US Pharm. 2013;38(8):18-20.
The induction of structural and functional changes in the kidneys of aging adults as part of the normal aging process is variable with regard to its timing and relationship to comorbid conditions. It is expected that the glomerular filtration rate (GFR) of the average individual will lose 0.8 mL/min/1.73m2 per year.1 And while these progressive changes are characterized by the development of glomerularsclerosis and interstitial fibrosis, approximately 30% of elderly individuals will not exhibit an age-related decrease in their GFR.1 Other seniors are not as fortunate.Nephrotic syndrome (NS) is kidney disease causing proteinuria (leakage of all plasma proteins), hypoalbuminemia, and edema. Since generalized edema is the major clinical manifestation of this condition, it is often misdiagnosed as congestive heart failure in geriatric patients.1
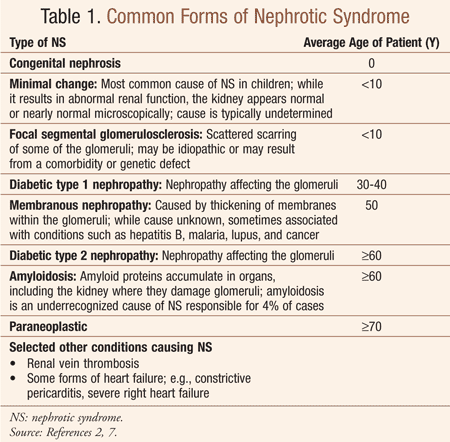
In the United States, the most common important cause or type of NS is diabetic nephropathy, occurring at an estimated rate of approximately 50 cases per million population.2 In children, NS may occur at a rate of 20 cases per million children.3 TABLE 1 lists the various common types of NS with the average patient age. Pharmacists are encouraged to become familiar with the medications and complications associated with NS (see below), and to specifically note that in geriatric patients with NS there is a higher incidence of hypertension, hypercholesterolemia, and nonselective proteinuria (vs. selective proteinuria that is more than 85% albumin).1,2 Furthermore, such seniors present with a lower GFR value and often exhibit microscopic hematuria.1,2
Etiology, Signs, and Symptoms
The etiological basis for the development of NS is damage to renal glomeruli causing proteinuria (primarily albumin), hypoalbuminemia, and thus disorder in fluid homeostasis. Nephrotic syndrome-range proteinuria is 3 g per day or more; on a single spot urine collection, it is 2 g of protein per gram of urine creatinine.2 NS produces symptoms that include 1) edema, especially peripherally as in the periorbital area and lower extremities; 2) urine with a foamy appearance, which may be associated with proteinuria; and 3) weight gain secondary to fluid retention.
The most common primary causes are minimal change disease, focal segmental glomerulosclerosis, and membranous nephropathy (MN); secondary causes account for more than 50% of adult cases, with the most common being diabetic nephropathy and preeclampsia.4 Certain drugs can induce nephrotic syndrome, including nonsteroidal anti-inflammatory drugs (NSAIDs), gold therapy, penicillamine, heroin, interferon-alfa, lithium, and pamidronate.2,5,6 In certain cases of NS, discontinuation of NSAID therapy may be the only necessary intervention.1
Complications
Potential complications of NS contribute to the complexity of its management and include:1,2,4,7,8
Hypercoagulability: Urinary loss of anticoagulant proteins (e.g., antithrombin III, plasminogen) in addition to an increase in clotting factors (e.g., factors I, VII, VIII, X) appears to be responsible for this condition; it is of particular risk for a bedridden geriatric patient who is already at risk for deep venous thrombosis and pulmonary embolus as a result of immobilization.
Hyperlipidemia: Rather than a mere complication, this condition may be considered a typical feature of NS; hypoproteinemia contributes to reactive hepatic synthesis of proteins, including lipoproteins.
Malnutrition: Excessive hypoproteinemia leads to poor nutrition and weight loss; gut edema may cause defective absorption, causing chronic malnutrition; decreased body weight may be masked by edematous body swelling including ascites and pleural effusion.
Hypertension: Uremia can induce elevated blood pressure.
Acute renal failure (ARF): ARF may be indicative of underlying glomerulonephritis; however, it is usually precipitated by hypovolemia or sepsis. Uremia may require emergency renal dialysis. NS may occur in persons with sickle cell disease and progress to renal failure.
Chronic kidney failure: May require renal dialysis or a renal transplant. Risk factors for progression to end-stage renal disease (ESRD) associated with MN include male gender, poorly controlled hypertension, renal insufficiency, and heavy proteinuria.
Increased risk of infection: Bacterial sepsis, cellulitis, pneumonia, and peritonitis are the most common infectious complications; varicella infection is also common. Proteinuria may also cause hypocalcemia with bone abnormalities and hypovolemia; MN may complicate bone marrow transplantation, in association with graft-versus-host disease.
Diagnosis
In the elderly, NS may go unrecognized, as it often presents in an atypical manner; edema frequently develops only in dependent areas of the body.1 The following measurements or tests are necessary: serum creatinine, blood urea nitrogen (BUN); albumin; cholesterol; urine collection to quantify proteinuria and creatinine clearance; electrophoresis and immunoelectrophoresis for serum protein and urine protein; antinuclear antibody (ANA); and antideoxyribonucleic acid (anti-DNA) antibody titer.1,2
When NS is secondary to a systemic comorbidity, it presents in the elderly much the same as it does in a younger adult; however, in seniors NS is frequently masked by other comorbid conditions. Each NS patient should undergo evaluation for amyloidosis, collagen vascular disorders, diabetes mellitus, hepatitis B and C, HIV, cryoglobulins, and plasma cell dyscrasias.1 Renal biopsy is essential to definitively determine histologic diagnosis and aid in the management of NS in elderly patients.1
Of all geriatric patients who pre-sent with NS, approximately 5% will either have an underlying malignancy or develop one within 1 year, and approximately one-third of these elderly patients will be diagnosed with MN.1 Since lung cancer is the most common malignancy associated with MN, and colon cancer is the next most common site for a non-evident malignancy, a chest x-ray and a stool guaiac test are recommended as the only tests that should be performed in all patients presenting with NS.1 If these tests are negative, it is recommended that the patient be followed carefully for the presentation of a malignancy for the next 15 months and receive routine care thereafter.
Management
Medication therapy management of NS is evolving continuously, so consultation with a nephrologist is appropriate. Exact treatment depends on the histologic type of NS (see Reference 4); corticosteroids (e.g., prednisone), cyclophosphamide, and cyclosporine are used to induce remission. In certain drug-induced cases, discontinuation of NSAID therapy may be the only necessary intervention. Control of signs and symptoms and treatment of complications of NS generally include the following medications regardless of histologic type:1,2,4,6,9,10
Antihypertensives: Blood pressure goal is around 125/75 mm Hg; owing to their efficacy in reducing proteinuria and data suggesting their potential to slow progression of renal disease, ACE inhibitors (ACEIs) or angiotensin II receptor blockers are becoming the mainstay of treatment; they may cause or exacerbate hyperkalemia in patients with moderate-to-severe renal insufficiency. ACEIs and non–dihydropyridine calcium channel blockers (e.g. diltiazem, verapamil) have greater antiproteinuric and renoprotective effects when used together, and their antiproteinuric effect is enhanced by sodium restriction.
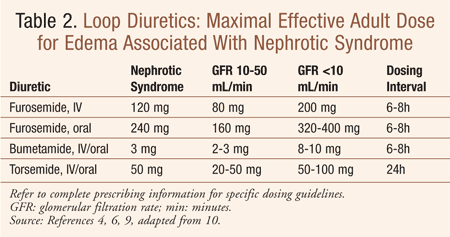
Diuretics: Edema associated with NS is treated pharmacologically with loop diuretics (TABLE 2) or spironolactone (25-200 mg/day orally divided once daily to twice daily) to the desired therapeutic outcomes of minimization of edema and improvement in organ function. Controversy does exist, however, as to the philosophy of diuretic use in cases of diuretic resistance associated with NS; specifically, whether combination diuretic therapy or higher-than-average doses of a single diuretic agent are preferable. If symptoms of orthostatic hypotension develop or serum creatinine increases by more than 30%, the diuretic dosage should be decreased.
Statins to control hyperlipidemia, such as atorvastatin, fluvastatin, lovastatin, pravastatin, rosuvastatin, and simvastatin, may be prescribed.
Anticoagulants to target hypercoagulability, such as heparin or warfarin, may be prescribed.
Immunosuppressants, such as corticosteroids, may decrease the inflammation that accompanies certain kidney disorders, such as MN, in which one-third of patients are expected to progress to ESRD; steroids, in combination with cytotoxic agents and cyclosporine, are considered with regard to dosage, duration, and other factors related to comorbidities. In steroid-resistant geriatric patients with minimal change disease, cyclophosphamide may be used with appropriate dosing based on GFR and white blood cell count monitoring.
Other medications used include mycophenolate mofetil, synthetic corticotropin, and rituximab. Outpatient monitoring for steroid toxicity (e.g., every 3 months) assists in the detection of adverse effects; annual monitoring for cataracts is recommended, and supplemental calcium and vitamin D may attenuate bone loss.
Lifestyle modifications such as dietary changes may help patients with nephrotic syndrome; referral to a registered dietician—which is reimbursed by Medicare—may be helpful for seniors to learn how to choose lean sources of protein and to reduce fat and cholesterol in their diet to assist with controlling hyperlipidemia.
Conclusion
NS ensues when damaged glomeruli cause edema, proteinuria, and hypoalbunemia; associated complications include thromboembolism and a particular risk for hypertension and hyperlipidemia in the elderly. Knowledge of causes and complications in vulnerable seniors can assist pharmacists in providing these patients with appropriate dietary, pharmacologic, and monitoring recommendations and interventions.
REFERENCES
1. Schlanger L, Sands JM, Bailey JL. Renal disease. In: Hazzard WR, Blass JP, Halter JB, et al. Hazzards Geriatric Medicine and Gerontology. 6th ed. New York, NY: McGraw-Hill, Inc.; 2009:1018-1034.
2. Cohen EP, Sinnakirouchenan R.
Nephrotic syndrome. Updated June 10, 2013.
http://emedicine.medscape.com/article/244631-overview#showall. Accessed
July 12, 2013.
3. Wong W. Idiopathic nephrotic syndrome
in New Zealand children, demographic, clinical features, initial
management and outcome after twelve-month follow-up: results of a
three-year national surveillance study. J Paediatr Child Health. 2007;43(5):337-341.
4. Nephrotic syndrome. Merck Manual
online. Updated November 2012.
www.merckmanuals.com/professional/genitourinary_disorders/glomerular_disorders/nephrotic_syndrome.html#v1055705.
Accessed July 16, 2013.
5. Nephrotic syndrome. Cause. WebMD. Updated May 17, 2011. www.webmd.com/a-to-z-guides/nephrotic-syndrome-cause. Accessed July 16, 2013.
6. Semla TP, Beizer JL, Higbee MD. Geriatric Dosage Handbook. 18th ed. Hudson, OH: Lexi-Comp, Inc; 2013.
7. Nephrotic syndrome. Mayoclinic.com.
January. 11, 2012. www.mayoclinic.com/health/nephrotic-syndrome/DS01047.
Accessed July 12, 2013.
8. Appel GB, Blum CB, Chien S, et al. The
hyperlipidemia of the nephrotic syndrome. Relation to plasma albumin
concentration, oncotic pressure, and viscosity. N Engl J Med. 1985;312(24):1544-1548.
9. Harvey RA, Champe PC, eds. Pharmacology. 4th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2009:472-473,489-490.
10. Coyle JD, Matzke GR. Disorders of sodium and water homeostatsis. In: DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 8th ed. New York, NY: McGraw-Hill Inc; 2011:873-890.
To comment on this article, contact rdavidson@uspharmacist.com.






