US Pharm. 2020;45(5):28-30.
Diabetes mellitus (DM) comprises several metabolic disease states characterized by chronic hyperglycemia, which results from defects in the action or secretion of insulin. The American Diabetes Association classifies DM into four categories: type 1 diabetes (T1DM), which involves beta-cell destruction or the body’s inability to produce its own insulin; type 2 DM, which ranges from insulin resistance with relative insulin deficiency to insulin secretory defects with insulin resistance; gestational DM; and other rare, specific types such as latent autoimmune diabetes in adults and cystic fibrosis–related DM.1,2 The incidence of DM is increasing globally every day. If improperly monitored, patients with DM are at greater risk for developing other chronic sequelae.
Epidemiology
In the most recent National Diabetes Statistics Report presented by the CDC, data collected for 2015 indicated that 30.3 million people in the United States (9.4%) had DM and only 23.1 million cases were clinically diagnosed, leaving an estimated 7.2 million people undiagnosed.3
In 2013 to 2015, American Indians and Alaska Natives (representing 15.1% of diabetic persons) had a higher prevalence, followed by non-Hispanic black (12.7%), Hispanic (12.1%), Asian (8.0%), and non-Hispanic white persons (7.4%). In 2015, an estimated 1.5 million new cases of diabetes were diagnosed in U.S. adults aged 18 years or older. Furthermore, 5% of the population diagnosed with DM had T1DM. The incidence of T1DM is greater in individuals younger than age 19 years, and T1DM is more prevalent in non-Hispanic white persons.3
Etiology
Although T1DM is recognized as an autoimmune disease, the specific cause is unknown. Possible causes include genetic predisposition and exposure to viruses and other environmental factors.4 Ultimately, the immune system attacks and destroys beta cells in the pancreatic islets of Langerhans, leading to chronic hyperglycemia.5,6
Monitoring
Implementation of an insulin pump for management of T1DM and consistent monitoring can substantially impact the reduction of associated complications. To mitigate severe adverse effects on cognitive function and long-term damage to the body, blood glucose levels should be closely monitored to ensure that the target goal (80-130 mg/dL) is attained. Particularly in T1DM, continuous glucose monitoring is an essential aspect of therapy. Additionally, a blood glucose log should be used to determine the effectiveness of the medication regimen.6,7 Continuous glucose monitoring allows the healthcare provider to view glycemic trends and helps the patient avoid hypoglycemia and hyperglycemia.8
MiniMed 670G Insulin Pump System
The MiniMed 670G insulin pump system (FIGURE 1) is used for management of T1DM in patients aged 7 years and older.9 This device uses a computerized program that continuously monitors the user’s glucose for up to 7 days and automatically adjusts the delivery of long-acting or basal insulin based on the glucose reading. If the blood glucose level is low, the MiniMed 670G will detect it and decrease or stop the supply of insulin. Conversely, when the blood glucose level is high, the device will increase the insulin delivery.9
The MiniMed 670G consists of a glucose-sensing wire that is placed on the skin of the abdomen. The glucose-sensing wire sends data to the insulin pump, resulting in adjusted insulin delivery based on the user’s readings. See FIGURE 2 for a sample sensor reading.9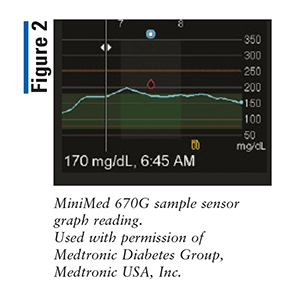
Efficacy
A prospective study published in 2019 analyzed the effectiveness of the MiniMed 670G device in children with T1DM.10 Included in the study were 105 patients aged 7 to 13 years who used the 670G device for 2 weeks in its manual mode, followed by 3 months in its automatic setting. Patients were scheduled for three office visits, three phone visits, and one hotel period during which they were directly monitored, uninterrupted, for a duration of 6 days and 5 nights. Compared with baseline, end-of-study data collection revealed a 6.9% decrease in serum glucose and an A1C decrease of 0.4% (7.9%-7.5%), and the percentage of time in target glucose range increased by 8.8% (56.2%-65.0%). Additionally, no patients experienced hypoglycemia or diabetic ketoacidosis.
Conclusion
Although T1DM is challenging to manage, the MiniMed 670G insulin pump system has shown high efficacy in reducing the risk of complications and improving glucose management. See www.fda.gov/medical-devices/recently-approved-devices/minimed-670g-system-p160017s031 for more information on this device.
REFERENCES
1. American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabetes Care. 2012;35(suppl 1):S64-S71.
2. Auday BC, Buratovich MA, Marrocco GF, Moglia P, eds. Diabetes mellitus. Salem Health Magill’s Medical Guide. 8th ed. Amenia, NY: Salem Press; 2018:678-682.
3. CDC. National Diabetes Statistics Report. www.cdc.gov/diabetes/data/statistics-report/index.html. Accessed April 23, 2020.
4. Kyoto Encyclopedia of Genes and Genomes. Disease: type 1 diabetes mellitus. www.kegg.jp/dbget-bin/www_bget?ds:H00408. Accessed February 19, 2020.
5. Mayo Clinic. Type 1 diabetes. www.mayoclinic.org/diseases-conditions/type-1-diabetes/symptoms-causes/syc-20353011. Accessed October 1, 2019.
6. Korsgren S, Molin Y, Salmela K, et al. On the etiology of type 1 diabetes: a new animal model signifying a decisive role for bacteria eliciting an adverse innate immunity response. Am J Pathol. 2012;181(5):1735-1748.
7. American Diabetes Association. The big picture: checking your blood glucose. www.diabetes.org/diabetes/medication-management/blood-glucose-testing-and-control/checking-your-blood-glucose. Accessed April 23, 2020.
8. American Diabetes Association. Standards of Medical Care in Diabetes—2019 abridged for primary care providers. Clin Diabetes. 2019;37(1):11-34.
9. Medtronic MiniMed 670G insulin pump system. www.medtronicdiabetes.com/products/minimed-670g-insulin-pump-system. Accessed April 23, 2020.
10. Forlenza GP, Pinhas-Hamiel O, Liljenquist DR, et al. Safety evaluation of the MiniMed 670G system in children 7–13 years of age with type 1 diabetes. Diabetes Technol Ther. 2019;21(1):11-19.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





