used cautiously in patients with lipid-metabolism disorders.31 The initial dose is 1 to 2 mg/h, titrated by 1 to 2 mg/h at 90-s intervals initially and then at 5-min intervals as the BP approaches goal; the maximum dose should not exceed 32 mg/h. Careful consideration must be given to the total lipid load, and the 24-h total volume administered should not exceed 1,000 mL.
Pharmacists' Role
Pharmacists can have a number of positive effects on the treatment of patients with hypertensive crises. First, pharmacists should assist with identifying the disease state and taking the medication history. With so many therapeutic options available, pharmacists can help decide which agent will be most effective and appropriate in a specific clinical scenario. Pharmacists should provide correct initial dosages, give titration recommendations, and advise about potential adverse effects to monitor. Because overly aggressive BP reduction can cause further end-organ damage, pharmacists should take part in developing therapeutic endpoints and assist in monitoring interim BP measurements. Finally, a primary cause of hypertensive crisis is poor compliance with maintenance antihypertensive medications. Pharmacists should proactively ensure that maintenance regimens are appropriate, simplified, and manageable for patients at or approaching discharge.
Conclusion
Patients with hypertensive crises exhibit severe elevations in BP that can lead to extensive morbidity and even mortality if the hypertension is improperly managed. The appropriate therapeutic approach in a given case depends on the patient's clinical presentation. Patients with hypertensive urgency lack end-organ damage and can be treated with oral medications that gradually reduce BP to goal over a period of several hours to several days. Hypertensive emergencies, on the other hand, require intense monitoring in an ICU setting and IV therapy with the goal of halting the progression of end-organ damage. Through their expertise in retrieving medication histories and their knowledge of pharmacotherapeutic options, pharmacists can have a positive influence on the care of patients with hypertensive crises.
REFERENCES
1. Ostchega Y, Yoon SS, Hughes J, Louis T. Hypertension Awareness, Treatment, and Control--Continued Disparities in Adults: United States, 2005-2006. NCHS Data Brief no. 3. Hyattsville, MD: National Center for Health Statistics; 2008.
2. Chobanian AV, Bakris GL, Black HR, et al. The seventh report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: the JNC 7 report. JAMA. 2003;289:2560-2572.
3. Ault MJ, Ellrodt AG. Pathophysiological events leading to the end-organ effects of acute hypertension. Am J Emerg Med. 1985;3(suppl 6):10-15.
4. Zampaglione B, Pascale C, Marchisio M, et al. Hypertensive urgencies and emergencies. Prevalence and clinical presentation. Hypertension. 1996;27:144-147.
5. Marik PE, Varon J. Hypertensive crises: challenges and management. Chest. 2007;131:1949-1962.
6. Vidt DG. Hypertensive crises: emergencies and urgencies. J Clin Hypertens (Greenwich). 2004;6:520-525.
7. Tisdale JE, Huang MB, Borzak S. Risk factors for hypertensive crisis: importance of out-patient blood pressure control. Fam Pract. 2004;21:420-424.
8. Bennett NM, Shea S. Hypertensive emergency: case criteria, sociodemographic profile, and previous care of 100 cases. Am J Public Health. 1988;78:636-640.
9. Lip GY, Beevers M, Potter JF, Beevers DG. Malignant hypertension in the elderly. QJM. 1995;88:641-647.
10. Wallach R, Karp RB, Reves JG, et al. Pathogenesis of paroxysmal hypertension developing during and after coronary bypass surgery: a study of hemodynamic and humoral factors. Am J Cardiol. 1980;46:559-565.
11. Gales MA. Oral antihypertensives for hypertensive urgencies. Ann Pharmacother. 1994;28:352-358.
12. Hirschl MM. Guidelines for the drug treatment of hypertensive crises. Drugs. 1995;50:991-1000.
13. Fami MJ, Ho NT, Mason CM. Another report of adverse reactions to immediate-release nifedipine. Pharmacotherapy. 1998;18:1133-1135.
14. Benfield P, Sorkin EM. Esmolol. A preliminary review of its pharmacodynamic and pharmacokinetic properties, and therapeutic efficacy. Drugs. 1987;33:392-412.
15. Gray RJ, Bateman TM, Czer LS, et al. Use of esmolol in hypertension after cardiac surgery. Am J Cardiol. 1985;56:49F-56F.
16. White WB, Radford MJ, Gonzalez FM, et al. Selective dopamine-1 agonist therapy in severe hypertension: effects of intravenous fenoldopam. J Am Coll Cardiol. 1988;11:1118-1123.
17. Munger MA, Rutherford WF, Anderson L, et al. Assessment of intravenous fenoldopam mesylate in the management of severe systemic hypertension. Crit Care Med. 1990;18:502-504.
18. Elliott WJ, Weber RR, Nelson KS, et al. Renal and hemodynamic effects of intravenous fenoldopam versus nitroprusside in severe hypertension. Circulation. 1990;81:970-977.
19. Shusterman NH, Elliott WJ, White WB. Fenoldopam, but not nitroprusside, improves renal function in severely hypertensive patients with impaired renal function. Am J Med. 1993;95:161-168.
20. MacCarthy EP, Bloomfield SS. Labetalol: a review of its pharmacology, pharmacokinetics, clinical uses and adverse effects. Pharmacotherapy. 1983;3:193-219.
21. Singh BN, Josephson MA. Clinical pharmacology, pharmacokinetics, and hemodynamic effects of nicardipine. Am Heart J. 1990;119:427-434.
22. Wallin JD. Intravenous nicardipine hydrochloride: treatment of patients with severe hypertension. Am Heart J. 1990;119:434-437.
23. Neutel JM, Smith DH, Wallin D, et al. A comparison of intravenous nicardipine and sodium nitroprusside in the immediate treatment of severe hypertension. Am J Hypertens. 1994;7:623-628.
24. Francis GS. Vasodilators in the intensive care unit. Am Heart J. 1991;121:1875-1878.
25. Flaherty JT, Magee PA, Gardner TL, et al. Comparison of intravenous nitroglycerin and sodium nitroprusside for treatment of acute hypertension developing after coronary artery bypass surgery. Circulation. 1982;65:1072-1077.
26. Friederich JA, Butterworth JF. Sodium nitroprusside: twenty years and counting. Anesth Analg. 1995;81:152-162.
27. Rindone JP, Sloane EP. Cyanide toxicity from sodium nitroprusside: risks and management. Ann Pharmacother. 1992;26:515-519.
28. Robin ED, McCauley R. Nitroprusside-related cyanide poisoning. Time (long past due) for urgent, effective interventions. Chest. 1992;102:1842-1845.
29. Hall VA, Guest JM. Sodium nitroprusside-induced cyanide intoxication and prevention with sodium thiosulphate prophylaxis. Am J Crit Care. 1992;1:19-25.
30. Baskin SI, Horowitz AM, Nealley EW. The antidotal action of sodium nitrite and sodium thiosulfate against cyanide poisoning. J Clin Pharmacol. 1992;32:368-375.
31. Cleviprex (clevidipine butyrate) injectable emulsion prescribing information. Clayton, NC: Hospira, Inc; August 2008.
32. Ericsson H, Bredberg U, Eriksson U, et al. Pharmacokinetics and arteriovenous differences in clevidipine concentration following a short- and a long-term intravenous infusion in healthy volunteers. Anesthesiology. 2000;92:993-1001.
33. Levy JH, Mancao MY, Gitter R, et al. Clevidipine effectively and rapidly controls blood pressure preoperatively in cardiac surgery patients: the results of the randomized, placebo-controlled efficacy study of clevidipine assessing its preoperative antihypertensive effect in cardiac surgery-1. Anesth Analg. 2007;105:918-925.
34. Singla N, Warltier DC, Gandhi SD, et al. Treatment of acute postoperative hypertension in cardiac surgery patients: an efficacy study of clevidipine assessing its postoperative antihypertensive effect in cardiac surgery-2 (ESCAPE-2), a randomized, double-blind, placebo-controlled trial. Anesth Analg. 2008;107:59-67.
35. Aronson S, Dyke CM, Stierer KA, et al. The ECLIPSE trials: comparative studies of clevidipine to nitroglycerin, sodium nitroprusside, and nicardipine for acute hypertension treatment in cardiac surgery patients. Anesth Analg. 2008;107:1110-1121.
36. Pollack CV, Varon J, Garrison NA, et al. Clevidipine, an intravenous dihydropyridine calcium channel blocker, is safe and effective for the treatment of patients with acute severe hypertension. Ann Emerg Med. 2009;53:329-338.
To comment on this article, contact rdavidson@jobson.com.





