US Pharm. 2022;47(9):35-40.
Cardiovascular disease (CVD) remains the leading cause of mortality and morbidity in the United States, with coronary heart disease (CHD) being the most common type of heart disease.1 Dyslipidemia is a major contributor to the development of CHD and other forms of atherosclerosis; individuals with high total cholesterol levels have about twice the risk for heart disease. This is not to say that all cholesterol is bad. Cholesterol is an important substance that the body requires to synthesize hormones and provide stability in the lipid bilayer of cell membranes.2 However, when there is an excess amount of cholesterol in the body, it can deposit in the blood vessels and lead to reduced perfusion of the blood through the arteries. Low-density lipoprotein cholesterol (LDL-C) and high-density lipoprotein cholesterol (HDL-C) are important modifiable risk factors for the prevention of atherosclerotic disease. Adults with extremely high levels of LDL-C (>190 mg/dL) are at a much greater risk for cardiovascular events compared with those with LDL-C levels of <130 mg/dL.3 Conversely, HDL-C levels are inversely correlated with the risk of cardiovascular events, with levels <40 mg/dL considered a negative risk.4 Almost 29% of adults have LDL-C levels above 130 mg/dL, and more than 18% have HDL-C levels below 40 mg/dL.5,6
There are certain health conditions, lifestyle habits, and nonmodifiable factors that are associated with an increased risk of developing high cholesterol. Health conditions such as type 2 diabetes, hypothyroidism, and chronic kidney disease can affect blood cholesterol to undesirable levels. A family history of high cholesterol may also increase risk of developing high cholesterol. At a BMI of 30 or greater, obesity is also capable of increasing LDL and triglyceride levels and lowering HDL levels. Accordingly, consuming a diet that is high in saturated fats and trans fats—which are found in most meat, poultry, and dairy products—will increase cholesterol production in the body. Lack of physical activity will promote weight gain and lead to higher levels of cholesterol. Increased levels of cholesterol can happen at any age in life but there is a higher risk in older ages. Men will generally have a higher risk compared with women, but women will have an increased risk especially after 55 years of age or after menopause. There are also certain drug classes that may promote high cholesterol, such as antiarrhythmic medications, beta-blockers, steroids, and high doses of diuretic medications. This is why it is important for everyone over the age of 20 years to have their cholesterol measured at least once every 5 years.7,8
In 2013, the American College of Cardiology (ACC) and the American Heart Association (AHA) released guidelines for the treatment of blood cholesterol: ACC/AHA Guideline on the Treatment of Blood Cholesterol to Reduce Atherosclerotic Cardiovascular Risk in Adults.9 Rather than providing specific cholesterol targets, the current guideline focuses on intensity of statin treatment in four different groups. In 2018, these guidelines were updated, providing specific recommendations for specific reductions in LDL-C.10 Recommendations for pharmacotherapy should be a shared decision between the provider and patient, including an interpretation of the patient’s 10-year risk of atherosclerotic disease.
Pharmacists are in an ideal position to provide and educate patients regarding the use of OTC products for the management of high cholesterol. They can help patients make informed decisions based on the available data. The following is a discussion of popular OTC agents and lifestyle changes utilized in the management of dyslipidemia.
Conventional Treatment of Dyslipidemia
Statins
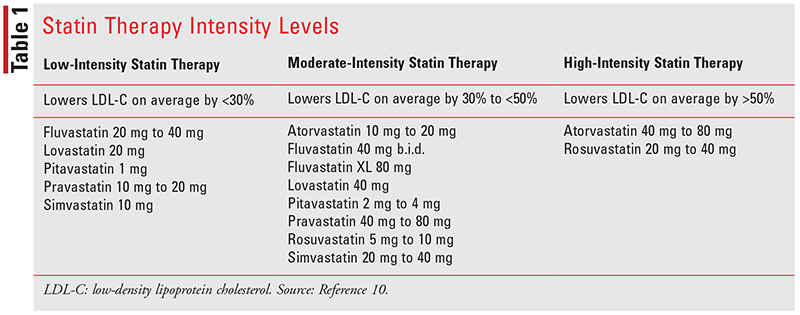
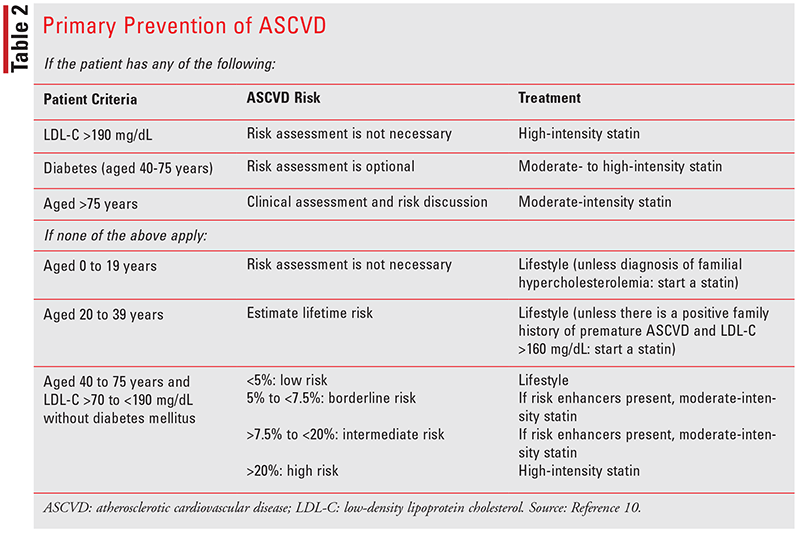
HMG-CoA reductase inhibitors, also known as statins, are the drugs of choice in the management of dyslipidemia. Statin drugs are divided into three categories based on intensity of statin therapy and will reduce LDL levels by as much as 50% to as low as 30%, depending on the intensity (see TABLE 1). In patients with established clinical atherosclerotic cardiovascular disease (ASCVD), including a history of myocardial infarction, ischemic stroke, peripheral arterial disease, or coronary artery disease, a high-intensity statin is recommended. Moderate-intensity statin therapy should be considered only in adults aged older than 75 years who are unable to tolerate high-intensity statin therapy. Primary prevention considers multiple factors, such as presence of diabetes, age, and estimated ASCVD risk (see TABLE 2).
Nearly one-half of treatment-eligible adults are not taking cholesterol-lowering medications.11 This can be attributed to many reasons, including cost, perceived susceptibility to cardiovascular risks, and most commonly, fear and concerns regarding safety and adverse effects.12,13 Some of these patients may be looking for alternative ways to lower their cholesterol and reduce their risk for CVD.
Complementary and Alternative Medicine
Approximately 34% of adults in the U.S. are using some form of complementary and alternative medicine (CAM).14 Cholesterol is included as one of the top-10 conditions for which adults are using CAM.15 Fish oil and garlic—two supplements commonly used for the reduction of high cholesterol—were among the top 10 most frequently used natural products.14
Omega-3 Fatty Acids
Omega-3 fatty acids, better known as fish oil, are the most frequently used natural product among adults, with consumption increasing almost 10-fold in the past decade.14,16 They contain two long-chain fatty acids, docosahexaenoic acid (DHA) and eicosatetraenoic acid (EPA), and a short-chain fatty acid known as alpha-linolenic acid. They have shown to be effective in lowering serum triglycerides up to 50%; however, DHA can raise LDL-C and HDL-C.17 In 2002, the AHA recommended omega-3 fatty acids (EPA and DHA) for the reduction of triglyceride levels in patients with hypertriglyceridemia, a condition in which triglyceride levels are 200 to 499 mg/dL.18 A daily dosage of 2 g to 4 g of EPA and DHA is recommended to achieve this effect, particularly with FDA-approved prescription products. Prescription omega-3 fatty acids are indicated as an adjunct to diet to reduce triglyceride levels in adults with severe hypertriglyceridemia (triglycerides ≥500 mg/dL). In patients taking 4 g/day of prescription omega-3 fatty acids, triglyceride levels were lowered up to 30% with no increase of LDL-C. In patients with severe hypertriglyceridemia, there was a greater reduction of triglycerides but also an increase in LDL-C with products containing DHA.18
There are over 400 OTC products currently marketed as omega-3 fish oil dietary supplements.19 These products not only contain EPA and DHA, but may also include saturated fats, fat-soluble vitamins, and cholesterol.20 Fish oil supplements vary in their EPA and DHA concentrations, ranging from 20% to more than 80%, leading to reduced efficacy. Some dietary supplements may contain saturated fats and oxidized lipids, which can impact and increase the risk of CVD.21 The FDA recommends 3 g as the maximum daily dose for dietary omega-3 fatty acid supplements for safe use. If patients require more than 3 g, they should be under a physician’s supervision.22 On average, patients will need to take 11.2 servings per day (one to three capsules per serving) to achieve this higher recommended dose.17 Many patients will have difficulty with this high pill burden.
Overall, these products are generally well tolerated. The most common adverse effects include stomach upset, diarrhea, and reflux. Many patients will complain about a “fishy” taste, especially if they are taking higher doses. Advising them to take enteric-coated formulations or freezing the capsules may help reduce this. Another effect associated with its use is excessive bleeding. Patients on anticoagulants or antiplatelet agents should use omega-3 fatty acids cautiously.
Garlic
Garlic is a bulbous perennial plant that belongs to the Amaryllis family. It has shown to produce a wide range of health effects and has been used as a supplement to treat and prevent different diseases, including CVD, by lowering blood pressure and preventing atherosclerosis.23 Garlic has been suggested to modestly reduce total cholesterol and LDL levels.24 A comprehensive meta-analysis on the effect of garlic on blood lipids discovered that garlic could reduce total cholesterol by approximately 17 mg/dL and LDL by 9 mg/dL.25 These results were particularly evident in those who took garlic for more than 2 months and in those who had elevated cholesterol and triglyceride levels prior to treatment. The possible mechanism of these actions results from reduced absorption of cholesterol and reduced synthesis of cholesterol and fatty acid.26 However, garlic has no effect on HDL or triglyceride levels.24
Garlic comes in several different oral formulations such as garlic powder (which is used to make tablets), garlic oil (which can also present as capsules), and aged extract. These different preparations may also play a role in how effectively they can treat dyslipidemia. Products that contain aged-garlic extract appear to be more effective at lowering total cholesterol levels compared with garlic powder products, although, among the garlic powder products, enteric-coated garlic powder products reduced total cholesterol levels to a significant degree.25
Study results have shown that garlic is highly tolerable and poses minimal side effects, in comparison to conventional therapies.27 Common adverse effects include bad breath and body odor, stomach pain, and gas. Garlic has antiplatelet effects and can increase a patient’s risk for bleeding. Patients who are on anticoagulants and antiplatelet agents should be warned about this potential risk.28
Niacin
Niacin, also known as nicotinic acid, is a form of vitamin B3 and is one of the most effective agents to raise HDL-C levels; it can raise HDL-C by almost 35%.29 Niacin also reduces LDL-C levels up to 25% and triglycerides 20% to 50%.29,30 This effect is dose related, requiring 1 g to 4 g per day. Despite this, cholesterol management guidelines do not recommend niacin as add-on therapy to statins because of the lack of cardiovascular benefit.10,31
Niacin is available in three formulations. Two formulations are available without a prescription: immediate-release and controlled-release or sustained-release. An extended-release product known as Niaspan is available only with a prescription and is FDA approved for its lipid-lowering properties. Niaspan is considered more tolerable compared with niacin supplements.32 Flushing of the skin is a very common side effect of niacin, especially with immediate-release products. Flushing presents as itchy and red skin that is warm to the touch and generally lasts for about an hour. A formulation was made specifically to target this side effect and is labeled on the shelves as “flush-free” niacin. However, it is important to note that these products do not contain niacin; rather, they contain inositol hexanicotinate, which has shown to be ineffective as a lipid-lowering agent.33 Niacin-induced flushing can be prevented by pretreatment of aspirin or a nonsteroidal anti-inflammatory drug 30 minutes prior to niacin with meals and avoiding spicy foods or hot beverages after taking niacin. Additionally, increasing the dose slowly over time will help to reduce incidences of flushing.34 Other adverse effects of niacin include pruritus, hyperglycemia, and hepatotoxicity. Hepatotoxicity is mostly seen with sustained-release niacin, and therefore this formulation is contraindicated in those with liver failure.
Red Yeast Rice
Red yeast rice (RYR) is white rice that has been cultivated with various strains of a yeast known as Monascus purpureus. RYR supplements have shown to lower cholesterol and related lipid levels. This activity may be due to the effect of monacolin K present in RYR products.35 Monacolin K is a molecule that inhibits the production of cholesterol and is chemically identical to lovastatin. Average daily doses of 1,200 mg to 2,400 mg of RYR resulted in reductions of up to 27% of LDL and 24% of non-HDL levels when taken for 12 weeks.36 Additionally, RYR has helped to reduce total cholesterol by approximately 17% and triglyceride levels by 8%. Clinical trials have shown that RYR reduces LDL on an average of 1.02 mmol/L, which was proportional to the reduction seen with low-intensity and low-dose statin medications.37
It is important to note that due to the lack of regulation, there is varying information about the content of monacolin in red yeast dietary supplements. Products can vary from having little to no monacolin content or having several different types at differing concentrations.38 In 2007, the FDA issued a warning against the use of red yeast products, determining that any product containing more than a trace amount of monacolin K cannot be sold legally as a dietary supplement.39 Another issue that arises from the lack of standardization of the production of red yeast products is the formation of toxic byproducts known as citrinin, which can be harmful to the kidneys.40 The adverse effect profile is like that of statin drugs, including hepatotoxicity and myopathy.
Soluble Fiber
According to the American Diabetic Association, it is recommended for adults to consume 14 g of dietary fiber per 1,000 kcal, which would equate to 25 g for women and 38 g for men.41 While soluble fiber can be obtained from fiber-rich foods, it is also available as a supplement. This includes oat beta-glucan, pectin, various gums, and psyllium. When ingested and allowed to ferment in the gut, soluble fiber produces short-chain fatty acids that decrease cholesterol synthesis in the liver. This promotes the reduction of blood cholesterol and increased excretion of cholesterol and bile acids.42
Clinical studies have shown that supplemental fiber can reduce LDL by 5% to 15%.43 Highly viscous fiber blends showed to be proportional with total cholesterol and LDL reduction.44 Notably, psyllium husk fiber has been the most studied among the others and revealed that an average of 10.2 g per day significantly reduced LDL by 5.94 mg/dL and non-HDL by 7.02 mg/dL.45 Adverse effects of fiber include flatulence, abdominal bloating, and diarrhea. When first starting fiber supplements, it is important to gradually increase dietary intake over time to reduce the occurrence of these side effects. Additionally, fiber supplements, especially those with high viscosity, may reduce the absorption of other medications, so it is recommended to take supplements 1 hour before or 2 hours after to avoid potential drug interactions.
Lifestyle Changes
Introducing and maintaining certain lifestyle modifications are crucial in lowering cholesterol and reducing cardiovascular risk. Following a healthy lifestyle is the foundation for maintaining healthy serum levels. One of the key messages from the 2018 ACC/AHA guidelines is the importance of a heart-healthy lifestyle to reduce ASCVD risk. There are many healthy diet patterns such as DASH (Dietary Approaches to Stop Hypertension), AHA (American Heart Association diet), or MED (Mediterranean diet) that can be incorporated into the diet to promote lowering cholesterol and LDL levels. These diet plans generally follow a similar format that encourages eating vegetables, fruits, and whole grains. It also includes fat-free or low-fat dairy products, lean protein sources such as fish and poultry, beans, and nuts. It limits foods that are high in saturated fats and drinks or sweets containing sugar. It is recommended to achieve 5% to 6% of calorie intake from saturated fat to help reduce dietary cholesterol and LDL levels. Weight is also an important modifiable factor. An average of 40 minutes of moderate-to-vigorous physical activity is recommended three to four times per week. Moderation and calorie restriction may also help with weight loss. Additionally, it will also be beneficial to avoid smoking and limit alcohol consumption.10,46
Role of the Pharmacist
Incorporating practices to help control cholesterol levels is an essential step towards living a heart-healthy lifestyle. During this process, pharmacists can promote appropriate lifestyle modifications. Pharmacists may also assess patient-specific risk factors to help guide treatment. It is also important to acknowledge and address challenges and barriers expressed by the patient including medication adherence or difficulties maintaining proper healthy practices or quitting poor habits that are damaging to one’s health.
Conclusion
Dyslipidemia is a prevalent condition affecting over 100 million people and can more than double a person’s risk for the development of CVD. Because of this, many individuals are seeking alternative ways to lower their cholesterol. Pharmacists can play a vital role in this process by educating patients and helping them make informed decisions regarding the use of the various available supplements.
Supplements that are supported by clinical evidence and guidelines include omega-3 fatty acids and soluble fiber. Pharmacists should keep in mind, however, that these supplements are not regulated by the FDA and there may be inconsistencies between different manufacturers and batches. Pharmacists should avoid recommending garlic, RYR, sustained-release niacin, no-flush niacin, and niacinamide due to lack of efficacy or documented adverse effects. Overall, OTC supplements should rarely be used for primary prevention of CVD because they have not been shown to improve outcomes or mortality. Pharmacists should place a strong emphasis on the importance of and benefits associated with therapeutic lifestyle changes, such as maintaining a healthy weight, eating a low-fat, low-cholesterol, high-fiber diet, and physical activity. Patients should also be reminded to inform their healthcare providers of any supplements that they be using.

What Is Cholesterol?
Cholesterol is a substance that your body needs to keep you healthy. It comes from two sources: your body and the food you eat, such as meat, poultry, and dairy products. Too much cholesterol can increase your risk for heart disease.
What Is the Difference Between “Good” and “Bad” Cholesterol?
“Bad” cholesterol, also known as LDL, will build up in the inner walls of your arteries, making them narrow. This slows down flow. If this buildup of plaque breaks off, a clot forms that can completely block flow, causing a heart attack.
“Good” cholesterol, also known as HDL, helps protect you from heart attacks and strokes. This type of cholesterol carries the bad cholesterol away from the arteries.
How Can I Improve My Cholesterol?
Eating healthy foods, maintaining a healthy weight, and staying physically active are all ways to help improve your cholesterol.
Can Supplements Help?
There are a few things you can take to help you lower your cholesterol, but you should speak with a healthcare provider before starting. Supplements that may have some benefit include omega-3 fatty acids/fish oil and soluble fibers (psyllium).
Supplements that should be avoided include red yeast rice, garlic, sustained-release niacin, “no-flush” niacin and niacinamide. These supplements have no data to support their use in lowering cholesterol levels or they have been associated with liver damage.
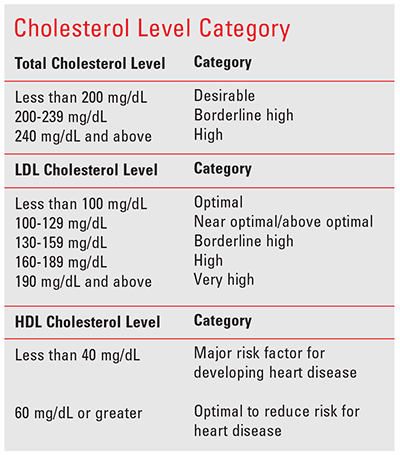
What Are “Normal” Cholesterol Numbers?
All individuals aged 20 years and older should have their cholesterol levels checked at least once every 5 years. The blood test should be taken after fasting for 9 to 12 hours.
REFERENCES
1. CDC. Heart disease facts. July 15, 2022. www.cdc.gov/heartdisease/facts.htm. Accessed August 9, 2022.
2. CDC. About cholesterol. June 24, 2021. www.cdc.gov/cholesterol/about.htm. Accessed August 9, 2022.
3. Perak AM, Ning H, de Ferranti SD, et al. Long-term risk of atherosclerotic cardiovascular disease in US adults with the familial hypercholesterolemia phenotype. Circulation. 2016;134(1):9-19.
4. Navab M, Reddy ST, Van Lenten BJ, Fogelman AM. HDL and cardiovascular disease: atherogenic and atheroprotective mechanisms. Nat Rev Cardiol. 2011;8(4):222-232.
5. Virani SS, Alonso A, Aparicio HJ, et al. Heart disease and stroke statistics—2021 update: a report from the American Heart Association. Circulation. 2021;143(8):e254-e743.
6. Carroll MD, Fryar CD, Nguyen DT. Total and high-density lipoprotein cholesterol in adults: United States, 2015-2016. NCHS Data Brief. 2017;(290):1-8.
7. NIH. Blood cholesterol causes and risk factors. March 24, 2022. www.nhlbi.nih.gov/health/blood-cholesterol/causes. Accessed August 9, 2022.
8. CDC. Knowing your risk for high cholesterol. January 31, 2020. www.cdc.gov/cholesterol/risk_factors.htm. Accessed August 9, 2022.
9. Stone NJ, Robinson JG, Lichtenstein AH, et al. 2013 ACC/AHA guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular risk in adults. Circulation. 2014;129(25 Suppl 2):S1-45.
10. Grundy SM, Stone NJ, Bailey AL, et al. 2018 AHA/ACC/AACVPR/AAPA/ABC/ACPM/ADA/AGS/APhA/ASPC/NLA/PCNA guideline on the management of blood cholesterol: executive summary: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J Am Coll Cardiol. 2019;73(24):3168-3209.
11. Mercado C, DeSimone AK, Odom E, et al. Prevalence of cholesterol treatment eligibility and medication use among adults—United States, 2005-2012. MMWR Morb Mortal Wkly Rep. 2015;64(47):1305-1311.
12. Fung V, Sinclair F, Wang H, et al. Patients’ perspectives on nonadherence to statin therapy: a focus-group study. Perm J. 2010;14(1):4-10.
13. Chee YJ, Chan HHV, Tan NC. Understanding patients’ perspective of statin therapy: can we design a better approach to the management of dyslipidaemia? A literature review. Singapore Med J. 2014;55(8):416-421
14. Clarke TC, Black LI, Stussman BJ, et al. Trends in the use of complementary health approaches among adults: United States, 2002-2012. Natl Health Stat Rep. 2015;(79):1-16.
15. National Center for Complementary and Alternative Medicine. The use of complementary and alternative medicine in the United States. December 2008. https://files.nccih.nih.gov/s3fs-public/camuse.pdf. Accessed August 16, 2022.
16. Kantor ED, Rehm CD, Du M, et al. Trends in dietary supplement use among US adults from 1999-2012. JAMA. 2016;316(14):1464-1474.
17. Bradberry JC, Hilleman DE. Overview of omega-3 fatty acid therapies. P T. 2013;38(11):681-691.
18. Skulas-Ray AC, Wilson PWF, Harris WS, et al. Omega-3 fatty acids for the management of hypertriglyceridemia: a science advisory from the American Heart Association. Circulation. 2019;140(12):e673-e691.
19. Omega-3. In: Dietary Supplement Label Database (DSLD). National Institutes of Health. https://ods.od.nih.gov/Research/Dietary_Supplement_Label_Database.aspx. Accessed January 8, 2017.
20. Fialkow J. Omega-3 fatty acid formulations in cardiovascular disease: dietary supplements are not substitutes for prescription products. Am J Cardiovasc Drugs. 2016;16:229-239.
21. Mason RP, Sherratt SCR. Omega-3 fatty acid fish oil dietary supplements contain saturated fats and oxidized lipids that may interfere with their intended biological benefits. Biochem Biophys Res Commun. 2017;483(1):425-429.
22. Miller M, Stone NJ, Ballantyne C, et al. Triglycerides and cardiovascular disease: a scientific statement from the American Heart Association. Circulation. 2011;123(20):2292-2333.
23. Bayan L, Koulivand PH, Gorji A. Garlic: a review of potential therapeutic effects. Avicenna J Phytomed. 2014;4(1):1-14.
24. Sun YE, Wang W, Qin J. Anti-hyperlipidemia of garlic by reducing the level of total cholesterol and low-density lipoprotein: a meta-analysis. Medicine (Baltimore). 2018;97(18):e0255.
25. Ried K, Toben C, Fakler P. Effect of garlic on serum lipids: an updated meta-analysis. Nutr Rev. 2013;71(5):282-299.
26. Matsuura H. Saponins in garlic as modifiers of the risk of cardiovascular disease. J Nutr. 2001;131:1000S-5S.
27. Gyawali D, Vohra R, Orme-Johnson D, et al. A systematic review and meta-analysis of Ayurvedic herbal preparations for hypercholesterolemia. Medicine (Kaunas). 2021;57(6):546.
28. Borrelli F, Capasso R, Izzo AA. Garlic (Allium sativum L.): adverse effects and drug interactions in humans. Mol Nutr Food Res. 2007;51(11):1386-1397.
29. Chapman MJ, Redfern JS, McGovern ME, Giral P. Niacin and fibrates in atherogenic dyslipidemia: pharmacotherapy to reduce cardiovascular risk. Pharmacol Ther. 2010;126(3):314-345.
30. Houston M. The role of nutraceutical supplements in the treatment of dyslipidemia. J Clin Hypertens. 2012;14(2):121-132.
31. D’Andrea E, Hey SP, Ramirez CL, Kesselheim AS. Assessment of the role of niacin in managing cardiovascular disease outcomes. JAMA Netw Open. 2019;2(4):e192224.
32. Knopp RH. Evaluating niacin in its various forms. Am J Cardiol. 2000;86(12A):51L-56L.
33. Norris RB. “Flush-free niacin”: dietary supplement may be “benefit-free.” Prev Cardiol. 2006;9(1):64-65.
34. Jacobson TA. A “hot” topic in dyslipidemia management—“how to beat a flush”: optimizing niacin tolerability to promote long-term treatment adherence and coronary disease prevention. Mayo Clin Proc. 2010;85(4):365-379.
35. National Center for Complementary and Integrative Health. Red yeast rice. July 2013. www.nccih.nih.gov/health/red-yeast-rice. Accessed August 9, 2022.
36. Moriarty PM, Roth EM, Karns A, et al. Effects of xuezhikang in patients with dyslipidemia: a multicenter, randomized, placebo-controlled study. J Clin Lipidol. 2014;8(6):568-575.
37. Cicero AFG, Fogacci F, Zambon A. Red yeast rice for hypercholesterolemia: JACC focus seminar. J Am Coll Cardiol. 2021;77(5):620-628.
38. Dujovne CA. Red yeast rice preparations: are they suitable substitutions for statins? Am J Med. 2017;130(10):1148-1150.
39. National Center for Complementary and Integrative Health. High cholesterol and natural products: what the science says. February 6, 2013. www.nccih.nih.gov/health/providers/digest/cholesterol-science. Accessed January 8, 2017.
40. Childress L, Gay A, Zargar A, Ito MK. Review of red yeast rice content and current Food and Drug Administration oversight. J Clin Lipidol. 2013;7(2):117-122.
41. Slavin JL. Position of the American Dietetic Association: health implications of dietary fiber. J Am Diet Assoc. 2008;108(10):1716-1731.
42. Soliman GA. Dietary fiber, atherosclerosis, and cardiovascular disease. Nutrients. 2019;11(5):1155.
43. Banach M, Patti AM, Giglio RV, et al. The role of nutraceuticals in statin intolerant patients. J Am Coll Cardiol. 2018;72(1):96-118.
44. Vuksan V, Jenkins AL, Rogovik AL, et al. Viscosity rather than quantity of dietary fibre predicts cholesterol-lowering effect in healthy individuals. Br J Nutr. 2011;106(9):1349-1352.
45. Jovanovski E, Yashpal S, Komishon A, et al. Effect of psyllium (Plantago ovata) fiber on LDL cholesterol and alternative lipid targets, non-HDL cholesterol and apolipoprotein B: a systematic review and meta-analysis of randomized controlled trials. Am J Clin Nutr. 2018;108(5):922-932.
46. Eckel RH, Jakicic JM, Ard JD, et al. 2013 AHA/ACC guideline on lifestyle management to reduce cardiovascular risk: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation. 2014;129(25 Suppl 2):S76-S99.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





