US Pharm. 2018;43(10):25-34.
ABSTRACT: Clinical inertia is the failure of a healthcare provider to initiate or intensify treatment when indicated. Achievement of treatment goals in patients with type 2 diabetes mellitus (T2DM) is suboptimal, which may be partly due to clinical inertia. T2DM is a complex disease that requires specialized knowledge, training, and a team-based collaborative approach to care. Many diabetes-related training opportunities exist to improve confidence, knowledge, and needed skills in pharmacists who may be involved in caring for patients with T2DM.
According to the CDC’s most recent estimates, 30.3 million people in the United States have diabetes and 7.2 million are undiagnosed.1 In 2015, almost 10% of the U.S. population had type 2 diabetes mellitus (T2DM) and 34% of persons aged 18 years and older had prediabetes.1 This number is expected to grow, with more than half of newly diagnosed cases each year occurring in adults aged 45 to 64 years.1 T2DM is a complex disease that imposes lifestyle, psychosocial, and financial burdens.2
The proportion of patients with T2DM who achieve recommended treatment goals has improved over the past 10 years, but it remains suboptimal.3 According to National Health and Nutrition Examination Survey data for 1998 to 2010, just over 50% of patients achieved a glycosylated hemoglobin (HbA1C) level below 7%, and fewer than 20% of patients attained metabolic control (based on HbA1C, blood pressure, and LDL cholesterol [LDL-C]).4 Evidence from landmark T2DM clinical trials has demonstrated that an HbA1C level higher than 7% increases the risk of microvascular diabetes-related complications such as retinopathy, nephropathy, and peripheral and autonomic neuropathy.5
As T2DM progresses, it becomes more difficult to manage—for both the healthcare team and the patient.6,7 At diagnosis, a patient may have already lost up to 50% of his or her beta-cell function (the clinical course of T2DM being characterized by progressive decline in beta-cell mass and function).8 Because these pathophysiological changes occur years before T2DM is diagnosed, early pharmacologic and nonpharmacologic therapy—without delays in treatment intensification—is important.
Clinical Inertia in Diabetes Care
Clinical inertia is the lack of treatment intensification in a patient who has not reached evidence-based goals for care.9 Stated another way, it is the failure of a healthcare provider to initiate or intensify therapy when indicated. Guideline recommendations suggest intensifying treatment if a T2DM patient is not at goal after 3 months of therapy.10,11 Studies have indicated, however, that the time frame is much longer: Treatment intensification is often delayed for several years, putting patients with T2DM at risk for microvascular and macrovascular complications.12,13 In two of the largest retrospective studies of clinical inertia to date, the median time to treatment intensification was 1 to 3 years.14-16 In these studies, patients with higher HbA1C were more likely to receive treatment intensification, which suggests that intensification should occur earlier in the course of disease.
The decision to intensify a patient’s diabetic treatment regimen is complex and multifactorial. Clinicians must individualize diabetes care based on drug efficacy, risk of side effects from antidiabetic medications (e.g., hypoglycemia), affordability, patient engagement, motivation, disease duration, life expectancy, and the patient’s support system.14,15 According to the Agency for Healthcare Research and Quality, clinical inertia has three primary sources: the physician, the patient, and office-system factors.9 Physician or provider factors include insufficient time during an office visit to address the complexities of diabetes care. Patient factors may include low health literacy, access to care, or trust in the patient-provider relationship. Office-system factors may involve the absence of clinical decision support or lack of a team-based approach to diabetes care.9 Pharmacists are well positioned to help mitigate clinical inertia. In fact, several organizations, including the CDC, the U.S. Public Health Service, and the American Medical Association, have issued statements in support of collaborative team-based care including a pharmacist for improving patient outcomes.17-19
Team-Based Care Models for Overcoming Clinical Inertia
Despite several clinical interventions developed over the past decade that focus on health system–level improvements in diabetes care, the quality of care for patients with diabetes remains suboptimal.20 As the U.S. healthcare system accelerates toward value-based contracting through private and government healthcare payers, pharmacists have an opportunity to play a key role in achieving quality and financial benchmarks. Specifically, pharmacists in these settings can focus on optimizing appropriate medication use, identifying gaps in care, and establishing clinical services—in collaboration with a medical provider—that are targeted to a particular patient population, such as persons with diabetes.
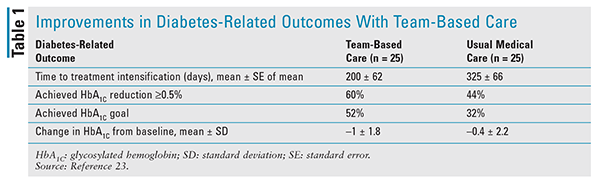
The benefits of integrating pharmacists into physician practices and working under a collaborative drug-therapy management (CDTM) arrangement are well described.21 CDTM agreements allow the pharmacist to initiate, adjust, and monitor pharmacotherapy in collaboration with a provider.22 Recent literature indicates that pharmacist-managed diabetes care can help patients achieve glycemic goals in a shorter time frame compared with standard care.23,24 In a study of two family-medicine practices in which pharmacists had a CDTM arrangement with a physician, patients with T2DM managed in this way achieved a shorter time to treatment intensification and a greater reduction in HbA1C compared with T2DM patients managed solely by a medical provider (TABLE 1).23 In a similarly designed study that lacked a CDTM arrangement, patients who participated in a pharmacist-managed diabetes clinic achieved goal HbA1C, systolic blood pressure, and LDL-C levels sooner than patients who were managed only by a medical provider.24 These results suggest that the use of a pharmacist in the primary care setting may help overcome clinical inertia.
Pharmacists not practicing under a CDTM arrangement may still potentially improve diabetes care by providing diabetes self-management education and support (DSME/S) as an instructor in an accredited or recognized program. DSME/S is a collaborative process through which patients with prediabetes or T2DM gain the knowledge and skills necessary to modify behavior and successfully self-manage diabetes and its related conditions.25 Since diabetes care is primarily self-directed by the patient, pharmacists are well positioned to provide self-management support and knowledge to sustain the behaviors needed to achieve optimal diabetes outcomes.26 The literature has shown that DSME/S is cost-effective, lowers HbA1C, and leads to greater use of recommended screenings (i.e., kidney and eye examinations) in patients with prediabetes or T2DM.27
An additional resource is the CDC’s Rx for the National Diabetes Prevention Program (DPP), which was developed to expand the reach of the National DPP in any pharmacy setting.28 Therefore, pharmacists who are looking to create and sustain a diabetes outreach program may consider targeting a specific diabetic population (i.e., prediabetes or T2DM) in line with the National DPP.
Reimbursement Opportunities for Diabetes-Related Services
An increasing number of healthcare systems and physician groups in the U.S. are entering into value-based contracts with payers to effectively manage the health and costs of at-risk populations by improving quality of care. One of the most common value-based care models, the accountable care organization (ACO), reflects a transition away from fee-for-service payment.29 In this healthcare-delivery model, pharmacists should focus on population health and addressing gaps in care. This may involve helping an ACO achieve quality metrics through DSME/S or direct patient-care services for a defined population, such as patients with prediabetes or T2DM. As shown in TABLE 2, pharmacists can impact several quality metrics in an ACO that are related to diabetes management.30

In the absence of recognition as healthcare providers under the Social Security Act or by the Centers for Medicare & Medicaid Services, many pharmacists are seeking opportunities to be reimbursed for their cognitive services. DSME/S is a reimbursable service that pharmacists can provide; depending on the setting, pharmacists may be active in providing DSME/S and collaborative disease management. Potential payers for pharmacist services include the federal government (Medicare Part B), private organizations (commercial insurers, self-insured employers), and state-run programs (Medicaid, insurance exchanges). Billing is determined by the state’s scope of pharmacy practice, but in general, pharmacists are considered auxiliary personnel and can bill under “incident-to” rules if they work in a hospital or provider-based facility.31,32 It is advisable to ensure compliance with billing requirements through local and state regulatory bodies.
Pharmacists seeking reimbursement for diabetes-related services may consider the use of diabetes education G-codes if they work within an accredited DSME program (TABLE 3).33 Organizations such as the American Association of Diabetic Educators and the American Diabetes Association provide accreditation. These programs may require credentialing as a Certified Diabetes Educator (CDE) or Board-Certified Advanced Diabetes Manager (BC-ADM).

Advanced-Training Opportunities in Diabetes Education and Care
Research has found that, among pharmacists, a perceived lack of knowledge or skills may be a barrier to providing diabetes-related education and related clinical services.34,35 As a result, many training opportunities have been created for pharmacists to expand their knowledge of diabetes care by completing certificate or training programs at various colleges and schools of pharmacy across the U.S. Additionally, the American Pharmacists Association (APhA) offers a certificate training program (“The Pharmacist and Patient-Centered Diabetes Care”) that will equip the pharmacist with the necessary skills, knowledge, and confidence to provide evidence-based and effective diabetes care. Self-study and live-seminar components are required to earn the APhA certificate.
Practice-based certifications also exist for licensed pharmacists. The two most common certifications are the CDE and BC-ADM. According to the National Certification Board for Diabetes Educators, a CDE educates and supports patients with diabetes and works to promote self-management to attain individualized behavior and treatment goals that optimize health outcomes.36 The BC-ADM credential is managed through the American Association of Diabetes Educators (AADE). According to the AADE, the BC-ADM manages complex patient needs and assists patients with therapeutic problem-solving within their discipline’s scope of practice. This may include adjusting medication, treating and monitoring acute or chronic complications, counseling patients on lifestyle modification, addressing psychosocial issues, and participating in research and mentoring.37 To date, nearly 20,000 health professionals hold the CDE credential; however, pharmacists account for only 7% of all CDEs.36
Conclusion
Pharmacists play a key role in the management of patients with prediabetes and T2DM. This may include providing direct patient care and disease management under a collaborative agreement, creation of screening or diabetes-related treatment protocols, DSME/S, or a combination of these services. The need to prevent, or to intervene to eliminate, clinical inertia in diabetes management has never been greater. Many training programs exist for pharmacists to further their knowledge and skill in providing diabetes care. Pharmacists have increasingly more opportunities to establish CDTM arrangements, improve quality of diabetes care, and receive reimbursement for diabetes education and management.
REFERENCES
1. CDC. National diabetes statistics report, 2017: estimates of diabetes and its burden in the United States. www.diabetes.org/assets/pdfs/basics/cdc-statistics-report-2017.pdf. Accessed June 19, 2018.
2. American Diabetes Association. 3. Comprehensive medical evaluation and assessment of comorbidities: Standards of Medical Care in Diabetes—2018. Diabetes Care. 2018;41(suppl 1):S28-S37.
3. Ali MK, Bullard KM, Saaddine JB, et al. Achievement of goals in U.S. diabetes care, 1999-2010. N Engl J Med. 2013;368(17):1613-1624.
4. Stark Casagrande S, Fradkin JE, Saydah SH, et al. The prevalence of meeting A1C, blood pressure, and LDL goals among people with diabetes, 1988-2010. Diabetes Care. 2013;36(8):2271-2279.
5. American Diabetes Association. 10. Microvascular complications and foot care: Standards of Medical Care in Diabetes—2018. Diabetes Care. 2018;41(suppl 1):S105-S118.
6. Kendall DM, Cuddihy RM, Bergenstal RM. Clinical application of incretin-based therapy: therapeutic potential, patient selection and clinical use. Am J Med. 2009;122(suppl 6):S37-S50.
7. Gromada J, Franklin I, Wollheim CB. Alpha-cells of the endocrine pancreas: 35 years of research but the enigma remains. Endocr Rev. 2007;28(1):84-116.
8. Garber AJ. Incretin effects on -cell function, replication, and mass: the human perspective. Diabetes Care. 2011;34(suppl 2):S258-S263.
9. O’Connor PJ, Sperl-Hillen JM, Johnson PE, et al. Clinical inertia and outpatient medical errors. In: Henriksen K, Battles JB, Marks ES, Lewin DI, eds. Advances in Patient Safety: From Research to Implementation. Volume 2: Concepts and Methodology. AHRQ Publication No. 05-0021-2. Rockville, MD: Agency for Healthcare Research and Quality; 2005.
10. American Diabetes Association. 6. Glycemic targets: Standards of Medical Care in Diabetes—2018. Diabetes Care. 2018;41(suppl 1):S55-S64.
11. Garber AJ, Abrahamson MJ, Barzilay JI, et al. Consensus statement by the American Association of Clinical Endocrinologists and American College of Endocrinology on the comprehensive type 2 diabetes management algorithm—2018 executive summary. Endocr Pract. 2018;24(1):91-120.
12. Mata-Cases M, Benito-Badorrey B, Roura-Olmeda P, et al. Clinical inertia in the treatment of hyperglycemia in type 2 diabetes patients in primary care. Curr Med Res Opin. 2013;29:1495-1502.
13. Paul SK, Klein K, Thorsted BL, et al. Delay in treatment intensification increases the risks of cardiovascular events in patients with type 2 diabetes. Cardiovasc Diabetol. 2015;14:100.
14. Pantalone KM, Misra-Hebert AD, Hobbs TM, et al. Clinical inertia in type 2 diabetes management: evidence from a large, real-world data set. Diabetes Care. 2018;41(7):e113-e114.
15. Pantalone KM, Wells BJ, Chagin KM, et al. Intensification of diabetes therapy and time until A1C goal attainment among patients with newly diagnosed type 2 diabetes who fail metformin monotherapy within a large integrated health system. Diabetes Care. 2016;39(9):1527-1534.
16. Khunti K, Wolden ML, Thorsted BL, et al. Clinical inertia in people with type 2 diabetes: a retrospective cohort study of more than 80,000 people. Diabetes Care. 2013;36(11):3411-3417.
17. CDC. Advancing Team-Based Care Through Collaborative Practice Agreements: A Resource and Implementation Guide for Adding Pharmacists to the Care Team. Atlanta, GA: CDC, U.S. Dept of Health and Human Services; 2017.
18. Giberson S, Yoder S, Lee MP. Improving Patient and Health System Outcomes Through Advanced Pharmacy Practice. A Report to the U.S. Surgeon General. Office of the Chief Pharmacist U.S. Public Health Service; December 2011.
19. Choe HM, Standiford CJ, Brown MT. Embedding pharmacists into the practice. AMA. www.stepsforward.org/Static/images/modules/46/downloadable/embedded_pharmacists.pdf. Accessed June 19, 2018.
20. Saaddine JB, Cadwell B, Gregg EW, et al. Improvements in diabetes processes of care and intermediate outcomes: United States, 1988-2002. Ann Intern Med. 2006;144(7):465-474.
21. Hwang AY, Gums TH, Gums JG. The benefits of physician-pharmacist collaboration. J Fam Pract. 2017;66(12):e1-e8.
22. McBane SE, Dopp AL, Abe A, et al. Collaborative drug therapy management and comprehensive medication management-2015. Pharmacotherapy. 2015;35(4):e39-e50.
23. Cowart K, Sando K. Pharmacist impact on treatment intensification and hemoglobin A1C in patients with type 2 diabetes mellitus at an academic health center. J Pharm Pract. 2018:897190018776178.
24. Yam FK, Adams AG, Divine H, et al. Clinical inertia in type 2 diabetes: a retrospective analysis of pharmacist-managed diabetes care vs. usual medical care. Pharm Pract (Granada). 2013;11(4):203-210.
25. Powers MA, Bardsley J, Cypress M, et al. Diabetes self-management education and support in type 2 diabetes: a joint position statement of the American Diabetes Association, the American Association of Diabetes Educators, and the Academy of Nutrition and Dietetics. Diabetes Educ. 2015;41(4):417-430.
26. Burke SD, Sherr D, Lipman RD. Partnering with diabetes educators to improve patient outcomes. Diabetes Metab Syndr Obes. 2014;7:45-53.
27. Chrvala CA, Sherr D, Lipman RD. Diabetes self-management education for adults with type 2 diabetes mellitus: a systematic review of the effect on glycemic control. Patient Educ Couns. 2016;99(6):926-943.
28. CDC. Rx for the National Diabetes Prevention Program: Action Guide for Community Pharmacists. Atlanta, GA: CDC, U.S. Dept of Health and Human Services; 2018.
29. Chee TT, Ryan AM, Wasfy JH, Borden WB. Current state of value-based purchasing programs. Circulation. 2016;133(22):2197-2205.
30. Centers for Medicare & Medicaid Services Medicare Shared Savings Program. Accountable care organization (ACO) 2018 quality measures. www.cms.gov/Medicare/Medicare-Fee-for-Service-Payment/sharedsavingsprogram/Downloads/2018-reporting-year-narrative-specifications.pdf. Accessed August 22, 2018.
31. Traynor K. Pharmacists praise new Medicare billing opportunities: provider status still critical, they say. Am J Health Syst Pharm. 2015;72(2):91-92.
32. Traynor K. CMS chief affirms incident-to billing for pharmacists is allowed. Am J Health Syst Pharm. 2014;71(12):977-978.
33. American Association of Diabetes Educators. Diabetes education services: reimbursement tips for primary care practice. www.integration.samhsa.gov/images/res/Diabetes_Education_Services6-10%20(2).pdf. Accessed August 28, 2018.
34. Schapansky LM, Johnson JA. Pharmacists’ attitudes toward diabetes. J Am Pharm Assoc (Wash). 2000;40(3):371-377.
35. Younis WS, Campbell S, Slack MK. Pharmacists’ attitudes toward diabetes and their involvement in diabetes education. Ann Pharmacother. 2001;35(7-8):841-845.
36. National Certification Board for Diabetes Educators. www.ncbde.org. Accessed June 19, 2018.
37. American Association of Diabetes Educators. Board certified-advanced diabetes management (BC-ADM). www.diabeteseducator.org/education/certification/bc_adm. Accessed June 19, 2018.
To comment on this article, contact rdavidson@uspharmacist.com.





