US Pharm. 2023;48(7):7-12.
ABSTRACT: Exercise-induced bronchoconstriction (EIB) is a common condition that affects many individuals, especially those with asthma. It is characterized by the narrowing of the airways in response to physical activity or exercise, leading to symptoms such as coughing, wheezing, shortness of breath, and chest tightness. Pharmacists play a critical role in managing EIB, including educating patients on appropriate use of bronchodilators and inhaled corticosteroids, detecting potential adherence issues, and providing guidance on the proper administration of medications. They can also advise patients on strategies to prevent and manage EIB, including warm-up exercises, avoiding triggers, and monitoring increased symptoms. By working collaboratively with healthcare teams, pharmacists can help improve outcomes and enhance the quality of life of patients with EIB.
According to the CDC, 4.9 million patients visit their physicians annually for asthma, with 1.2 million patients diagnosed with asthma visiting the emergency department.1 Exercise-induced bronchoconstriction (EIB) is a common condition that can affect patients with or without an asthma diagnosis. Exercise can cause shortness of breath in most people; however, patients with asthma will also experience tightness in their lungs, making breathing more difficult. Up to 90% of patients with an asthma diagnosis also have EIB, demonstrating how widespread it is.2 To properly advise patients on pharmacologic therapy, pharmacists must have a thorough understanding of the mechanism and symptoms of EIB.
Prevalence and Risk Factors
The Asthma and Allergy Foundation of America estimates that roughly 25 million Americans—or nearly one in every 13 people—have asthma.3 EIB can occur in both asthmatic and nonasthmatic patients; however, it is thought to affect approximately 90% of asthma sufferers.4 Children are a common group impacted by EIB. EIB is present in 40% to 90% of asthmatic children, particularly those with severe asthma who are not receiving appropriate medication therapy.5 Given the prevalence of asthma, it is crucial for pharmacists to familiarize themselves with the risk factors for EIB.
Additional risk factors for EIB include allergies, allergic rhinitis, and history of asthma or wheezing.4 Since EIB is caused by exercise, strenuous exercise and sports are likely to cause bronchospasm and constriction due to increased breathing. The likelihood of experiencing EIB is also influenced by environmental variables. Factors such as humidity, cold air, and pollutants are related to an increased risk of EIB.5 Breathing in cold environments is frequently a major contributor to EIB and is common in those who are exposed to cold, dry air.6
Mechanism of Action
The mechanism of action of EIB must be understood to guarantee that the appropriate treatment option is prescribed. The two mechanisms proposed to cause EIB are drying of the airway and mucosal cooling. When the airway surface liquid in the lungs dries up from excessive breathing brought on by exercise, it results in increased coughing and mucus production.7 This loss in water produces a hyperosmolar environment, shifting water out of the cell, thereby shrinking it. Inflammatory mediators such histamines, prostaglandins, and leukotrienes are released as a result.8 Additionally, as mucus cools from breathing, cholinergic airway receptors are stimulated, leading to an increase in mucus output and smooth muscle tone.7 These dual mechanisms feed into each other, causing bronchoconstriction when people exercise.
Recognizing Signs of EIB
Pharmacists play an important role in recognizing signs of EIB and referring patients to their physician. The signs and symptoms of EIB are often indistinguishable from asthma symptoms. The differentiating factor between the two is when these symptoms occur after 5 to 10 minutes of exercise. Symptoms such as tightness in the chest, shortness of breath, coughing, wheezing, and difficulty breathing occur in patients with EIB.9 Additionally, these symptoms usually dissipate within 30 to 90 minutes and cause a refractory period of 1 to 3 hours.10 Pharmacists will encounter many patients with asthma during the course of a day; thus it is vital to be aware of these symptoms and intervene when necessary.
EIB Treatment Options
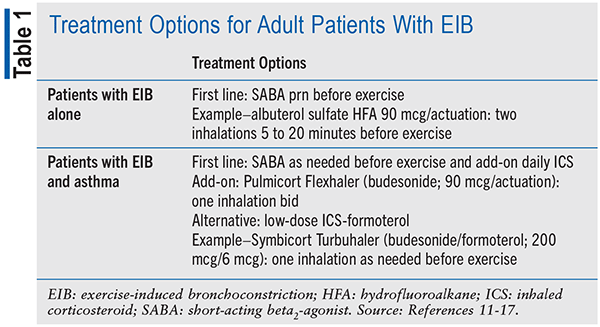
Although EIB is regarded as an asthmatic condition, the treatment process is somewhat different for patients with EIB alone versus patients with concomitant asthma and EIB. Patients with EIB alone are usually recommended an inhaled short-acting beta2-agonist (SABA) to be used 5 to 20 minutes before beginning exercise. However, if these patients end up requiring a SABA daily, it would be more effective to add a controller medication such as an inhaled corticosteroid (ICS).11 For patients with EIB and diagnosed asthma, the addition of a controller agent such as an ICS used daily is highly recommended.11,12 The use of low-dose inhaled budesonide and formoterol before exercise, as opposed to SABA monotherapy before exercise, was superior in lowering EIB symptoms, according to a 6-week study of the use of ICS with formoterol on individuals with moderate asthma.13 Additionally, it found that the use of ICS-formoterol is noninferior in reducing EIB compared with daily ICS and as-needed SABA use.11-13 TABLE 1 illustrates the treatment and baseline dosing options for both patients with EIB alone and patients with EIB with asthma. These treatment options serve as the baseline and may need to be titrated for symptom resolution. Furthermore, it is advised that patients with seasonal allergies take an oral antihistamine daily before exercise.12
Dangers of SABA Overuse
Although SABAs are the first-line therapy for the management of EIB, pharmacists must be aware of the long-term risks associated with SABA usage. In reality, many patients who are given SABAs have a tendency to overuse them when their asthma is uncontrolled.18 Overuse of SABAs is risky since it raises the possibility of exacerbations and asthma-related mortality.19 According to a 2004 retrospective study of 100,000 patients with asthma, individuals who needed to use three or more SABA inhaler canisters per year had a higher chance of experiencing an asthma exacerbation.20 Furthermore, the overuse of beta2-agonists can lead to tolerance, which can greatly reduce their effectiveness in the treatment and prevention of EIB.21 This is an important issue of concern, particularly if patients begin to refill their inhalers too early or more frequently, in which case pharmacists can swiftly intervene should any trends of nonadherence or misuse be detected.
Pharmacist’s Role
Pharmacists are historically considered the most accessible healthcare provider. A recent study found that patients visit their community pharmacies approximately 1.5 to 2 times more frequently than they do their physicians or other qualified healthcare professionals.22 This means that community pharmacists will see patients more than physicians do, which gives them the opportunity to make valuable interventions. Asthma medications prescribed to patients can lose their effectiveness over time. This could be attributed to various factors like asthma severity, intensity of exercise, SABA tolerance, or patient nonadherence.21 Patients with EIB experience similar symptoms as those with asthma, which is why it is important to counsel both new patients and existing patients when they receive their medication from the pharmacy.
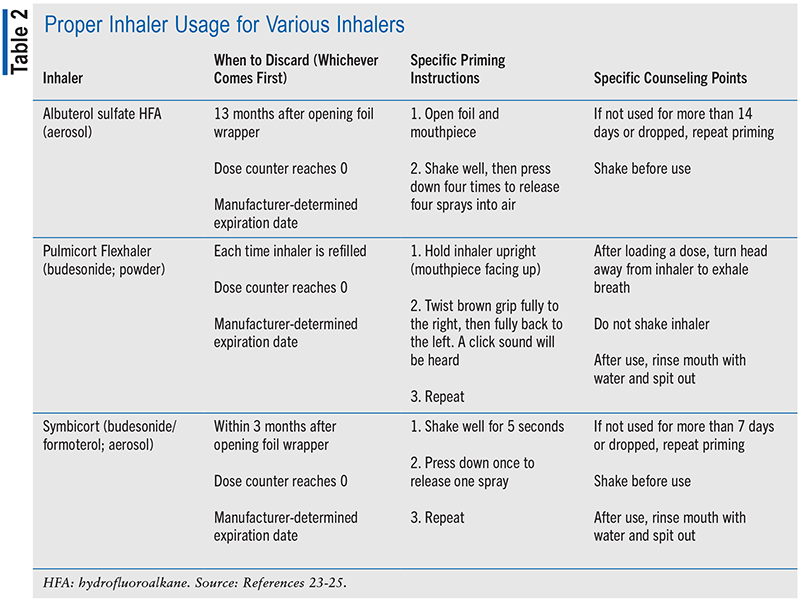
During counseling, pharmacists can demonstrate for newly diagnosed EIB patients how and when to use their inhaler. There are many inhalers on the market, and each has its own unique usage requirements, such as the number of times the inhaler needs to be primed before use and beyond-use dates. For example, albuterol aerosol inhalers require priming with four sprays, budesonide powder inhalers require priming with one spray, and budesonide/formoterol aerosol inhalers require priming with two releases.23-25 When priming, patients should be instructed to aim the inhaler away from their face and away from any people nearby. Also, remember to counsel patients to write on the inhaler the date that it was removed from the foil wrapper. Information regarding beyond-use dates, priming instructions, and specific counseling points is further illustrated in TABLE 2.
Patients with EIB alone are normally prescribed only a reliever medication; patients with asthma will also have a controller medication. The use of multiple inhalers might become confusing for patients, making comprehensive patient counseling even more essential. Pharmacists should also be checking for possible drug-drug interactions and contraindications and alert patients on possible adverse effects. Additionally, pharmacists should follow up with patients when they receive their new and refill medications, ensuring that their EIB, with or without asthma diagnosis, is being treated properly.
Furthermore, pharmacists can greatly impact and improve patient medication adherence. This is especially important with asthma medications since inconsistent use of controller medications can lead to ineffective therapy. Pharmacists can implement prescription reminders for patients to take and refill their asthma medications. By suggesting coupons and drug discount programs, pharmacists may assist patients in overcoming financial obstacles. This will help to ensure that patients willingly refill and pickup their medication and realize the importance of informing their pharmacist or healthcare practitioner if they are experiencing a worsening of symptoms or adverse effects from their medications.
Although EIB is normally controlled through prescription medication, pharmacists have a responsibility also to advise patients on various nonpharmacologic methods to prevent EIB. Patients should not rely solely on medication to relieve and prevent EIB but should also make lifestyle modifications. TABLE 3 shows various ways of managing and preventing EIB. The most studied and validated method to prevent EIB is to induce a refractory period by performing a moderate physical warm-up before exercise.12,21 This essentially “prepares” the lungs for exercise by reducing bronchoconstriction over the following 2 hours. Furthermore, dietary supplements such as omega-3 fatty acids (fish oil) and vitamin C might be beneficial.10,26 In general, maintaining a healthy body weight and a consistent exercise routine can help improve EIB.10,26

Conclusion
EIB is a common condition that is experienced by patients with and without asthma. It is a physiologic phenomenon that can quickly spiral out of control and impose limitations on patients who desire to live a healthy lifestyle through exercise. The health of individuals with EIB may deteriorate as a result of overprescribing and overusing SABAs. Therefore, it is important for pharmacists to be aware of their patient population and educate patients on not only the use of their prescription medications, but also how to implement nonpharmacologic interventions that may further enhance their quality of life.
REFERENCES
1. CDC. Asthma. January 24, 2023. www.cdc.gov/nchs/fastats/asthma.htm. Accessed June 5, 2023.2. Asthma and Allergy Foundation of America. June 2022. Exercise-induced bronchoconstriction (asthma). https://aafa.org/asthma/asthma-triggers-causes/exercise-induced-asthma/#:~:text=In%20the%20past%2C%20it%20was. Accessed June 5, 2023.
3. Asthma and Allergy Foundation of America. March 2023. Asthma facts and figures. https://aafa.org/asthma/asthma-facts/. Accessed June 5, 2023.4. Aggarwal B, Mulgirigama A, Berend N. Exercise-induced bronchoconstriction: prevalence, pathophysiology, patient impact, diagnosis and management. NPJ Prim Care Respir Med. 2018;28(1):31.
5. Klain A, Indolfi C, Dinardo G, et al. Exercise-induced bronchoconstriction in children. Front Med (Lausanne). 2022;8:814976.6. Molis MA, Molis WE. Exercise-induced bronchospasm. Sports Health. 2010;2(4):311-317.
7. Koya T, Ueno H, Hasegawa T, et al. Management of exercise-induced bronchoconstriction in athletes. J Allergy Clin Immunol Pract. 2020;8(7):2183-2192.8. Rodriguez Bauza DE, Silveyra P. Asthma, atopy, and exercise: sex differences in exercise-induced bronchoconstriction. Exp Biol Med (Maywood). 2021;246(12):1400-1409.
9. University of Rochester Medical Center. Exercise-induced bronchoconstriction (EIB). www.urmc.rochester.edu/encyclopedia/content.aspx?contenttypeid=56&contentid=251. Accessed April 4, 2023.10. Gerow M, Bruner PJ. Exercise-induced asthma. Updated August 8, 2022. In: StatPearls [Internet]. Treasure Island, FL: StatPearls Publishing; 2023 Jan-. https://www.ncbi.nlm.nih.gov/books/NBK557554/.
11. Lanz MJ, Gilbert IA, Gandhi HN, et al. Demographics, treatment patterns, and morbidity in patients with exercise-induced bronchoconstriction: an administrative claims data analysis. J Asthma Allergy. 2021;14:1485-1495.12. Global Initiative for Asthma. Global strategy for asthma management and prevention, 2022. https://ginasthma.org/wp-content/uploads/2022/07/GINA-Main-Report-2022-FINAL-22-07-01-WMS.pdf. Accessed June 12, 2023.
13. Lazarinis N, Jørgensen L, Ekström T, et al. Combination of budesonide/formoterol on demand improves asthma control by reducing exercise-induced bronchoconstriction. Thorax. 2014;69(2):130-136.14. Albuterol. Lexi-Drugs. Lexicomp. Hudson, OH. https://online.lexi.com/. Accessed April 4, 2023.
15. Albuterol sulfate aerosol, metered, package insert. Orange, CA: NuCare Pharmaceuticals, Inc; 2019.16. Budesonide (oral inhalation). Lexi-Drugs. Lexicomp. Hudson, OH. https://online.lexi.com/. Accessed April 4, 2023.
17. Budesonide and formoterol. Lexi-Drugs. Lexicomp. Hudson, OH. https://online.lexi.com/. Accessed April 4, 2023.18. Bakakos P, Kostikas K, Loukides S, et al. Reducing tolerance for SABA and OCS towards the extreme ends of asthma severity. J Pers Med. 2022;12(3):504.
19. Nwaru BI, Ekström M, Hasvold P, et al. Overuse of short-acting beta2-agonists in asthma is associated with increased risk of exacerbation and mortality: a nationwide cohort study of the global SABINA programme. Eur Respir J. 2020;55(4):1901872.20. Stanford RH, Shah MB, D’Souza AO, et al. Short-acting beta-agonist use and its ability to predict future asthma-related outcomes. Ann Allergy Asthma Immunol. 2012;109(6):403-407.
21. Weiler JM, Brannan JD, Randolph CC, et al. Exercise-induced bronchoconstriction update-2016. J Allergy Clin Immunol. 2016;138(5):1292-1295.e36.22. Valliant SN, Burbage SC, Pathak S, et al. Pharmacists as accessible health care providers: quantifying the opportunity. J Manag Care Spec Pharm. 2022;28(1):85-90.
23. MedlinePlus. Albuterol oral inhalation. www.medlineplus.gov/druginfo/meds/a682145.html. Accessed April 4, 2023.24. MedlinePlus. Budesonide oral inhalation. www.medlineplus.gov/druginfo/meds/a699056.html. Accessed June 5, 2023.
25. Symbicort (budesonide/formoterol fumarate dihydrate) package insert. Wilmington, DE: AstraZeneca Pharmaceuticals LP; 2006.26. Dickinson J, Amirav I, Hostrup M. Nonpharmacologic strategies to manage exercise-induced bronchoconstriction. Immunol Allergy Clin North Am. 2018;38(2):245-258.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.





