US Pharm. 2022;47(5):23-28.
Skin cancer is the most diagnosed cancer in the United States, with most cases considered preventable. The incidence of skin cancer has steadily been increasing over time. In the past 3 decades, incidence rates have risen fivefold. It has been estimated that one in five Americans will be diagnosed with skin cancer in their lifetime, with an estimated 9,500 newly diagnosed cases per day.1-4
Melanoma is a type of skin cancer that affects melanocytes. Melanocytes are found in the epidermis and are responsible for producing melanin, a dark pigment responsible for giving skin and hair its color. Melanin can also act as photoprotective agents in the skin and eyes. Melanoma occurs when malignant transformation in these cells occur, causing uncontrolled growth and ultimate spread. Melanoma, also known as malignant melanoma and cutaneous melanoma, is the most aggressive skin cancer, and its incidence is on the rise. In the past 10 years, the number of newly diagnosed invasive melanoma cases increased by 31%. While melanoma is not the most common type of skin cancer, it is one of the more dangerous skin cancers; it accounts for only 1% of skin cancers but causes most skin cancer deaths. It is projected that approximately 99,780 new melanomas will be diagnosed in the U.S. in 2022, and almost 7,650 people are expected to die from this cancer. The incidence of cutaneous melanoma is greater in men than in women; however, the incidence is rising in both men and women, with an increase of 4.4% and 3.1% per year, respectively.5-9
Even with the surplus information available on different diseases and disorders, patient compliance and knowledge of essential lifestyle modifications seem to be at an all-time low. Taking preventative measures—and especially being aware of any risk factors—is important when it comes to taking care of one’s health. Discussing risk factors, preventative measures, and what to look out for with a patient are important conversations. These proactive measures can decrease likelihood of disease and allow one to seek care in a timely manner.
Risk Factors
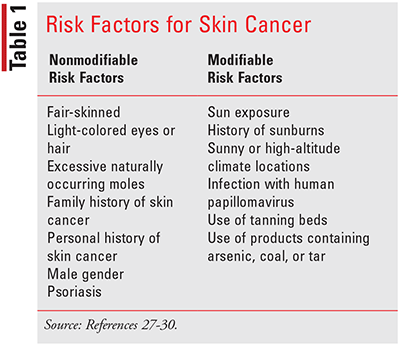
Melanomas can be categorized as a multifactorial disease that can occur via environmental exposure, family history, and phenotypic characteristics. There are many individual factors and determinants that may predispose a patient to skin cancer (see TABLE 1), but exposure to ultraviolet (UV) radiation is one of the most important, modifiable environmental factors that can contribute to the development of melanomas. While UV exposure via the sun can pose this increased risk of melanoma development, artificial UV exposure can also impact the progression of melanomas. Ultraviolet-A (UVA) light present in a tanning bed session has been noted to be higher compared with regular outdoor activities, like sunbathing. Alongside UV rays, psoralen-UVA radiation photochemotherapy, a treatment for psoriasis, has been linked to an increase in the risk of melanomas as well. The most vital genetic factors that serve as risk factors for the development of melanomas include the number of melanocytic nevi and family history. Melanocytic nevi are cancerous abnormal growths that result from the proliferation of melanocytes that can be acquired or innate. A meta-analysis conducted showed that patients who have 101 to 120 melanocytic nevi have a 6.89% increased risk of developing a melanoma. Additionally, a family history of melanomas confers a greater risk for cancer; according to the Skin Care Foundation, one in every 10 patients diagnosed with melanomas have a family member with a history of this disease. Physical characteristics of patients such as having moles, fair skin, many freckles, and blond or red hair are all associated with an increased risk of developing melanoma.10-14
Clinical Presentation and Classification
Melanomas can present on the skin in different ways, but initially it will present as a skin abnormality with distinct characteristics or changes in appearance of an existing abnormality or mole. These changes can be identified using the ABCDE mnemonic: Asymmetry, Border, Color, Diameter, and Evolved. The mole of a melanoma patient is often characterized as being asymmetric. The borders of the mole are uneven, blurred, or notched in appearance. The colors of these moles can range from shades of black, brown, and tan with areas of white, gray, red, or blue. Although the diameter of the mole can be smaller when detected early, melanoma moles can grow to a diameter of greater than 6 mm (the size of a pencil eraser). Lastly, existing moles changing size, shape, color, appearance, or texture can also be clinical presentations of melanoma. The mole can expand and encompass an area of healthy skin without symptoms of pain. Any unusual changes in the appearance of a skin abnormality should be evaluated by a dermatologist for further testing.10,15
Melanomas can be classified with the assistance of the tumor, node, metastasis (TNM) staging system to differentiate the progression of the cancer. Once TNM factors have been identified, a melanoma is assigned a stage from 0 to IV. Stage I and II melanomas are localized, while stage III melanomas have regional lymph node involvement. Stage IV melanomas have distant metastasis.16 Approximately 85% of patients with melanoma will present with localized disease at the time of diagnosis. Regional disease accounts for almost 9% of patients at time of diagnosis, with distant disease accounting for an estimated 4%.17 As melanoma progresses throughout its various stages, the survival rates drastically decrease. The 5-year survival rate depends on the stage of the melanoma at time of diagnosis. Patients diagnosed with localized disease have a 99% 5-year relative survival rate, while those diagnosed with regional disease have a 65% 5-year survival rate, and those with distant disease have a 25% 5-year survival rate.18This decrease in survival rate illustrates the importance of early detection and treatment to prevent the progression of the cancer.
Screening
Proper education about skin cancer and routine skin self-examinations are crucial to preventing the progression of skin cancer, as most melanomas are detected in their early stage through self-screening. Most skin cancers present as a skin abnormality anywhere on the body—even areas that were not exposed to the sun. Different types of screenings are accessible to determine if a patient is experiencing signs of melanoma. First and foremost, it is imperative that individuals are educated about self-screening through self-examination. An early detection of melanoma can result in a better prognosis. Melanoma can occur in any part of the body, including both exposed and unexposed areas to the sun. Performing an examination of the common areas in which skin cancer can present, such as the face, scalp, trunk, torso, legs, and arms, with a full-length body mirror and a hand mirror allows for a thorough check on any new or unusual growth. Aside from the common body parts, individuals should also examine their fingernails, toenails, hands, toes, and mucosal membranes, as these are also locations where new growth can occur. Any unusual or suspicious changes, new lesions on the skin, or a sore that has not healed within 2 weeks should be reported to a healthcare provider or dermatologist for further evaluation.
Prevention
The sun is known to be the biggest contributor to melanoma. The exact mechanism on how sunlight causes melanoma is not fully understood, which is why there is not one fully effective, preventative behavioral strategy that is utilized. However, there are many different approaches that can be taken to lower an individual’s risk of melanoma. Limiting the exposure to UV rays is one of the most important approaches to lowering the risk of melanoma. Some of these prevention methods include limiting or avoiding direct exposure to sunlight when the rays are at its strongest (10 AM to 4 PM), avoiding sunbathing/sun lamps/tanning beds, wearing sun-protective clothing such as a wide-brimmed hat and long-sleeved shirt, protecting the skin if the UV index is 3 or higher in areas, and applying the appropriate sunscreen for optimal protection. It is important to apply a broad-spectrum, water-resistant sunscreen prior to expected exposure to UV radiation. Furthermore, the American Cancer Society also states that a great way to remember what to do when being exposed to the sun is to “SLIP! SLOP! SLAP! and WRAP!” These four words can help an individual remember to SLIP on a shirt, SLOP on sunscreen, SLAP on a hat, and WRAP on sunglasses to protect the eyes and sensitive skin around them.19,20
UV rays can be found in several different places other than the sun. Tanning beds and sun lamps are two common places where individuals are exposed to high amounts of UV rays. Many people have a common misconception that tanning is not as bad being exposed to the sun’s UV rays. The very first tan an individual has in a tanning bed can cause skin damage, and with subsequent visits the damage accumulates, creating more genetic mutations, leading to a greater risk. Additionally, the National Cancer Institute reports that women who use tanning beds multiple times a year have an increased risk of 55% of developing melanoma, especially in teenage girls. Instead of going to a tanning bed, a safer approach would be to use tanning spray or lotions. These products will give the tan look that people are going for without damaging the skin and increasing the risk of melanoma.21,22
Sunscreen
There are many different types of sunscreens available, which can make choosing the optimal product difficult. Sunscreens have a certain sun protection factor (SPF), which ranges from 15 to 100 SPF. The SPF of a sunscreen is a measurement of the sunscreen’s ability to protect the skin from ultraviolet-B (UVB) radiation, not UVA. Each SPF is a factor of the time it takes for an individual’s skin to redden (without sunscreen protection) upon constant exposure to UV radiation. For example, if it takes 15 minutes for an individual’s skin to turn red upon continuous exposure to sunlight, applying an SPF 30 sunscreen allows the skin to be exposed for 450 minutes (30 × 15 minutes) before it starts to turn red from continuous sunlight exposure. When sunscreen is applied prior to going out on a sunny day, the skin has an additional barrier that protects it from the harmful effects of UVB radiation. Sunscreens should be applied every 2 hours to maintain skin protection.23,24
In the past, some sunscreen products have been labeled as “waterproof.” This labeling implies that individuals using a waterproof sunscreen product would not need to reapply sunscreen after swimming or after coming into contact with water (such as sweating). The FDA prohibited the usage of “waterproof” on sunscreen products as it “overstated the effectiveness” of sunscreen upon exposure to water. However, sunscreen products can be labeled as “water-resistant” or “very water-resistant,” depending on the effectiveness of the ingredients to prolong reapplication time of sunscreen after exposure to water or sweat. A rating of 40 or 80 on water-resistant sunscreen products indicates the duration of effectiveness of the sunscreen while swimming or sweating. A rating of 40 indicates that the sunscreen is effective for 40 minutes while swimming or sweating and should be reapplied after 40 minutes. “Very water-resistant” labeling is indicated with a rating of 80 and remains effective after 80 minutes of swimming or intense sweating. Sunscreen should be reapplied after 40 to 80 minutes after swimming or sweating, or immediately after towel-drying.23,24
It is important to help patients select the right sunscreen product to provide the most optimal barrier against UVA and UVB radiation in order to reduce the risk of skin cancer. Early sunscreen products protected the skin from only UVB radiation and not UVA radiation. However, after studies demonstrated the damage caused by UVA radiation, sunscreen manufacturers incorporated a broad-spectrum sunscreen to provide both UVB and UVA protection. All individuals should select a broad-spectrum sunscreen to provide protection against both harmful UV radiations. Individuals with a fair complexion and skin easily reddened upon exposure to sunlight should select a sunscreen product with a SPF of 30 or higher. If a person is expected to sweat throughout his/her activity or is expected to swim, the individual should select a sunscreen that is water-resistant or very water-resistant, depending on how long he/she would be performing the activity. For maximal protection, the American Academy of Dermatology recommends using a sunscreen with an SPF of at least 30 that is broad spectrum and water resistant. Creams are best for dry skin and use on the face, while gels are good for hairy areas.25
Role of the Pharmacist
As melanoma is the most serious form of skin cancer, pharmacists play a vital role in educating patients about UV radiation and the development of skin cancer. Upon providing education to patients about skin cancer, pharmacists can evaluate and inform patients about any additional risk factors that they may have that would warrant concern of potential skin cancer. Pharmacists are also instrumental in promoting skin self-examinations, encouraging patients to reduce sun exposure, and helping patients with choosing the optimal sunscreen products based on skin type and color, as well as teaching them how to appropriately use sunscreen products (see TABLE 2). Pharmacists should also emphasize the dangers of tanning and how patients should never intentionally expose their skin to the sun—as there is no such thing as a “healthy tan.” The pharmacist-patient relationship will allow the pharmacist to communicate to the patient the dangers of sun exposure to exposed skin and will allow the patient to make more informed decisions.

As pharmacists are considered one of the most accessible healthcare professionals, it is vital to understand the influence that they can have on their patients. Many patients are more apt to go into a pharmacy to talk with the pharmacist about an abnormal mole on their skin before going to their doctor, as patients go to their pharmacies often to pick up their medications. Many community pharmacists counsel their patients on their medications, but it is crucial that they have prior knowledge of risk factors and prevention. Furthermore, empathy shown by the pharmacist is a great way to strengthen the pharmacist-patient relationship.
Conclusion
Melanoma is the most detrimental form of skin cancer. Although it is not the most common type of skin cancer, it raises a cause for concern due to its high risk of metastases and mortality. Its clinical presentation and erratic growth of melanocytes make it a difficult disease to diagnose. Melanoma is a multifactorial disease that can result from environmental factors, family history, and physical characteristics. Exposure to UV rays—artificial or natural—can be one of the most pernicious causes of the disease. A family history of a high count of melanocytic nevi also serves to increase the risk of developing this cancer. Moreover, fair skin, numerous freckles, and blond or red hair are among numerous phenotypic traits that are associated with an increased risk of developing melanomas. Prevention of this cancer includes early detection, the application of sunscreen with appropriate reapplication frequency, avoiding tanning beds, selecting alternative products for a tan, and limiting extensive exposure to the sun’s harmful rays. As pharmacists, it is vital to educate patients about UV radiation, modifiable risk factors, and selecting the most appropriate sunscreen for their needs. The incidence rate of melanomas increases about 3% annually while overarching cancer incidence rates are decreasing. Our goal as pharmacists is to elicit change by decreasing this annual rate by promoting methods of prevention, providing proper education, and informing patients about modifiable risk factors.2

Who Is at Risk of Getting a Melanoma?
Individuals who experience extended ultraviolet (UV) radiation exposure are more likely to develop melanomas. This includes tanning in the sun and using tanning beds. People who have fair skin, many freckles, moles, and blond or red hair have an increased risk of developing a melanoma. Genetic factors also serve as risk factors for the development of melanomas, such as the number of melanocytic nevi one has and their family history of melanoma. Melanocytic nevi, also called birth marks or moles, can be flat, rough, or raised and can exist at birth or appear later in life.
How Can I Prevent Getting Melanoma?
The best measure you can take to help prevent melanoma is to reduce your exposure to prolonged sunlight. You should always make sure you wear sunscreen and protect your skin by staying in the shade or wearing clothes that cover exposed skin. By effectively and appropriately using sunscreens that cover both UVA and UVB radiation with a sun protection factor of at least 30, you can greatly decrease your risk of developing skin cancer.
What Signs Should I Look for?
Skin cancer generally starts with the development of a pigmentation or mole on the skin, or the change in color or structure of an existing mole. These abnormalities could also be painful, be irritating, or begin to bleed. Any change in color, structure, or integrity of the skin that does not improve on its own should be evaluated by a dermatologist.
Are There Screenings for Melanomas?
When melanoma is detected early, it is more likely to be cured. Being aware of the freckles, moles, and blemishes on your skin is vital to observe changes on your skin. You should perform a self-examination of your entire body and look for any abnormalities at least once a month. You can conduct a self-examination at home using a full-body mirror to examine any unusual or new formations of the skin, and a hand mirror for not easily–visible locations. If a notable growth is identified, you should speak to your dermatologist about further screening. A dermatologist will likely examine the suspected growth and possibly perform a biopsy or dermoscopy for further analysis.
Where Can I Learn More Information About Melanomas?
For more information about melanomas and other skin cancers, visit the Skin Cancer Foundation website (www.skincancer.org/skin-cancer-information/melanoma) and the American Cancer Society website (www.cancer.org/cancer/melanoma-skin-cancer/about.html).
REFERENCES
1. Guy GP Jr, Thomas CC, Thompson T, et al. Vital signs: melanoma incidence and mortality trends and projections- United States, 1982-2030. MMWR. 2015;64(21):591-596.
2. National Cancer Institute. Cancer stat facts: melanoma of the skin. SEER. www.seer.cancer.gov/statfacts/html/melan.html. Accessed April 4, 2022.
3. Leiter U, Eigentler T, Garbe C. Epidemiology of skin cancer. Adv Exp Med Biol. 2014;810:120-140.
4. American Academy of Dermatology Association. Skin cancers: incident rates. www.aad.org/media/stats-skin-cancer. Accessed April 4, 2022.
5. Davey MG, Miller N, McInerney NM. A review of epidemiology and cancer biology of malignant melanoma. Cureus. 2021;13(5):e15087.
6. American Cancer Society. Key statistics for melanoma skin cancer. www.cancer.org/cancer/melanoma-skin-cancer/about/key-statistics.html. Accessed April 4, 2022.
7. American Cancer Society. Cancer facts & figures 2022. www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/annual-cancer-facts-and-figures/2022/2022-cancer-facts-and-figures.pdf. Accessed April 23, 2022.
8. Bellenghi M, Puglisi R, Pontecorvi G, et al. Sex and gender disparities in melanoma. Cancers (Basel). 2020;12(7):1819.
9. Schlessinger DI, Anoruo M, Schlessinger J. Biochemistry, melanin. StatPearls. StatPearls Publishing; 2022. www.ncbi.nlm.nih.gov/books/NBK459156. Accessed April 4, 2022.
10. Rastrelli M, Tropea S, Rossi CR, Alaibac M. Melanoma: epidemiology, risk factors, pathogenesis, diagnosis and classification. In Vivo. 2014;28(6):1005-1011.
11. Conforti C, Zalaudek I. Epidemiology and risk factors of melanoma: a review. Dermatol Pract Concept. 2021;11(Suppl 1):e2021161S.
12. Damsky WE, Bosenberg M. Melanocytic nevi and melanoma: unraveling a complex relationship. Oncogene. 2017;36(42):5771-5792.
13. Gandini S, Sera F, Cattaruzza MS, et al. Meta-analysis of risk factors for cutaneous melanoma: I. Common and atypical naevi. Eur J Cancer. 2005;41(1):28-44.
14. Titus-Ernstoff L, Perry AE, Spencer SK, et al. Pigmentary characteristics and moles in relation to melanoma risk. Int J Cancer. 2005;116(1):144-149.
15. Ward WH, Lambreton F, Goel N, et al. Clinical presentation and staging of melanoma. In: Ward WH, Farma JM, eds. Cutaneous melanoma: etiology and therapy. Codon Publications; 2017. www.ncbi.nlm.nih.gov/books/NBK481857/. Accessed April 4, 2022.
16. Amin MB, Edge S, Greene F, et al, eds. AJCC Cancer Staging Manual. 8th ed. Springer International Publishing; 2017. www.springer.com/gp/book/9783319406176. Accessed April 4, 2022.
17. National Comprehensive Cancer Network. Melanoma: cutaneous (Version 3.2022). www.nccn.org/professionals/physician_gls/pdf/cutaneous_melanoma.pdf. Accessed April 25, 2022.
18. American Cancer Society. Survival rates for melanoma skin cancer. www.cancer.org/cancer/melanoma-skin-cancer/detection-diagnosis-staging/survival-rates-for-melanoma-skin-cancer-by-stage.html. Accessed April 4, 2022.
19. CDC. Skin cancer: sun safety. www.cdc.gov/cancer/skin/basic_info/sun-safety.htm. Accessed April 4, 2022.
20. American Cancer Society. How do I protect myself from ultraviolet (UV) rays? www.cancer.org/healthy/be-safe-in-sun/uv-protection.html. Accessed April 4, 2022.
21. FDA. Indoor tanning: the risks of ultraviolet rays. December 18, 2015. www.fda.gov/consumers/consumer-updates/indoor-tanning-risks-ultraviolet-rays. Accessed April 4, 2022.
22. Skin Cancer Foundation. Tanning & your skin. www.skincancer.org/risk-factors/tanning/. Accessed April 4, 2022.
23. FDA. Questions and answers: FDA announces new requirements for over-the-counter (OTC) sunscreen products marketed in the U.S. www.fda.gov/drugs/understanding-over-counter-medicines/questions-and-answers-fda-announces-new-requirements-over-counter-otc-sunscreen-products-marketed-us. Accessed April 4, 2022.
24. FDA. Labeling and effectiveness testing: sunscreen drug products for over-the-counter human use—small entity compliance guide. www.fda.gov/regulatory-information/search-fda-guidance-documents/labeling-and-effectiveness-testing-sunscreen-drug-products-over-counter-human-use-small-entity. Accessed April 4, 2022.
25. American Academy of Dermatology Association. Sunscreen FAQs. www.aad.org/public/everyday-care/sun-protection/shade-clothing-sunscreen/sunscreen-faqs. Accessed April 4, 2022.
26. Tripp MK, Watson M, Balk SJ, et al. State of the science on prevention and screening to reduce melanoma incidence and mortality: the time is now. CA Cancer J Clin. 2016;66(6):460-480.
27. U.S. Department of Health and Human Services. Skin cancer as a major public health problem. Office of the Surgeon General (US); 2014. www.ncbi.nlm.nih.gov/books/NBK247164/. Accessed April 4, 2022.
28. Siegel RL, Miller KD, Jemal A. Cancer statistics, 2020. CA Cancer J Clin. 2020;70(1):7-30.
29. Fraser MC, Hartge P, Tucker MA. Melanoma and nonmelanoma skin cancer: epidemiology and risk factors. Semin Oncol Nurs. 1991;7(1):2-12.
30. Apalla Z, Lallas A, Sotiriou E, et al. Epidemiological trends in skin cancer. Dermatol Pract Concept. 2017;7(2):1-6.
31. Skin Cancer Foundation. Ask the expert: which is better, a combination insect repellent and sunscreen or separate products? www.skincancer.org/blog/ask-the-expert-which-is-better-a-combination-insect-repellent-and-sunscreen-or-separate-products/. Accessed April 4, 2022.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





