US Pharm. 2013;38(7):51-56.
ABSTRACT: Acute pharyngitis is a common infection that is typically managed in the outpatient setting. While respiratory viruses are responsible for the majority of cases, group A streptococcus (GAS) is the most common bacterial cause of what is generally referred to as strep throat. The Infectious Diseases Society of America recently released updated clinical practice guidelines for the diagnosis and management of GAS pharyngitis. First-line treatment for GAS pharyngitis is penicillin or amoxicillin, and alternative agents include a first-generation cephalosporin, clindamycin, clarithromycin, and azithromycin. Pharmacists are in a key position to improve outcomes for patients with acute pharyngitis through recommendations for appropriate antimicrobial therapy, monitoring of adverse effects, and prevention of drug interactions.
Acute pharyngitis is one of the most common childhood diseases throughout the world, with more than 7 million outpatient office visits each year.1 In the United States, approximately 20% to 30% of cases of acute pharyngitis in children and 5% to 15% of cases in adults are due to group A streptococcus (GAS).1-3 According to the 2010 National Hospital Ambulatory Care Survey, acute pharyngitis is ranked among the top 20 most-reported diagnoses for outpatient emergency department visits, resulting in an economic burden to society ranging from $224 to $539 million per year.4,5
While many patients presenting with sore throat have an underlying infection, fewer than 20% have a clear indication for antibiotic therapy.6 It is important to discern which patients require antibiotic therapy to avoid unnecessary use of antibiotics. The Infectious Diseases Society of America (IDSA) released updated clinical practice guidelines for the diagnosis and management of GAS pharyngitis in November 2012.3 The purpose of this review is to educate pharmacists on the proper management of adult and pediatric patients presenting with pharyngitis according to the IDSA guidelines.
Etiology, Risk Factors, and Transmission
While respiratory viruses such as adenovirus, influenza virus, para-influenza virus, respiratory syncytial virus, and rhinovirus are the most common causes of acute pharyngitis, GAS is by far the most common cause of bacterial pharyngitis and is generally referred to as strep throat (TABLE 1).3,7 Streptococcal pharyngitis is rare among children under the age of 3 years when signs and symptoms suggestive of viral infections (discussed later in the article) are present.8 It occurs most commonly among children older than 5 years and among young adolescents in winter and early spring when the weather is usually colder.3,7 Neisseria gonorrhoeae can cause pharyngitis in sexually active persons.3,7 Other risk factors for pharyngitis include crowded environments such as schools and exposure through household contacts.9 The primary mechanism of spread is via respiratory droplets; however, food-borne outbreaks have been well described.8,9

Pathophysiology
Streptococcal pharyngitis results from the proliferation of GAS in the pharynx. GAS has several surface proteins and produces numerous extracellular products that facilitate infiltration and subsequent evasion of the immune system.8 The M protein is responsible for its virulence and clinical complications.9
Clinical Presentation and Complications
Most cases of acute pharyngitis present with sore throat and are self-limited.10 While it is often difficult to differentiate between viral and bacterial pharyngitis based on symptoms alone,11 TABLE 2 highlights the symptoms suggestive of viral and streptococcal pharyngitis.3,7 Streptococcal pharyngitis is associated with rare but serious complications that can be divided into suppurative complications (i.e., peritonsillar abscess, retropharyngeal abscess, cervical lymphadenitis, mastoiditis, otitis media, sinusitis, and necrotizing fasciitis), and nonsuppurative complications (i.e., acute rheumatic fever, acute glomerulonephritis, and reactive arthritis.)10 Believed to result from an autoimmune response, rheumatic fever and rheumatic heart disease mainly affect children in underdeveloped countries and are the leading causes of cardiovascular death during the first five decades of life.12

Diagnostic Considerations
Individual signs and symptoms are not generally considered powerful enough to distinguish between viral and bacterial pharyngitis except when overt clinical and epidemiologic features that suggest a viral etiology such as common cold symptoms are present and in children younger than 3 years.3,13 Swabbing the throat and testing for GAS by rapid antigen detection test (RADT) and/or microbiology culture is recommended to establish a diagnosis of GAS pharyngitis because even patients who present with all of the typical features of streptococcal pharyngitis are found to have GAS only 30% to 50% of the time.3,14 Since currently available tests are highly specific, if a RADT is positive, it is not necessary to verify the results using a backup culture.3 However, if a RADT is negative, it is recommended to follow up with culture in children and adolescents because currently available tests are not highly sensitive, and this population has a relatively high incidence of streptococcal pharyngitis.3
Treatment
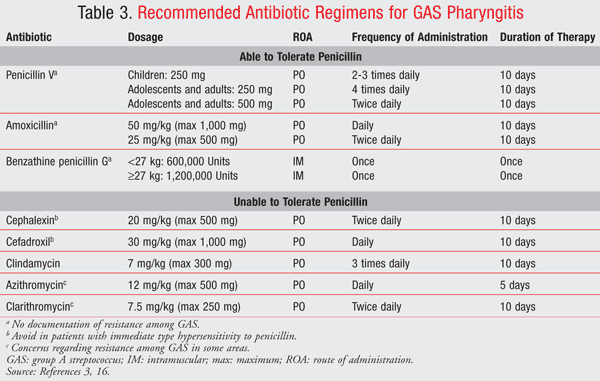
The recommended agent of choice for the treatment of GAS pharyngitis in patients without a penicillin allergy is penicillin or amoxicillin.3 Penicillin is considered to be the preferred agent in most patients because of its proven efficacy, inexpensive cost, narrow spectrum of activity, and benign side-effect profile.3 Amoxicillin is often used as the first-line agent in children because its suspension tastes better than that of penicillin.3 For patients with a nonanaphylactic penicillin allergy, a first-generation cephalosporin is recommended3; however, hypersensitivity to cephalosporins has been reported in patients with penicillin allergy with a prevalence ranging from 3% to 18%.15 Clindamycin or a macrolide, preferably clarithromycin or azithromycin, is recommended for those with a severe allergy to penicillin.3
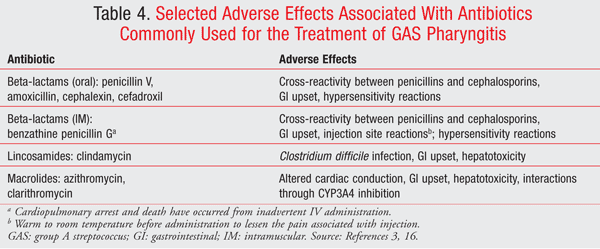
TABLE 3 summarizes recommended antibiotic regimens for GAS pharyngitis, and TABLE 4 details their side-effect profiles.3,16
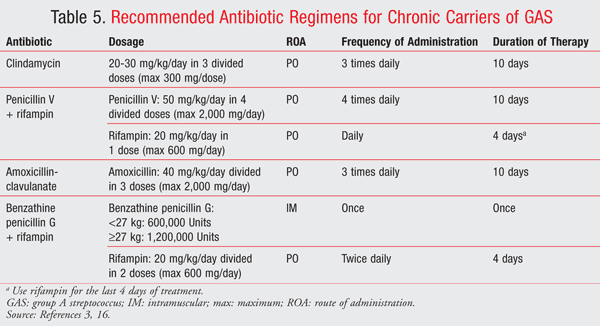
There are certain patients who experience recurrent episodes of pharyngitis and have laboratory evidence of GAS.3 In these cases, the clinician needs to determine whether the patient is having a repeated GAS infection or is merely a chronic GAS carrier who is experiencing recurrent viral pharyngitis.3 Antibiotic therapy is not indicated for most patients who are chronic carriers of GAS, but may be used in selected circumstances. These include during a community outbreak of invasive GAS infection (including acute rheumatic fever or post-streptococcal glomerulonephritis); during an outbreak in a closed or partially closed community; in a patient with a personal or family history of acute rheumatic fever; when a particular family has excessive worry about infections caused by GAS; or when tonsillectomy is being considered.3 TABLE 5 summarizes the antibiotic regimens that may be used for the management of chronic carriers of GAS.3,16
In terms of adjunctive treatment for streptococcal pharyngitis, an agent with analgesic and antipyretic properties such as acetaminophen or a nonsteroidal anti-inflammatory drug (NSAID) may be used in addition to an antibiotic for patients with a fever or moderate-to-severe symptoms.3 It is important to note that aspirin should be avoided in children because of the risk of Reye syndrome.3
The Pharmacist’s Role
Pharmacists play an important role in educating health care providers and patients about the judicious and appropriate use of antibiotics in the management of acute pharyngitis, as antibiotics are only indicated in the management of GAS pharyngitis and other selected cases. Using RADT in a walk-in setting, pharmacists were able to provide a cost-effective treatment for adults with GAS pharyngitis.17 Pharmacists can also assist patients in the selection of OTC agents that are most likely to be beneficial given clinical symptoms, and can actively work with clinicians in the selection of the most suitable antimicrobial agent if antibiotic therapy is warranted. Pharmacists are in a key position to appropriately dose antimicrobial agents and to monitor for adverse reactions and drug interactions when managing patients with acute pharyngitis.
REFERENCES
1. World Health Organization. Initiative for Vaccine Research (IVR). Bacterial infections. Group A Streptococcus. www.who.int/vaccine_research/diseases/soa_bacterial/en/index3.html. Accessed March 20, 2013.
2. CDC. Acute pharyngitis in adults: physician information
sheet (adults).
www.cdc.gov/getsmart/campaign-materials/info-sheets/adult-acute-pharyngitis.html.
Accessed March 20, 2013.
3. Shulman ST, Bisno AL, Clegg HW, et al. Clinical
practice guideline for the diagnosis and management of group A
streptococcal pharyngitis: 2012 update by the Infectious Diseases
Society of America. Clin Infect Dis. 2012;55:1279-1282.
4. CDC. National Hospital Ambulatory Medical Care Survey:
2010 outpatient department summary tables.
www.cdc.gov/nchs/data/ahcd/nhamcs_outpatient/2010_opd_web_tables.pdf.
Accessed March 20, 2013.
5. Pfoh E, Wessels MR, Goldmann D, et al. Burden and economic cost of group A streptococcal pharyngitis. Pediatrics. 2008;121:229-234.
6. Vincent MT, Celestin N, Hussain AN. Pharyngitis. Am Fam Physician. 2004;69:1465-1470.
7. Wessels MR. Clinical practice. Streptococcal pharyngitis. N Engl J Med. 2011;364:648-655.
8. Wessels MR. Streptococcal and enterococcal infections. In: Kasper DL, Fauci AS, eds. Harrison’s Infectious Diseases. New York, NY: McGraw-Hill Medical; 2010:399-403.
9. Weber R. Pharyngitis. In: Bope ET, Kellerman RD, eds. Conn’s Current Therapy. Philadelphia, PA: Elsevier; 2013:40-43.
10. Frei C, Frei B, Zhanel G. Upper respiratory tract infections. In: DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 8th ed. New York, NY: McGraw-Hill; 2011:1867-1880.
11. Aalbers J, O’Brien KK, Chan WS, et al. Predicting
streptococcal pharyngitis in adults in primary care: a systematic review
of the diagnostic accuracy of symptoms and signs and validation of the
Centor score. BMC Med. 2011;9:67.
12. Gerber MA, Baltimore RS, Eaton CB, et al. Prevention
of rheumatic fever and diagnosis and treatment of acute streptococcal
pharyngitis: a scientific statement from the American Heart Association
Rheumatic Fever, Endocarditis, and Kawasaki Disease Committee of the
Council on Cardiovascular Disease in the Young, the Interdisciplinary
Council on Functional Genomics and Translational Biology, and the
Interdisciplinary Council on Quality of Care and Outcomes Research:
endorsed by the American Academy of Pediatrics. Circulation. 2009;119:1541-1551.
13. Linder JA, Bates DW, Lee GM, et al. Antibiotic treatment of children with sore throat. JAMA. 2005;294:2315-2322.
14. Choby BA. Diagnosis and treatment of streptococcal pharyngitis. Am Fam Physician. 2009;79:383-390.
15. Apter AJ, Kinman JL, Bilker WB, et al. Is there cross-reactivity between penicillins and cephalosporins? Am J Med. 2006;119:354.e11-354.e19.
16. Lexi-Comp Online [online database]. Hudson, OH: Lexi-Comp, Inc; 2013. www.lexi.com. Accessed March 20, 2013.
17. Klepser DG, Bisanz SE, Klepser ME. Cost-effectiveness of pharmacist-provided treatment of adult pharyngitis. Am J Manag Care. 2012;18:e145-e154.
To comment on this article, contact rdavidson@uspharmacist.com.






